The debate over Medicaid expansion is hardly new. It began in 2012 after the Supreme Court made expansion voluntary for states under the Affordable Care Act. On January 1, 2014, when the law’s coverage components became effective, 23 states immediately expanded Medicaid eligibility. In the years since, additional states have expanded their programs, and no state has dropped it. Today, 36 states are providing coverage through the expansion. (In addition, Nebraska has adopted expansion but not yet implemented.) The arguments for and against expansion have become familiar, but we are now in a starkly different time. A massive public health emergency and deepening economic crisis offer new and compelling reasons to reconsider Medicaid expansion.
The Health Crisis
First, of course, is the COVID-19 public health crisis, which has put everyone in the country at risk and placed extraordinary strain on our health care system. States are responding with their own resources; federal policymakers also have responded, providing new flexibilities and funding. Nonetheless, many states rightly wonder whether those funds will be sufficient.
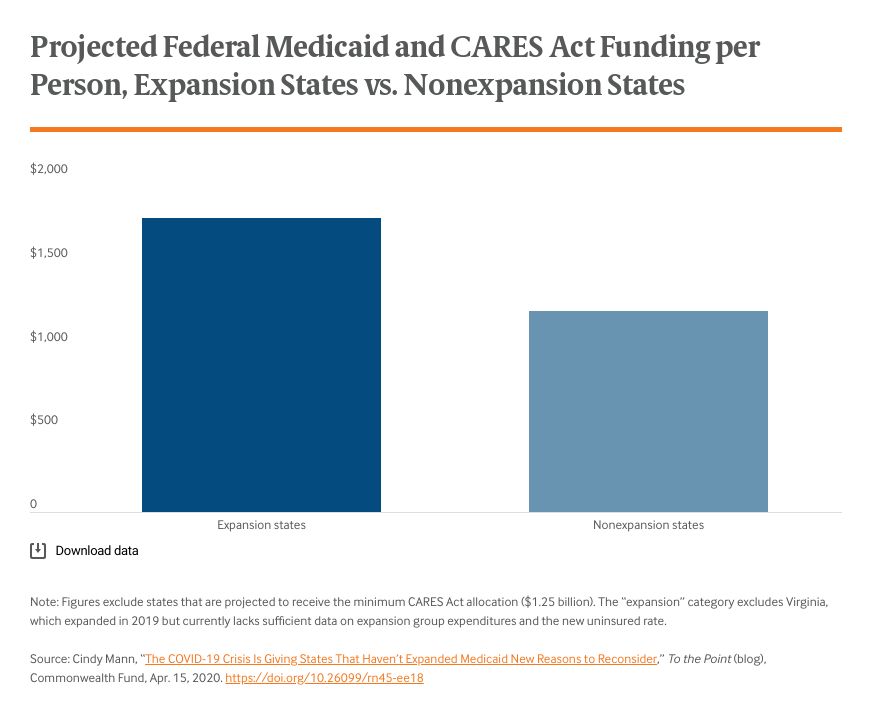
States do have one source of federal funding within their control that can directly address the crisis. Medicaid expansion, which has a 90 percent federal matching rate, offers states the ability to care for tens of thousands of residents. The fact that nonexpansion states are missing out on federal funding is not new. But now we have an urgent need for coverage and funds to pay providers. States that don’t take up the expansion face this crisis with considerably fewer federal resources. We calculated the federal dollars states will receive through the new Coronavirus Aid, Relief, and Economic Security Act (CARES) Act, which will be allocated to all states by population, along with the federal funding states receive through Medicaid. We found that expansion states will receive $1,755 in federal funding per state resident; in comparison, nonexpansion states will receive $1,198 per resident.1 Looking at states with similar populations, Kansas, which has not yet expanded, will receive $1,083 per state resident, compared to $1,436 per resident in its neighboring expansion state, Iowa.
A Rising Uninsured Rate and a Fragile Health Care System
The second new reason: millions of people are losing their jobs, income, and health insurance because of the crisis. As the uninsured rate skyrockets, states that have expanded Medicaid will be in a much stronger position. Medicaid expands when people lose their jobs and health insurance. But in nonexpansion states, millions of low-income parents and other adults will not qualify for coverage no matter how low their income. A recent study found that in states that have expanded Medicaid, the program covered 35.8 percent of all unemployed adults ages 19 to 64; in nonexpansion states, Medicaid reached only 16.4 percent of unemployed adults. As a result, the uninsured rate among the unemployed in nonexpansion states was nearly double the rate in expansion states (42.5% vs. 22.6%).
Timing and State Costs
It’s important to consider the timing of an expansion. Implementation could not happen overnight but experience with expansion and previous disaster-related coverage initiatives (e.g., post-Hurricane Katrina) suggests it could be put into place relatively quickly. This is particularly true if states streamline their requests for the purpose of initial implementation and the Centers for Medicare and Medicaid Services acts with the same level of urgency it has employed throughout this crisis. Expansion could come in time to address the current COVID-19 crisis, depending on how long the crisis extends and whether it recurs. And expansion certainly could be in place to address the economic consequences of the pandemic. Another concern is states’ costs, particularly as state revenues plummet. States have found that general revenue spending has not grown as a result of expansion because of offsetting savings and reliance on other sources of funding for the nonfederal share, such as existing or recalibrated provider fees.
States that have yet to expand Medicaid are forgoing billions of federal dollars that can cover the uninsured and dramatically reduce the losses sustained by hospitals and other health providers. The current public health crisis, skyrocketing number of uninsured, and fragility of our health care system offer compelling reasons for nonexpansion states to take another look.




