Summary: Prices for health care services vary significantly among providers, even for common procedures, and it's often difficult for patients to determine their out-of-pocket costs before receiving care. Some consumer advocates, employers, and health plans are pushing for greater reporting of the prices of health care services as a way to encourage consumers to choose low-cost, high-quality providers and to promote competition based on the value of care. In spite of the challenges, price transparency may be spurred by the growing number of health care consumers who are being required to pay a larger share of their medical bills.
By Martha Hostetter and Sarah Klein
It's no secret that the U.S. health care market is unlike any other market: patients rarely know what they'll pay for services until they've received them; health care providers bill different payers different prices for the same services; and privately insured patients pay more to subsidize the shortfalls left by uninsured patients.1 What's more, prices for health services vary significantly among providers, even for common procedures such as laboratory tests or mammograms, although there's no consistent evidence showing that higher prices are linked to higher quality.2
For these reasons, consumer advocates as well as some employers and health plans are pushing for greater price transparency. They argue that if consumers realized that they could receive high-quality services from lower-cost providers, they would seek them out. This, in turn, could encourage competition among providers based on the value of care—not just on reputation and market share.
Impediments to Price Reporting
There are many challenges to making comparative pricing information available. A September 2011 report from the U.S. Government Accountability Office outlined some of the most significant, including the difficulty of determining in advance the health services any given patient will need.3 The wide variety of insurance benefit structures, a lack of standard formatting for reporting prices, and the difficulty of determining prices when charges originate from multiple providers further complicate these efforts.
Legal hurdles to reporting prices, including contractual obligations that in some cases prevent health plans from disclosing their negotiated rates with providers, are also factors, as are concerns from consumer advocates that making patients more price-sensitive requires significant cost-shifting, which may create financial burdens for lower-income patients.
Even if these challenges could be overcome, there's still the question of whether consumers would use price information to inform their health care decision making. A Congressional Research Service study found that early price transparency initiatives, such as one that required California hospitals to publish their charges, did not led to changes in consumer behavior or pricing.4 One reason may be that many people equate higher costs with higher quality—an assumption that often holds true when shopping for furniture or appliances, but not necessarily in health care. Studies of the costs and quality of care reveal a more nuanced relationship between the two.5
Engagement Approaches
Despite the complications, there is likely to be greater interest in price information from consumers as their cost-sharing responsibilities increase. Researchers have begun to determine the most effective way of engaging and educating them about the relationship between cost and quality data. "It could be counterproductive if quality and cost are not reported effectively [because] people may choose higher-cost providers assuming they are the higher-quality providers," says Judith Hibbard, Dr.P.H., senior researcher at the Institute for Policy Research and Innovation and a professor emerita in the University of Oregon's department of planning, public policy, and management.
Hibbard was the lead author of a recent study that sought to determine how different presentations of cost and quality information affected the likelihood that consumers would make high-value choices.6 The study, which involved 1,421 consumers, found that significant numbers of respondents—though not a majority—viewed higher cost as a proxy for higher quality. This was true even among those with high-deductible health plans that would expose them to a higher share of costs. But when the cost and quality information was reported side by side in an easy-to-interpret format, more respondents made high-value choices. Labels indicating that providers made "appropriate usage" of resources or were "careful with your health care dollars" also led more people to choose high-value providers.
Insurers have been working to make this sort of data more accessible and understandable to consumers. Aetna was one of the first insurers to provide price information to its members. It does so via its Member Payment Estimator, which provides comparative cost estimates for more than 550 common services, taking into account users' specific plan type and remaining deductible. Users are able to look up total out-of-pocket costs for service "bundles," so they are not surprised by, say, separate charges for a colonoscopy, for the facility, and the professional fees.
Health Care Service Corp., the parent company of Blue Cross and Blue Shield plans in Illinois, New Mexico, Oklahoma, and Texas, this month plans to launch a cost estimator tool that reports prices for the individual elements of an episode of care, such as facility costs, surgeon's prices, and costs of durable medical equipment. This disclosure may spur competition within these categories. Other Blues plan will be following a similar approach. Meanwhile, UnitedHealthcare this month launched a price estimator program that enables patients to see the contracted fee schedule for individual providers involved in treating a particular condition. The Web-based program also allows members to see whether their physician has met quality and efficiency standards, as indicated through a star-ranking system.
