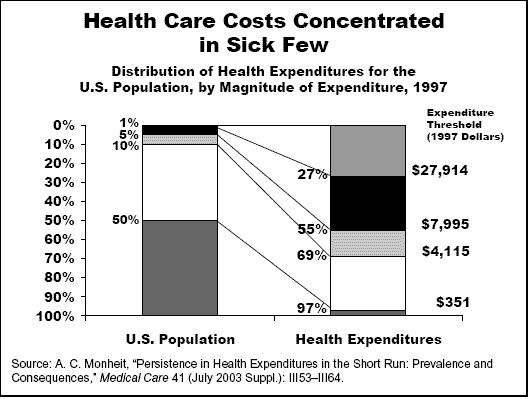
New York City, August 19, 2004—Consumer-directed health care (CDHC)—high-deductible plans often touted as the answer to spiraling health care costs—is not likely to curb health care costs, and could even worsen health outcomes by reducing patients' receipt of needed preventive care and care for chronic conditions, says a new report from The Commonwealth Fund. A more effective and equitable alternative to increased cost-sharing for patients would be care management for high-cost patients, says Commonwealth Fund President Karen Davis in Will Consumer-Directed Health Care Improve Health System Performance?, noting that ten percent of individuals account for 69 percent of health care costs. The key missing element in consumer-directed health care plans—which generally consist of a high-deductible health plan combined with a health reimbursement account (HRA)—is any strategy that would promote high-quality care. To effectively slow health care cost increases, health care plans will need to reward providers of high-quality care and efficiency, and better manage care for patients with costly conditions. "Longer-term solutions aimed directly at the root causes of higher costs are needed to improve health system performance and to achieve better quality, safety, and efficiency of care provision," says Davis.
- Studies in both the U.S. and Canada find that increased cost-sharing for prescription drugs led to a reduction in filling prescriptions known to be effective in controlling chronic conditions
- Healthier, higher-income individuals are more likely to enroll in CDHC plans, leaving sicker and lower-wage employees in higher-cost plans.
- While reenrollment in CDHC plans is high-about 90 percent-only about 30 percent of enrollees would recommend the plans to others.
- Public reporting of cost and quality data
- Investment in IT
- Development of guidelines and standards
- Rewarding high-quality performance including better management of high-cost conditions
- Investment in health care quality research by the federal government