In less than one year, Medicare beneficiaries will be able to sign up for the new prescription drug plan, known as Part D. About 20 percent of potential enrollees will be eligible for subsidies, due to their low-income status. But how will others fare?
A new Commonwealth Fund–supported study estimates that, in the first year under the standard drug benefit, 38 percent of enrollees will be subject to the no-coverage gap, known as the "doughnut hole," and 14 percent will exceed the threshold of catastrophic coverage. Over three years, enrollees, on average, will incur out-of-pocket costs of 44 percent of their total drug spending. Enrollees with higher spending could pay as much as 67 percent of total costs.
In the article, "Riding the Rollercoaster: The Ups and Downs in Out-of-Pocket Spending Under the Standard Medicare Drug Benefit" (Health Affairs, July/August 2005), a research team led by Bruce Stuart of the University of Maryland, Baltimore, illustrates how Medicare's drug benefit design could have serious financial consequences for beneficiaries. Individual drug spending levels are highly persistent over time, the authors say, so beneficiaries who face the greatest gaps in coverage are likely to do so year after year.
The Doughnut Hole
In 2006, enrollees will pay all drug costs until meeting a $250 deductible, after which Medicare will cover 75 percent of costs until reaching an initial limit of $2,250. Enrollees will then enter the so-called doughnut hole, paying all drug costs out-of-pocket until they reach a catastrophic limit of $5,100. After that, enrollees will pay only 5 percent of costs. The cycle is repeated each calendar year, with deductibles increasing by $25 and the doughnut hole expanding by 9 to 10 percent, until reaching $5,066 in 2013.
Although there will be some options available that could provide partial coverage for expenses in the doughnut hole, beneficiaries generally will not have the option of purchasing coverage to offset their liabilities for these costs. New Medigap policies no longer will offer drug benefits, and other private coverage will not count toward the true out-of-pocket costs that determine eligibility for catastrophic coverage.
Methods
Using data from the 1998–2000 Medicare Current Beneficiary Survey, the study projects out-of-pocket costs for beneficiaries who are likely to enroll in Part D. It focuses on two subgroups: "high spenders," with projected 2006 drug spending above the initial benefit limit of $2,250; and "catastrophic spenders," with spending above the catastrophic threshold of $5,100.
Projected Out-of-Pocket Spending
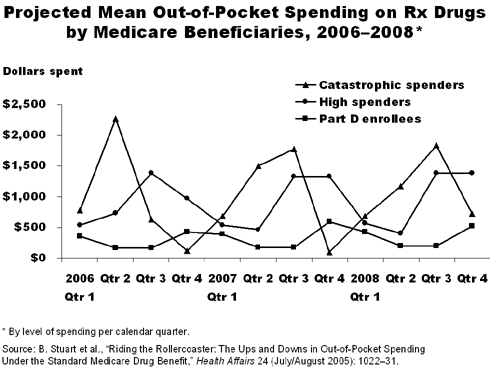
The authors estimate that quarterly out-of-pocket payments for someone with average prescription drug spending will vary from a low of $163 in the second and third quarters of 2006 to a high of $590 in the fourth quarter of 2007. High spenders will face much greater variation: their projected quarterly out-of-pocket payments will vary from $401 in the second quarter of 2008 to $1,391 in the third and fourth quarters of that year. A catastrophic spender will face out-of-pocket costs that range from a high of $2,276 in the second quarter of 2005 to a low of $95 in the fourth quarter of 2007.
Variation in out-of-pocket costs increases with drug spending—the higher the costs, the greater the ups and downs—illustrating what the authors describe as "riding the benefit rollercoaster."
Consequences of the Rollercoaster
According to the study, beneficiaries with average drug costs in 2006 will fare much better than the high-spender group, while catastrophic spenders will incur costs that fall in between those of the other groups. Enrollees will tend to face the same cost-sharing obligations from year to year. This may be beneficial for those with relatively low spending, but for high or catastrophic spenders, the benefit will exclude considerable portions of their drug bills. The study projects that an average high spender will incur drug bills of nearly $11,000 from 2006 to 2008. An average catastrophic spender will incur drug bills of $12,300 over those three years.
Policy Implications
For many, the cost-sharing obligations under Medicare's drug benefit will be an improvement over the coverage provided by standard Medigap policies or Medicare Advantage plans. But for some beneficiaries, out-of-pocket costs will increase. The authors suggest that the drug benefit could be restructured to meet the needs of all beneficiaries, perhaps by creating a uniform rate of coinsurance or capping the proportion of household income paid out-of-pocket for drugs.
In addition, they urge Congress and the Centers for Medicare and Medicaid Services to launch a public education campaign to help beneficiaries plan for the cost-sharing obligations under the new benefit.
Facts and Figures
- Over three years, Part D enrollees are projected to face average out-of-pocket drug costs of 44 percent of their total spending.
- Under the standard drug benefit, 38 percent of enrollees will hit the no-coverage zone known as the "doughnut hole," and 14 percent will exceed the threshold of catastrophic coverage.
- A high spender from a median-income household will spend 12.6 percent of his or her income on out-of-pocket drug costs from 2006 to 2008. A catastrophic spender from a median-income house-hold will spend 14.2 percent of income.