In the Literature
Patient-centered care—defined by the Institute of Medicine as "care that is respectful of and responsive to individual patient preferences, needs, and values"—is one of the key ingredients of health care quality. Professional, licensing, and regulatory bodies as well as board certification processes have begun to include patient-centered criteria. But how many physicians are currently practicing patient-centered care?
According to a new Commonwealth Fund study, the answer is "not enough." In "Adoption of Patient-Centered Care Practices by Physicians: Results from a National Survey" (Archives of Internal Medicine, Apr. 10, 2006), the Fund's Anne-Marie J. Audet, M.D., Karen Davis, Ph.D., and Stephen C. Schoenbaum, M.D., say that while physicians favor patient-centered care, only 22 percent scored high in incorporating such techniques into their day-to-day practices. Use of some patient-centered care practices—like providing same-day appointments to patients who request them—is common. But others, particularly those related to care coordination, team-based care, and information systems, have yet to take hold.
About the Study
The analysis was based on the Commonwealth Fund 2003 National Survey of Physicians and Quality of Care, a nationally representative study targeting primary care physicians (PCPs) and specialists likely to be involved in patient care over the long term. The survey focused on 11 specific patient-centered care practices: same-day appointments; e-mail with patients; reminder notices for preventive or follow-up care; registries of patients with chronic conditions; patient medication lists; electronic medical records; information from referral physicians promptly available; medical records/test results readily available when needed; patient survey data fed back to practice; patient ratings of care affecting compensation; information on quality of care of referral physicians available.
Audet and her colleagues rated physicians' patient-centered practice scores as low, medium, or high, based on the number of practices adopted. One-fifth (20%) scored in the low range (0–2 practices adopted), 58 percent in the medium range (3–5), and 22 percent in the high range (6–11).
Results
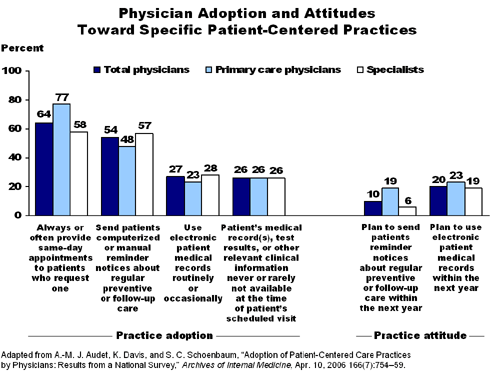
Access to care: Overall, 64 percent of physicians said they always or often provide same-day appointments, with PCPs more likely than specialists to do so (77% vs. 58%). Only 18 percent of all physicians use e-mail to communicate with patients, and only another 11 percent said they plan to use e-mail with patients in the next year.
Patient engagement: More than half (54%) of all physicians send reminder notices about preventive or follow-up care. A large majority (83%) of PCPs said they favor sharing medical records with patients.
Information systems: Only 42 percent of PCPs said it was very or somewhat easy for them to generate disease registries, and only 18 percent said the same about generating lists of patients who take high-risk medications that require closer follow-up. Fewer than one-quarter (23%) of PCPs currently use electronic medical records; another 23 percent plan to do so within the next year.
Care coordination: While 71 percent of PCPs reported they always or often receive timely information about referrals, 74 percent cited problems related to the availability of patients' medical records, test results, or other information at scheduled visits.
Team-based care: A large majority (87%) of PCPs think improved teamwork or communication among providers would be very or somewhat effective in improving quality of care.
Patient feedback: Only 36 percent of PCPs and 20 percent of specialists said they receive data based on patient surveys. About one-quarter (27%) said they were rewarded based on patient survey data.
Publicly available information: More than half (55%) of PCPs think that performance data should be shared with patients, but only 13 percent definitely agree with this proposition. Twenty-one percent of PCPs always or often have access to specialists' quality data when making referrals.
Conclusions
A gap exists between knowledge and practice—between physicians' endorsement of patient-centered care and their adoption of practices to promote it, the authors say. Physicians reported several barriers to their adoption of patient-centered care practices, including lack of training and knowledge (63%) and costs (84%).
Education, professional and technical assistance, and financial incentives might facilitate broader adoption of patient-centered care practices. "With the right knowledge, tools, and practice environment, and in partnership with their patients, physicians should be well positioned to provide the services and care that their patients want and have the right to expect,' the authors conclude.
Facts and Figures
- Physicians in practices of 50 or more were more likely to adopt components of patient-centered care than were solo physicians.
- While 73 percent of PCPs think that team-based care results in better care decisions, one-third (33%) thought the team process makes care cumbersome and 21 percent thought it increased the likelihood of medical errors.
- Only 2 percent of PCPs are paid for e-mail correspondence with patients.