Private firms are entering the price transparency market as well. Castlight and Change Healthcare, both founded within the past five years, are using proprietary software to analyze claims data to estimate the costs of common medical procedures. The reports also include performance data on various providers, enabling users to take into account both cost and quality. They sell these health care "shopping" tools to self-insured companies and, in the case of Change Healthcare, health plans, which in turn encourage their employees and health plan members to use them to choose providers based on their quality and costs.
The products have only been on the market for a few years, so it is too early to see clear trends in the use of the price information, says Ethan Prater, M.B.A., vice president of products at Castlight Health, who notes that most behavior changes (i.e., switching to lower-cost providers) are for laboratory tests or imaging services—routine procedures with widely varying price tags for which consumers may feel more comfortable comparison shopping than, say, office visits or surgical procedures. "We are already seeing true consumer behavior—not just a flight to the lowest-cost provider," he says. "People seem to be asking: 'What kind of tradeoff do I want to make if I have to make one?'"
Change Healthcare proactively alerts people via text or e-mail if they have an opportunity to save money on routine care or prescription drugs. "We look at consumers' existing claims data and identify opportunities for savings," says Doug Ghertner, the company's president. A message might say, for example, 'You can save $250 a year on your health care costs,' and then provide instructions about how to look up lower-cost providers. Some of the alerts incorporate principles of behavioral economics such as loss aversion or social norming to prod action: 'Did you know that your peers are spending $500 less than you are on their blood sugar tests?'
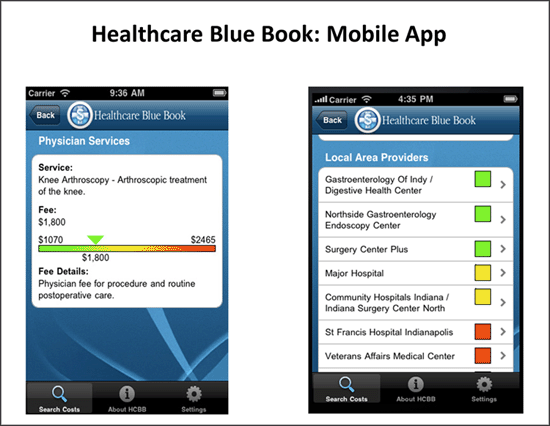
The Healthcare Blue Book, which is freely available to consumers, publishes what it determines to be a "fair price" for various medical services, based on a review of claims data as well as consumer-submitted reports. Employers and insurance companies can pay for access to a version that lists in-network providers ranked by value. Recently, Healthcare Blue Book launched a subscription service for patient-centered medical homes, so that primary care physicians can work with their patients to make referrals to high-quality, lower-cost providers. "This is the best way to make these kinds of decisions, with patients alongside their doctors," says Jeffrey Rice, M.D., J.D., Healthcare Blue Book's founder and CEO. A review of one primary care practice's historical endoscopy orders revealed that most of the procedures were priced at around $1,000—but some were $4,000 and one was over $6,000.
Some have argued that all physicians have a responsibility to become aware of the costs of their services as well as laboratory fees or drug costs, and to help patients explore various treatments.7 Costs of Care, founded by a medical student, seeks to use social media and other communication tools to help physicians understand how the decisions they make affect patients' out-of-pocket costs. And a few providers, including members of the Wisconsin Hospital Association, are making price information available to patients. Some comparative price reports flag providers that refuse to allow insurers to share the claims data that makes price estimates possible—which in itself might be a spur to providers to allow more widespread price reporting.
Price Transparency: One Piece of Cost Control Puzzle
Because consumers have been slow to make use of health care quality reports, it remains to be seen if price information will be enough of a hook to engage them in comparison shopping for care.
Interest may increase as growing numbers of insured Americans pay more of their health care bills, due to greater use of high-deductible health plans and greater cost-sharing in traditional plans.8 One study found these plans led to lower use of name-brand medications, less inpatient care, and lower use of specialists, as well as a troubling reduction in preventive cancer screenings and childhood immunizations.9 In addition to the increasing use of consumer-driven health plans, there are a growing number of "retail" consumers buying coverage for themselves.10 These trends suggest that in the future Americans may become more price sensitive—and more willing to take cost into consideration when seeking care.
