
This brief is the first of four in The Commonwealth Fund’s Medicare at 50 Years series that explore the key issues confronting the Medicare program and discuss potential policy options. Two earlier reports in the series traced the evolution of Medicare and its major accomplishments over the past 50 years and examined the Affordable Care Act’s reforms to the program and the challenges facing policymakers going forward.
The Commonwealth Fund’s Medicare at 50 Years series is now available in its entirety for viewing and download as an e-book.
Abstract
The Affordable Care Act (ACA) has provided the Medicare program with an array of tools to improve the quality of care that beneficiaries receive and to increase the efficiency with which that care is provided. Notably, the ACA has created the Center for Medicare and Medicaid Innovation, which is developing and testing promising new models to improve the quality of care provided to Medicare beneficiaries while reducing spending. These new models are part of an effort by the U.S. Department of Health and Human Services to increase the proportion of traditional Medicare payments tied to quality or value to 85 percent by 2016 and 90 percent by 2018. This issue brief, one in a series on Medicare’s past, present, and future, explores the evolution of Medicare payment policy, the potential of value-based payment to improve care for beneficiaries and achieve savings, and strategies for accelerating its adoption.
BACKGROUND
Medicare payment policy has evolved from the cost- and charge-reimbursement approach that was the predominant model when the program was enacted to the establishment of prospective payment systems in the 1980s and 1990s and, more recently, to movement toward value-based payment.1 The enactment of the Affordable Care Act of 2010 (ACA) and the recent announcement of value-based payment goals for Medicare, along with the enactment of the Medicare Access and CHIP Reauthorization Act of 2015 (MACRA), have accelerated that movement and provided Medicare with the means to accomplish the goals of better health care, smarter spending, and a healthier population.2,3 The first two papers in this series focused on Medicare’s accomplishments over its first 50 years, the impact of the ACA on the program, and the challenges that remain; this paper focuses on the evolution of Medicare payment policy and the potential of payment reform to help address those challenges.4,5
EVOLUTION OF MEDICARE PAYMENT POLICY
When Medicare was first established, it adopted the payment methods used by Blue Cross and Blue Shield plans at the time. Hospitals were paid on the basis of their own costs, and physicians were paid on the basis of the fees they charged. These payment systems provided no incentive to control costs—in effect rewarding higher hospital costs and physician fees—and did not take into account the quality or appropriateness of care or its contribution to patient outcomes. Between 1975 and 1985, annual Medicare spending per beneficiary rose from $472 to $1,579—a growth rate of 12.8 percent per year, or 5.3 percent when adjusted for economywide inflation.6
To counter this trend, Medicare in 1983 adopted a prospective payment system for hospital inpatient services, under which hospitals receive a fixed rate of payment per patient based on the average hospital cost nationwide for patients in the same diagnosis-related group (DRG). If the hospital’s cost is less than the DRG payment rate, it retains the surplus payment, and if its cost exceeds the DRG payment rate, it bears the loss on that case. Hospitals responded by sharply reducing average length of stay. Spending per beneficiary by Medicare Hospital Insurance (Part A, which covers hospital inpatient and other facility-based care) subsequently declined sharply (Exhibit 1). Similar payment approaches subsequently were adopted by many private insurers and state Medicaid programs, as well as in more than 40 other countries. Medicare also has adopted prospective payment methods for postacute care, including home health and skilled nursing facility services.
