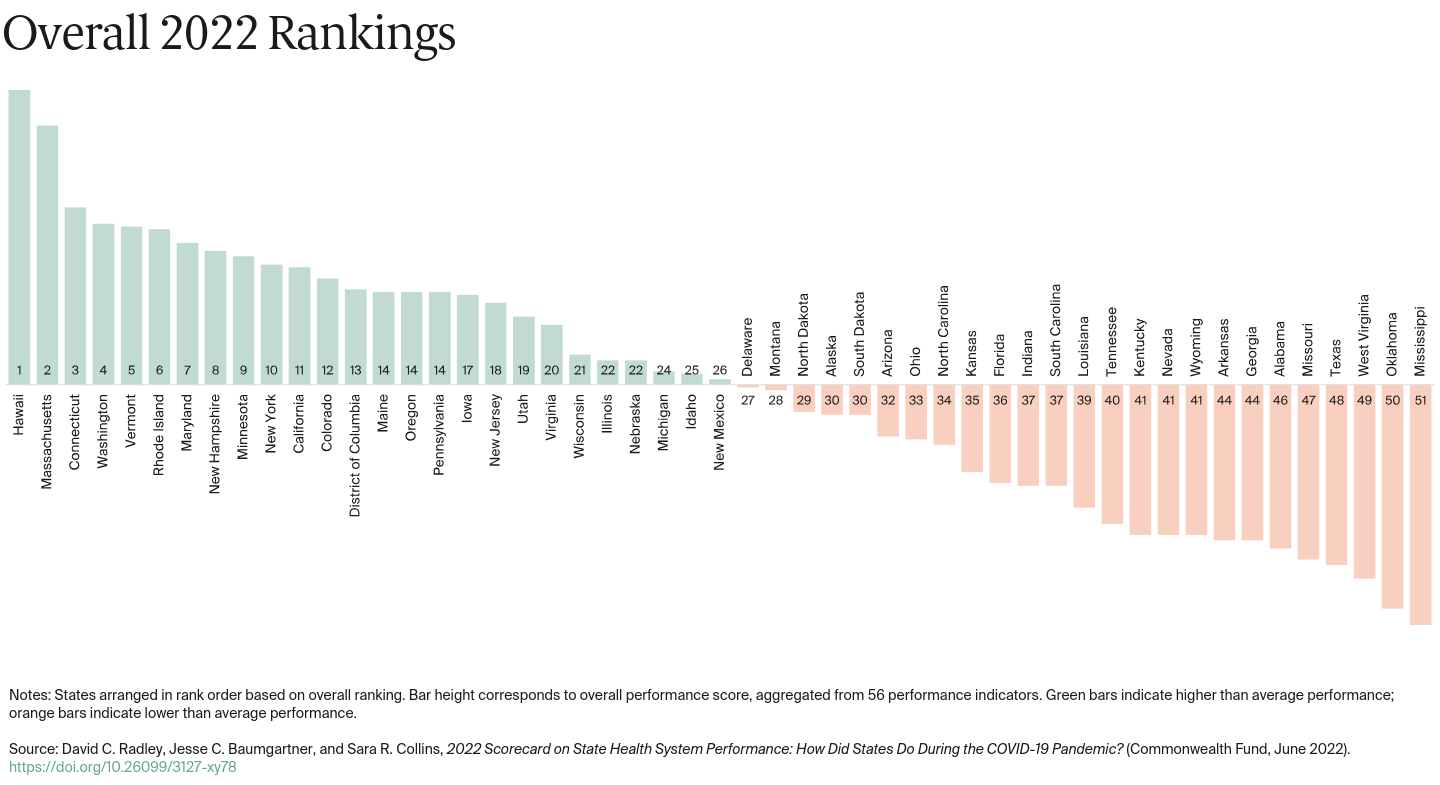
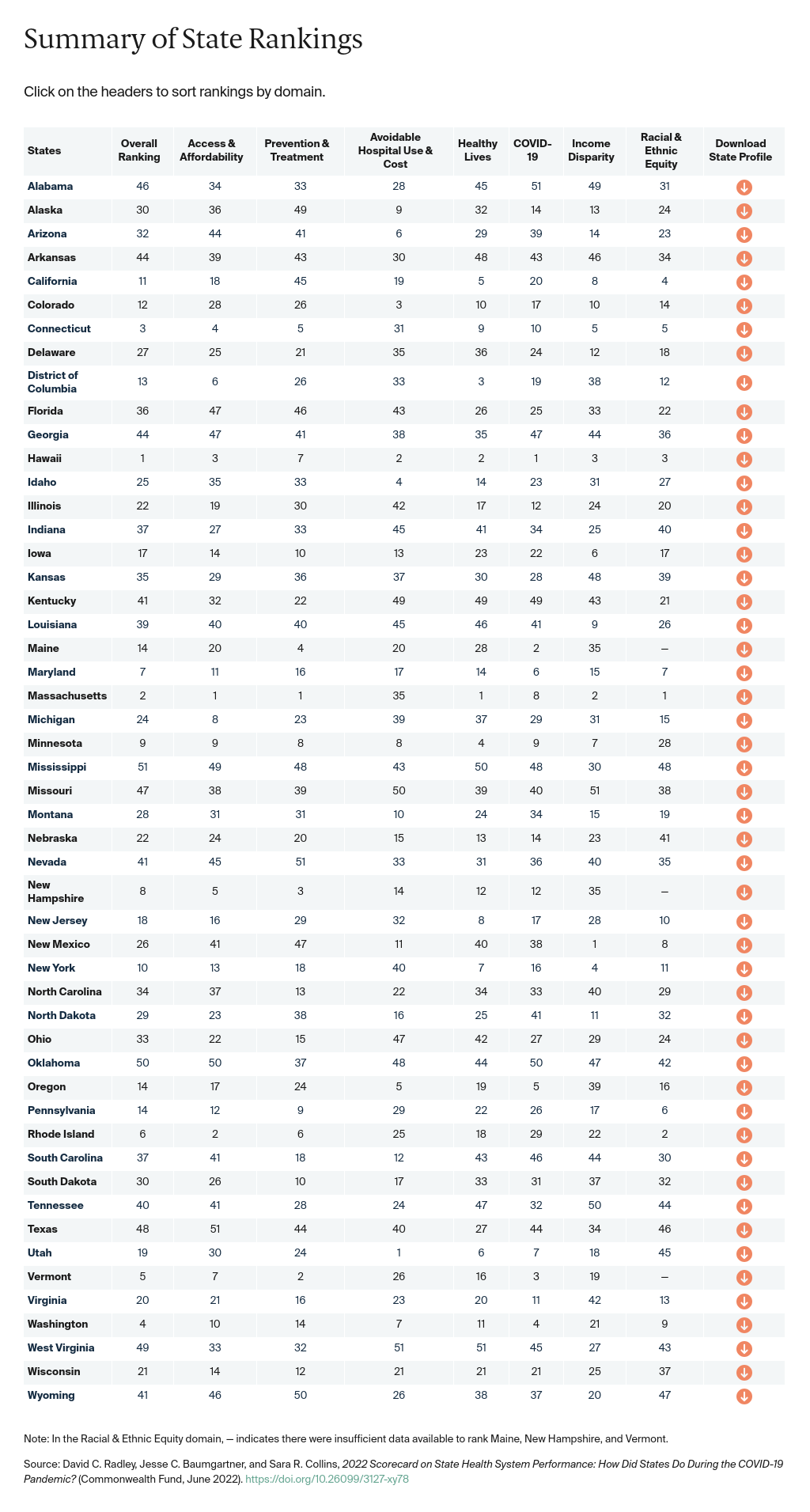
The Commonwealth Fund’s 2022 Scorecard on State Health System Performance evaluates states on 56 performance indicators grouped into five dimensions, including a new dimension focused on how well states responded to and managed the COVID-19 pandemic.
The report generally reflects data from 2020. The seven new measures related to efforts to combat COVID-19 incorporate data through the first quarter of 2022.
Access and Affordability (8 indicators): includes rates of insurance coverage for children and adults, as well as individuals’ out-of-pocket expenses for health insurance and medical care, cost-related barriers to receiving care, rates of medical debt, and receipt of dental visits.
Prevention and Treatment (14 indicators): includes measures of receipt of preventive care and needed mental health care, as well as measures of quality in ambulatory, hospital, postacute, and long-term care settings.
Avoidable Hospital Use and Cost (14 indicators; including several measures reported separately for distinct age groups): includes indicators of hospital and emergency department use that might be reduced with timely and effective care and follow-up care, estimates of per-person spending among Medicare beneficiaries and working-age adults with employer-sponsored insurance, and the share of Medicare and employer-sponsored insurance spending directed toward primary care.
