Executive Summary
A growing number of employers, health plans, and government programs are seeking to link their health care spending to quality care through pay-for-performance (P4P) activities. The Medicaid program is no exception: over the past several years, the number of state Medicaid pay-for-performance programs has dramatically increased, and all indications are that new programs and approaches will continue to be added.
This report examines the existing and planned pay-for-performance activities of state Medicaid programs. It should inform state governments and other stakeholders that are considering modifying existing programs, implementing new ones, or coordinating their efforts. It focuses on programs that provide financial rewards not only for quality, but also for efficiency and other attributes.
The report is based on findings of a survey of all state Medicaid directors, follow-up interviews with Medicaid directors and their staffs, and review of documents received from the interviewees and on state Web sites. The study was conducted from mid-May through mid-October 2006, and reflects information that was current at the time.
Key Trends
- As of July 1, 2006, more than half of all state Medicaid programs were operating one or more pay-for-performance programs. Within the next five years, if all current plans to start new programs are realized, nearly 85 percent of states will be operating Medicaid pay-for-performance programs (Figure ES-1).
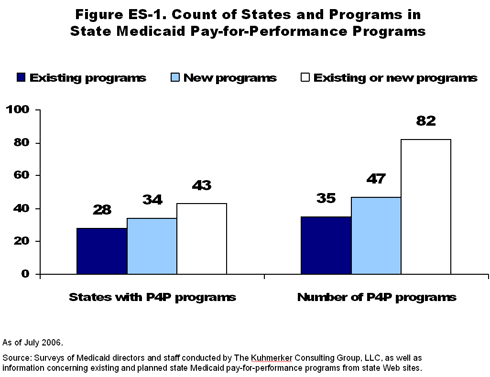
- Medicaid is not a new entrant to the field of pay-for-performance: almost half of all existing programs are more than five years old. A similar percentage of programs began operations within the past two years. More than 70 percent of planned new programs are expected to start within the next two years.
- Seventy percent of existing Medicaid pay-for-performance programs operate in managed care or primary care case management (PCCM) environments, focusing on health care for children, adolescents, and women. While planned programs are still focused on managed care and PCCM providers, they appear to be shifting their emphasis to environments in which quality and cost issues related to chronic disease management can be better targeted. Rewarding the provision of primary care continues to be a component in the vast majority of Medicaid pay-for-performance programs.
- There are several noteworthy trends in planned new programs:
- Nine Medicaid programs are joining with other payers, employers, consumers, and providers in statewide and regional pay-for-performance and quality improvement efforts. For example, the Oregon Health Care Quality Corporation, involving state government, health plans, medical groups, insurers, purchasers, providers, and consumers, is working to incorporate standardized performance measures into their P4P activities. Several Medicaid directors in other states expressed an interest and willingness to join such efforts. The common principles and requirements emerging from these efforts should improve P4P programs around the nation by promoting consistency and stability. However, this movement toward the use of community and national standards may pose a significant challenge to some states, where many of the performance measures used are unique to the Medicaid program and its concerns.
- Health information technology (HIT) is a focus of numerous Medicaid pay-for-performance programs. Several Medicaid programs are "paying for participation," rather than "performance," in an effort to encourage providers to adopt electronic health records, electronic prescribing, and other technologies. For example, Alabama is offering reimbursement increases tied to provider participation in a program using technology to improve monitoring of patients with chronic diseases. HIT also has the potential to reduce data collection costs in P4P programs, which should allow P4P programs to expand into less-traditional venues.
- Several Medicaid directors were concerned that P4P activities might impinge upon beneficiaries' access to care by causing providers to leave the Medicaid program or limit the number of Medicaid beneficiaries served in their practices. This concern is shaping some of the approaches taken in pay-for-performance programs, particularly in states with large rural or sparsely populated areas. For example, South Carolina is offering increased reimbursement to providers who agree to establish a medical home for Medicaid beneficiaries.
- The vast majority of Medicaid directors reported that their priority in operating pay-for-performance programs is to improve quality of care rather than reduce costs. Some states are targeting specific aspects of care, such as the overuse of emergency department services. Maine's Physician Incentive Program ties 30 percent of a performance bonus to emergency department utilization measures.
- Few state Medicaid programs have conducted formal evaluations of their programs.
