New York City, June 25, 2003—As Congress debates Medicare proposals that would shift more beneficiaries into private insurance plans, legislators may first want to examine the often tumultuous history of the six-year-old Medicare+Choice program, Medicare's managed care alternative to its traditional fee-for-service program. According to a new policy brief from The Commonwealth Fund, many Medicare+Choice enrollees have been faced with a limited choice of plans in their area and instability in provider participation compared with fee-for-service Medicare, as well as significantly increased out-of-pocket costs—especially for those with chronic and disabling illnesses—and a confusing, complicated benefit structure
"Seniors may suddenly find that their physician is no longer a member of their plan or, if they have health problems, that their out-of-pocket costs have increased substantially," said Karen Davis, president of The Commonwealth Fund. "These are the realities of the health care marketplace, and we should be cautious about inflicting them on the elderly and disabled."
 The analysis, Lessons from Medicare+Choice for Medicare Reform, by Geraldine Dallek, an independent health policy consultant, and Brian Biles and Lauren Hersch Nicholas of George Washington University, provides seven lessons for the current debate:
Lesson #1: Private plans do not participate in many regions. Attracting private plans to some regions, particularly rural areas, has been difficult because of the small number of hospitals and physicians in these areas and their reluctance to contract with managed care plans. Only 13% of rural beneficiaries have an option of joining a Medicare+Choice plan.
Lesson #2: Premiums and benefits vary greatly by geographic area. Wide variation in premiums, benefits, and cost-sharing will undermine the promise of Medicare to provide the same health care benefits to beneficiaries no matter where they live. Enrollment-weighted average monthly premiums in Medicare+Choice plans ranged from $3 in New York City to $87 in neighboring Long Island in 2002.
Lesson #3: Participation by Medicare HMOs has been unstable. Because Medicare+Choice payments to participating plans are related to overall growth in traditional Medicare costs, rate increases have been limited in recent years, generally to 2 percent annually. With continued participation in the Medicare market less financially attractive, plans have reduced their service area or simply withdrawn from local markets altogether, disrupting health care for more than 2.4 million beneficiaries from 1999 to 2003. Any new Medicare program that depends on private plans is likely to face the same circumstances.
Lesson #4: Physician and hospital participation has been unstable. Medicare+Choice enrollees have experienced high rates of turnover in the physicians and hospitals that participate in their plans. Statewide primary care provider turnover rates ran as high as 33 percent in New Mexico in 2001. Nine of 36 states had Medicare+Choice primary care turnover rates of 20 percent or more, including plans in large states such as Florida, Illinois, and Texas.
Lesson #5: Medicare+Choice options are too complicated for many beneficiaries. Although choice of health plans is the cornerstone of competition in the private marketplace, the complicated range of choices in Medicare+Choice benefits and cost-sharing make it difficult for anyone-let alone elderly people with cognitive impairments-to make an informed choice. Medicare+Choice plans do not provide standardized benefit packages, so beneficiaries must choose between plans with wide variation in the benefits offered, including prescription drug coverage. Plans can differ greatly in the level of drug benefits provided, coverage of brand names or generics, copayments, and method of determining drug costs that count toward benefit limits.
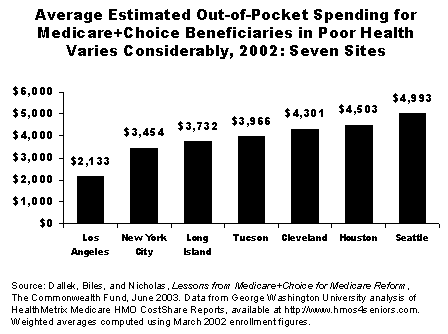
Lesson #6: Medicare+Choice plan design can discourage enrollment by high-risk beneficiaries. Medicare+Choice plans have historically enrolled healthier, lower-cost individuals than traditional fee-for-service Medicare. Moreover, private insurers increasingly show an interest in risk selection, encouraging enrollment by healthier beneficiaries. In particular, increases in cost-sharing for some services by some plans seem to be directly related to the fear of enrolling high-cost beneficiaries. Across the nation, plans have increased costs on specific services most likely to be used by enrollees with high-cost chronic conditions, such as hospital care, oxygen, dialysis, chemotherapy, and radiation therapy.
