Access to the full article is available at: http://content.healthaffairs.org/cgi/content/abstract/28/4/1145
Synopsis
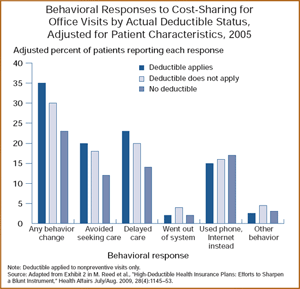 Americans enrolled in deductible-based health insurance plans are more likely than those with no deductible to alter their care-seeking behavior—including delaying or avoiding care—according to a survey of 1,515 members of Kaiser Permanente California, an integrated delivery system. This was true even in cases where the services were exempt from the deductible, indicating that patients did not understand their deductible plan details.
Americans enrolled in deductible-based health insurance plans are more likely than those with no deductible to alter their care-seeking behavior—including delaying or avoiding care—according to a survey of 1,515 members of Kaiser Permanente California, an integrated delivery system. This was true even in cases where the services were exempt from the deductible, indicating that patients did not understand their deductible plan details.
The Issue
Enrollment in high-deductible health insurance plans and other plans with substantial cost-sharing has been growing. While seeking to encourage consumers to use care more judiciously, these plans can have unintended clinical and economic consequences, particularly if consumers do not have the knowledge or tools to make prudent decisions in seeking health care. This study sought to learn how well consumers understand the often complex benefit structure of their plan and how their care-seeking behavior is affected by cost-sharing.
Key Findings
- In the survey, 52 percent of members of Kaiser Permanente California with medical deductibles knew they had a deductible; 35 percent of those individuals knew the amount of their deductible, and only 5 percent knew all of the services applicable to it. In contrast, 88 percent of those without a deductible were aware they did not have one.
- About 39 percent of respondents with deductibles reported they had altered how they sought care from the emergency department because of out-of-pocket costs—most frequently, by delaying or avoiding care, or by using the telephone or Internet to consult with a provider—compared with 27 percent of those without deductibles. Younger or sicker and nonwhite respondents were more likely to report behavior change.
- Of those respondents whose plan exempted office visits from the deductible, an estimated 30 percent reported cost-related changes in their care-seeking behavior, compared with 23 percent of members without a deductible.
- Among those with deductibles that included medical tests, 30 percent reported cost-related changes in their care-seeking behavior. Meanwhile, an estimated 12 percent of members who had deductibles that exempted medical tests reported cost-related changes in behavior.

Addressing the Problem
Health insurance deductibles can create "powerful yet potentially indiscriminate and blunt incentives for consumers to alter their care-seeking behavior," the authors say. To align cost-sharing incentives with treatment goals, consumers require more informational and decision support, according to the authors, to understand their plan’s benefits and "differentiate when care is necessary, discretionary, or unnecessary."
About the Study
A stratified random sample of members of Kaiser Permanente California, a prepaid integrated delivery system, was interviewed by telephone beginning in January 2006. Interviewers ascertained members’ knowledge of various cost-sharing structures, including whether they had a deductible and which services applied to the deductible, as well as how out-of-pocket spending affected decisions to seek emergency department visits, medical tests, and office visits. Responses from enrollees in various deductible plans were compared with those from members enrolled in plans without deductibles.
The Bottom Line
Complex benefit design and poor understanding of plan benefits can lessen the intended effects of cost-sharing in reducing enrollees' unnecessary use of services, as well as limit protection against unintended effects of exempting preventive care and other selected services.


