ABSTRACT
Background: In recent years, Medicaid supplemental payments have grown in importance as a way for states to support safety-net hospitals and compensate providers for low payment rates. However, because these payments are typically not tied to services or quality, they detract from states’ efforts to support value-based purchasing. Goal: To review state and hospital reliance on these payments and describe how the funds might be redeployed. Methods: The authors held interviews and roundtables with current and former state Medicaid officials and hospital leadership; conducted a review of state Medicaid authorities to identify examples of supplemental payment methodologies; and analyzed relevant federal policies and datasets. Key findings: Change is coming for supplemental payments, prompted by state efforts to move to value-based Medicaid payment systems, growth in managed care, and new federal rules and oversight. Because of the way the nonfederal share of these payments is typically funded, reform may require a shift in both how these funds are distributed and how they are financed. Conclusions: While challenging, several options exist to redeploy Medicaid supplemental payments to align with states’ efforts to promote high-quality, cost-effective care, ensure fair payment rates, and support safety-net hospitals.
INTRODUCTION
Over the past 20 years, Medicaid has emerged as the nation’s largest health insurer, covering some 69 million—nearly one of four—U.S. residents.1 Jointly funded by the federal government and states, the program accounted for over $500 billion in spending in 2015.2 It is the single largest purchaser of health services in states, one of the largest items in state budgets, and the largest source of federal revenue for states. Not surprisingly, states are increasingly intent on using Medicaid’s market power to promote the delivery of cost-effective, high-quality care for Medicaid patients and across the health system.
States’ reliance on supplemental payments complicates these efforts. Supplemental payments are made by state Medicaid programs to providers, most commonly hospitals, outside of regular Medicaid payment mechanisms. They take two forms: disproportionate share hospital (DSH) payments and upper payment limit (UPL) payments. Historically the payments have been used to achieve two objectives: 1) to stabilize funding for safety-net hospitals that serve large numbers of uninsured and Medicaid patients; and 2) to compensate providers for low Medicaid payments.3
The formulas that drive these payments to providers can be complicated and opaque and typically are not connected to a specific service delivered to a specific Medicaid or uninsured patient or to patient outcomes. States usually fund the nonfederal share of these payments through assessments or taxes on health care providers or intergovernmental transfers (IGTs) from another governmental entity, including counties on behalf of publicly owned hospitals. These financing mechanisms are legal and an important source of funding for Medicaid programs. However, sources of the nonfederal share can influence the distribution of the payments; the entities paying the taxes or IGTs often benefit most from supplemental payments. For all these reasons, while supplemental payments have helped states address important objectives and provide significant support to providers that serve Medicaid and uninsured patients, they can detract from efforts to promote value tied to quality, costs, and outcomes. This is true particularly when supplemental payments make up a large share of payments to a class of providers.
Shifting from a reliance on supplemental payments is difficult, but change is coming, prompted by state efforts to promote value, federal guidance constraining the use of UPL payments, and impending reductions in federal DSH allotments. This report reviews states’ and hospitals’ reliance on these payments, describes relevant new federal rules, and explores how Medicaid supplemental payments can be redeployed to support value-based purchasing while still fulfilling the goals of supporting safety-net hospitals and ensuring fair provider reimbursement levels.4
