By Karen Davis and Kristof Stremikis
As President Obama and the new Congress embark on an ambitious agenda to reform the American health care system, the need to develop a national policy to encourage the spread of health information technology (IT) is resurfacing as a key issue. The health care proposals from both the Obama–Biden campaign and Senator Max Baucus (D–Mont.) call for expansion of health IT as a means of facilitating quality reporting and improvement activities, empowering individual patients, and expanding provider access to evidence and clinical decision-support tools. More recently, significant investment in national IT infrastructure was put forward as an integral component of the economic stimulus bill, which aims to expand employment while increasing efficiency and lowering costs in the long run.
Still, modern IT is not a panacea for all that ails health care in this country. Data from high-performance health systems within the United States and throughout the broader international community show that investments in health IT must be supported by other actions, including financial incentives to make a provider case for adoption and use, and standards set by government. IT investments must also be coupled with strong commitments to performance improvement.
The Evidence Base and Business Case for Health Information Technology
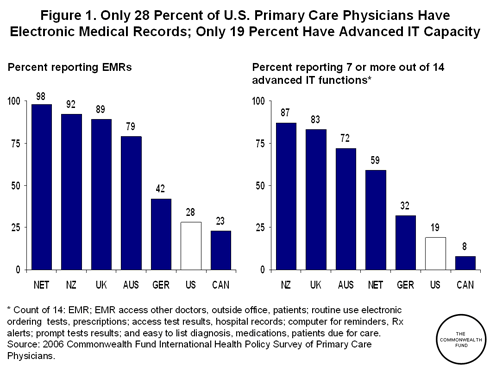
U.S. health providers have been slow to adopt health IT, in part, because of concerns about its value and the costs of implementation. Analysis of the 2006 Commonwealth Fund International Health Policy Survey of Primary Care Physicians demonstrates that the United States has fallen far behind the Netherlands, New Zealand, the United Kingdom, Australia, and Germany on a number of measures related to the utilization of health IT. The contrast between the United States and the Netherlands is particularly stark, with 98 percent of Dutch primary care physicians reporting the use of electronic medical records compared with only 28 percent of their American counterparts. This general pattern persists when examining the prevalence of other IT functions such as electronic prescribing, decision support, and computerized access to test results.
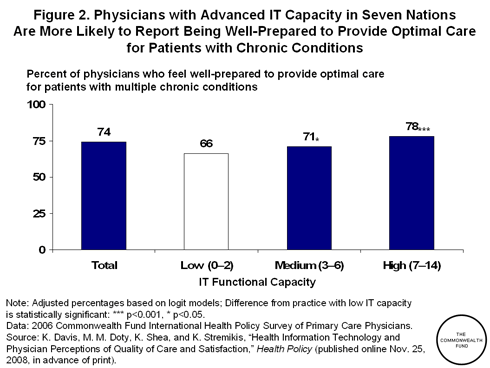
Evidence from the literature demonstrates that investments in health information technology show substantial promise for improving the quality of care that patients receive. Recent analysis of the 2006 Commonwealth Fund Survey of Primary Care Physicians that Commonwealth Fund colleagues and I published recently in the professional journal Health Policy confirms that advances in information technology are making it easier for physicians to provide coordinated, high-quality care by streamlining many crucial tasks, including sending patient reminders, creating disease registries, prescribing and refilling medications, and viewing lab results. Doctors with a high level of health IT functionality were also more likely to think the health system works well and be satisfied with the practice of medicine. In addition, Fund-sponsored work led by Ruben Amarasingham, M.D., M.B.A., of the University of Texas Southwestern Medical Center has shown that hospitals with more advanced information technology capacity have fewer complications and decreased mortality rates.
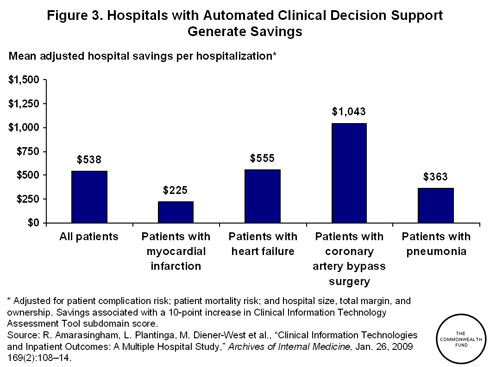
Several studies have also suggested that a business case can be made for the adoption of health IT, both at the facility level and within the health system as a whole. Amarasingham and his colleagues' findings importantly show that utilizing IT to automate test results, order entry, and decision support was not only associated with better quality but also lower average adjusted costs for hospital admissions and lower mean hospital costs for a variety of clinical conditions, including heart failure and coronary artery bypass grafting. Computerized decision support was particularly effective at generating savings. Higher degrees of decision support automation were associated with lower average adjusted costs of $538 for all conditions. If these reductions were realized among the 37 million hospital admissions in the United States in 2005, facilities across the country would stand to save almost $20 billion a year.
