The Commonwealth Fund commissioned the Lewin Group, a health care policy research and management consulting firm, to estimate the effect of this bill on stakeholder and health system costs and the projected number of people the bill would insure. The Fund also commissioned Health Policy R&D, another health policy firm, to create detailed comparative analysis of the bill as well as summaries. The analysis appears in the Appendix Table.
The Commonwealth Fund contracts with The Lewin Group to provide the estimates in this report of the impact and costs of health reform options, based on that firm's health system modeling capacity. The Lewin Group is a wholly owned subsidiary of Ingenix, which is in turn a subsidiary of UnitedHealth Group. Through extensive due diligence examinations, the Fund has ascertained that The Lewin Group modeling team functions as an independent analytic group without owner interference, and that data security and confidentiality protections are in place. The Lewin Group has complete responsibility for the reliability and integrity of its estimates.
Representative Stark's "Medicare Early Access Act of 2005" (H.R. 2072)
Excerpted from: S. R. Collins, K. Davis, and J. L. Kriss, An Analysis of Leading Congressional Health Care Bills, 2005–2007: Part I, Insurance Coverage (New York: The Commonwealth Fund, March 2007).
Medicare Buy-In for Older Adults
Older adults ages 55–64 without coverage through an employer would be allowed to buy in to Medicare under the "Medicare Early Access Act of 2005" (H.R. 2072) introduced in May 2005 by Representative Stark (D–Calif.).
Medicare Early Access Act of 2005 (for more detail see Table 1)
Overall Approach: Older adults who do not currently have coverage through an employer (other than COBRA or retiree health benefits), a public insurance program, or a public employee's health insurance program would be allowed to enroll in Medicare.
Benefits Package: Same as that available to Medicare beneficiaries. Employers providing retiree health benefits could provide wraparound benefits.
Cost-Sharing: Premiums based on national per-capita cost of services to older adults 55–64, with premiums varying by age; cost-sharing is same as in Medicare.
Affordability: Advanceable, refundable tax credits for up to 75 percent of premium cost. Employers that offer retiree benefits could pay the remaining 25 percent.
Financing: Medicare program would finance the coverage of those who become newly eligible.
Lewin Group Estimates of Coverage and Costs in 2007
Under the "Medicare Early Access Act"
Number of uninsured covered ages 55–64 3.5 million
Remaining uninsured
Ages 55–64 1.3 million
All uninsured 44.3 million
Net change in costs in 2007
Total health spending $4.9 billion
Federal $26.9 billion
State and local ($2 billion)
Employers ($9.4 billion)
Household ($10.6 billion)
What the Estimates Mean
There are an estimated 29.5 million people ages 55–64 in 2007. Of those, an estimated
4.8 million are uninsured, 1.5 million purchase insurance through the individual market, and 2.7 million are early retirees and receive retiree health benefits through their employer (Figure 1). Under a Medicare buy-in, The Lewin Group estimates that 3.5 million currently uninsured older adults would buy in to Medicare, all of the 1.5 million who are currently buying coverage in the individual market would buy in, and 2.1 million early retirees with employer health benefits would buy in, with wraparound coverage from their employer.
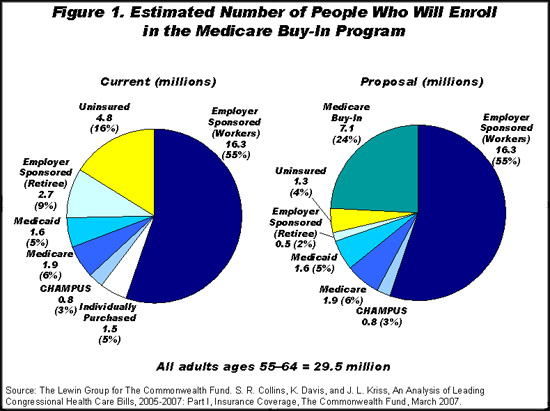
The cost to the federal government of the 75 percent premium subsidy for those who buy in to Medicare is estimated at $26.9 billion in 2007. State and local governments might see savings of approximately $2 billion in that year because of a decline in uncompensated care at government-funded safety-net institutions. Employers who provide retiree health benefits would save $9.4 billion as a result of retirees buying into the program. And savings on premiums and out-of-pocket costs would reduce family spending on health care by $10.6 billion.
National spending on health care overall is estimated to increase by a net $4.9 billion in 2007 as a result of the program. Health care use would rise, increasing spending by $6.4 billion (data not shown). But the costs of insurance administration, because of Medicare's lower administrative costs relative to the individual and employer markets, are estimated to decline by $2 billion.
