The COVID-19 pandemic has wreaked havoc on the U.S. economy and put countless businesses at risk of failure. The health care industry has been hit particularly hard because of drops in revenue driven by decreases in elective care, stay-at-home orders, and the costs of preparing for a pandemic, such as increasing hospital capacity and purchasing personal protective equipment. Recognizing these challenges, and the critical role the industry plays, Congress and the U.S. Department of Health and Human Services (HHS) acted quickly to support the health care system and frontline workers in three primary ways: provider relief funds, the Paycheck Protection Program, and the Medicare Accelerated and Advance Payment Program.
The support was intended to compensate providers for drops in revenue, shore up provider finances during the disruption, and preserve jobs. Lawmakers also recognized the importance of supporting the pandemic response itself, by: providing assistance to “hot spots,” supporting financially vulnerable providers who are least able to afford the additional costs of the pandemic, and ensuring access to COVID testing and services to the uninsured. But this wide range of goals has led to some confusion: Who should get relief funds? How much is enough?
A Closer Look at Provider Support
The CARES Act and Paycheck Protection Program and Health Care Enhancement Act provided the largest amount of funding for health care providers by appropriating a combined $175 billion to the provider relief funds. For context, Medicare spent $147 billion on inpatient services for all of 2019.
There was little to no guidance or established rules on how to distribute an investment of this size efficiently and effectively in a pandemic. As a result, HHS was left to determine how to best allocate these dollars.
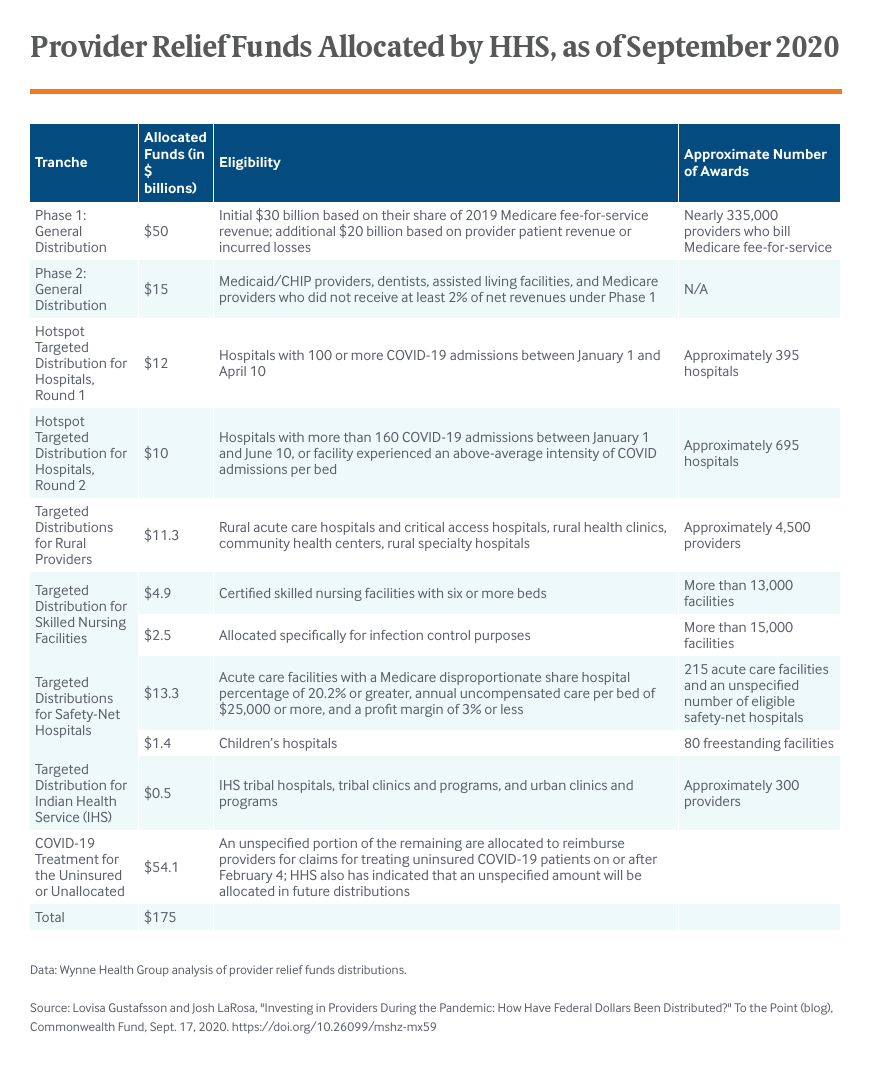
The dollars in the table, however, do not reflect what HHS has actually distributed to providers. According to data from the Centers for Disease Control and Prevention, providers have received approximately $78 billion thus far through the general and targeted funds. (Data on the separate dedicated uninsured fund is available here.) Unfortunately, these data do not show funding by provider type, so we are unable to discern whether certain providers have received adequate amounts and if others received more than necessary. The data also do not show the tranche that each disbursement came from, making it difficult to determine whether an individual tranche has funding remaining and how successful each has been in reaching intended recipients.
