Summary: Seven groups that have been approved to receive Medicare claims data will soon begin to publicly report on the quality and cost of health care services provided to Medicare beneficiaries. The data-sharing program, mandated in the Affordable Care Act, is expected to galvanize quality improvement efforts by providing physicians and others with feedback on their performance.
By Martha Hostetter and Sarah Klein
Though data drives performance improvement in many sectors of the economy, it can be maddeningly difficult to acquire in health care. Information on the cost and quality of health care services is mostly disaggregated among payers and providers, making benchmarking and other forms of performance measurement a challenge. Several states and private groups have attempted to address the problem by creating all-payer claims databases, which aggregate medical, dental, and/or pharmacy claims from public and private payers to create a fuller picture of quality and resource use.
While this information has in some locations enabled providers to compare their performance with their peers and in others has increased the transparency of price and quality information for consumers, it has been incomplete without outpatient and pharmacy claims from Medicare's fee-for-service program, which together with inpatient services accounted for 21 percent of all health care spending in 2011.1 That is now changing. Thanks to lobbying by quality improvement collaboratives, health plans, and other purchasers, the Centers for Medicare and Medicaid Services (CMS) has begun to open its rich store of Medicare claims to outside groups through the Medicare Data Sharing for Performance Measurement Program, as mandated by the Affordable Care Act. This marks the first time that CMS has shared its outpatient and pharmacy data for purposes other than research.2
The information on outpatient and pharmacy claims supplements claims data on since most states mandate reporting of hospital discharge data for all patients.3 The new claims will allow those that receive them to explore the quality, costs, and resource use in ambulatory care settings, increasing the reliability of reporting on primary care or specialty care practices. This is because many chronic and expensive-to-treat conditions are more prevalent among the elderly and, without access to large volumes of data on Medicare beneficiaries, denominators are not large enough to accurately rate provider performance.
"We are quite excited because the program will make our reporting much more robust," says Mylia Christensen, executive director of the Oregon Health Care Quality Corp., one of the first of seven organizations (known under the program as "qualified entities") to receive provisional approval from CMS to participate in the program. The nonprofit, which hopes to receive the claims data this spring, plans to use it to enhance its reporting on the quality and utilization of health care services, which is now based on claims data from commercial health plans and the state's Medicaid program.
The Health Improvement Collaborative of Greater Cincinnati, another one of the qualified entities, will use Medicare data to explore the cost and utilization of ambulatory care in its region, with the ultimate goal of combining the claims information with clinical data. That "will let us see whether improvements made on the clinical side result in reduced costs—[and] see if we're meeting our goal of working toward the Triple Aim of improved care, improved health, and reduced costs," says Tim Salvage, the collaborative's project manager for performance measures.
All seven of the groups that have received provisional approval to participate in the program are regional organizations with experience in handling large data sets for the purposes of public reporting (see Box for a complete list.) Many have also participated in the Robert Wood Johnson Foundation's Aligning Forces for Quality program, which required public reporting by participants. But with the exception of California, the regions covered account for a relatively modest proportion of Medicare beneficiaries. One reason there aren't more qualified entities may be the process of acquiring the data, which has thus far proven complicated and expensive. Qualified entities have to demonstrate an ability to securely handle data and must pay a fee for them, which varies based on the size of the regions for which data is collected. They also are required to combine the Medicare data with data from another source, such as Medicaid or private claims—a complicated process that requires significant expertise.
And while the qualified entities are required to use the data for public reporting on provider performance, there are limitations on the use of data for purposes other than public reporting. For example, physicians cannot drill down into the data to compare performance or inform their improvement efforts. Qualified entities also have responsibilities for responding to physicians' concerns about its accuracy.4
According to those with experience combining and analyzing claims data, it can cost upwards of $1 million a year to do this, at least initially, money that can't be recouped by selling the information to others such as health plans and providers that have paid for other claims data in the past. The Affordable Care Act statute bars qualified entities from charging for providing the data or performance reports to physicians. Some say these and other requirements have discouraged potential applicants and limit the value of the program. "We ought to have thousands of [organizations] clamoring for this [data]," says John Toussaint, M.D., a leading proponent of using physician performance data as way of catalyzing improvement. "Instead we have seven."