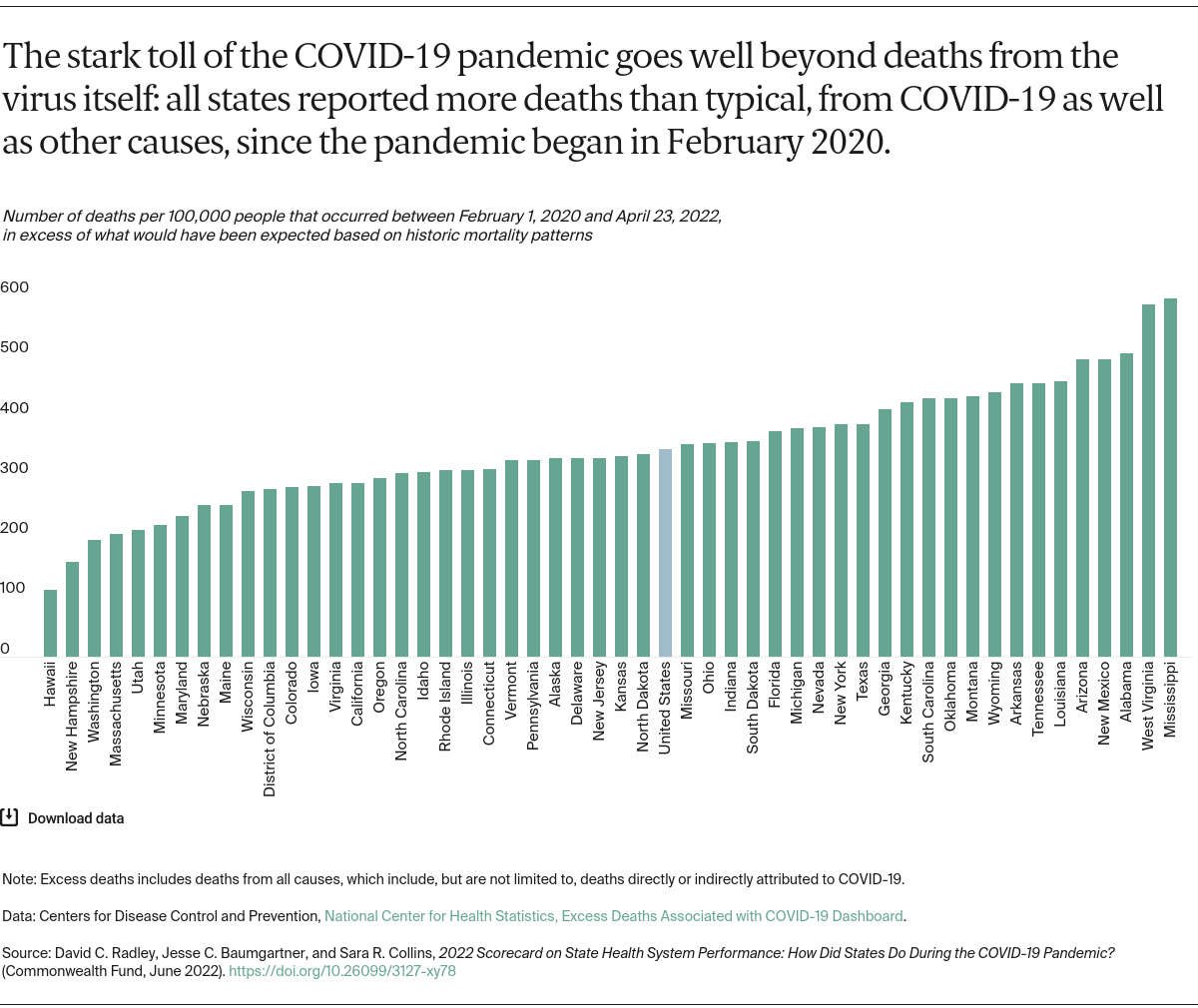
Healthy Lives (13 indicators): includes measures of premature death, health status, health risk behaviors and factors (including smoking and obesity), tooth loss, and state public health funding.