The Commonwealth Fund report, Bending the Curve, put the aggregate system-wide savings of promoting health information technology at $88 billion over 10 years. The authors estimated that the cost reductions would result from a lower rate of medical errors, more efficient use of diagnostic testing, more effective drug utilization, and decreased provider costs, among other improvements. Additional savings would likely flow from better care coordination among multiple providers—and improved chronic care management—that would lead to a decrease in provider utilization and better health outcomes. Financial benefits accrue to all payers, with investments in health IT estimated to result in substantial cumulative net savings to all levels of government and households over 10 years and cumulative savings to private insurers after 11 years.
Health Information Technology in High Performance Health Systems
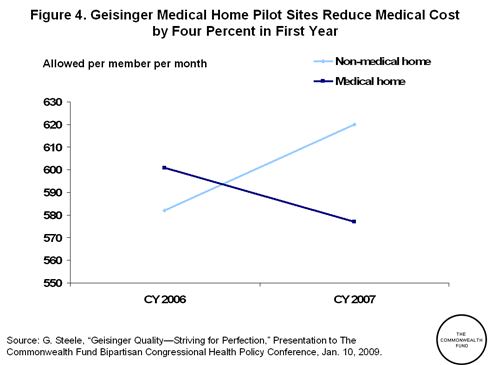
While technology has the potential to improve care, save lives, and reduce cost, data from high performance health systems within the United States and the broader international community show that investments in health IT must be made in conjunction with performance improvement activities. Analysis of Geisinger Health System, a nonprofit integrated delivery network in Pennsylvania on whose Board of Directors I serve, shows that information technology is a crucial component of that organization's efforts to empower consumers and enhance value. Use of electronic health records within Geisinger's ProvenHealth Navigator medical home initiative improved quality while decreasing costs by 4 percent per enrollee during the first phase of implementation. Similarly, utilization of health IT in Geisinger's ProvenCare acute episodic payment program helped decrease readmission rates by 5 percent, while the rate among the Medicare control population increased.
The Geisinger experience shows that realizing the full benefit of electronic health records requires a strategy that leverages technological innovation while simultaneously realigning provider incentives and encouraging greater organization of care delivery. This approach parallels that employed by Kaiser Permanente (KP), where investment in health IT was done concurrent to key changes in care process design and the introduction of a performance-based, patient-centered culture. As a result of these initiatives, more than 2.4 million KP members are now able to check lab results, access health information, and send secure messages to their doctor online. Integrating this functionality with KP's HealthConnect inpatient and outpatient care delivery systems has driven higher quality and better clinical outcomes.
The promulgation of health IT and the establishment of national information exchanges are also key components of high-performance health systems in Denmark and the Netherlands. Upwards of 99 percent of Danish primary care physicians now use electronic health records and e-prescribing. All prescriptions, lab tests, and hospital discharge letters flow through a single electronic portal accessible to patients—and with the permission of patients—to physicians and home health nurses involved in the patients' care. A 10-country study shows the importance of financial incentives, delivery system organization, a standards-setting organization, and peer influence in achieving and sustaining near-universal levels of participation in Denmark. Meanwhile, government funding, an electronic billing mandate, and accreditation of vendor systems all contributed to similar levels of health IT adoption in the Netherlands.
Advancing the Health Information Technology Policy Agenda
President Obama and Congress must draw on the data and lessons from high-performance health systems as they design policies to encourage the spread of health information technology. Not only does the country need to implement health IT within the context of broader quality improvement, international and domestic experience show that concerted federal action is needed to encourage the spread of health information technology and ensure a substantial return on investment. In a new Commonwealth Fund policy perspective, David Blumenthal, M.D., of the Massachusetts General Hospital proposes five important strategies for federal leaders to consider:
- The federal government should provide financial assistance to safety-net providers and small physician practices without the resources to purchase and implement health IT systems.
- Federal financial support is needed to design and implement information exchange networks in local communities.
- The federal government should support research to improve the capabilities of health IT and further evaluate its effects on health care costs and quality.
- Federal leaders must enact payment reform initiatives that encourage adoption of IT and improve health system performance.
- National regulations and standards are needed to ensure privacy and enhance certification, improving both doctor and patient confidence in the security of electronic medical records and the utility of a national network.
Just as investment in railroads, air traffic control, and interstate highways facilitated economic development and national prosperity in the 20th century, so too will the spread of health IT and the development of a national health information network bring long-run benefits and gains to the nation in the 21st century. It is crucial that our federal leadership move now to harness the power of information technology and put the nation on a path to high performance.