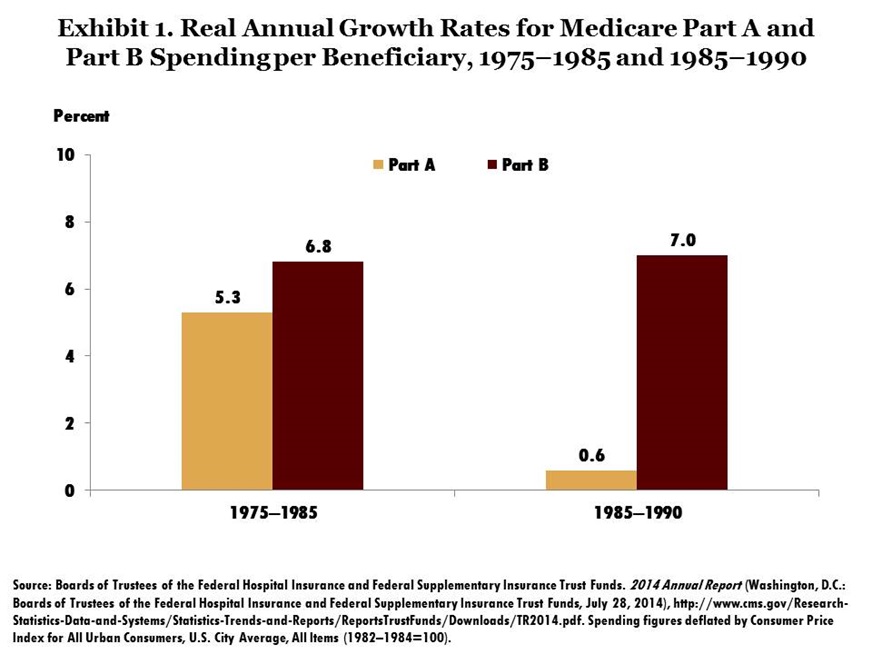
At the same time, Supplementary Medical Insurance (Part B, which covers physician and other ambulatory care) continued to rise rapidly, as physicians continued to receive payments based on usual, customary, and reasonable charges, which rewarded increased spending. In 1989, legislation was enacted to replace the old system. The Medicare fee schedule, implemented in January 1992, was based on an estimate of the resources required to provide each service, rather than having each provider set his or her own charges. Part B spending subsequently slowed dramatically (Exhibit 2). This resource-based relative value scale (RBRVS) has become the standard in the health insurance industry, with most private insurers using a form of RBRVS to set or negotiate rates.
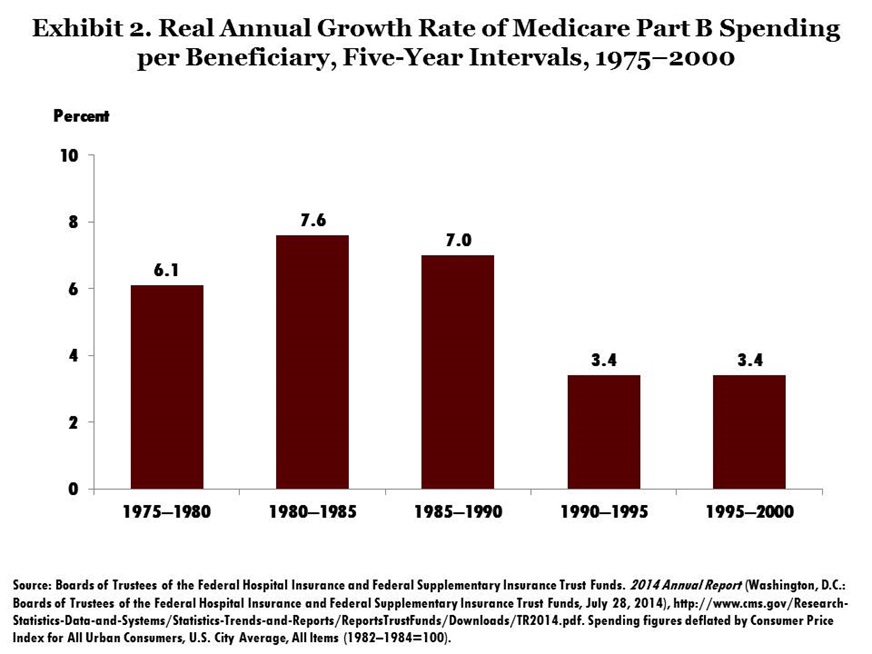
Outpatient prescription drugs were not part of the initial Medicare benefit package. When Congress enacted Medicare prescription drug coverage in 2003, it was made available only through newly created private prescription drug plans. Those plans negotiate payment rates with pharmaceutical companies or contract with private pharmaceutical benefit managers. Unlike other countries, the U.S. does not negotiate pharmaceutical prices for the entire population—and it pays much higher prices for brand-name drugs.7
In 1982, Congress established the Medicare risk contracting program, which provided an alternative option for enrollees who chose to obtain their Medicare benefits from private managed care plans. In 1997 and again in 2003, Congress expanded the number and scope of private plans available through this program, now called Medicare Advantage. Medicare Advantage plans receive a monthly payment for each Medicare beneficiary enrolled in the plan, based on the location, age, and health status of the beneficiary. The fixed per-member per-month payment should give the plan a financial incentive to provide more coordinated, effective, and efficient care—but payments to Medicare Advantage plans historically have exceeded what their enrollees were expected to cost in traditional Medicare, diluting the incentive for efficiency; moreover, although Medicare Advantage plans receive a fixed payment per enrollee, it is not clear how those incentives influence the way the plans actually pay their providers.8