STRUCTURE OF MEDICAID’S SUPPLEMENTAL PAYMENTS
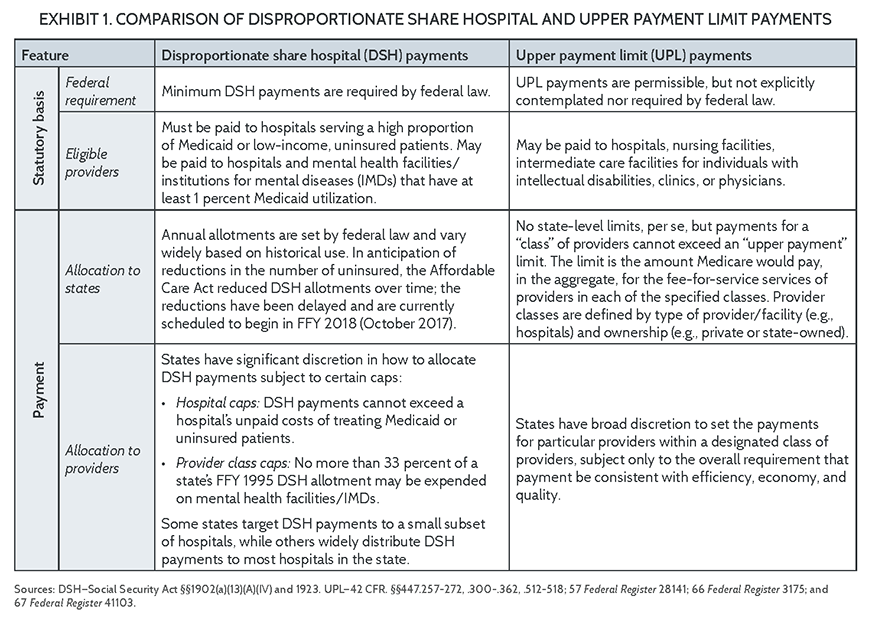
Supplemental payments include both DSH and UPL payments. While the two funding streams are often used interchangeably, they have different statutory bases and regulatory frameworks. DSH payments are required by federal law for the purpose of supporting hospitals that serve large numbers of Medicaid and uninsured patients.5 States receive a federal DSH allocation under a formula set by federal law. These allocations, which vary widely by state, are slated to be reduced under a provision in the Affordable Care Act. After two delays enacted by Congress, the reductions are scheduled to be implemented in Federal Fiscal Year (FFY) 2018 (October 2017) but may again be delayed. States have considerable discretion in how they distribute DSH funds, although payments to individual hospitals cannot exceed hospital-specific DSH caps. Some states tightly target DSH payments, while others provide all or nearly all hospitals with some level of DSH support.
In contrast to DSH payments, UPL payments are not required or even explicitly authorized by federal law, and states do not receive “allocations” to make these payments to Medicaid providers. UPL payments evolved over time as a consequence of flexibility in Medicaid fee-for-service payment rules. In 1987, Congress imposed an upper payment limit (“UPL”) that constrains how much can be paid through these types of payments.6 Under the law, UPL payments, when combined with Medicaid fee-for-service payments, cannot exceed what Medicare would pay for the same services. The UPL is calculated in the aggregate for designated classes of providers (e.g., state-owned hospitals). As long as states comply with the aggregate limit, they have broad discretion to determine the amount of UPL payments they make to individual providers within a designated class, subject to the rule that all Medicaid payments be “consistent with efficiency, economy, and quality of care.”7
Exhibit 1 provides an overview of the basic features of DSH and UPL supplemental payments.
Financing of Supplemental Payments
Like regular Medicaid payments, both DSH and UPL payments are jointly funded: the state provides the nonfederal share, which is then matched by the federal government. And like other Medicaid payments, federal law authorizes states to fund the nonfederal share of supplemental payments from a range of sources, including state general funds, provider taxes, and intergovernmental transfers (IGTs).
Relative to regular Medicaid payments, the state share of supplemental payments is financed disproportionately through provider taxes and IGTs. Provider taxes and IGTs made up approximately 12 percent of the nonfederal share of Medicaid managed care payments and 23 percent of the nonfederal share of fee-for-service Medicaid payments in 2012. By contrast, these sources accounted for approximately 60 percent of the nonfederal share of DSH payments and 74 percent of the nonfederal share of UPL payments.8 This is entirely legal. While states are required to support at least 40 percent of their nonfederal share of total Medicaid costs through state sources (including state-levied provider taxes), states may raise as much as 60 percent of their nonfederal share through nonstate sources, including funds from counties, cities, and local hospital districts.9
Provider-based sources of financing for the nonfederal share of supplemental payments, while legal, can affect the distribution of these payments. The providers who are shouldering the cost of the state share understandably have a strong interest in how the payments are expended, making it challenging to redeploy supplemental payment funds in new ways.
