Telemedicine has proven to be a crucial lifeline in some rural communities, helping to address workforce shortages and reducing the burden on patients who might otherwise have to travel long distances for specialty care. In addition to enabling patients to have remote consults with specialists (particularly for psychiatrists or other providers who are mostly absent in rural communities), telemedicine allows rural hospitals to outsource diagnostic or other services and can help reduce providers’ sense of isolation.1
Some rural health systems have invested heavily in telehealth — seeing it not just as a way to fill gaps in services but to enable team care delivery using a hub-and-spoke model. The integrated delivery system Avera Health is one of the leaders, providing telemedicine services to a network of more than 130 rural clients from a virtual hospital based in Sioux Falls, S.D.
Despite the potential, a 2013 review found that two-thirds of rural hospitals did not use any telemedicine services, in part because of lack of access to broadband.2 And some rural providers remain skeptical that technology will solve their problems.
Avera Health: Reaching into Rural Communities from a Virtual Hospital
Avera Health, an integrated delivery system based in Sioux Falls, S.D., ventured into telemedicine 25 years ago to offer patients in rural parts of the state access to specialists. Over the next two decades, the health system has vastly expanded the services it provides remotely — supporting not just its own facilities but small and rural hospitals in 13 states, enabling these hospitals to leverage the expertise of clinicians gathered in a virtual hospital at the health system’s Sioux Falls headquarters.

From the 30,000-square-foot facility and outposts in Michigan and New Hampshire, a wide range of specialists — including critical care and emergency medicine physicians and pharmacists — are available at all hours to provide support via video and telephone to facilities that might not otherwise be able to recruit or retain such providers.
More than 130 rural hospitals use its “eEmergency” service, allowing them to handle complex cases including trauma that may arise only a few times a year. Having this support permits many to lean on nurse practitioners and physician assistants for overnight shifts, improving the call schedule for area physicians, which in turn helps with recruitment.
“People can have careers that are more like what they would have in urban settings,” says Deanna Larson, CEO of Avera’s eCARE division. It also helps build the confidence and competency of local staff. “One of our physicians helped a nurse practitioner in a very remote area insert a chest tube in a young girl who had been in an ATV accident — guiding the intubation using a camera to see airway. Those kinds of procedures are very scary for people working in isolation. People begin to doubt themselves.”

Roughly 75 rural hospitals have signed up for Avera’s “ePharmacy” service, through which pharmacists with access to each of the hospital’s electronic medical record systems review medication orders, provide discharge instructions, and alert staff to changes that may be needed based on lab results. Pharmacists can then send orders that unlock dispensing units on site. “A lot of these hospitals don’t have a pharmacist 24/7,” Larson says.3
Avera charges hospitals a flat rate for its eEmergency service — roughly equivalent to a nurse’s salary — which Larson says facilities are able to recoup by keeping patients in their communities rather than transferring them to tertiary care centers in large cities for some procedures. This also keeps jobs in the communities, she says. One study found the potential for savings for rural hospitals is greatest for those relying on physician assistants in the emergency department, because this reduces the need for locum tenens, and keeps patients, including the commercially insured, in the community.4
The process of establishing programs can be protracted, however, because of the credentialing required to provide services remotely, changes needed to hospital bylaws, and the time it takes to build the broadband capacity to get imaging back and forth. Some hospitals get support for initial investment in equipment and fees from the Leona M. and Harry B. Helmsley Charitable Trust, which provides funding for rural hospitals in Iowa, Montana, Nebraska, North and South Dakota, and Wyoming.
There’s also an adjustment period for hospital staff. “People feel at first as though someone is looking over their shoulder, but after one or two good interactions, they’re glad to have that partner in the room,” Larson says. Sioux Falls clinicians attend staff meetings at the hospitals they serve via video or teleconference.
Patients also seem to like it, she says. “They want to support their local hospital to ensure access and viability. They also get attached to the providers via video and want to meet them in person, we find.”
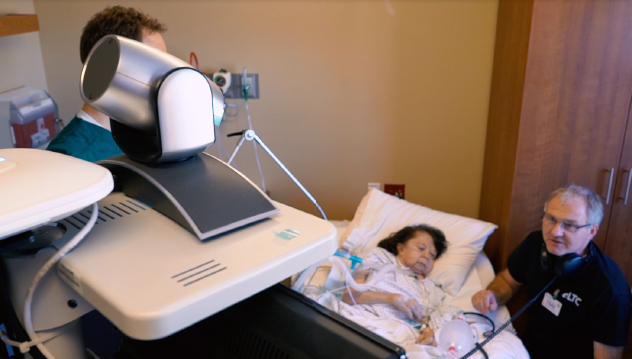
Avera is now expanding into other settings that have difficulty recruiting providers, including prisons, schools, and long-term care facilities. For the latter, it relies on a geriatrician-led team that includes a social worker, pharmacist, behavioral health counselor, and advanced practice nurse. They respond to urgent care needs, help oversee care transitions and medication management, and train nursing home staff to identify health issues before they become more acute.
Avera tested the model in more than 30 nursing homes across four states, with funding from the Center for Medicare and Medicaid Innovation. Preliminary data show it reduced unplanned transfers to hospitals and emergency departments from 2.84 per 1,000 resident days in March 2015 to 1.73 in December 2016, a decline of nearly 40 percent, according to the health system.
Descriptions of products and services in Transforming Care are based on publicly available information and self-reported data provided by the institution(s) featured. Their inclusion should not be construed as an endorsement by The Commonwealth Fund.
Notes
1 B. Darves, “Telemedicine: Changing the Landscape of Rural Physician Practice,” New England Journal of Medicine CareerCenter, May 17, 2013, http://www.nejmcareercenter.org/article/telemedicine-changing-the-landscape-of-rural-physician-practice/. The adoption of telemedicine infrastructure in rural communities has been supported by federal grant programs, including the Distance Learning and Telemedicine program, (https://www.rd.usda.gov/programs-services/distance-learning-telemedicine-grants), as well as the growing number of payers that cover telemedicine services.
2 RUPRI Center for Rural Health Analysis reviewed 4,727 hospitals in the 2013 Healthcare Information and Management Systems Society’s Analytics database, see http://www.beckershospitalreview.com/healthcare-information-technology/how-telemedicine-is-transforming-treatment-in-rural-communities.html.
3 Avera clinicians also provide 24/7 oversight of patients in critical care through its e-ICU service but few rural hospitals have need for this, given their limited scope of services.
4 A. C. MacKinney, M. M. Ward, and F. Ullrich, “The Business Case for Tele-Emergency,” Telemedicine and e-HEALTH, Dec. 2015 21(12):1005–11.