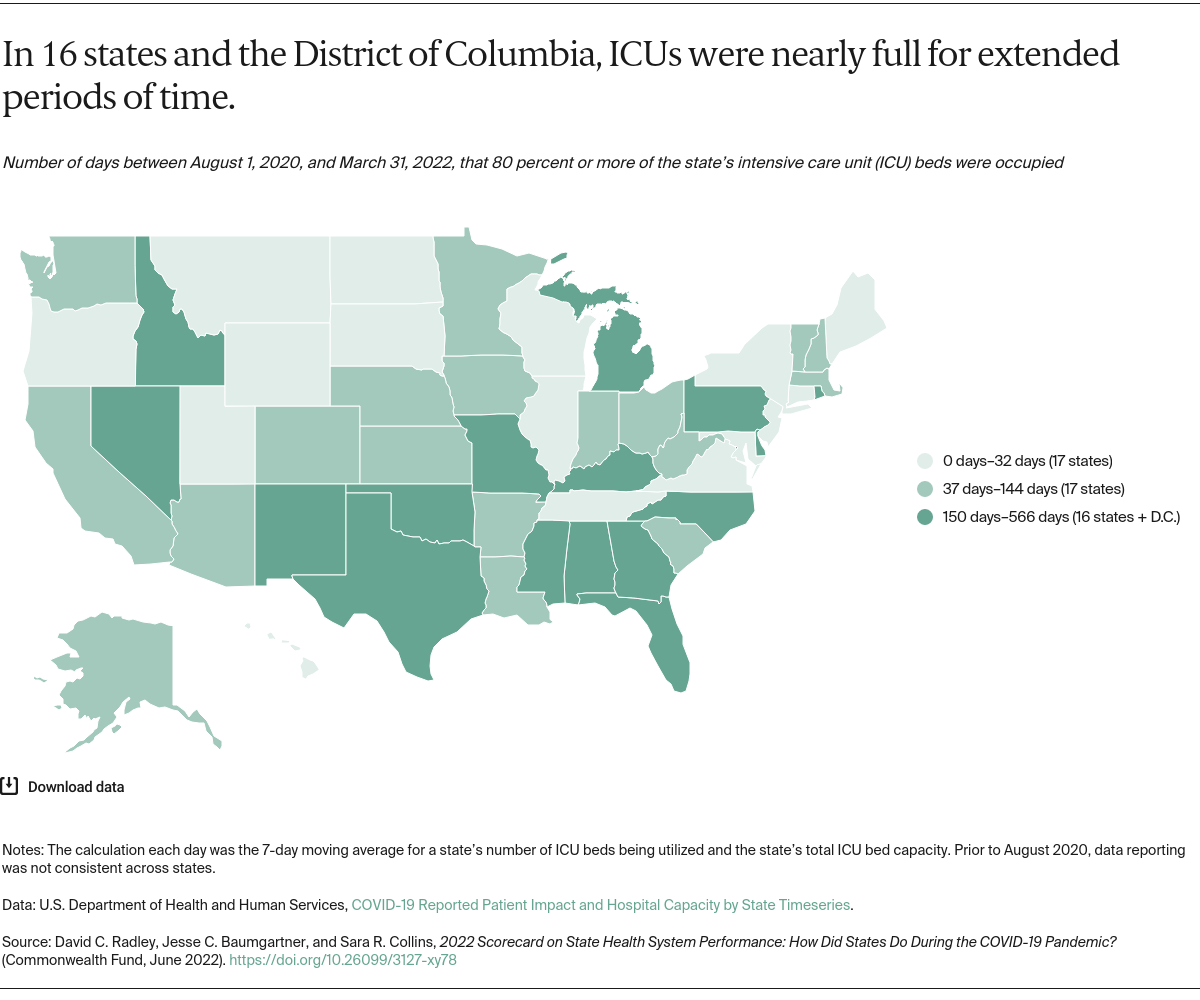
COVID-19 (7 indicators): includes measures to reflect state progress in vaccinating residents, COVID-related hospitalization rates and health system stress, and COVID-related mortality through the end of March 2022.
For several measures in our COVID-19 domain (high ICU stress, hospital staffing shortages, hospitalizations, nursing home deaths), data did not become consistently available, across all states, until May–August 2020, depending on the data source. This means that information from the earliest months of the pandemic may not be fully reflected in our assessment of state COVID-19 performance. This may have a larger impact on states like New York, where the pandemic first emerged in early 2020.
INCOME DISPARITY DIMENSION
This year, the State Scorecard reports on performance differences within states associated with individuals’ income level for 13 of the 56 indicators where data are available to support a population analysis by income; these indicators span three of the five dimensions. For each indicator, we measure the difference between rates for a state’s low-income population (generally less than 200% of the federal poverty level) and higher-income population (generally more than 400% of the federal poverty level). States are ranked on the magnitude of the resulting disparities in performance.
The income disparity indicators are different than those used in previous scorecards; hence, these disparity rankings are not strictly comparable to those published previously. For some indicators, we combined multiple years of data to ensure adequate sample sizes for stratified analysis.
RACIAL AND ETHNIC HEALTH EQUITY DIMENSION
This year, the State Scorecard ranks states based on racial and ethnic health equity. To do this, we incorporated summary state health system performance scores for each of four racial and ethnic groups, pulled directly from our November 2021 report, Achieving Racial and Ethnic Equity in U.S. Health Care: A Scorecard of State Performance.
