Full text available at: http://www.urban.org/publications/411771.html
Also see: Who Gained the Most Under Health Reform in Massachusetts?
Background
When Massachusetts enacted its health care reform initiative in 2006, ensuring the affordability and adequacy of insurance coverage was a key goal. If residents were to be required to have health insurance, then the plans available to them must offer enough financial protection so that low-income residents who were formerly uninsured were now not simply underinsured. There was a concern among state leaders that the individual mandate might cause some people to choose plans that offer limited benefits and high cost-sharing in exchange for lower monthly premiums—the kind of coverage that could put them at risk of incurring high costs relative to income and skipping needed care to avoid the expense. As such, improving access to care while providing financial protection was central to the state's discussions about benefit design. To help protect residents from becoming underinsured, the state established a standard for "minimum creditable coverage." Under this standard, all insurance plans must provide a broad scope of key benefits, including preventive and primary care, prescription drugs, and maximums for annual deductibles and out-of-pocket spending.
Overview of the Study

Researchers led by the Urban Institute's Sharon Long assessed the impact of the Massachusetts health reform initiative on the number of underinsured state residents, as compared with national trends. The study team—supported by the Blue Cross Blue Shield Foundation, The Commonwealth Fund, and the Robert Wood Johnson Foundation—interviewed adults ages 18 to 64 years old in fall 2006, before the implementation of the reform, and again in fall 2007, one year after reform efforts began. The study defined individuals as being underinsured if they had health insurance coverage for the full year and had high costs not covered by their plan. "High costs" were defined as 1) having out-of-pocket costs of 10 percent or more of family income, or 2) for families with income of less than 200 percent of the federal poverty level, having out-of-pocket costs of 5 percent or more of income. For 2007 data, the definition was expanded to include deductibles of 5 percent or more of family income, which added about 1 percentage point to the numbers of uninsured. This definition was used in a national study in Health Affairs. The Massachusetts study examined underinsured rates by income level and for adults with health problems, including those who report poor or fair health, a health condition that limits the ability to work, or one of four chronic conditions—hypertension, heart disease, diabetes, or asthma.
Key Findings
- In fall 2006, 7.3 percent of all Massachusetts adults were underinsured (using the definitions above: out-of-pocket costs equal to 10% or more of income for higher–income people, 5% or more for lower-income people). After the enactment of health reform, that share declined to 5.6 percent. During the same time period, the number of underinsured people nationally increased by 5 percentage points.
- In Massachusetts, the greatest reductions in underinsurance occurred for lower-income adults, with rates down by 5.5 percentage points, and adults with health problems, with rates down about 3 percentage points. For higher-income adults, the researchers found low underinsured rates in both time periods.
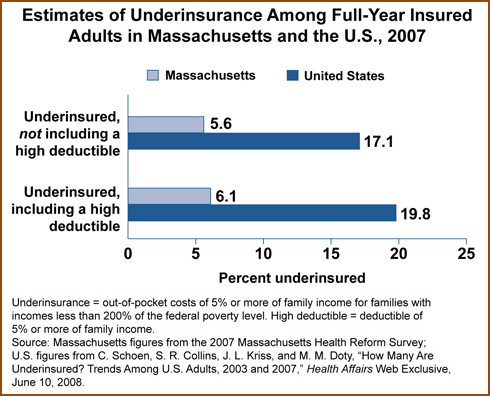
- Notably, trends in Massachusetts moved in the opposite direction from national rates. Based on the Health Affairs study, in 2007, 20 percent of adults who were insured all year were underinsured. In contrast, only 6 percent of Massachusetts insured adults were underinsured. (Both figures use the definition of underinsurance that includes deductibles of 5 percent or more of family income.)
The share of all Massachusetts adults insured all year and not underinsured increased by about 5 percentage points. Coverage improved markedly for lower-income adults (up 13 percentage points) and adults with health problems (up 7 percentage points).
Discussion
The experience of Massachusetts underscores the importance of benefit design for insurance expansion strategies. To achieve the twin goals of health insurance—access to services and financial protection—core benefits must be broad in scope and cost-sharing affordable relative to income. Massachusetts' reform efforts focused on affordability of both premiums and care. Based on the results of this study, reforms that set minimum insurance benefit standards and offered low-cost sharing options for low-income individuals and families showed improved access to care and health security for residents. Both efforts will be essential for national reform.