Reliance on Supplemental Payments
An estimated $47 billion, or 10 percent of total Medicaid expenditures, was spent in FFY 2014 in the form of supplemental payments.10 Reliance on these payments varies greatly, but in some states they account for as much as 22 percent of total Medicaid expenditures (Exhibits 2 and 3). Their impact is most apparent when viewed through the lens of hospital financing; supplemental payments account for as much as half of all Medicaid payments to hospitals in some states.11
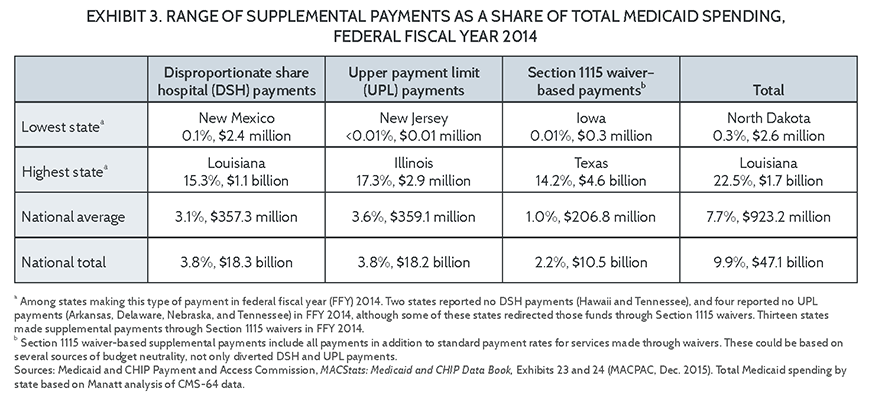
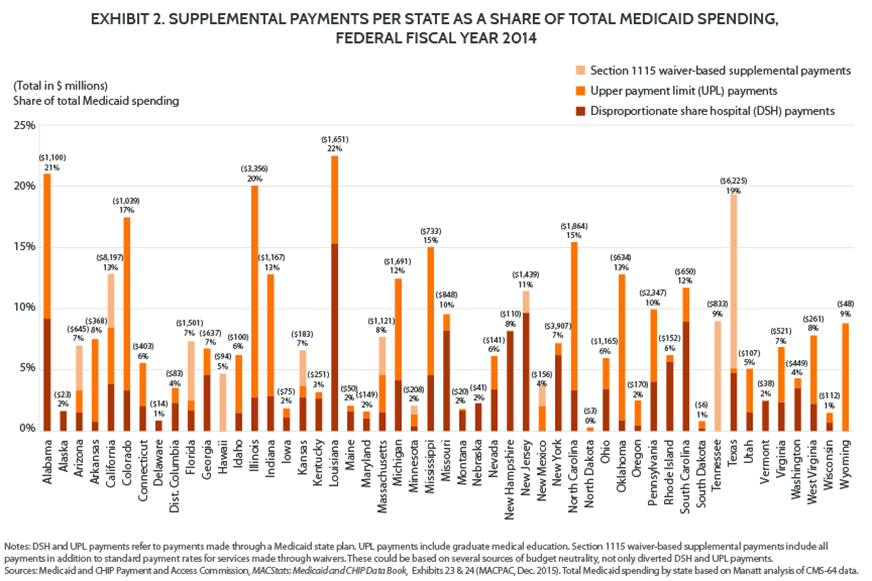

Supplemental payments have grown in part because they have provided a way to fund hospitals without using state general fund dollars. Indeed, following the recession in 2008, supplemental payments became an increasingly important payment strategy to maintain access to services. Driven by declining state revenues, many states cut or froze Medicaid provider rates (where state dollars were implicated) and in some cases backfilled them with supplemental payments (where no state dollars were implicated).12 As a result, supplemental payments, while not an ideal payment methodology from the perspective of states and hospitals, have become a key component of hospital reimbursement in a large number of states.

The growth in these payments has triggered increased federal scrutiny. The Government Accountability Office (GAO), the Office of the Inspector General (OIG) of the Department of Health and Human Services, and the Medicaid and CHIP Payment and Access Commission (MACPAC) have issued a number of reports over the previous decade highlighting the need for enhanced transparency and accountability for supplemental payments.13 More recently, GAO has focused attention on the link between supplemental payments and the source of the nonfederal share of the payments.14 CMS has announced its plan to issue a rule on supplemental payments in 2016.15
THE CHANGING POLICY LANDSCAPE
Changes in state and federal policy are driving states and hospitals to consider new ways to deploy supplemental payments. One key change driven by state policy is that states are relying less on fee-for-service payments and more on managed care arrangements in their Medicaid programs. UPL supplemental payments have historically been used to supplement fee-for-service payments; indeed, as discussed above, the upper payment limit itself is determined based on the extent to which fee-for-service payments to a designated class of providers fall below what Medicare would pay for those services. Because the maximum amount of allowed UPL payments is tied to the total amount of fee-for-service payments for a class of providers, as managed care grows and reliance on fee-for-service declines, the amount of dollars a state can spend on UPL payments also declines.