MOVING THE FOCUS OF PAYMENT POLICY FROM VOLUME TO VALUE
Medicare has made significant improvements in the original payment methods modeled on the private insurance payment practices of the 1960s, and recent actions by Congress and the Department of Health and Human Services (HHS) have focused on accelerating that change. The ACA includes an array of provisions that are laying the foundation for fundamental Medicare payment reform, linking payment to patient outcomes and experiences of care, and giving providers an incentive to limit spending by rewarding reductions in the projected spending for their Medicare patients.9
The HHS secretary has set a goal of linking 85 percent of traditional Medicare provider payment to quality or value by the end of 2016, and 90 percent by the end of 2018.10 A recent study indicates that, as of the end of 2013, 42 percent of provider payments in traditional Medicare are tied to the value of care. This represents significant progress, but much still remains to be done (Exhibit 3).11 Many initiatives that were not included in that study are in place now or will soon be implemented, supporting expectations that the percentage will increase considerably over the next few years.
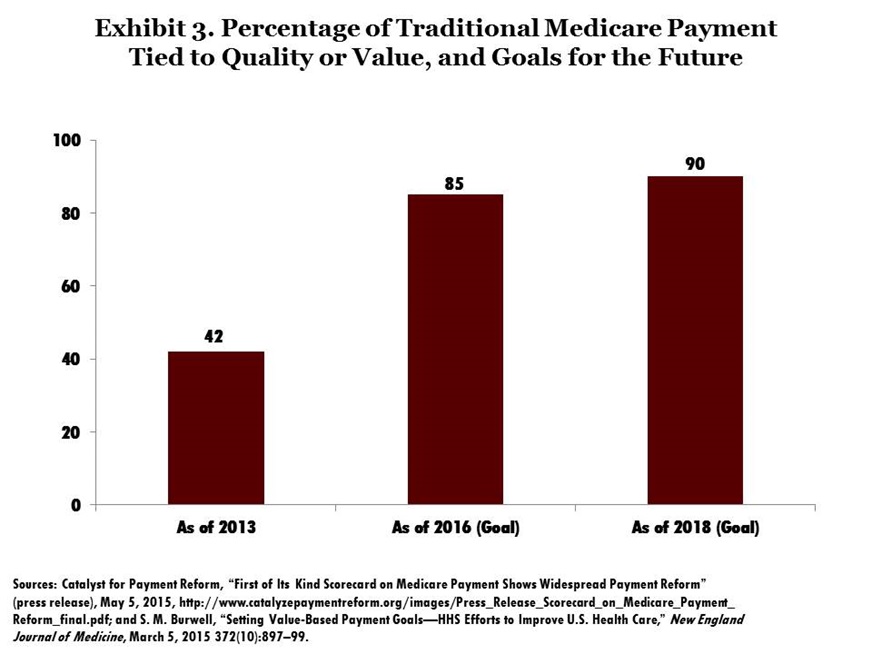
In addition, Medicare Advantage plans, which cover 30 percent of Medicare beneficiaries as of 2014, are now financially rewarded under the ACA for receiving a high rating based on their performance on measures of quality and patient experience.12 Although little is known about how Medicare Advantage plans actually pay their providers, the addition of rewards for plan performance to the existing incentive for efficiency in a per-enrollee per-month payment system can be expected to support the move from volume to value in Medicare.