Measures and Incentives
Measures (the performance standards) and incentives (the ways in which states reward providers for good performance) used in state Medicaid programs vary widely. Some programs include as few as one or two measures, while others include 10 or more. The complexity and number of incentives used in programs also vary, though not as substantially. Nonetheless, there are several commonalities and trends:
- Medicaid directors reported that they select measures for their pay-for-performance programs that they feel are best suited to address their specific improvement goals. It is important to them that measures are scientifically sound, feasible to collect, and regularly reviewed and updated.
- This study characterized the measures used in state Medicaid pay-for-performance programs into five types: Health Plan Employer Data and Information Set (HEDIS) and HEDIS-like measures; structural measures; cost/efficiency measures; measures based on patient experiences; and measures based on medical records. Using this categorization, the most commonly used measures in existing programs are HEDIS and HEDIS-like measures, followed by structural measures. Few programs use measures based on medical records, or review medical records in conjunction with other types of measures.
- The most common assessment methodologies in existing programs are attainment of a specified level of performance and degree of improvement. This continues to be the case with planned programs. Yet, in an effort to address shortcomings in each of these separate approaches, more than 40 percent of new programs are planning to include assessment methodologies that combine attainment and improvement goals for the same measures. To ensure a basic level of attainment is reached, Nevada established a bottom level of performance, beneath which no incentive payment is provided. Massachusetts is considering using incentives to reward attainment of specified levels of performance as well as improvement.
- This study characterized incentives into six types: bonuses; differential reimbursement rates or fees; penalties; auto-assignment of beneficiaries to a plan or provider; withholds; and grants. While not technically a financial incentive, auto-assignment is included as a pay-for-performance incentive because it drives market share and, therefore, compensation. Most Medicaid directors said that bonuses and differential reimbursement are the most effective types of incentives, and the types of incentives planned for new programs are consistent with this assessment. In existing programs, penalties are the second most common type of incentive. Medicaid directors thought that penalties were the least effective incentive and, in fact, could be detrimental to a pay-for-performance program. Only two new programs are currently planning to include penalties.
- A few states are offering grants rather than performance-based pay. New York
is offering five grants for pay-for-performance demonstration projects, while Pennsylvania allows hospitals to compete for grants to support quality-related investments. - Many pay-for-performance programs include non-financial incentives in addition to financial incentives. The most common of these is public reporting of performance.
- Some states are directly emphasizing physician performance—both primary care providers and specialists—in their pay-for-performance programs. Primary care case management programs in several states, among them Alabama, Louisiana, and Pennsylvania, provide incentives directly to participating providers.
Medicaid directors raised concerns about the potential unintended consequences of pay-for-performance programs. In particular, they feared that: providers might steer beneficiaries with complicated conditions away from their practices; providers might decide to leave the Medicaid program if the wrong kinds of incentives (primarily penalties) were included; and mandatory participation in pay-for-performance might, in and of itself, result in providers leaving the program.
Conclusions
Medicaid directors and their staffs generally report positive feedback on their pay-for-performance programs and believe that the overall quality of care being provided is improving, although they have mixed opinions about cost savings resulting from the programs. Directors are considering changing some of the measures, incentives, and even the data collection strategies to improve their existing programs and to shape planned programs. Overall, they believe that pay-for-performance is adding to their repertoire of tools to improve the care provided to their Medicaid populations.
As state governments and other stakeholders move forward with pay-for-performance activities, several challenges will need to be addressed. For example, the growing trend toward collaboration among health care purchasers and other stakeholders may present competing priorities. Medicaid programs will need to consider the particular needs in their own states—including ensuring access to care, promoting high-quality prenatal and postpartum care, and addressing the needs of beneficiaries with chronic conditions—as well as broader community and national standards. The expansion of HIT will provide opportunities for more precise and comprehensive measurement and more efficient data collection, making it easier to satisfy the demands of all stakeholders.
Ultimately, the biggest challenge facing both state Medicaid P4P programs, and those operated under other auspices, is to determine their effectiveness. Given that individuals change providers and may lose coverage altogether, and that standards of care change over time, this is difficult to do in any environment. However, Medicaid programs operate in a public setting. To the extent that Medicaid directors believe that pay-for-performance is improving care and reducing inappropriate spending, it is important that quantifiable and reliable results are available to demonstrate the value of continuing the financial investment that states are making in these programs.