That report aggregated data on 24 performance indicators (reflecting health outcomes, health care access, and health care quality), stratified by race and ethnicity for Black, white, Latinx/Hispanic, American Indian/Alaska Native (AIAN), and Asian American, Native Hawaiian, and Pacific Islander (AANHPI) populations.
Each population group in each state received a percentile score from 1 (worst) to 100 (best) reflecting the state’s overall health system performance for that group. This enabled comparisons within and across states. For example, a state health system score of 50 for Latinx/Hispanic people in California indicates that the health system is performing better for those residents than Latinx/Hispanic people in Florida, who have a score of 38, but worse than for white residents in California, who have a score of 89.
The overall percentile scores from that report for AIAN, AANHPI, Black, and Latinx/Hispanic people were used in this year’s State Scorecard to reflect each state’s performance for nonwhite racial and ethnic groups. States were evaluated and ranked on their health system performance for each of the four groups separately (contingent on data availability), and those scores were then combined for the state’s final overall equity composite score. Summary scores for each group can be found in Appendix I1. State health system performance scores for white residents are included in the appendix for comparative purposes.
We also include performance data for each of the 24 metrics used in that equity report — updated to the most current year — in each state’s 2022 scorecard profile.
GUIDING PRINCIPLES
The following principles guided the development of the State Scorecard:
Performance Metrics. The 56 metrics selected for this report span health care system performance, representing important dimensions and measurable aspects of care and response to the COVID-19 pandemic. Where possible, indicators align with those used in previous scorecards. Several indicators used in previous versions of the State Scorecard have been dropped either because all states improved to the point where no meaningful variations existed (for example, measures that assessed hospitals on processes of care) or the data to construct the measures were no longer available (for example, hospitalizations for children with asthma). New indicators have been added to the State Scorecard series over time in response to evolving priorities or data availability (e.g., measures of maternal mortality and medical debt).
Measuring Change over Time. We were able to track performance over time for 45 of the 56 indicators. Not all indicators could be trended because of changes in the underlying data or measure definitions, and some reflect newly collected data (e.g., COVID-19-specific measures).
For indicators where trends were possible, there were generally five years between indicators’ baseline and current-year data observation, though the starting and ending points depended on data availability (see Appendix A1).
We considered a change in an indicator’s value between the baseline and current-year data points to be meaningful if it was at least one-half (0.5) of a standard deviation larger than the indicator’s combined distribution over the two time points — a common approach used in social science research. We did not formally evaluate change over time for indicators in the income dimension.
Data Sources. Indicators generally draw from publicly available data sources, including government-sponsored surveys, registries, publicly reported quality indicators, vital statistics, mortality data, and administrative databases. The most current data available were used in this report whenever possible. Appendix A1 provides detail on the data sources and time frames.
Scoring and Ranking Methodology. For each indicator, a state’s standardized z-score is calculated by subtracting the 51-state average (including the District of Columbia as if it were a state) from the state’s observed rate, and then dividing by the standard deviation of all observed state rates. States’ standardized z-scores are averaged across all indicators within the performance dimension, and dimension scores are averaged into an overall score. Ranks are assigned based on the overall score. This approach gives each dimension equal weight and, within each dimension, it weights all indicators equally. This method accommodates the different scales used across State Scorecard indicators (for example, percentages, dollars, and population-based rates).
As in previous scorecards, if historical data were not available for a particular indicator in the baseline period, the current-year data point was used as a substitute, thus ensuring that ranks in each time period were based on the same number of indicators.
REGIONAL COMPARISONS
The State Scorecard groups states into the eight regions used by the Bureau of Economic Analysis to measure and compare economic activity. The regions are: Great Lakes (Illinois, Indiana, Michigan, Ohio, Wisconsin); Mid-Atlantic (Delaware, District of Columbia, Maryland, New Jersey, New York, Pennsylvania); New England (Connecticut, Maine, Massachusetts, New Hampshire, Rhode Island, Vermont); Plains (Iowa, Kansas, Minnesota, Missouri, Nebraska, North Dakota, South Dakota); Rocky Mountain (Colorado, Idaho, Montana, Utah, Wyoming); Southeast (Alabama, Arkansas, Florida, Georgia, Kentucky, Louisiana, Mississippi, North Carolina, South Carolina, Tennessee, Virginia, West Virginia); Southwest (Arizona, New Mexico, Oklahoma, Texas); and West (Alaska, California, Hawaii, Nevada, Oregon, Washington).