Payment Approaches That Reinforce Quality
Medicare provides bonuses to hospitals and other providers that achieve top-level scores on patient outcomes and care experiences. As of 2015, 1.5 percent of base payments for more than 3,500 hospitals is withheld and used to reward top-performing hospitals for the quality of their care and their patients’ experiences of care; this amount increases to 2.0 percent by 2017.13 A similar program was initiated in 2015 for physicians in larger practices, and will expand to include all physicians by 2018.14
Several ongoing initiatives involve penalties for specific indicators of poor performance. One such program focuses on hospital readmissions; for several decades, almost 20 percent of Medicare beneficiaries who were hospitalized were readmitted within 30 days.15,16 The Medicare program began to target specific surgical procedures and medical conditions, with the expectation that the list would expand over the years; in just a few years, the overall rate of readmissions has dropped below 18 percent.17 Another initiative penalizes hospitals with higher-than-expected rates of hospital-acquired conditions; those conditions decreased across all hospitals by 17 percent between 2010 and 2013.18
In the MACRA legislation, a merit-based incentive payment system (MIPS) will be established, beginning in 2019, that will combine several current value-based purchasing initiatives and will tie payment more closely to measures of performance.19 The success of these efforts will depend greatly on the ability to develop metrics that are viewed by a broad spectrum of stakeholders as accurate measures of performance—an endeavor that has made great progress but still faces substantial challenges.20
Alternative Payment Models That Reward Value
The ACA created the Medicare Shared Savings Program (MSSP) for accountable care organizations (ACOs), which are groups of providers who accept joint responsibility for the quality and cost of the Medicare patients they treat and can share in the savings they generate as compared with a cost target.21 The ACA also created the Center for Medicare and Medicaid Innovation (CMMI) to develop and test value-based alternative payment methods.22,23 Many of those initiatives represent more far-reaching reforms, and put providers at financial risk for a portion or all of the cost of providing Medicare services. Among the most prominent activities being conducted by the CMMI are several aimed at transforming primary care, and several of its models involve a bundled payment for specified sets of hospital and/or postacute care related to specific procedures or conditions.24
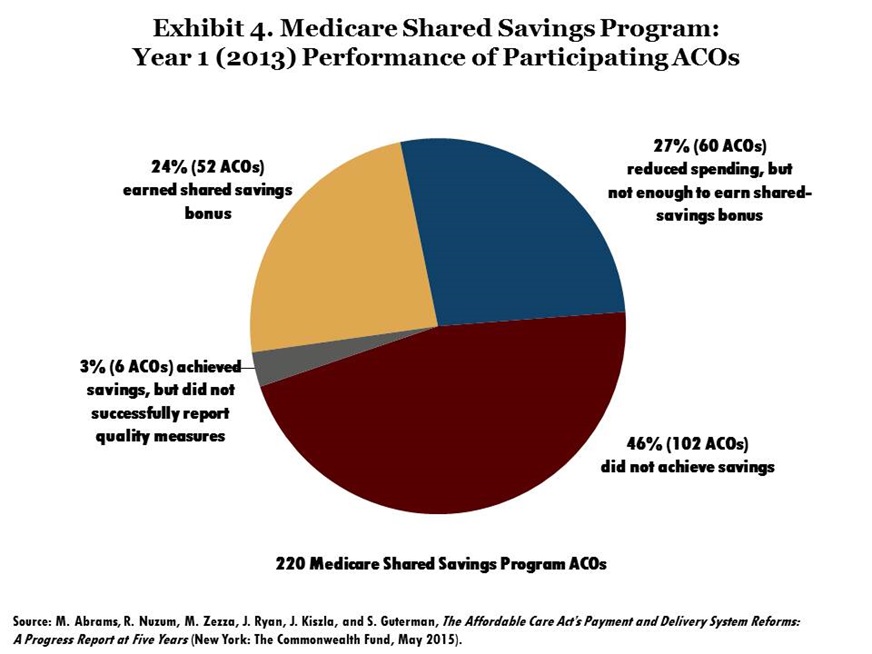
Accountable Care. The MSSP began in 2012; as of April 2015, there were more than 400 ACOs participating in the program, serving more than 7 million Medicare beneficiaries in 49 states, the District of Columbia, and Puerto Rico.25 Early results from the MSSP participants indicate that, as a whole, they have achieved modest savings and generally improved the quality of care.26 In the first year, 54 percent of the organizations for which results were available spent less than their targets, and 24 percent saved enough to earn shared-savings bonuses (Exhibit 4).27
The CMMI designed the Pioneer ACO Model for early adopters of coordinated care. It offers both upside shared savings and downside risk for losses in return for a larger share of achieved savings.28 When it began in 2012 there were 32 participating organizations in 18 states; the number of Pioneer ACOs has fallen to 19 as of 2015, but most of the organizations that left the initiative switched to the MSSP. Over the first two years of the program, total Medicare expenditures increased more slowly for beneficiaries aligned with Pioneer ACOs than for beneficiaries in traditional Medicare, with little difference in patient experience.29 These findings established the Pioneer ACO Model as the first CMMI initiative to meet the ACA criteria (proven potential to reduce Medicare spending while maintaining the quality of care) for expansion to other areas and organizations.