States and providers have tried to maintain UPL-based supplemental payments—or the value of these payments—in a managed care environment in various ways, but these strategies are neither widely available nor likely to be sustainable. Several states with robust managed care delivery systems have maintained supplemental payment funds by converting them to uncompensated care pools in Section 1115 demonstration waivers. However, this approach has been constrained by recent CMS guidance. In 2015, CMS determined that it will no longer authorize waiver-based uncompensated care pool funding to cover Medicaid payment shortfalls or the uncompensated care costs of individuals who would be eligible for Medicaid if the state had expanded coverage to low-income adults.16 In Florida, where renewal of the uncompensated care pool authorized by the state’s Section 1115 waiver triggered CMS’s first application of these uncompensated care pool principles,17 the new policy led to a 40 percent reduction in the state’s uncompensated care pool funds.18 CMS is also curbing states’ ability to condition uncompensated care pool payments on providers’ payment of the nonfederal share (as it has done for other types of Medicaid payments), which is also likely to make it difficult for states to continue to rely heavily on these pools.
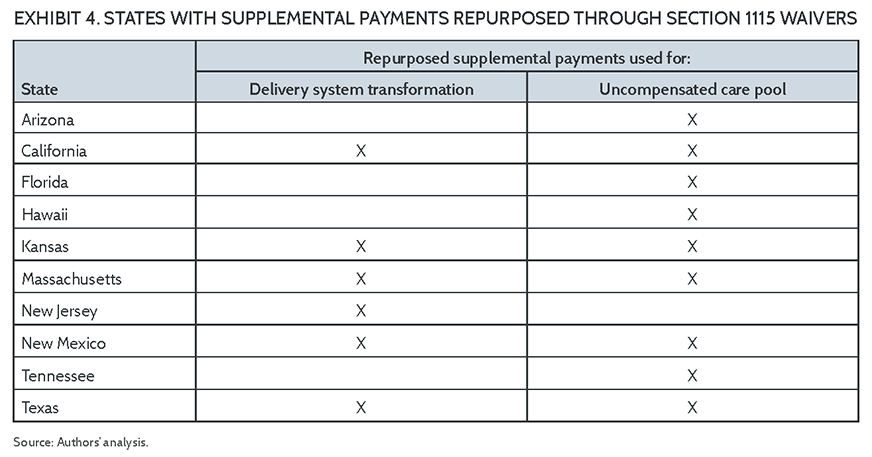
States also have used Delivery System Reform Incentive Payment (DSRIP) waivers to maintain supplemental payments after conversion to a managed care delivery model. While DSRIP waivers can help a state redeploy supplemental payments to support its delivery system reform objectives, not all states are in a position to secure such a waiver. In addition, a DSRIP waiver is not a permanent solution to redeployment, because these waivers are intended to be time-limited.19 Exhibit 4 lists the 10 states that have redirected supplemental payments through Section 1115 waivers to support delivery system transformation or uncompensated care pools, or both.
Finally, some states have sought to maintain their UPL payments in a managed care environment by passing them through to providers via the managed care organizations. In recently issued regulations, however, CMS restated its longstanding policy that “pass-through” payments are not consistent with managed care payment principles and are not permitted.20 When CMS first proposed to eliminate pass-through supplemental payments, some states and providers protested loudly, resulting in CMS’s final Medicaid managed care regulations allowing states a transition period to phase out these arrangements. In the case of pass-through payments to hospitals, the phase-out period is 10 years, with allowable payments decreasing by 10 percentage points each year.21 Although the regulations apply the 10-year phaseout period to both existing and new hospital pass-through payments, soon after the regulations were issued CMS announced its intention to revise the rules and not permit new pass-through payments (that is, those not in place in July 2016).22
Together, these changes in state and federal policies are prompting a review of supplemental payments in many states. The disconnect between supplemental payments and value-driven payment strategies provides further impetus for states to consider reform, as described below.
REDEPLOYING SUPPLEMENTAL PAYMENTS TO PROMOTE VALUE-BASED PURCHASING
Supplemental payments, in particular UPL payments, detract from efforts to promote value-based purchasing in Medicaid in a number of ways:
- Typically, supplemental payments are not linked to particular services provided to particular patients. In some cases, they are linked to the volume of services provided years earlier.
- The connection between supplemental payments and value is further attenuated because the method for distributing the funds is often based on complicated and opaque allocation formulas. With limited exceptions, supplemental payments are made regardless of the quality, efficiency, or outcomes of care.