Table 1. Analysis of the Medicare Early Access Act of 2005
Bill name |
Medicare Early Access Act of 2005 |
Bill number(s) |
H.R. 2072 |
Bill sponsor(s) |
H.R. 2072 is sponsored by Representative Stark and has 112 cosponsors.
|
Latest Congressional action |
H.R. 2072 was referred to the House Waysand Means Subcommittee on Health on May 16, 2005, the Education and Workforce Subcommittee on Employer-Employee Relations on May 20, 2005, and the Energy and Commerce Subcommittee on Health on May 23, 2005.
|
Basic structure of coverage expansion |
Allows certain near elderly persons to buy in to Medicare. This coverage expansion would be financed fully through premiums, although individuals could claim a partial federal tax credit for the premiums. Enrollees could claim a refundable tax credit for up to 75 percent of the premium amount. The tax credit could be claimed in advance (on a monthly basis) or at the end of the year on the individual's federal income tax return. Employers offering retiree benefits could provide wraparound benefits for enrollees in the buy-in program. In addition, employers could pay 25 percent of the Medicare buy-in amount on behalf of retirees. |
Description of eligible participants |
This expansion would target near-elderly individuals who are not eligible for employer-sponsored coverage or coverage through a federal health program.
|
Eligibility criteria |
Individuals 55 to 64 years of age who would be eligible for Medicare Part A if they were 65 years of age would be able to enroll in the Medicare Early Access program as long as they are not eligible for:
· Medicare, Medicaid, Federal Employees Health Benefits Program (FEHBP), TRICARE or health benefits provided to active duty military; or · Employer-sponsored health coverage. However, individuals eligible for COBRA or enrolled in a retiree health plan may enroll in the Medicare buy-in program.
|
Benefits |
Enrollees would receive the same benefits available to Medicare beneficiaries. In addition, employers offering retiree benefits could pay for items and services not covered by Medicare.
|
Premium and cost-sharing requirements |
Enrollees would pay premiums, based on the average national per capita cost of providing services to near-elderly persons under this program. Premiums could vary by age. Cost-sharing for covered services would be the same as for other Medicare beneficiaries.
|
Incentives and federal subsidies |
Individuals would be given a refundable tax credit for up to 75 percent of the premium amount. Since the credit would be refundable, the taxpayer would receive the entire amount of the credit regardless of the amount owed in taxes for the year (e.g., if the credit is more than the amount owed by the taxpayer, the taxpayer would receive the remaining amount of the credit in the form of a refund). The tax credit could be claimed at the end of the year when filing the federal income tax return or in advance on a monthly basis. If paid in advance, the Internal Revenue Service (IRS) would pay the Department of Health and Human Services (HHS) directly as a partial payment of the enrollee's premium.
|
Changes to public program(s) |
The bill would permit near-elderly individuals to obtain Medicare benefits. Enrollees in the Medicare buy-in program would not be eligible for Medicaid program services otherwise available to Medicare beneficiaries (e.g., Medicaid long-term care assistance). The annual capitation rate for Medicare Advantage plans (Medicare Part C) would be adjusted to reflect differences in expected costs between near-elderly buy-in enrollees and Medicare beneficiaries.
|
Administration and oversight of the coverage expansion
|
The IRS would administer the tax credit. HHS would administer the Medicare benefits for these enrollees. |
Changes to federal or state oversight of health coverage
|
None specified. |
Financing |
A new, separate trust fund (the Medicare Early Access Trust Fund) would be established to collect premiums and pay for benefits. Coverage expansion would be paid for by a combination of enrollee premiums, general federal revenues (the tax credit), and employer contributions to enrollee premiums.
|
Key implementation dates
|
To be determined (current effective date: January 1, 2006). |
Other key elements of the bill |
Employers offering retiree benefits whose retirees enroll in the program could provide wraparound coverage and pay a portion of the premium (25 percent) on behalf of retirees. The bill would establish limited enrollment periods, as described below: · Initial enrollment would be limited to a four-month period following initial implementation of the bill for eligible individuals; · After the initial enrollment period, individuals who subsequently become eligible would have a limited period of time to enroll (e.g., persons who turn 55 and do not have access to federal or employer-sponsored coverage or who lose access to coverage after age 55). These individuals would be required to enroll within a four-month period. An annual report on the status of the newly created Medicare trust fund would be issued by the trust fund's board of trustees. The General Accounting Office (GAO) would periodically report on the adequacy of the financing of coverage provided under this Medicare buy-in program. The legislation does not address the sale of Medigap policies to enrollees. Currently, federal law does not require insurers to sell Medigap policies to beneficiaries under age 65. Insurers may sell policies to persons under 65 voluntarily (but can charge a higher rate) or because of requirements established by some states.
|