Primary Care Transformation. Since 2012, the Centers for Medicare and Medicaid Services (CMS) has been collaborating with commercial and state health insurance plans to offer population-based care management fees and shared-savings opportunities to participating primary care practices in order to support prevention, access to care, care coordination, chronic care management, and shared decision-making among patients and their providers. As of February 2015, the Comprehensive Primary Care (CPC) initiative includes 480 sites in seven regions, including more than 2,700 providers who serve 2.7 million patients, of which 400,000 are Medicare and Medicaid beneficiaries. Altogether, there are 38 public and private payers participating in this initiative.30 Results from the first year are mixed: there was a statistically significant reduction in total Medicare expenditures per beneficiary, but not quite enough to offset the care management fees paid to the practices; several quality measures improved among participants, but none of the changes was statistically significant.31
Through the Multi-Payer Advanced Primary Care Practice demonstration, begun in 2011, CMS is participating in multi-payer reform initiatives currently under way in eight states to make advanced primary care practices more available.32 The demonstration, which was originally planned for three years, has been extended through 2018; it is anticipated that approximately 1,200 medical homes, serving more than 900,000 Medicare beneficiaries, will participate. In the first year, only two of the seven states for which data were available generated savings; no evidence is yet available on access to or quality of care.33
Although the initial results have been mixed, these models do show some promise for providing vehicles for increasing the emphasis on primary care and facilitating more coordinated care. More time may be needed to overcome the adverse incentives and fragmented delivery and payment systems that still predominate in the U.S. health system.
Bundled Payment. Bundled payment is designed to provide financial incentives to improve the continuity and effectiveness of care, reduce the use of unnecessary services, and slow spending growth by creating financial incentives for providers to coordinate care across settings.34 The CMMI has developed the Bundled Payments for Care Improvement (BPCI) initiative, which provides a single payment amount for a specified course of inpatient and/or post-hospital care. Four payment models cover different combinations of those services, with almost all of the approximately 7,000 participating providers opting for Model 2 (acute and postacute care episodes) or Model 3 (postacute care only).35 Evaluation of first-year performance indicates that Model 2 may decrease variation in the use of postacute care, which has been a major factor in health spending differences across regions.36,37
Progress, But a Long Way to Go
The testing of alternative payment models is still in an early stage. General evaluations have found gains in quality and modest savings, but the results so far have been mixed. There is some evidence that, as experience with alternative payment models accumulates, savings can increase.38 Key requirements for success include setting incentive payments so that they align with potential savings; targeting interventions that help high-cost, high-need individuals avoid unnecessary hospitalization or emergency room use39; and aligning policies among public and private insurers.