- To the extent that supplemental payments constitute a substantial portion of hospitals’ total Medicaid payments, they limit the opportunity a state has to leverage its regular Medicaid payments to drive value.
- When these payments are made only or largely to the hospitals or jurisdictions that contribute to the nonfederal share, they may not be equitably or efficiently addressing either of the intended purposes of the payments: namely, making up for Medicaid shortfalls in regular payments and helping to support safety-net hospitals.
Prompted by new federal policies, the growth of managed care, and the goals of promoting value-based payments, states and stakeholders are considering ways to redeploy supplemental payment funds.
Conceptually, there are some straightforward paths to ensure that the funds now expended through supplemental payments serve the basic purpose of those payments and advance value-based purchasing. However, it can be challenging to untangle financing arrangements that have evolved over many years. In particular, separating the payments from the sources of the nonfederal share is tricky. For example, if a county makes an IGT payment, it has generally been able to ensure its IGT payment will result in a supplemental payment to its hospitals. But when funding for supplemental payments is folded into a state’s standard payment mechanism, such as the rate paid for hospital visits, a county that provides an IGT cannot be assured that its contributions will result in a commensurate increase in payments to its hospitals. In such cases, counties may be reluctant to continue those intergovernmental payments.23 A similar tension arises when the nonfederal share of supplemental payments is funded with provider taxes.
These challenges may affect the timing and approach a state adopts to redeploy supplemental payments. Those approaches are described below.
Fold supplemental payments into base payment rates and apply value-based strategies to such payments. Where supplemental payments have been used to compensate for low Medicaid rates, states can redirect the funding for supplemental payments into payment rates to achieve the same goal. This would provide a far greater level of transparency, accountability, and support for value-based purchasing strategies. In addition, redeployment of supplemental payment funds into “regular” Medicaid payments (fee-for-service or managed care) can have significant fiscal benefits to the extent that a state has expanded Medicaid under the Affordable Care Act and can take advantage of the higher federal matching rate applicable to this population (see box).
FISCAL ADVANTAGE TO FOLDING IN SUPPLEMENTAL PAYMENT FUNDS TO PAYMENT RATES IN MEDICAID EXPANSION STATESTo the extent that a state’s UPL supplemental payments are not tied to fee-for-service care provided to specific patients, the nonfederal share for those payments is matched at a state’s “regular” federal matching rate, which ranges from 50 percent to 78 percent. This rate applies even in states that have expanded Medicaid and receive a higher matching rate (95% in 2017) for the Medicaid expansion population. However, if a state folds its supplemental payments into managed care rates, the increased rates for care provided to expansion adults would qualify for the higher federal match. This has nonfederal share implications. Consider the following scenario: State X has a “regular” match rate of 57 percent and receives $50 million in provider payments to finance the nonfederal share of $116 million in UPL supplemental payments. State X has expanded Medicaid, and 20 percent of its Medicaid expenditures under managed care are attributable to members in the new adult group. If the same $50 million in nonfederal share were invested in a rate increase, 20 percent (or $10 million) would be matched at the enhanced rate. The $50 million nonfederal share investment would result in $292.8 million in improved rates. Alternatively, in order to finance a rate increase valued at $116 million (the aggregate value of the UPL payments), the nonfederal share required would drop from $50 million to $41.16 million.