"As Americans have been called on to pay more for essential and non-essential services, the evidence has shown that they spend less on both," says A. Mark Fendrick, M.D., director of the University of Michigan Center for Value-Based Insurance Design. "There's strong evidence that small price differentials matter—even a $1 difference in a drug co-pay can lead to behavior change."
Some innovative employers are seeking to use value-based insurance designs to engage their employees in making high-value purchases. Delhaize Group, the parent company of more than 1,000 supermarkets on the East Coast including the Food Lion chain, reduces coinsurance from 40 percent to 20 percent for employees willing to undergo minimally invasive procedures in place of more invasive alternatives. The company also offers to eliminate copayments and pay travel expenses for employees willing to get hip and knee replacements (and soon cardiac and back procedures) in certain facilities in other markets where costs are lower and quality higher. The program works well until patients meet their deductible for the health plan. "Once you get to your coinsurance level and it's paid at 100 percent, we seem to see a slowdown in the uptake of medical tourism," says Joanne Abate, director of health and wellness strategy for the company.
Delhaize also places "wellness professionals" in its retail locations in Maine (and soon its larger markets in North Carolina) to help employees navigate the health care system. "It gives them an opportunity to really get to know people and see what we can do to help them seek the right care at the right time in the right place," Abate says.
Such education may be particularly important for patients with low health literacy, or those faced with serious illnesses, as they weigh their treatment options. Once patients start to look into health care prices, they may also become engaged in exploring the quality and safety of their care as well. "In our experience, when patients don't ask about prices, they don't ask about quality either," says Healthcare Blue Book's Rice. "When they start to become consumers [by comparing prices], they start to ask good questions about quality too."
Ultimately, this kind of health care consumerism might be part of a generational shift. "Young people—who use their phones to choose restaurants and buy airplane tickets—might be predisposed to use price transparency tools," says Brent Parton, director of health policy and programs at SHOUTAmerica, a nonprofit aimed at engaging young people in health care system reform. But, he says, price information must be made available at "teachable moments," such as when people are seeking out routine or planned services, and must be integrated into their health care experiences (e.g., through mobile apps or as part of physician visits). "Health care data is not following us as much as it should be; the onus can't be on the consumer to dig it up," Parton says.
SIDEBARState and Federal Policies Promoting Price Transparency Legislators in more than 30 states have proposed or are pursuing legislation to promote price transparency, with most efforts focused around publishing average or median prices for hospital services.1 Some states have already have price transparency policies in place.2 For example, using its all-payer claims database New Hampshire publishes information about total and out-of-pocket costs. California requires hospitals to give patients cost estimates for the 25 most common outpatient procedures. The state's Office of Statewide Health Planning and Development also runs a "Common Surgeries and Charges Comparison" site, which posts median charges per hospital stay for common, elective inpatient procedures—searchable by year, procedure, county, and city. Pending legislation would require California hospitals to publicly disclose all charges, including physician and laboratory fees, for certain procedures. Texas requires providers to disclose price information to patients upon request. Florida's www.FloridaHealthFinder.gov enables consumers to view the range of prices charged for various procedures, alongside quality-of-care ratings, mortality rates, infection rates, and other measures for hospitals, surgery centers, nursing homes, and hospice centers in the state. Massachusetts' Health Care Quality and Cost Council is developing strategies to promote consumer engagement in seeking high-value care through promotion of medical homes and shared decision-making. On a federal level, the Affordable Care Act requires hospitals to publish and annually update a list of standard charges for their services. Starting in 2014, the health insurance exchanges will require participating health plans to create Web sites or other communication tools to enable consumers to look up their expected out-of-pocket costs for specific services under the plans. Three bills have been introduced in Congress to promote price transparency, including H.R. 4700: Transparency in All Health Care Pricing Act of 2010, which would require physicians, pharmacies, and insurers to publicly disclose the prices of the services and products they provide.