STRATEGIES FOR EXPANDING VALUE-BASED PAYMENT
One powerful tool that the HHS secretary possesses is the authority, granted by the ACA, to adopt innovations found to save money and improve quality for use throughout the Medicare program. In addition to continuing to test how well different incentives improve value, HHS is focused on improving the way care is delivered through learning networks such as the recently announced Health Care Payment Learning and Action Network.40 It also aims to increase the availability of information to guide decision-making, by increasing the use of health information technology, enhancing transparency, and generating information through the Patient-Centered Outcomes Research Institute that can guide care decisions.
As described above, the MACRA legislation provides strong impetus to support Medicare’s movement toward value-based payment: it provides 5 percent fee increases to physicians who receive a significant portion of their revenue from an alternative payment model, such as a blended, bundled, or global payment model, or from care provided through patient-centered medical homes or ACOs. In addition, MACRA provides funding to increase the rewards for providers who achieve exceptionally high performance on measures of health care quality, patient experience, and efficiency. Further legislation may be necessary to fix the flawed fee-for-service physician payment system, since it is likely to remain a component of payment methods for some time.41
To accelerate movement away from fee-for-service payment with no link to value, it may be necessary to continue to widen the differential in payment rates for providers that participate in value-based payment models. Rewarding beneficiaries for seeking care from high-value providers would align provider and beneficiary incentives, and could go a long way toward supporting the success of those incentives.42 It would require that beneficiaries be given access to useful information on the prices and quality of participating providers.
Finally, the move to value-based payment will be much more effective if Medicare continues to actively seek partnerships with private insurers, state Medicaid, and other federal programs that adopt value-based payment methods. The ultimate goal is to transform the delivery of care for everyone, improving patient outcomes and care experiences, preventing avoidable hospitalization, and lowering costs. Reducing or eliminating avoidable, unnecessary, and ineffective care, and redeploying those savings to provide better financial protection and lower federal outlays, would be a major step toward improving the financial sustainability of the Medicare program in particular, and the U.S. health system in general.
Notes
1D. Blumenthal, K. Davis, and S. Guterman, “Medicare at 50—Origins and Evolution,” New England Journal of Medicine, Jan. 29, 2015 372(5):479–86.
2S. M. Burwell, “Setting Value-Based Payment Goals—HHS Efforts to Improve U.S. Health Care,” New England Journal of Medicine, March 5, 2015 372(10):897–99.
3S. Guterman, “With SGR Repeal, Now We Can Proceed with Medicare Payment Reform,” The Commonwealth Fund Blog, April 15, 2015.
4K. Davis, C. Schoen, and F. Bandeali, Medicare: 50 Years of Ensuring Coverage and Care (New York: The Commonwealth Fund, April 2015).
5K. Davis, S. Guterman, and F. Bandeali, The Affordable Care Act and Medicare: How the Law Is Changing the Program and the Challenges That Remain (New York: The Commonwealth Fund, May 2015).
62014 Annual Report of the Boards of Trustees of the Federal Hospital Insurance and Federal Supplementary Insurance Trust Funds (Washington, D.C.: Boards of Trustees of the Federal Hospital Insurance and Federal Supplementary Insurance Trust Funds, July 28, 2014), http://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/ReportsTrustFunds/Downloads/TR2014.pdf; and Bureau of Labor Statistics, CPI Detailed Report (Washington, D.C.: BLS, March 2015), https://www.bls.gov/news.release/archives/cpi_04172015.pdf.
7G. F. Anderson, U. E. Reinhardt, P. S. Hussey et al., “It’s the Prices, Stupid: Why the United States Is So Different from Other Countries,” Health Affairs, May/June 2003 22(3):89–105.