But others see this initial release of the data as a crucial first step in a program that is likely to evolve. "With the Medicare data we can begin to look across the health system and raise questions about variation in care delivery—this is a first step in engaging physicians," says Denise Love, executive director of the National Association of Health Data Organizations (NAHDO).
Some say a cautious approach will help avoid missteps that harm efforts to increase transparency for consumers and providers. "I like the fact that CMS is being careful [in its release of the data]," says Keith Kanel, M.D., chief medical officer of the Jewish Healthcare Foundation, which leads the Pittsburgh Regional Health Initiative, another one of the groups with provisional approval to receive Medicare data. "If not done well, public reporting can be a damaging thing to a community," Kanel says. Having a neutral party, such as the Pittsburgh Regional Health Initiative working in partnership with Quality Insights of Pennsylvania (the state's quality improvement organization), to assemble the data also adds to credibility of the program, he says. "Patients, purchasers, employers—everyone is trying to sort through the mess of health care now and make good decisions. It's our responsibility to step up and provide objective and relevant information for our community."
The Power of Big Data
Existing all-payer claims databases (APCDs)—17 are in operation or development around the nation—demonstrate that even without Medicare's fee-for-service claims for ambulatory care, aggregated data has tremendous potential to inform health care decision making (see figure). Some, run by states, have combined data contributed by legislative mandate from private insurers with state Medicaid programs and hospital discharge data, while others supported by purchasers, providers, or employers depend on voluntary contributions. Among their many benefits, the APCDs have helped to assess the prevalence of chronic conditions in different communities to allocate public health dollars, populate public reporting sites for consumers, inform rate-setting by state regulators, and identify opportunities for policy reform.
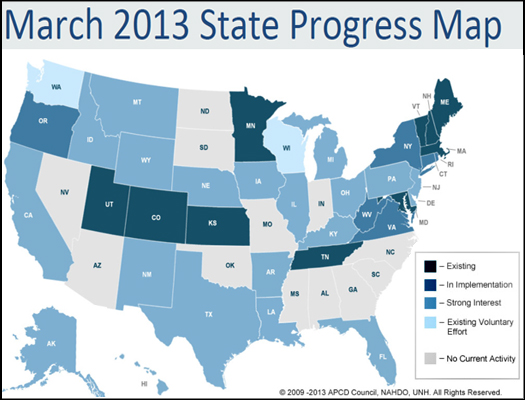
Source: APCD Council, a collaboration between the University of New Hampshire and the National Association of Health Data Organizations.
State-run or affiliated APCDs also have access to the Medicare claims data for research purposes—for instance to assess regional variation or population health, under a second program CMS rolled out in June 2013 to provide states with claims data. (States were able to apply to CMS to get Medicare data under a previous data-use agreement, but the new program will release data in a more timely way and, for bigger states, the costs of obtaining it may be lower.) Colorado's APCD, one of the country's most advanced, plans to obtain the claims information this way, and use it to assess the quality and cost of services in large physician groups, hospitals, and ambulatory surgery centers, ultimately publishing it on its website for consumers. The claims data may also be used for public health services such as monitoring vaccination rates, by ACOs to find the most efficient providers, and in the future, for comparative effectiveness research.
Because Wisconsin's APCD is run by a private organization, the Wisconsin Health Information Organization (WHIO), which has collected data on 4.2 million state residents, and is not state-run, it faces challenges in adding Medicare fee-for-service claims to its comparisons of physicians and physician groups on cost and quality for discrete episodes of treatment. To do so, WHIO would need to develop a business model that does not depend on data sales. It would also face limitations on acceptable measures for reporting (See Q&A for more detail.)
Next Steps
CMS is optimistic that more groups will join the program. "Over the next year—as the first performance reports utilizing Medicare reports are released—we expect to see the program grow significantly as more organizations join," says Niall Brennan, director of CMS' Office of Information Products and Data Analytics. "Our ultimate goal is to have at least one qualified entity in every state."