Lesson #7: Private plans are not less costly than traditional Medicare. While a major goal of private plans is to control growth in costs, the Medicare+Choice experience shows that private plans can increase program costs. Among the reasons are Medicare's need to increase payments to attract private plans in rural areas, as well as the higher administrative costs for Medicare+Choice compared with fee-for-service Medicare. It is difficult for private plans to offer additional benefits, cover marketing and administrative costs, and make a profit while at the same time pricing their products below the costs of traditional Medicare.
The analysis, Lessons from Medicare+Choice for Medicare Reform, by Geraldine Dallek, an independent health policy consultant, and Brian Biles and Lauren Hersch Nicholas of George Washington University, provides seven lessons for the current debate:
Lesson #1: Private plans do not participate in many regions. Attracting private plans to some regions, particularly rural areas, has been difficult because of the small number of hospitals and physicians in these areas and their reluctance to contract with managed care plans. Only 13% of rural beneficiaries have an option of joining a Medicare+Choice plan.
Lesson #2: Premiums and benefits vary greatly by geographic area. Wide variation in premiums, benefits, and cost-sharing will undermine the promise of Medicare to provide the same health care benefits to beneficiaries no matter where they live. Enrollment-weighted average monthly premiums in Medicare+Choice plans ranged from $3 in New York City to $87 in neighboring Long Island in 2002.
Lesson #3: Participation by Medicare HMOs has been unstable. Because Medicare+Choice payments to participating plans are related to overall growth in traditional Medicare costs, rate increases have been limited in recent years, generally to 2 percent annually. With continued participation in the Medicare market less financially attractive, plans have reduced their service area or simply withdrawn from local markets altogether, disrupting health care for more than 2.4 million beneficiaries from 1999 to 2003. Any new Medicare program that depends on private plans is likely to face the same circumstances.
Lesson #4: Physician and hospital participation has been unstable. Medicare+Choice enrollees have experienced high rates of turnover in the physicians and hospitals that participate in their plans. Statewide primary care provider turnover rates ran as high as 33 percent in New Mexico in 2001. Nine of 36 states had Medicare+Choice primary care turnover rates of 20 percent or more, including plans in large states such as Florida, Illinois, and Texas.
Lesson #5: Medicare+Choice options are too complicated for many beneficiaries. Although choice of health plans is the cornerstone of competition in the private marketplace, the complicated range of choices in Medicare+Choice benefits and cost-sharing make it difficult for anyone-let alone elderly people with cognitive impairments-to make an informed choice. Medicare+Choice plans do not provide standardized benefit packages, so beneficiaries must choose between plans with wide variation in the benefits offered, including prescription drug coverage. Plans can differ greatly in the level of drug benefits provided, coverage of brand names or generics, copayments, and method of determining drug costs that count toward benefit limits.
Lesson #6: Medicare+Choice plan design can discourage enrollment by high-risk beneficiaries. Medicare+Choice plans have historically enrolled healthier, lower-cost individuals than traditional fee-for-service Medicare. Moreover, private insurers increasingly show an interest in risk selection, encouraging enrollment by healthier beneficiaries. In particular, increases in cost-sharing for some services by some plans seem to be directly related to the fear of enrolling high-cost beneficiaries. Across the nation, plans have increased costs on specific services most likely to be used by enrollees with high-cost chronic conditions, such as hospital care, oxygen, dialysis, chemotherapy, and radiation therapy.
Lesson #7: Private plans are not less costly than traditional Medicare. While a major goal of private plans is to control growth in costs, the Medicare+Choice experience shows that private plans can increase program costs. Among the reasons are Medicare's need to increase payments to attract private plans in rural areas, as well as the higher administrative costs for Medicare+Choice compared with fee-for-service Medicare. It is difficult for private plans to offer additional benefits, cover marketing and administrative costs, and make a profit while at the same time pricing their products below the costs of traditional Medicare.


