Maintaining continuity in patients' medical care is especially critical following discharge from the hospital. For elderly patients with multiple chronic conditions, this "hand-off" period takes on even greater urgency: research shows that one-quarter to one-third of these patients have to return to the hospital for problems that could have been prevented. With support from the Fund, Mary Naylor, R.N., Ph.D., F.A.A.N., a professor of gerontology at the University of Pennsylvania School of Nursing, will assess the feasibility of implementing a post-acute care model in which advanced practice nurses follow high-risk patients from hospital to home. Aetna, one of the nation's largest insurance carriers, will test this care as a covered service in part of its Mid-Atlantic market. We asked Dr. Naylor about this promising model and how it came to be.
How did this problem—the lack of continuity in care from hospital to home—come to your attention?
Mary Naylor: In the mid-1980s, I was working for the U.S. Senate Committee on Aging when the Medicare Prospective Payment System was put into place, which was a major change in how hospital care was financed. We began to see that hospital stays were getting shorter, and that this was having a negative effect on post-discharge medical outcomes for many elders. There wasn't a safety net in place to help patients and families make the difficult transition to home. It became clear to me that patients' emotional and physical health, their medication regimens, and their strategies for coping over the long term needed to be managed better.
What are some of the problems that arise when elderly patients are discharged?
Naylor: There are huge issues around communication and coordination of care when multiple players are involved—even within the hospital system. And when people being discharged are handed off to yet another group of providers, communication gets even more challenging. What's more, these patients are exceedingly vulnerable at the time of discharge. They've just been dealing with a traumatic event. It's hard to give patients and their families all the information they need to manage successfully at home.
So how do advanced practice nurses create a plan for coordinating care?
Naylor: The nurses work with patients and their families to create a discharge plan, and then follow them for a period after discharge to implement it. The focus isn't just on the patient's heart failure or diabetes. Rather, it's a soup-to-nuts plan, driven by priority issues but with a long-term view. The nurses provide patients and their families with the knowledge and management skills necessary to prevent poor outcomes and avoid the need for acute care. They also pay attention to often-neglected areas like depression, which is common among elders with chronic illness but too often goes unrecognized.
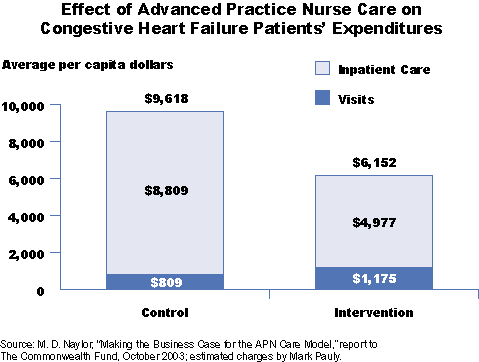
Tell us what you found in the early clinical trials funded by the National Institute of Nursing Research.
Naylor: Elderly patients with heart failure have the highest hospitalization rate among all adults. In the most recent trial, we saw that a comprehensive intervention, delivered by advanced practice nurses in the hospital and followed up at home, substantially reduced repeat hospitalizations for these patients. It's not simply a matter of managing their heart condition better, it's about managing all the accompanying problems, like diabetes and hypertension, as well.
What barriers remain in getting this system implemented?
Naylor: There's no explicit, direct reimbursement for care coordination services that span hospital and home. In this country, we tend to deliver care in independent silos, with little attention to the gaps in between. But working with a major insurer like Aetna is a big step forward. Not only will they be paying for this care, they're helping to translate the model from research into practice.