Source: 78 Federal Register 19917, “Medicaid Program; Increased Federal Medicaid Assistance Percentage Changes Under the Affordable Care Act of 2010,” April 2013. |
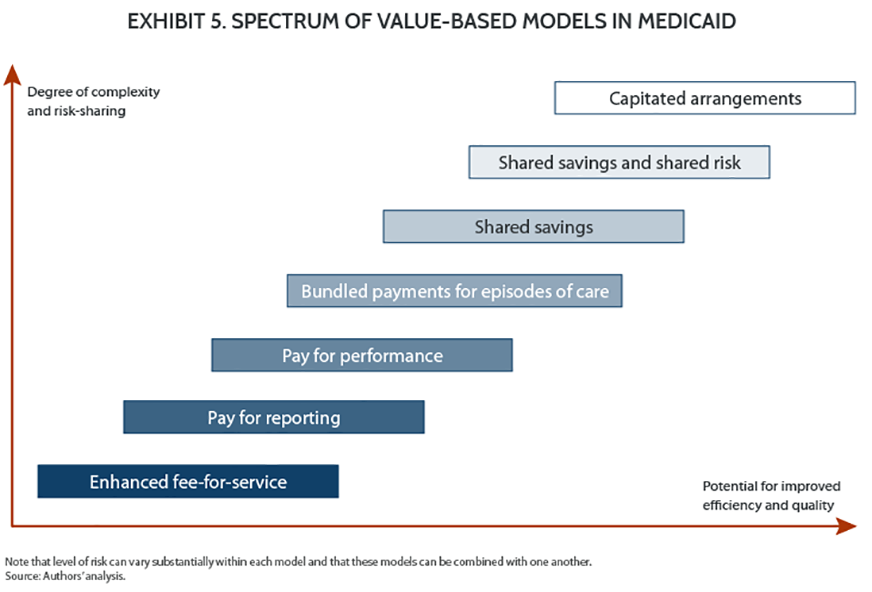
Folding supplemental payments into base rates can work whether the state relies on fee-for-service or managed care. In one state, for example, a large hospital system is recommending that supplemental payments be folded into that state’s fee-for-service rates, in part to promote more predictable and stable financing. By moving supplemental payment funds into the fee-for-service rate structure, the value-based strategies employed by a state would apply to all payments to the hospitals, rather than just to a portion of those payments (see Exhibit 5 for examples). States that fold their supplemental payment funds into fee-for-service rates can still ensure support for safety-net institutions by establishing differential methodologies or payment levels for reimbursing safety-net hospitals. The boost in payments to safety-net hospitals, however, cannot be tied to whether or the extent to which a safety-net hospital contributes to the nonfederal share.
A similar strategy can be adopted in states with a managed care delivery system. Those states can redirect funding for supplemental payments to health plans and require those plans to pay minimum payment levels for all hospitals or enhanced payments for high-priority services or providers. For example, New Hampshire requires its managed care plans to pay providers no less than the amount Medicare would have paid for the same services.24 Facing a reduction in UPL payments from a transition to managed care, New Mexico shifted part of its UPL funds into hospital base rate increases targeting former UPL recipient hospitals’ inpatient services.25 Other states have similar pending redeployment approaches. Alabama plans to fold most hospital UPL payments into rates under a transition to provider-led managed care.26 North Carolina has proposed to incorporate some of its supplemental payments into managed care capitation rates to support value-based purchasing, improved health outcomes, and other Medicaid program goals.27
As is the case in fee-for-service, states can also ensure in the context of managed care that the redeployed funds are used for certain purposes, including providing added support to safety-net hospitals. Under Medicaid managed care regulations issued in May 2016, CMS explicitly permits states to direct their contracted managed care plans to boost rates to designated groups of providers, such as safety-net or critical-care providers, or to provide payments targeted to specified groups of providers to promote access to care or improve its quality.28 The higher rates or payments must be reflected in the capitation rates paid to the plans. In addition, a state could take steps to ensure that the directive to pay at a higher rate does not discourage plans from contracting with the targeted providers. While the regulations permit states to adopt different approaches within managed care to promote quality and drive value, directives to provide enhanced payments cannot be conditioned on participation in an IGT agreement.29
Once supplemental payment funds are folded into base payments (whether fee-for-service or through managed care), they are then subject to and become part of the state’s value-based purchasing strategy. Exhibit 6 lists select examples of state Medicaid program approaches to value-based purchasing.