1 A. D. Sinaiko and M. B. Rosenthal, "Increased Price Transparency in Health Care—Challenges and Potential Effects," New England Journal of Medicine, 2011 364(10):891–4. |
1 In this article, "prices" refers to consumers' out-of-pocket costs as well as the amount paid by an insurer on their behalf. Understandably, consumers are mainly interested in what they will have to pay, and therefore most price transparency efforts attempt to distinguish between total prices (the actual charges by hospitals and other providers) and consumers' out-of-pocket costs.
2 One analysis found considerable price variation for common preventive services: 755 percent cost variation for diabetes screenings (from $51 to $437); 264 percent variation for Pap smears (from $131 to $476); and 132 percent cost variation for colonoscopies (from $786 to $1,819) over a 12-month period. Since the Affordable Care Act mandates these preventive screenings come at no cost to individuals, the costs are borne by plan sponsors. Healthcare Transparency Index, "Affording the Affordable Care Act: Engaging Employees in Finding Lower-Cost Preventive Care," March 2012, Change Healthcare. Another analysis found that hospital charges for appendicitis in California hospitals ranged from $1,529 to a high of $182,955. R. Y. Hsia, A. H. Kothari, T. Srebotnjak et al., "Health Care as a "Market Good"? Appendicitis as a Case Study," Archives of Internal Medicine, published online April 23, 2012. One analysis found that U.S. spending on health care could be reduced by $36 billion a year if the 108 million Americans with employer-sponsored coverage comparison shopped for 300 common medical procedures. B. Coluni, "Save $36 Billion in U.S. Healthcare Spending Through Price Transparency," Thomson Reuters, February 2012. Several studies have found that higher costs do not equate with higher quality. See Note 5.
3 "Meaningful Price Information Is Difficult for Consumers to Obtain Prior to Receiving Care," U.S. Government Accountability Office, Sept. 23, 2011, http://www.gao.gov/products/GAO-11-791.
4 D. Andrew Austin and J. G. Gravelle, "Does Price Transparency Improve Market Efficiency? Implications of Empirical Evidence in Other Markets for the Health Sector," CRS Report for Congress, July 24, 2007.
5 See, for example: Investigation of Health Care Cost Trends and Cost Drivers, January 2010, Office of Massachusetts Attorney General; A. K. Jha, E. J. Orav, A. Dobson et al., "Measuring Efficiency: The Association of Hospital Costs and Quality of Care," Health Affairs, May/June 2009 28(3):897–906; and K. E. Joynt and A. K. Jha, "The Relationship Between Cost and Quality: No Free Lunch," Journal of the American Medical Association, March 2012 307(10):1082–83.
6 J. H. Hibbard, J. Greene, S. Sofaer et al., "An Experiment Shows That a Well-Designed Report on Costs and Quality Can Help Consumers Choose High-Value Health Care," Health Affairs, March 2012 31(3):560–68.
7 See N. Vailas, "Cost-Consciousness: An Essential Competency for Physicians," http://healthcaretransparencynow.com/?p=434, and the American College of Physicians Code of Ethics, http://www.acponline.org/clinical_information/journals_publications/ecp/mayjun99/tavistock.htm.
8 According to a Kaiser Family Foundation survey, from 2006 to 2010, the percentage of covered workers enrolled in high-deductible health plans increased from 4 percent to 13 percent, and the percentage of covered workers with a deductible of $1,000 or more for single coverage almost tripled, from 10 percent to 27 percent. The Kaiser Family Foundation and Health Research & Educational Trust, Employer Health Benefits 2010 Annual Survey (2010). In 2012, 73 percent of employers will be offering at least one consumer-directed health plan, most commonly a high-deductible health plan attached to a health savings account, see http://pnhp.org/blog/2011/08/19/employers-continue-to-shift-health-care-costs-to-employees/.
9 A. M. Haviland, N. Sood, R. McDevitt et al., "The Effects of Consumer-Direct Health Plans on Episodes of Health Care," Forum for Health Economics and Policy, Sept. 2011 14(2):1–27.
10 M. Dick Tocknell, "Health Plans Must Prep for Consumer-Oriented Business Model," Nov. 9, 2011, HealthLeaders Media.