As the Medicare Data Sharing for Performance Measurement Program does evolve, those soon to be using the data and those that would like to acquire it hope to see more flexibility in the rules for reporting performance so that they can find new ways of identifying opportunities for improvement. For instance, CMS might allow the APCDs to report on episodes of care, which could help reveal variations in costs of care, patterns of hospital readmissions, or gaps in treatment.5 Others hope the application and data-handling process will be made easier and cheaper, perhaps by standardizing data formats across payer sources—something the APCD Council and NAHDO have been promoting. Because CMS is releasing Medicare claims to accountable care organizations, to states, and now to the qualified entities, there may be efficiencies of scale and opportunities for shared learning if CMS were to harmonize some of its data-use agreements across these various efforts.
"If we could figure out a way to [combine data sources] more efficiently—and stop doing it duplicatively within regions—we could make it much more efficient," says Michael DeLorenzo, interim CEO and director of health analytics at the Maine Health Management Coalition Foundation, another of the qualified entities to receive Medicare data. "Making data widely available to improve quality and efficiency for the benefit of patients, should be more important than the potential barriers."
Others would like CMS to allow providers to analyze the data directly. "If data is on a public site, we decide what's going to be displayed and in what format—that doesn't necessarily help providers," says Toussaint. "Providers need to have access to a full data set. They can then decide what it is they want to drill down into to find where the problems are."
In fact, President Obama's 2014 budget seeks to address this issue by expanding the program to give qualified entities greater leeway in their use of the claims data, beyond performance measurement. Under the proposal, Brennan says, qualified entities would be allowed to use the data for "value-added analysis" for providers, including releasing data to Medicare providers to inform their care coordination and improvement activities." The data might also be used for fraud prevention, he says.
Giving providers data with some identifying information on patients would also help them identify high utilizers of services and target care management interventions. "Eventually, we'd like to set up portals for providers so they can look at their panels of patients, all the services they are getting, where they are getting them from, and the costs of the services," DeLorenzo says.
NAHDO's Love notes that, in the short term, states are likely to use the APCDs as their core data set and link into clinical data as it becomes more easily accessible through electronic health record systems. "We're going to get smarter, more strategic, about pulling in specific elements of clinical data in order to look at what's driving variation, instead of just going after all of the clinical data we can get."
"We've not had the capability to begin to understand the cost side of the equation until APCDs began to emerge in Wisconsin and elsewhere," says Christopher Queram of the Wisconsin Collaborative for Healthcare Quality, a voluntary consortium of providers and health plans, employers, and other stakeholders. "So there is a pent-up interest in looking at cost or resource use. And then I think the challenge will be how do we pair those measures with the available clinical quality measures so we get at some actionable concept of value."
Qualified Entities Under Medicare's Data Sharing for Performance Measurement ProgramOregon Health Care Quality Corporation will combine Medicare's fee-for-service claims with those it already collects from commercial and Medicaid plans. The latter have been used to publicly report on measures of ambulatory care quality and resource use—including rates of cancer screening and use of generic drugs—by provider and provider group. The information has been available to consumers on PartnerForQualityCare.org, as well as to providers who use it not only to compare their results against local and national benchmarks but also to obtain the names of patients who have not received recommended care. "It gives them a free registry so they can do appropriate follow-up," says Mylia Christensen, executive director of the organization.
Health Improvement Collaborative of Greater Cincinnati runs an all-voluntary public reporting site, YourHealthMatters.org, which includes data on the performance of primary care practices on composite measures of diabetes and cardiovascular care as well as colon cancer screening rates—areas identified as in need of improvement. The site also includes data comparing hospitals on the process-of-care and patient experience measures reported on the Centers for Medicare and Medicaid Services' (CMS) Hospital Compare website. The group plans to use the Medicare data to round out its public reports and to facilitate its involvement in the Comprehensive Primary Care Initiative, a Center for Medicare and Medicaid Innovation–funded initiative that aims to improve care coordination and prevention.