8B. Biles, J. Pozen, and S. Guterman, The Continuing Cost of Privatization: Extra Payments to Medicare Advantage Plans Jump to $11.4 Billion in 2009 (New York: The Commonwealth Fund, May 2009).
9M. K. Abrams, R. Nuzum, M. A. Zezza, J. Ryan, J. Kiszla, and S. Guterman, The Affordable Care Act’s Payment and Delivery System Reforms: A Progress Report at Five Years (New York: The Commonwealth Fund, May 2015).
10S. M. Burwell, “Setting Value-Based Payment Goals—HHS Efforts to Improve U.S. Health Care,” New England Journal of Medicine, March 5, 2015 372(10):897–99.
11Catalyst for Payment Reform, “First of Its Kind Scorecard on Medicare Payment Shows Widespread Payment Reform,” Press release (Berkeley, Calif.: CPR, May 5, 2015), https://www.catalyze.org/wp-content/uploads/2017/04/Medicare_Scorecard_Press_Release_2015.pdf.
12B. Biles, G. Casillas, G. Arnold, and S. Guterman, The Impact of Health Reform on the Medicare Advantage Program: Realigning Payment with Performance (New York: The Commonwealth Fund, Oct. 2012).
13Centers for Medicare and Medicaid Services, “Hospital VBP Program Payment Adjustments,” Fact sheet (Washington, D.C.: CMS, Dec. 2014), http://www.medicare.gov/HospitalCompare/Data/payment-adjustments.html.
14Centers for Medicare and Medicaid Services, “Timeline to Phase In the Value-Based Payment Modifier,” Fact sheet (Washington, D.C.: CMS, April 2015).
15G. F. Anderson and E. P. Steinberg, “Hospital Readmissions in the Medicare Population,” New England Journal of Medicine, Nov. 22, 1984 311(21):1349–53.
16S. F. Jencks, M. V. Williams, and E. A. Coleman, “Rehospitalizations Among Patients in the Medicare Fee-for-Service Program,” New England Journal of Medicine, April 2, 2009 360(14):1418–28.
17N. Brennan, “Findings from Recent CMS Research on Medicare,” Presentation at AcademyHealth Annual Research Meeting, June 9, 2014.
18Agency for Healthcare Research and Quality, “Interim Update on 2013 Annual Hospital-Acquired Condition Rate and Estimates of Cost Savings and Deaths Averted from 2010 to 2013” (Washington, D.C.: AHRQ, Dec. 2014), https://www.ahrq.gov/sites/default/files/publications/files/interimhacrate2013_0.pdf.
19Guterman, “With SGR Repeal,” 2015.
20Institute of Medicine, Vital Signs: Core Metrics for Health and Health Care Progress (Washington, D.C.: National Academies Press, 2015).
21D. M. Berwick, “Making Good on ACOs’ Promise—The Final Rule for the Medicare Shared Savings Program,” New England Journal of Medicine, Nov. 10, 2011 365(19):1753–56.
22S. Guterman, K. Davis, K. Stremikis, and H. Drake, “Innovation in Medicare Will Be Central to Health Reform’s Success,” Health Affairs, June 2010 29(6):1188–93.
23M. A. Zezza, M. K. Abrams, and S. Guterman, “The Innovation Center at One Year: Much Progress, More to Be Done,” The Commonwealth Fund Blog, Nov. 29, 2011.
24Abrams, Nuzum, Zezza et al., ACA’s Payment and Delivery System Reforms, 2015.
25Centers for Medicare and Medicaid Services, “Fast Facts: All Medicare Shared Savings Program ACOs” (Washington, D.C.: CMS, April 2015), http://www.cms.gov/Medicare/Medicare-Fee-for-Service-Payment/sharedsavingsprogram/Downloads/All-Starts-MSSP-ACO.pdf.
26Center for Medicare and Medicaid Services, “Fact Sheets: Medicare ACOs Continue to Succeed in Improving Care, Lowering Cost Growth” (Washington, D.C.: CMS, Nov. 10, 2014), http://www.cms.gov/Newsroom/MediaReleaseDatabase/Fact-sheets/2014-Fact-sheets-items/2014-11-10.html.
