Watch a Medscape video editorial by Karen Davis on payment reform. (Sign-in is required.)
By Karen Davis
Any discussion of payment reform in health care raises a fundamental question: What do we want out of our health system? Our current fee-for-service system reimburses "inputs"—hospital stays, physician visits, and procedures—rather than the most appropriate care over an episode of illness or over the course of a year. Fee-for-service payments create incentives to provide more and more services, even when there may be better, lower-cost ways to treat a condition. What most of us want is a health system that offers the best possible outcomes at an affordable price.
Changing the Incentives
The unfortunate consequences of fee-for-service play out clearly in hospitals. As hospital patients, we naturally want safe and effective care—and to avoid an unnecessary repeat stay. But there are no incentives for hospitals to ensure we won't come back through their doors, despite compelling evidence that appropriate discharge instructions, home visits, and other follow-up care can help reduce hospital readmissions.
Similarly, in primary care settings, there are few financial incentives to avoid hospitalizations through preventive measures and high-quality, ongoing care for chronic conditions. Chronic care management systems, in which nurses reach out to patients to check symptoms and adherence with recommended treatments, can be more cost effective than emergency room visits or doctor's office care. But most insurance plans don't cover these services, so providers that offer them have to cover the costs themselves.
The potential for lowering health costs by reducing the number of hospital stays is significant. As demonstrated by the Fund's State Scorecard on U.S. Health System Performance, if all states reached the low levels of potentially preventable admissions and readmissions achieved in the five best-performing states (Hawaii, Utah, Washington, Alaska, and Oregon), hospitalizations among Medicare beneficiaries could be reduced by 30 to 47 percent and save Medicare $2 billion to $5 billion each year.
The Way Forward
Still, it's not realistic to tell hospitals and doctors that they must improve quality if by doing so they are likely to lose money. Fund-supported research into the "business case" for quality has shown that, even in programs that do save money, the savings aren't likely to accrue to the physician or hospital that implements the changes. And some patients and physicians are concerned that there will be an incentive to skimp on care if we move away from fee-for-service payments.
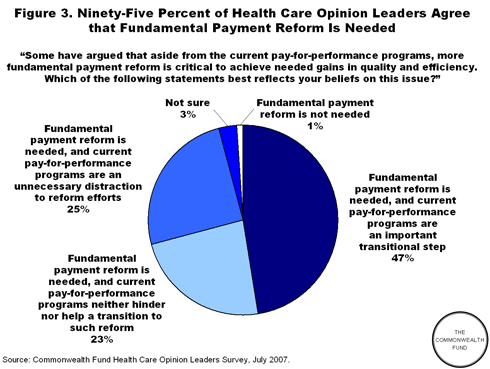
Despite these concerns, many experts, as well as those delivering health care services, support change in the payment system. According to the Commonwealth Fund Health Care Opinion Leaders Survey on Quality and Safety of Care, nearly all respondents believe fundamental payment reform is needed, with nearly half saying pay-for-performance is an important transitional step. Experiments with pay-for-performance methods are yielding promising results—and a common approach across public programs and private plans would reduce paperwork for doctors and hospitals.
Some reforms are already taking shape. To create incentives to reduce readmissions, one hospital group, Geisinger Health System of Pennsylvania, on whose board of directors I serve, now charges a flat fee for surgery, including a "warranty" for 90 days of follow-up treatment. And last month, the Centers for Medicare and Medicaid Services (CMS) announced that Medicare will no longer reimburse health care providers for the extra costs incurred when beneficiaries contract certain hospital-acquired infections. CMS also will withhold payment for other complications considered preventable, including injuries resulting from falls, bed sores, and objects left in patients during surgery.
A recent Fund report by Harold D. Miller, strategic initiatives consultant for the Pittsburgh Regional Health Initiative and the Jewish Healthcare Foundation, offers options for addressing problems with existing pay-for-performance programs and creating a payment system that will improve the quality of health care and reduce (or slow the growth in) costs. According to the report, payment reform needs to answer questions such as: What basic method should be used to compensate providers for care—episode-of-case, fee-for-service, or capitation? Should payments for multiple providers be bundled together? What are appropriate payment levels? Should there be performance incentives for providers? Should there be incentives for patients?

One approach would be to move the health system toward blended payments, in which payment for hospitals and physicians includes fee-for-service payments, per-patient payments, and performance bonuses. Hospitals receiving a per-patient episode fee would be encouraged to provide transitional care to reduce the risk of re-hospitalizations, and physician practices would be encouraged to set up their offices as medical homes, which patients could join to receive coordinated, accessible care. Medical homes, in turn, should lead to improved chronic care management, ensure patients receive preventive care, and offer accessible, off-hours care. Medical homes could also reduce the number of emergency room visits.
Experimentation with different payment reforms is clearly needed, and this can be accomplished through various types of demonstrations. If Medicare and Medicaid provide leadership here, more private insurers would be encouraged to follow suit. Once new payment methods are in place, we can observe their effects, see what works best, and give providers time to learn how to improve through them. We must start testing different approaches now to begin to rein in costs—and to make sure we are paying for the best available care, not just more services.
As always, I'm interested in your feedback. Please e-mail me at [email protected].
Written with the assistance of Christine Haran and Martha Hostetter.