Congress also made loans available to small businesses, including health care providers, through the PPP. These loans do not need to be repaid if funds are used for payroll costs, interest on mortgages, rent, and utilities. Many smaller health care providers were eligible and in total received approximately $51 billion–$97 billion. (A more precise value is difficult to determine because the Small Business Administration did not provide exact dollar amounts for all loans.) These funds went to physician offices ($12 billion–$23 billion), dentists ($7 billion–$11 billion), and skilled nursing facilities ($4 billion–$8 billion), among others.
Beginning in late March, the Centers for Medicare and Medicaid Services accelerated more than $100 billion in payments to increase cash flow to Medicare providers and suppliers. More than 80 percent went to hospitals. These advanced payments can be deducted from future Medicare billings from the provider. Funds were intended to address cash flow issues resulting from a reduced number of admissions, procedures, visits, or delays in billing or processing. Many stakeholders are urging lawmakers and the administration to reduce or eliminate the interest rate owed on these payments.
Looking Forward
Health care providers have faced unique challenges given their COVID caseloads, patient demographics, and underlying financial positioning. Many hospitals, especially for-profit and the largest systems, are staying afloat, some even reporting better financials than in other years. In contrast, community-based providers that primarily serve Medicaid patients (e.g., pediatricians and behavioral health providers) continue to experience significant losses and have not benefited from any targeted distribution.
The pandemic is ongoing. Despite the investments already made, there are still large unmet needs among providers, patients, essential workers, and communities. HHS has not distributed the full allocated amount of the provider relief funds. Some stakeholders are concerned that current funding won’t cover the costs of uninsured patients. There also is concern that the distributions leave providers that mostly serve Medicaid patients at risk of closing their doors. And, as new hotspots emerge, providers at the frontlines will need access to additional rounds of funding. Arizona, Florida, Texas, and California have received some of the lowest amounts of funding per COVID-19 caseload, though they have recently emerged as hotspots.
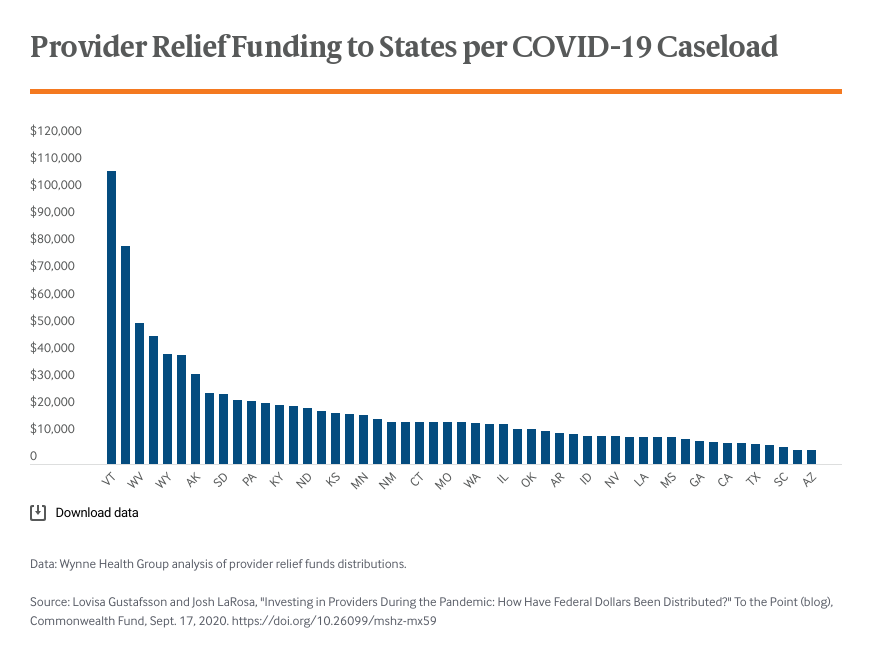
The federal government has made efforts to make the funding transparent, but it remains difficult to determine whether distributed amounts have been sufficient and if certain providers are slipping through the cracks. To effectively craft a fourth COVID funding package, Congress and other key stakeholders — including states that are obligated under law to ensure access to care through their Medicaid programs — need information on the current status of distributions. Specifically, they need to know how allocation decisions have been made, which dollars have been distributed, and which providers have received funds. Making these data transparent can help stakeholders assess if funds are meeting intended goals and if additional funding is needed. In addition, accurate data on the financial health of institutions can help target relief dollars to the providers who most need it.


