An abstract is available at:
http://www.annals.org/cgi/content/abstract/149/12/854
Synopsis
A review of hospital discharge data in California revealed that interruptions in Medicaid coverage increased the risk of hospitalization for ambulatory care–sensitive conditions such as heart failure, diabetes, and chronic obstructive pulmonary disease, which can often be managed in an outpatient setting. Hospital admissions for these conditions may signal a decline in health status among patients who no longer have access to preventive and primary care services because of an interruption in their health care coverage.
The Issue
Interruptions in health insurance coverage are common in the United States. An estimated 85 million people younger than age 65, or 38 percent of the U.S. population, were uninsured for at least part of a recent three-year period. Low-income people are particularly at risk. Medicaid beneficiaries must demonstrate eligibility for benefits each year. In some states, this can be as often as every three months, making people especially vulnerable to such disruptions. (During most of the time this study was conducted, 1998 to 2002, California required beneficiaries to report on their eligibility every three months. The state has since reduced the frequency of eligibility determination.) Research suggests that people who experience interruptions in health coverage are less likely to receive primary and preventive care that could prevent hospitalizations.
Key Findings
- More than 60 percent of the 4.7 million Medicaid beneficiaries included in the analysis experienced some interruption in their health coverage during the study period. The average duration of an interruption in coverage was 25 months.
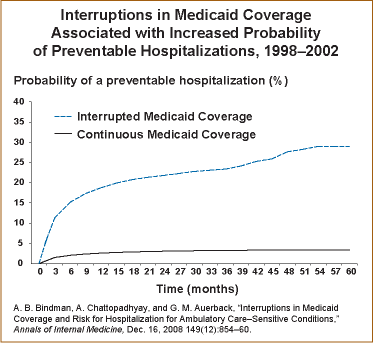
- Beneficiaries who experienced an interruption in Medicaid benefits had a substantially higher risk of hospitalization for ambulatory care–sensitive conditions than did those with continuous coverage.
- The majority of adults who had an interruption in their Medicaid coverage became uninsured and did not acquire another form of insurance.
- Patients who qualified for Medicaid through Supplemental Security Income (SSI) because of a chronic disability had more hospitalizations for ambulatory care–sensitive conditions than those who received benefits through Temporary Assistance for Needy Families (TANF). However, the TANF beneficiaries are more vulnerable to interruptions in Medicaid coverage than the SSI beneficiaries, who typically also have Medicare coverage that can preserve their access to primary care.
Addressing the Problem
 Public insurance programs can help significantly reduce the number of uninsured. But the administrative burdens they often place on beneficiaries can impede their success in reaching those in need. Policies that reduce the frequency of coverage interruptions could prevent hospitalizations and other events that trigger negative health consequences and high costs.
Public insurance programs can help significantly reduce the number of uninsured. But the administrative burdens they often place on beneficiaries can impede their success in reaching those in need. Policies that reduce the frequency of coverage interruptions could prevent hospitalizations and other events that trigger negative health consequences and high costs.About the Study
The study examined hospital discharge data for more than 4.7 million adults (ages 18 to 64 years) in California who were covered by Medicaid for at least one month between 1998 and 2002 and were hospitalized for an ambulatory care–sensitive condition. These conditions included asthma, angina, congestive heart failure, chronic obstructive pulmonary disease, dehydration, diabetes, hypertension, lower-extremity amputation, pneumonia, ruptured appendix, and urinary tract infection. The authors compared hospitalization rates among Medicaid enrollees with continuous coverage and those who experienced interruptions in their benefits.
The Bottom Line
Interruptions in Medicaid coverage are associated with a higher rate of hospitalization for ambulatory care–sensitive conditions, like heart failure, diabetes, and chronic obstructive pulmonary disease.


