Executive Summary
Serious budget problems have recently forced all 50 states to implement cost-containment strategies in Medicaid and other public insurance programs. In early 2003, the Oregon Health Plan (OHP) implemented cost-saving strategies of its own. OHP increased premiums, reduced benefits, and implemented copays for a substantial portion of its members. OHP also eliminated premium exemptions and instituted a six-month lockout policy for those who missed premium payments. In 2004, OHP rolled back some of these changes, eliminating copays and reintroducing some benefits.
To help understand the impact of Oregon's policy redesign on Medicaid beneficiaries, the Oregon Health Research and Evaluation Collaborative (OHREC), a unique public–private partnership of health care researchers, launched a longitudinal cohort study in March 2003. This ongoing study follows a representative sample of individuals who were enrolled in OHP when the initial wave of changes occurred. The study's objectives are to assess the short- and long-term effects of changes to premiums, cost-sharing and benefit structures in five key areas: beneficiaries' health care coverage, access to care, utilization of services, financial well-being, and overall health status.
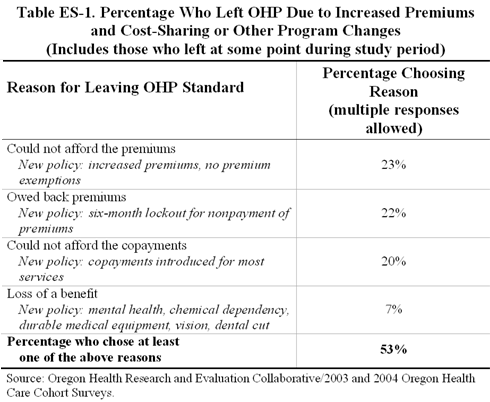
The study findings so far suggest that even small changes to premiums, cost-sharing, or benefit structures can have a dramatic effect on enrollment. After the initial cost-sharing increases and benefit reductions, nearly two-thirds of individuals surveyed had lost their coverage, many as a direct result of the increased premiums and cost-sharing. Those who left the program because of the premium and cost-sharing policies reported worse access to care, less primary care utilization, more emergency department utilization, and greater financial hardships than those who remained enrolled or left OHP for other reasons.
Among those who left OHP and did not find other insurance, overall health status declined over the course of the study. The unemployed and those with very low incomes were hardest hit. All of these effects were evident 18 months after the initial policy changes.
Analysis of gaps in coverage for those who left OHP suggest that the most severe impacts associated with loss of coverage may be reduced considerably if coverage is restored, or new coverage can be found, within three to six months.
As other states and the federal government move to increase premiums or cost-sharing as a means of controlling Medicaid expenditures, they will need to consider the impact those changes might have on such critical areas as health care coverage, access to care, utilization of care, and individuals' financial well-being.