Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) is a required benefit for all "categorically needy" children (e.g., those who have poverty-level income, receive Supplemental Security Income, or receive federal foster care or adoption assistance). EPSDT's rules reflect the greater health needs of low-income children, as well as children whose special health needs qualify them for assistance. Low-income children covered by public insurance are more likely to be born at low birthweight, which increases the risk for lifelong disability,1 and more likely to be in fair or poor health, to have developmental delays or learning disorders, or to have medical conditions (e.g., asthma) requiring ongoing use of prescription drugs.2 Serious health conditions affect 80 percent of children in foster care. For these children, Medicaid is essential to ensure access to preventive and developmental services.3
Medicaid and Child Development
In 1965, Congress enacted Medicaid, extending medical benefits to all children in households receiving Aid to Families with Dependent Children. The original legislation also gave states the option of extending coverage to all very poor children under age 21, regardless of welfare status.
In 1967, Congress broadened Medicaid for children because of evidence of widespread disability among military recruits and preschool children in Head Start. Many of the disabilities were conditions whose effects could have been ameliorated through early prevention.4 Particularly influential was the 1964 report One Third of a Nation, which showed pervasive health problems among young military draftees that could have been avoided had proper care been provided in childhood.4 EPSDT was thus added to expand coverage for children beyond adult limits and to ensure availability of treatments for conditions affecting growth and development. In 1989, EPSDT was further broadened to ensure access to all treatments within the federal definition of "medical assistance." EPSDT thus focuses on comprehensive care that treats potentially disabling conditions as early as possible.
Table 1. Medicaid and Children: A Timeline | |
| 1965 | Medicaid is enacted, mandating coverage for children receiving AFDC and making coverage optional for other very poor children. |
| 1967 | Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) benefit is added to promote healthy child development and ameliorate conditions that disable children. |
| 1972 | Supplemental Security Income (SSI) is enacted, providing cash assistance and Medicaid to children with disabilities. |
| 1984–1990 | Through incremental steps, Congress expands Medicaid to cover all poverty-level pregnant women and children born after September 30, 1983. States are given options to extend coverage to low-income children and women (i.e., with incomes slightly above poverty). |
| 1989 | The Omnibus Budget Reconciliation Act of 1989 expands EPSDT to ensure that all treatments allowed under the definition of "medical assistance" are covered in all states in response to evi-dence of limited coverage for children with mental and developmental disabilities. |
| 1997 | The Balanced Budget Act of 1997 established the State Children's Health Insurance Program (SCHIP), which makes EPSDT an optional service for children covered under separately administered SCHIP plans. |
| Source: Kaiser Family Foundation, State Health Facts, http://www.statehealthfacts.org (accessed July 11, 2005); C. Mann, D. Rowland, and R. Garfield, Historical Overview of Children's Health Care Coverage, http://www.futureofchildren.org (accessed July 5, 2005). |
EPSDT and Managed Care
Most children in Medicaid are in managed care and remain entitled to the full EPSDT benefit. In some states, managed care plans are responsible for providing all EPSDT services. In others, the Medicaid agency may be responsible for covering supplemental services beyond those listed in the managed care agreement. Certain children, such as those in foster care, may receive all of their coverage on a fee-for-service basis.
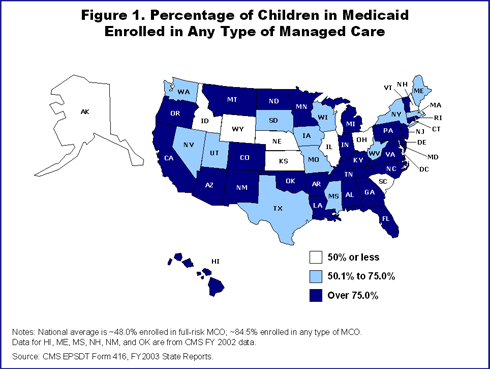
Table 2. The EPSDT Benefit |
| MEDICAL |
Periodic and "as needed" screening services that include:
|
| Vision services (assessment, diagnosis,and treatment, including eyeglasses) |
| Hearing services (assessment, diagnosis, and treatment, including hearing aids and speech therapy |
| Dental services preventative, restorative, and emergency care beginning not later than age 3 or earlier if medically indicated) |
| Necessary health care diagnosis services, treatment, and other measures classified as medical assistance to correct or ameliorate defects and physical and mental health conditions discovered by screening services, whether or not such services are covered under the state medical assistance plan. These services include:
|
| "Preventive" standard of medical necessity: recognized in agency implementing guidelines and a long line of judicial decisions, which recognizes the prevention of disabilities as the standard of coverage and emphasizes attainment of growth and development. |
| ADMINISTRATIVE |
|
1M. Hack, H. G. Taylor, D. Drotar et al., "Chronic Conditions, Functional Limitations, and Special Health Care Needs of School-Aged Children Born with Extremely Low-Birth-Weight in the 1990s," Journal of the American Medical Association 2005 294(3):318–25.
2 L. Ku and S. Nimalendran, Improving Children's Health: A Chartbook About the Roles of Medicaid and SCHIP (Washington, D.C.: Center on Budget and Policy Priorities, 2004).
3 A. Markus, S. Rosenbaum, A. Stewart et al., How Medical Claims Simplification Can Impede Delivery of Child Developmental Services (New York: The Commonwealth Fund, 2004).
4Special Message to the Congress Recommending a 12-Point Program for America's Children and Youth, Feb. 8, 1967. Transcript available at: http://www.presidency.ucsb.edu/ws/index.php?pid=28438&st=Medicaid&st1=Johnson. (See: S. Rosenbaum et al., National Security and U.S. Child Health Policy: The Origins and Continuing Role of Medicaid and EPSDT, Policy Brief [Washington, D.C.: George Washington University, 2005].)