Tie payments to patient outcomes and delivery system reform priorities. Medicaid supplemental payments—particularly when they are modest relative to underlying base payments—might be maintained as separate payments in a value-based purchasing environment to the extent that the state ties them to patient outcomes or other delivery system priorities, such as greater physical and behavioral health integration. This approach would leverage the funding from the supplemental payments to drive improvements consistent with state priorities. Payments and metrics would be public, increasing transparency and accountability, both central principles of many states’ payment and delivery system reform initiatives. These types of incentive payments are permitted under federal law in both fee-for-service and managed care settings.30
For example, Colorado—which operates its Medicaid program through fee-for-service primary care case management—has adopted this approach for its hospital supplemental payments. Passed in 2013, “Hospital Quality Incentive Payments” provide supplemental payments for inpatient services meeting quality targets in at least one specified area. In FY 2015, hospitals had the opportunity to receive supplemental payments from this $61.5 million pool for meeting quality targets on reductions in nonemergent emergency department visits, elective deliveries or C-sections for uncomplicated deliveries, postoperative complications, and 30-day hospital readmissions.31 For this type of approach to work in a managed care delivery system, such payments could be designed as incentive payments, which are explicitly authorized by the recently issued managed care regulations.32
Target supplemental payments to hospitals with large uncompensated care costs. A different approach to reforming Medicaid supplemental payments might be appropriate where the payments are being used to address the cost of uncompensated care. DSH funding was established to help hospitals manage the cost of uncompensated care. To serve this goal, it is appropriate (and, indeed, required by law) to retain supplemental DSH payments. However, as of 2011, more than one-third of DSH payments were made to hospitals that did not serve a sufficient number of Medicaid or low-income patients to be required DSH hospitals.33 With DSH funds scheduled to decline beginning in FFY 2018 (October 2017), it is especially important to consider how to best target the remaining funds to the highest-need hospitals. In fact, better targeting may also help a state minimize its DSH reductions.34

To promote better value, some states and local health systems also have been exploring ways to redirect DSH funds to improve how care is delivered to the uninsured. For example, a pilot in Ohio’s Cuyahoga County, authorized through a Section 1115 waiver, used DSH funds to provide monthly premium payments to the county-based health system to coordinate care to otherwise uninsured patients through patient-centered medical homes, electronic health records, and other interventions. As a result, patient outcomes improved and costs were reduced.35 Similarly, in December 2015, CMS approved California’s Section 1115 waiver request to combine its UPL-based uncompensated care pool funding with DSH funds to develop a more coordinated care delivery system for uninsured Californians through a global budget approach.36
Financing Reform and Transition Approaches
Current methods for financing the nonfederal share of supplemental payments make it challenging to convert supplemental payments to value-based payments. When supplemental funding is folded into the state’s regular payment system or converted to incentive payments, the funds continue to be paid to providers, but they may no longer go to the providers that paid the nonfederal share in proportion to their tax or IGT contributions.
For a state to redeploy supplemental payments, one of two things must happen: either provider contributions continue but are delinked from payment allocation (for example, a provider tax on hospitals or IGTs from local government fund a general increase in hospital rates), or provider contributions are replaced in whole or in part with state general funds. Either approach is likely to require a transition plan to gradually move to the new financing arrangement and to ensure that hospitals are not subject to a precipitous loss of revenue.
One transition approach would be to phase in supplemental payment reforms. The size of supplemental funding could be reduced gradually, while a different payment system and its associated nonfederal share approach was ramping up. This could mitigate the disruption to hospitals that have relied heavily on supplemental payments, or to states that might directly finance more of the nonfederal share. For example, in 2014 Illinois proposed a time-limited transition pool of UPL payments to create a buffer for hospital losses from payment reform initiatives.37 In addition, as discussed above, to the extent that redeployment of supplemental payments results in the funds being directly tied to services provided to individual patients, the associated fiscal benefit from an enhanced federal match rate in a Medicaid expansion state could help ease the transition.
As discussed above, Medicaid managed care rules explicitly allow a 10-year transition for pass-through supplemental payments made to hospitals. States can maintain the payments, with a phase-down, while potentially redirecting a portion to value-based arrangements. In other words, as pass-through payments decline under the reductions set out in the managed care regulations, new ways to pay for hospital care and finance those payments can gradually be phased in. By the end of the 10-year period (or sooner if states choose), the full amount of the pass-through payment will have been redeployed or eliminated.
Another approach would be for a state to redirect some of the current supplemental funding, financed with IGTs or provider taxes, into a DSRIP waiver focused on transitioning to value-based payments. DSRIPs are intended to help states reform their delivery and payment systems. Providing transitional support to smooth the path to a strengthened delivery system prepared to accommodate value-based payment approaches fits well within the DSRIP concept and has been applied in at least one state.
CONCLUSION
In a stakeholder roundtable convened for this report, one hospital association referred to supplemental payments as both “a blessing and a curse.” It is an apt description. Supplemental payments have enabled states to drive funds to safety-net hospitals and bolster hospitals’ Medicaid revenues, but hospitals have largely picked up the cost of the nonfederal share, and states have limited control and accountability for the funds.
In their current form, supplemental payments—in particular, UPL payments—are not compatible with emerging payment reforms. The federal government also has made clear that such payments will need to be significantly revamped. The question now is how best to drive this transition and achieve an equitable and sustainable system of financing that ensures access to care and adequate provider payments in a value-based payment system.



