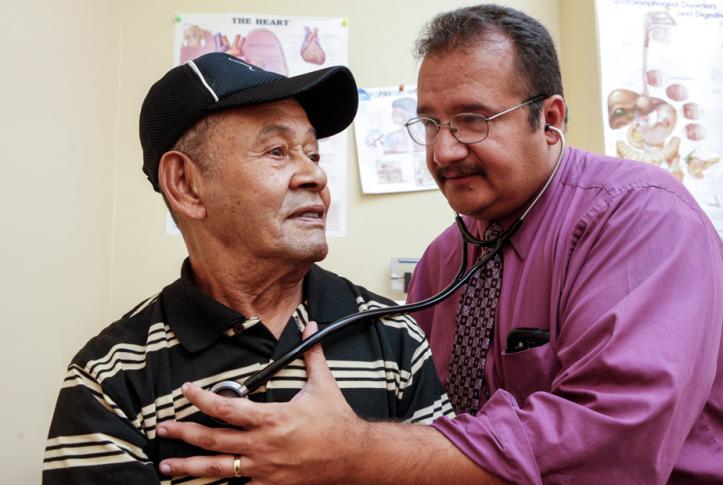
How would block-granting Medicaid work?
States would receive a fixed, preset amount of federal Medicaid funding—a block grant—each year to use to provide health coverage to their low-income residents. The federal contribution to state Medicaid programs in a given year would not change if the number of enrollees were to increase or if the cost of health care services were to rise. But it would likely rise annually by some amount, such as the rate of consumer inflation plus one percentage point.
What’s the backstory?
Over the years, Medicaid—the health care program for low-income Americans that is funded jointly by the federal government and the states—has employed a variety of targeted cost-containment measures to control spending. These include reforms to lower outpatient prescription drug costs, expand access to preventive care, and scale up managed care. Together, they have helped keep growth in spending per beneficiary comparable to or below Medicare or private insurance levels since the early 1990s.1
The primary reason that Medicaid spending grows is rising enrollment, which accounted for 71 percent of program growth between 1975 and 2012. In 2014, total Medicaid spending rose 8 percent, largely as a result of the Affordable Care Act’s (ACA) expansion of eligibility to people with incomes up to 138 percent of the federal poverty level (about $16,000 for an individual). Because the federal government fully covered the costs of these new enrollees, the federal portion of Medicaid spending grew 13 percent, although the state portion increased only 1 percent.
Still, some conservative policymakers believe Medicaid’s cost growth is too high. They are calling for across-the-board limits on the federal contribution to state Medicaid programs.
How does this differ from current policy?
To fulfill its mission as a health care safety net, Medicaid has historically relied on federal funding that rises in tandem with enrollment and states’ health care needs—as well as on contributions from states. This flexible funding approach allows Medicaid to address health care needs arising from economic or societal disruptions: a rise in poverty rates during a recession, the erosion of employer coverage for low-wage workers, longer life spans for people with serious disabilities, and natural or manmade disasters such as Hurricane Katrina or the September 11 terrorist attacks.
How would block grants affect states and adults who are currently Medicaid-eligible?
States already vary enormously in the proportion of low-income residents they deem eligible for Medicaid coverage and in the amount spent per enrollee. But when faced with budget shortfalls, it’s likely that all states would at some point deny Medicaid coverage to new applicants, even if they are eligible, or scale back benefits—or both. Again, that’s because federal block grants would likely not increase when the population in need grows or the underlying cost of health care ticks up. These cost increases affect all sources of insurance, including employer health plans.
An ACA repeal-and-replace bill introduced by Senate and House Republicans in 2015 would have ended funding for the Medicaid expansion for low-income adults and created block grants to states based on pre-expansion funding levels.2 RAND researchers Christine Eibner and Sarah Nowak estimated the proposed legislation would reduce federal spending by $62 billion in 2018, with much of the savings coming from a drop in Medicaid enrollment of 17.6 million people.