27Abrams, Nuzum, Zezza et al., ACA’s Payment and Delivery System Reforms, 2015.
28H. H. Pham, M. Cohen, and P. Conway, “The Pioneer Accountable Care Organization Model: Improving Quality and Lowering Costs,” Journal of the American Medical Association, Oct. 22/29, 2014 312(16):1635–36.
29D. J. Neiweide, W. Lee, T. T. Cuerdon et al., “Association of Pioneer Accountable Care Organizations vs. Traditional Medicare Fee-for-Service with Spending, Utilization, and Patient Experience,” Journal of the American Medical Association, published online May 4, 2015.
30Centers for Medicare and Medicaid Services, “Comprehensive Primary Care Initiative,” Fact sheet (Washington, D.C.: CMS, Feb. 2015), http://innovation.cms.gov/initiatives/Comprehensive-Primary-Care-Initiative/.
31E. F. Taylor, S. Dale, D. Peikes et al., Evaluation of the Comprehensive Primary Care Initiative: First Annual Report (Princeton, N.J.: Mathematica Policy Research, Jan. 2015), http://innovation.cms.gov/Files/reports/CPCI-EvalRpt1.pdf.
32Centers for Medicare and Medicaid Services, “Multi-Payer Advanced Primary Care Practice,” Fact sheet (Washington, D.C.: CMS, Feb. 2015), http://innovation.cms.gov/initiatives/Multi-Payer-Advanced-Primary-Care-Practice/.
33N. McCall, S. Haber, M. van Hasselt et al, Evaluation of the Multi-Payer Advanced Primary Care Practice Demonstration: First Annual Report (Research Triangle Park, N.C.: RTI International, Urban Institute, and National Academy for State Health Policy, Jan. 2015), https://downloads.cms.gov/files/cmmi/MAPCP-FirstEvaluationReport_1_23_15.pdf.
34M. A. Zezza, S. Guterman, and J. Smith, “The Bundled Payment for Care Improvement Initiative: Achieving High-Value Care with a Single Payment,” The Commonwealth Fund Blog, Jan. 7, 2012.
35Centers for Medicare and Medicaid Services, “Innovation Models” (Washington, D.C.: CMS), http://innovation.cms.gov/initiatives/index.html#views=models.
36L. Dummit, G. Marrufo, J. Marshall et al., CMS Bundled Payment for Care Improvement Initiative Models 2–4: Year 1 Evaluation & Monitoring Annual Report (Falls Church, Va.: The Lewin Group, Feb. 2015), http://innovation.cms.gov/Files/reports/BPCI-EvalRpt1.pdf.
37Institute of Medicine, Variation in Health Care Spending: Target Decision Making, Not Geography (Washington, D.C.: National Academies Press, 2013).
38Z. Song, S. Rose, D. G. Safran et al., “Changes in Health Care Spending and Quality 4 Years into Global Payment,” New England Journal of Medicine, Oct. 30, 2014 371(18):1704–14.
39Commonwealth Fund Commission on a High Performance Health System, The Performance Improvement Imperative: Utilizing a Coordinated, Community-Based Approach to Enhance Care and Lower Costs for Chronically Ill Patients (New York: The Commonwealth Fund, April 2012).
40Centers for Medicare and Medicaid Services, “Health Care Payment Learning and Action Network” (Washington, D.C.: CMS, April 8, 2015), http://innovation.cms.gov/initiatives/Health-Care-Payment-Learning-and-Action-Network/.
41J. D. Reschovsky, L. Converse, and E. C. Rich, “Solving the Sustainable Growth Rate Formula Conundrum Continues Steps Toward Cost Savings and Care Improvements,” Health Affairs, April 2015 34(4):689–96.
42K. Davis, C. Schoen, and S. Guterman, “Medicare Essential: An Option to Promote Better Care and Curb Spending Growth,” Health Affairs, May 2013 32(5):900–9.



