Executive Summary
Employer-sponsored health insurance is the main source of coverage for working adults. Recently, there has been an erosion in both the proportion of workers covered under employer plans and the adequacy of such coverage, as rising health care costs have made it increasingly difficult for employers to continue offering comprehensive coverage.
Most workers who lose access to employer health insurance have few coverage options. Many turn to the individual insurance market, where coverage is often unaffordable—and sometimes unavailable—to older adults or people with health problems. For those families who continue to have employer coverage, ever-rising deductibles and other cost-sharing are consuming larger and larger shares of family income, particularly among families with low or moderate incomes.
The consequences are serious. According to this analysis of the Commonwealth Fund Biennial Health Insurance Survey, most adults who seek to purchase insurance coverage through the individual market never end up buying a plan, finding it either very difficult or impossible to find one that met their needs or is affordable. Compared with adults with employer coverage, adults with individual market insurance give their health plans much lower ratings, pay more out-of pocket for their premiums, face much higher deductibles, and spend a greater percentage of their income on health insurance premiums and health care expenses. Eight percent of adults ages 19 to 64 who are privately insured all year, or 8.5 million people, are covered through the individual insurance market. Only a third (34%), however, rate their coverage as excellent or very good, compared with over half (54%) of those enrolled in employer plans.
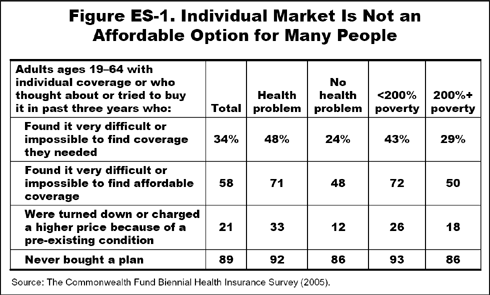
Other key survey findings on the individual insurance market include:
- Insurance in the individual market is often impossible to obtain or unaffordable. Nearly nine of 10 people who explored obtaining coverage through the individual market never bought a plan, citing difficulties finding affordable coverage or being turned down.
- More than half of adults with coverage through the individual market have annual premium costs of $3,000 or more, compared with one of five covered by employer plans.
- Two of five adults (43%) covered through the individual market spent more than 10 percent of their incomes on premiums and family out-of-pocket medical expenses, compared with one of four (24%) of those insured through employer plans.
Key survey findings on high-deductible health care plans include:
- Thirty-seven percent of those insured through the individual market have per-person deductibles of $1,000 or more, as do 8 percent of those insured through employer plans, for a total of 11 million people (8 million covered by employer plans and 3 million covered by individual plans).
- Individuals covered by high-deductible plans—either through the individual insurance market or an employer—have financial burdens. Of those adults with per-person deductibles of $1,000 or more, two of five (43%) spent 10 percent or more of their incomes on premiums and family out-of-pocket medical expenses, compared with one of five (22%) of those enrolled in plans with deductibles of $500 or less.
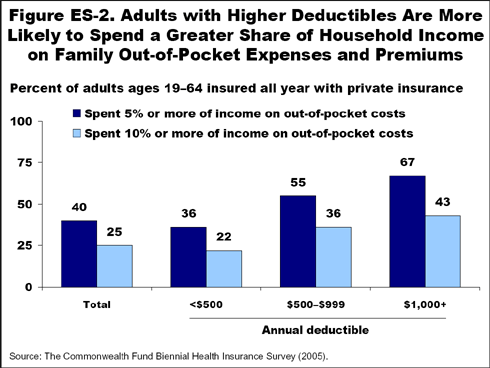
- Privately insured adults enrolled in high-deductible plans are less satisfied with coverage and care than those with lower deductibles. Forty-one percent of those with deductibles of $1,000 or more rated their coverage as fair or poor, compared with 15 percent of those enrolled in plans with deductibles of $500 or less. In addition, those with high deductibles were less satisfied with the quality of their health care. Only 29 percent of adults with deductibles of $1,000 or more said they were very satisfied with the quality of care they had received in the past 12 months, compared with more than half (54%) of adults with deductibles under $500.
- People with higher deductibles also are more likely to have problems getting needed care than those with lower deductibles. Forty-four percent of adults with deductibles of $1,000 or more reported one of four access problems: did not fill a prescription; did not see a specialist when needed; skipped a recommended test, treatment, or follow-up; or had a medical problem but did not see a doctor. Twenty-five percent of adults with deductibles under $500 cited similar access problems.
- Medical bill problems or accumulated medical debt were reported more frequently by those with higher deductibles compared with those with lower deductibles. Two of five (41%) of those with deductibles of $1,000 or more reported a medical bill problem or outstanding debt compared with one of four (23%) of those with deductibles of less than $500.
Some states, such as Maine, Massachusetts, and Vermont, have created new pooling mechanisms and have provided subsidies for lower-wage individuals to make coverage more affordable for those not insured under employer plans. Massachusetts and Vermont have taken the additional step of requiring some financial contribution from employers who do not provide coverage to their workers. By drawing upon the experience of these innovative states and others, policymakers at the national level may be able to devise effective ways to address this increasingly urgent problem.



