The growth in overall health spending, as well as Medicare spending, has slowed over the past few years, and that trend is beginning to affect long-term projections. As a result, the Congressional Budget Office (CBO) estimated last week that it would cost $138 billion to replace the formula used to determine Medicare physician fees, which is just about half their previous estimate from June 2012. The new, lower estimate provides an opportunity to replace the existing payment formula with an approach that promotes high-quality and efficient health care.
Congress enacted the Medicare payment formula, known as the sustainable growth rate (SGR), in 1997 to control spending growth. Under this formula, a target is set for physician spending in each year (based on annual increases in the gross domestic product), and automatic, across-the-board cuts in payment rates are triggered if those targets are exceeded. The formula has produced cuts in every year since 2002. 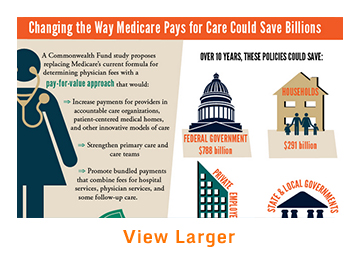
Concerned about potential disruptions in Medicare beneficiaries' access to care if physician fees were reduced, Congress has overridden those cuts annually since 2003—without changing the formula or addressing the underlying causes of spending growth. As a result, the scheduled cuts have accumulated and Medicare physician fees are now scheduled to be reduced by about 25 percent in January 2014. The high CBO "score"—the estimated increase in federal spending resulting from legislative action—has deterred Congress from repealing the SGR altogether.
CBO's reduction in the estimated impact of repealing the SGR offers a chance to pursue a new value-based approach to Medicare payment for physicians and other providers. A move away from the traditional fee-for-service payment model could produce savings that offset the net cost of repealing the SGR, while better aligning provider incentives with Medicare's goals of high-quality, efficient care.
The set of policies recently proposed by The Commonwealth Fund Commission on a High Performance Health System would replace the SGR formula with a broad-based policy that would:
- Maintain Medicare physician fees at their current level (including the current 10 percent payment increase for primary care) through 2023;
- Devote any new payments to supporting innovative payment and delivery system arrangements, such as accountable care organizations and patient-centered medical homes that offer coordinated, around-the-clock care;
- Recalibrate relative values for overpriced and underpriced services;
- Revise payments for other providers to better align payment and value;
- Enhance payment for primary care providers in patient-centered medical homes and for high-cost care management teams;
- Offer lower out-of-pocket costs for people with Medicare who designate and use primary care providers or, as appropriate, high-cost care management teams;
- Provide higher compensation for providers who participate in innovative, high-value health systems and perform well; and
- Make a single "bundled payment" for hospital episodes, including all physician services provided in the inpatient setting and related readmissions within 30 days, with postacute care also included in the bundled payment for selected conditions and procedures.
These proposals could produce estimated Medicare savings of $587 billion and federal savings of $788 billion over the next 10 years, more than offsetting the cost of repealing the SGR. They are part of a broader three-pronged systemwide strategy that would reform provider payment to support delivery system innovation, engage consumers by providing and encouraging high-value health care choices, and help health care markets reduce administrative costs by simplifying their policies and making them more consistent. These policies would involve all stakeholders in taking action to improve health and lower costs.
The Commission's recommendations would address the factors driving health care costs rather than cutting payments, reducing benefits, or restricting access to care for vulnerable populations. Although those strategies might achieve short-term savings, they will not solve the health system's long-term problems. Repealing the SGR and implementing payment reforms like those outlined here would be an important step in the right direction. The new CBO estimates should increase Congress' willingness to finally take on these important issues, and it should, indeed, strike while the iron is hot.



