Children's Special Needs
Medicaid's Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) program ensures that low-income children receive not only preventive and primary health care, but comprehensive coverage for serious conditions that affect growth and development. Low-income, publicly insured children are more likely than privately insured children to have special health care needs, such as developmental delays, learning disabilities, or attention deficit hyperactivity disorder (Figure 1).1
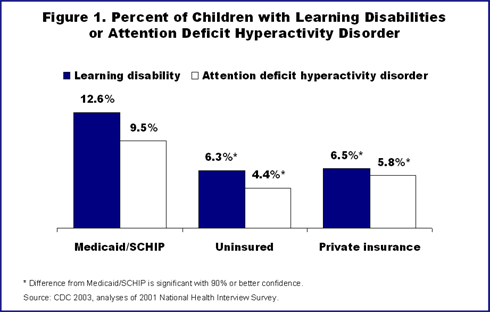
Low-income children also are more likely to be in poorer health overall. For example, extreme prematurity (birthweight less than 1,000 grams),2 which is more common in poor communities, is associated with visual and hearing disabilities, asthma, poor motor skills, emotional disorders, and other problems (Figure 2).3 For these children, Medicaid is an essential source of coverage for preventive and special developmental services.4
Commercial Insurance Coverage5
The commercial market operates differently from Medicaid. Private insurers follow principles of risk avoidance and seek to limit situations where they depart from actuarially based, standardized, population risk norms with respect to coverage. Private insurance is designed for a healthy population, which results in strict coverage limits, including exclusion of most or all developmental disabilities.
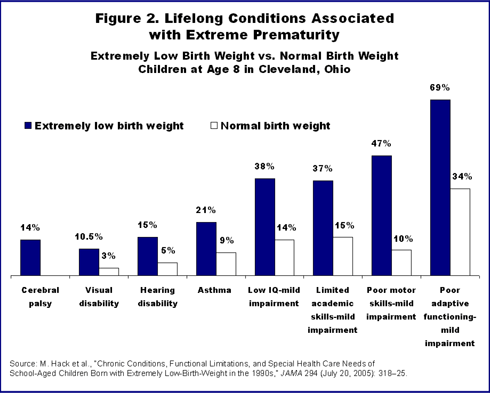
Medicaid and commercial insurance also differ on the definition of medical necessity. Commercial plans tend to limit "necessary care" to that which diagnoses or treats illnesses or injuries and is needed to restore normal functioning. These rules can exclude the types of treatments needed by children with long-term developmental disabilities linked to prematurity and other conditions, such as cerebral palsy. EPSDT, on the other hand, ties medical need to children's individual conditions and requires coverage consistent with the goal of ensuring healthy child development.
Commercial Coverage More Restrictive
Table 1 compares coverage rules used in commercial insurance to those used in Medicaid for children.
Table 2 compares the content of child health coverage offered in the Federal Employees Health Benefits Program (FEHBP) Blue Cross Blue Shield Standard Option to the coverage available in EPSDT. FEHBP is considered generous when it comes to benefits; however, when comparing EPSDT to FEHBP, there are numerous differences in coverage. Unlike FEHBP, EPSDT was designed to meet the needs of children rather than adults to promote health and development.
Table 1. A Comparison of Commercial Insurance and Medicaid | ||
| Commercial insurance | Medicaid | |
| Preexisting condition exclusions | Permitted within HIPAA limitations | Prohibited |
| Categories of covered benefits | Limited to "major medical" care with certain preventive benefit additions to limit risk exposure | All service classes within federal medical assistance definition are mandatory for children. Broad coverage includes care related to special health care needs. |
| Benefit definitions | Insurer's discretion | Defined by federal law |
| Limitations and exclusions | Typically included | No limits where care is medically necessary and service falls under definition of medical assistance |
| Patient cost-sharing | Left to the discretion of the insurer and purchaser | Prohibited for children under age 18 |
| Medical necessity | Left to the discretion of the insurer | Preventive pediatric standard |
| Source: S. Rosenbaum, A. Markus, C. Sonosky et al., Policy Brief #2: State Benefit Design Choices Under SCHIP-Implications for Pediatric Health Care (Washington, D.C.: George Washington University, 2001). |
Table 2. A Comparison of Benefits for Infants and Young Children: Medicaid and the FEHBP Standard Option Blue Cross/Blue Shield Plan | ||
| Benefit | Medicaid | FEHBP |
| Developmental assessment | Covered | Limited to "healthy newborn visits," "routine screening," "routine physical examinations," "neurological testing," and initial examination of a newborn needing "definitive treatment," when the infant is covered under a family enrollment. |
| Anticipatory guidance | Covered | Not explicitly covered |
| Physical, speech, and related therapies | Covered without limitations other than medical necessity; no "recovery" requirements; therapy covered for conditions identified through early intervention and child care programs. | Limited to inpatient coverage. "Maintenance therapy" expressly excluded. Also excluded are "recreational and educational" therapy and "any related diagnostic testing except as provided by a hospital as part of a covered inpatient basis." All services billed by schools or a member of school staff are excluded. |
| Hearing services | Covered without limitations, including tests, treatment, hearing aids, and speech therapy related to hearing loss and speech development. | Testing covered only when "related to illness or injury." Routine hear-ing tests excluded other than as standard part of "routine" screening for children; hearing aids excluded along with testing and examinations for the prescribing or fitting of hearing aids. |
| Eye examinations and eyeglasses | Covered without limitations, as medically necessary. | One pair of eyeglass replacement lenses or contact lenses to "correct an impairment directly caused by a single instance of accidental ocular injury or intraocular injury;" eye examinations for specific medical conditions; nonsurgical treatment for amblyopia and strabismus from birth through age 12. Eyeglasses and routine eye examinations specifically excluded, as are eye exercises, visual training, and orthoptics except in connection with the specific diagnosis of amblyopia or strabismus. |
| Durable medical equipment (DME) | Covered without limitations, as medically necessary. | Certain DME covered but only if prescribed for the treatment of "illness or injury." |
| Home nursing | Covered without limitations, as medically necessary; home visits can cover health educators, therapists, health aides, and others. | Covered for two hours per day, 25 visits per year, when furnished by a nurse or licensed practical nurse and under a physician's orders. |
| Sources: S. 1905(r) of the Social Security Act, 42 U.S.C. 1396d(r); Part 5, Section 5122 of the State Medicaid Manual; OPM, FEHBP Blue Cross and Blue Shield Service Benefit Plan, 2005. |
1 L. Ku and S. Nimalendran, Improving Children's Health: A Chartbook About the Roles of Medicaid and SCHIP (Washington, D.C.: Center on
Budget and Policy Priorities, 2004).
2 M. Hack, H. G. Taylor, D. Drotar et al., "Chronic Conditions, Functional Limitations, and Special Health Care Needs of School-Aged
Children Born with Extremely Low-Birth-Weight in the 1990s," Journal of the American Medical Association July 20, 2005 294(3):318–25.
3 Ibid.
4 A. Markus, S. Rosenbaum, A. Stewart et al., How Medical Claims Simplification Can Impede Delivery of Child Developmental Services (New York:
The Commonwealth Fund, Aug. 2005).
5 S. Rosenbaum, A. Markus, C. Sonosky et al., Policy Brief #2: State Benefit Design Choices Under SCHIP—Implications for Pediatric Health Care (Washington, D.C.: George Washington University, 2001).


