The new Medicare Part D prescription drug benefit entails big changes for nursing home residents. Those residents who had prescription coverage under another program, like Medicaid or Medigap, must now switch their coverage to a private Part D plan. For others, like the one of five nursing home residents who had no drug coverage at all in 2001, Part D offers welcome assistance. Even with its deductibles, coinsurance, and coverage gap, Part D should provide "considerable financial relief" to many residents, say the authors of a new study.
In "Coverage and Use of Prescription Drugs in Nursing Homes: Implications for the Medicare Modernization Act," (Medical Care, March 2006), the University of Maryland's Bruce Stuart, Ph.D., and colleagues examine the former sources of drug coverage for Medicare beneficiaries residing in nursing homes and explore how this coverage affected their use of medications.
Sources of Drug Coverage
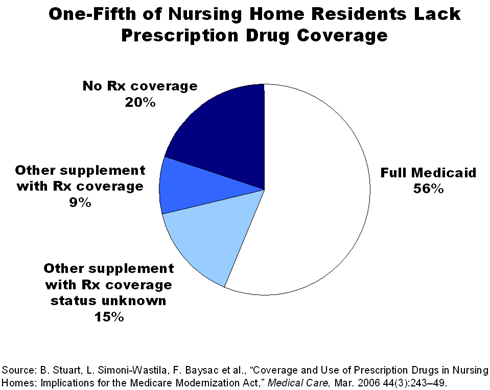
Using data from the 2001 Medicare Current Beneficiary Survey, augmented with information about residents' prescription medications, Stuart and his fellow researchers analyzed drug coverage and use for 789 nursing home residents. They found that more than half (56%) of the sample had drug coverage through traditional Medicaid or low-income Medicare programs. Another quarter (24%) had another source of prescription drug coverage, but one of five residents (20%) had no drug coverage at all in 2001.
No Difference in Drug Use by Coverage Status
In examining drug utilization, the research team estimated that residents used a mean of 5.7 unique prescription drugs per month. Perhaps surprisingly, this estimate did not vary significantly by drug coverage status: the utilization rates for those with and without coverage differed by less than half a prescription. Furthermore, the difference ran counter to the standard economic premise that beneficiaries with drug coverage would use more drugs. The mean utilization rates for those with and without coverage was, respectively, 5.7 and 6.1 drugs per month.
The finding that at least 20 percent of Medicare beneficiaries in nursing homes had no prescription drug coverage is unexpected, say the authors. "[T]here is a much greater need for Part D drug coverage among nursing home residents than commonly thought," the authors conclude. In addition, they say many residents will likely qualify for the subsidized coverage that is available to those with incomes less than 150 percent of the federal poverty level.
Given the high utilization rates among tesidents without coverage (6.1 prescriptions per month in 2001), the Medicare drug benefit should provide substantial assistance, the researchers say. Still, Part D coverage is unlikely to raise the total level of drug use in nursing homes—news that may be surprising to economists, but not to physicians and pharmacists who practice in these facilities. That's because government regulations on nursing homes, and the cognitive and physical impairments that afflict so many residents, preclude residents from having significant input into which prescriptions they take.
Conclusions
The Medicare drug benefit will mean big adjustments, not just for beneficiaries, but for the long-term care pharmacy industry. Through various mechanisms to control spending—formularies, prior authorization, mandated generic prescribing—private drug plans have the ability to change the quality of drug therapy in nursing homes. This could result in reduced access to specific medications and changes in utilization patterns, say the researchers.
Furthermore, the Medicare Modernization Act specifically excludes certain medications, like barbiturates and weight gain drugs, that are commonly prescribed to nursing home residents. Other programs, like Medicaid, can choose to cover these drugs, but they will forgo federal matching funds, the authors warn, if they choose to do so.
Facts and Figures
- More than 80 percent of all nursing home beds in the United States are served by specialized long-term care pharmacies.
- More than one-third of nursing home residents have incomes below the poverty level.
- More than two of five residents (44%) had both Medicaid and other supplemental coverage during 2001, although not necessarily at the same time.