Synopsis
According to a national survey, 28 percent of accountable care organizations (ACOs) have teamed up with community health centers, an indication that these safety-net providers are viewed by ACOs as valuable partners. ACOs with safety-net partners and those without are very similar in size, organizational structure, and the services they offer patients. But ACOs with community health centers have greater experience implementing reforms like care management programs, public reporting, and risk‐sharing, which may prove helpful in meeting ACOs’ goals of improving quality, cost performance, and population health.
The Issue
Community health centers (CHCs) provide primary care for some 22 million Americans, many of whom have low incomes, are in poor health, and live in medically underserved areas. Historically, CHCs have been somewhat isolated from other health care providers; doctors at safety-net clinics report difficulty obtaining appointments with specialists or nonemergency hospital care for their patients. As providers and insurers increasingly coalesce into ACOs and assume responsibility for the total cost and quality of care for their patient populations, the role of CHCs is unclear. If most ACO networks exclude safety-net providers, community clinics will be further segregated from the mainstream. On the other hand, the integration of ACOs and CHCs could bring better access to specialists, ambulatory care, and hospitals to underserved areas, while also increasing ACOs’ expertise in caring for high-need, high-cost patients. With Commonwealth Fund support, Dartmouth researchers set out to determine if, in fact, ACOs are contracting with CHCs for care delivery, and to compare the capabilities of ACOs with and without CHC partnerships.
Key Findings
Between 2012 and 2013, 28 percent of all ACOs contracted with a community health center. Researchers found that ACOs that included CHCs are similar to other ACOs in terms of organization, size, structure, and capabilities. But there are some key differences:
- ACOs with CHCs are slightly more likely to include nursing facilities and specialty groups than ACOs without health center partners.
- ACOs with CHCs more often have contracts with Medicaid and less often have contracts with commercial insurers. ACOs with CHCs have more experience with reforms intended to improve care and reduce costs, such as patient-centered medical homes, patient care management, and quality data reporting.
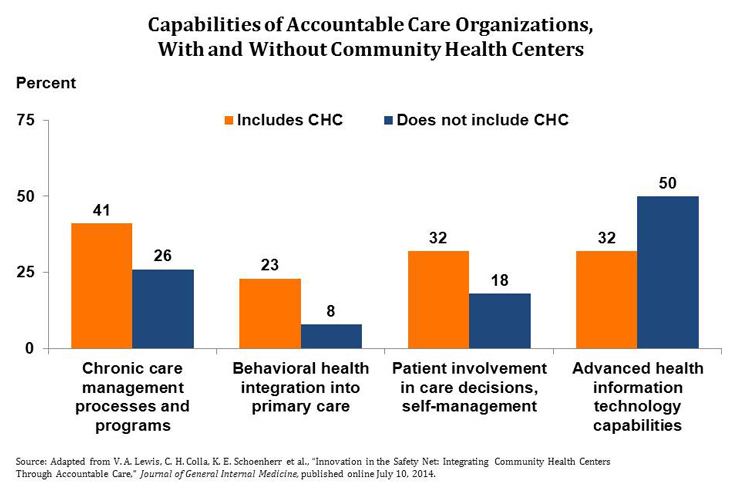
- ACOs with CHCs are more likely than those without to have integrated behavioral health into primary care (23% vs. 8%) and have chronic care management programs (41% vs. 26%).
- ACOs with CHCs had a harder time securing original funding to launch their organization (40% vs. 24%).
- ACOs with CHCs report having less-advanced health information technology, although their use of electronic health records was comparable to that in ACOs without health centers.
Looking Forward
It appears that a significant portion of accountable care organizations consider community health centers to be valuable partners that offer expertise in delivering coordinated services to patients with complex care needs. More research is necessary, the authors say, to see how these partnerships develop over time and if CHCs do in fact help ACOs advance the goals of higher-quality care and lower spending. The authors also recommend that Medicare and state Medicaid programs develop policies to facilitate the integration of community health centers with ACOs.
About the Study
"The move toward accountable care organizations provides one venue through which safety net primary care providers such as community health centers may integrate in new ways."
Researchers examined data from a national survey of 173 ACOs between 2012 and 2013 to determine the percentage that had community health center partners. Survey results were paired with in-depth interviews with executives from 18 ACOs as well as with 22 leaders from eight CHCs that participate in ACOs.
THE BOTTOM LINE
More than a quarter of accountable care organizations now include community health centers in their networks, a sign that key safety-net providers are being integrated into the broader health care delivery system.