Medication errors are the most common cause of preventable injuries in hospitals. Computerized physician order entry (CPOE) systems can reduce the incidence of serious medication errors by 55 percent, but only 10 percent to 15 percent of hospitals use them. While previous studies have described some of the challenges regarding CPOE implementation, it is still unclear what hospitals can do to overcome these challenges.
In their article, "Overcoming Barriers to Adopting and Implementing Computerized Physician Order Entry Systems in U.S. Hospitals" (Health Affairs, July/August 2004), researchers from Harvard Medical School and Brigham and Women's Hospital, with support from The Commonwealth Fund, interviewed top management officials at U.S. hospitals to identify the barriers hospitals face in adopting and implementing CPOE systems and strategies for overcoming these barriers.
Data and Methods
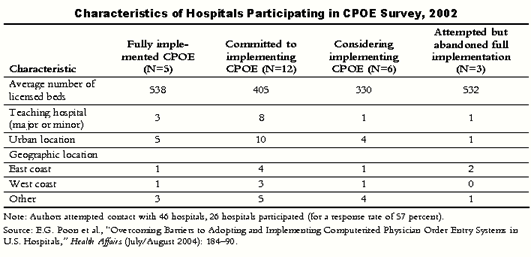
The researchers defined CPOE as an electronic application used by doctors to enter orders for medications, diagnostic tests, and ancillary services. They established a database of 72 hospitals and divided them into five categories, each relating to a different stage of CPOE implementation. Then the researchers randomly selected hospitals in each category and interviewed their top managers, although they were unable to recruit hospitals that were not considering CPOE. They conducted 56 interviews at 26 hospitals between February and July 2002.
Barriers and Strategies to Overcome Them
Physician and organizational resistance was one of the top barriers cited in the interviews. Physicians seemed to believe that CPOE systems would create more work and that the traditional paper-based ordering method was faster. Some hospitals abandoned implementation plans, fearing that physician resistance could escalate to a point of "physician rebellion." The interviewers also noted low levels of computer literacy among some physicians and a lack of user involvement in implementation processes. To overcome this resistance, the study points to several strategies, including establishing strong, committed hospital leadership that is facile at managing change, identifying physicians who will champion CPOE and encourage other physicians, addressing workflow concerns by providing training, and involving younger, computer-savvy physicians in the implementation process.
Another barrier to implementation and adoption is the high cost of implementing CPOE. Prior studies have estimated that the cost of CPOE has ranged from $3 million to $10 million, depending on hospital size and level of existing IT infrastructure. The high costs, coupled with the uncertainties associated with CPOE projects, could lead hospital officials to focus on competing, visible priorities, like building a new hospital wing. To offset this financial challenge, the interviewees in the study suggest realigning the hospital's priorities to focus on patient safety. By making patient safety part of the mission, hospitals can turn CPOE into mission-critical projects. Another strategy is to leverage external influences, like public outcry against medical errors and the threat of market share loss, as motivators in the push to adopt CPOE. Additionally, hospitals can point to the improved efficiencies that successful CPOE implementations can bring to institutions.
In addition to these internal tactics to overcoming costs, U.S. health care can also look to external approaches. In the interviews, hospital officials said that CPOE could be made more affordable by improving system interoperability. Because CPOE systems have to interface with other, existing IT systems in hospitals, managers are forced to either purchase CPOE from their primary vendors, even if the products do not meet their needs, or to rebuild their entire IT infrastructures around new CPOE vendors. If CPOE vendors adopted standards, hospitals could build their systems over time, without fearing obsolescence. Some interviewees thought that government influence could have an impact on the cost barrier, either by imposing standards that hospitals and vendors would readily adopt or by providing financial incentives in the form of grants or loans to defray costs or in increased reimbursements to hospitals that meet certain CPOE standards.
The final barrier cited in the study is product and vendor immaturity. Hospital managers noted that many vendor products did not fit the needs of their institutions and required extensive software modifications. They felt other products were underdeveloped, others were soon to become obsolete, and others were produced by companies without CPOE expertise. To tackle this challenge, the interviewees suggest selecting vendors who are committed to the CPOE market, ready to identify hospital workflow issues and adapt their products accordingly, and committed to long-term relationships with hospitals, as the process can take several years.
Conclusions and Policy Implications
The researchers found that physician resistance was cited repeatedly by interviewees as an impediment, more than the issue of cost. Therefore, they believe that efforts must focus on rallying physicians' support behind CPOE. Cost issues, also a major impediment, could be defrayed by differential reimbursements from payers that could be passed on to physicians, by encouraging malpractice insurers to discount rates for physicians who use CPOE, or by issuing governmental or commercial grants or loans to assist hospitals in implementation.
Outside the hospital, the researchers also identified opportunities for policymakers to promote CPOE adoption. They should do this by exerting pressure on hospitals to improve patient safety. In terms of defraying the cost issue, they should encourage public and private payers to provide financial incentives to institutions adopting CPOE systems and should provide access to capital through loans or grants. In addition, they should promote standardization to help improve interoperability of CPOE systems and encourage and support research that addresses the barriers to CPOE adoption.
Widespread CPOE implementation will take time, and the process is difficult and marked by challenges. However, policymakers have many opportunities to speed nationwide adoption of this proven patient-safety intervention.