Kansas City Quality Improvement Consortium assesses primary care practices on measures of patient experience and selected quality measures (e.g., for asthma and diabetes treatment) on its public reporting site, QualityHealthTogether.org. It also compares hospitals on measures of care processes, patient experiences, outcomes, and procedure costs reported on Hospital Compare. It plans to use the Medicare data to supplement its efforts to measure quality at the physician group level, particularly in areas such as treatment for low back pain and diabetes care, and by focusing more attention on variation in costs. Catherine Davis, the group's president and CEO, said that CMS has been helpful during the application process by providing technical assistance and streamlining the process. Eventually, the group hopes to assemble an all-payer database to report costs.
Maine Health Management Coalition Foundation operates GetBetterMaine.org, a site comparing physician practices, by type (adult care, pediatrics, cardiology, or orthopedics) on measures of safe and effective care. The site also compares hospitals on measures of safety, quality, and patient experiences drawn from Hospital Compare, the Leapfrog Group, and other sources. Among other things, the group plans to use the Medicare data to create reports comparing costs and resource use among physician practices and systems.
HealthInsight New Mexico is the first quality improvement organization to receive provisional approval to participate in the qualified entity program. HealthInsight New Mexico will incorporate the Medicare data from CMS with the claims data provided voluntarily by private health plans and the state's Medicaid program as well as federally reported data received from the Indian Health Service. The previously collected data captures the performance of medical groups in the state's most populous county on measures of ambulatory care quality, including prevention and adherence to best practices for diabetes care. The group is also reporting selected cost and quality indicators for hospital care. These performance measures are public reported on a site that was created as part of the group's participation in the Robert Wood Johnson Foundation's Aligning Forces for Quality initiative. In the next year, HealthInsight plans to expand this reporting to the metropolitan statistical area (or four-county area) and then, over time, expand its public reporting to capture the performance of providers statewide.
California Healthcare Performance Information System plans to combine Medicare claims data with similar data reported voluntarily by three large private insurers in the state and enhance its reporting for consumers first on the performance of ambulatory care providers in early 2014, and later on resource use and hospital care. The first report may include up to 20 quality measures, capturing both preventive care and chronic disease treatment. Kristy Thornton, senior manager at the Pacific Business Group on Health (which staffs the program), says the addition of Medicare claims will add three million lives to the number it has to assess physician performance. "It gives us a more complete picture for a given physician and it also allows us to reliably score more physicians," she says.
Pittsburgh Regional Health Initiative will combine Medicare's fee-for-service claims data with claims data it obtains voluntarily from commercial payers in order to launch quality improvement initiatives and understand recurrent problems such as unnecessary hospital readmissions. It has not yet created public performance reports, but plans to pursue what Keith Kanel, M.D., chief medical officer of the Jewish Healthcare Foundation (which leads the Pittsburgh Regional Health Initiative), calls the "Holy Grail" of data analysis: total cost of care. "We want to look at all the costs of taking care of a population." This will let the group determine, for example, "if you try to lower readmissions, are you driving emergency department costs up? Perhaps those discharged patients end up in someone else's hospital—the hospital that discharged the patient wouldn't know," Kanel says.
*The groups are listed based on the order in which they were designated as qualified entities. |
1 See http://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/NationalHealthExpendData/downloads/highlights.pdf.
2 Section 10332 of the Affordable Care Act instructs the Health and Human Services secretary to make Medicare claims data from Parts A, B, and D (excluding Part C, Medicare Advantage) to "qualified entities" to enable them "to evaluate the performance of providers of services and suppliers on measures of quality, efficiency, effectiveness, and resource use."
3 Forty-eight states mandate reporting of hospital discharge data for all patients—the privately insured, publicly insured, and uninsured.
4 Applicants, which can be public or private groups, also must agree to several conditions for use of the data: a) review of methodology to be used for evaluation; b) use of valid measures, such as those endorsed by the National Quality Forum; c) must combine Medicare claims data with data from other sources; d) must request data for one or more specified geographic areas; e) must include information in aggregate form; f) must be shared with providers before public release; and g) must use the data to produce and make publicly available performance reports on individual providers and suppliers in aggregate form.
5 The Affordable Care Act says that use of "alternative measures" may be permitted if the "Secretary, in consultation with appropriate stakeholders, determines that use of such alternative measures would be more valid, reliable, responsive to consumer preferences, cost-effective, or relevant to dimensions of quality and resource use not addressed by such standard measures."


