Synopsis
Low-income adults often cycle in and out of the Medicaid program when their income or life circumstances change. As a result, they face disruptions in care that put them at risk for poor health outcomes. Two policy options—extending coverage until the end of a calendar year or for 12 months following enrollment—are effective in reducing this “churning.”
The Issue
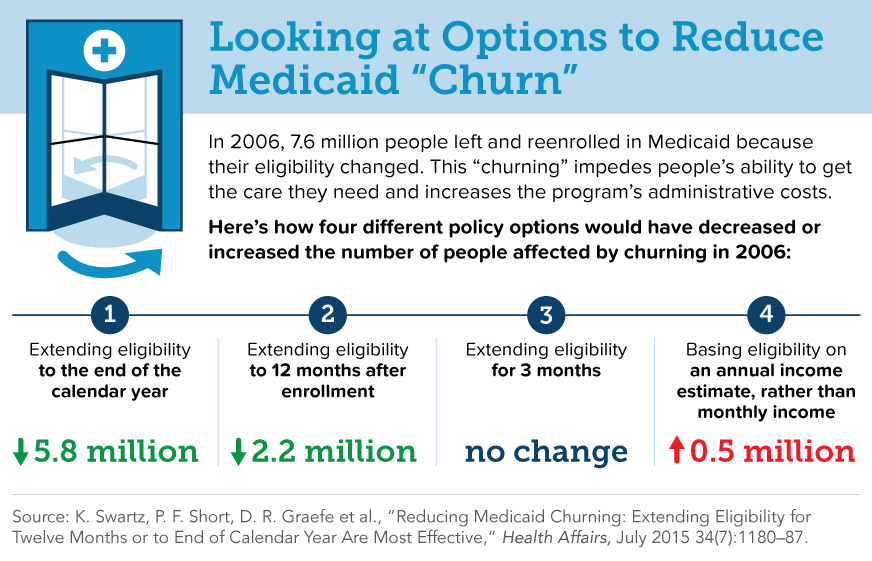
Because eligibility for Medicaid is determined by current monthly income, many beneficiaries temporarily lose coverage when their seasonal employment or overtime pay increases—and later requalify when their income dips. This churning in enrollment places administrative burdens on states and Medicaid managed care plans. The authors of this Commonwealth Fund–supported study looked at four policy options for addressing the problem and simulated their impact on churning and enrollment. The options include: 1) extending coverage to the end of the calendar year; 2) granting coverage for 12 continuous months, regardless of changes in income or life circumstances; 3) basing eligibility on an estimate of annual income; and 4) extending coverage by three months when a change in income or life circumstances causes a loss of eligibility.
Key Findings
- Extending coverage until the end of the calendar year reduced churning by 78 percent and virtually eliminated the administrative burden on states and Medicaid managed care plans. But by stabilizing access, it increased the number of adults covered all year by 50 percent and increased the average monthly caseload by 14 percent.
- Offering 12 months of continuous coverage was less effective, reducing churning by 30 percent. This option increased enrollment throughout the year by 20 percent and raised the average monthly caseload by 17 percent. Because churning and average monthly caseloads are higher, this option may be more expensive than extending coverage until the end of the calendar year.
- A three-month extension of eligibility had virtually no impact on churning yet produced a 4 percent increase in enrollment throughout the year and an increase in the average monthly caseload of 3 percent.
- Estimating annual income to determine eligibility increased churning by 5 percent while increasing enrollment by 7 percent and the average caseload by 4 percent.
The Big Picture
"States should consider implementation of the option that best balances costs while improving access to coverage and, thereby, the health of Medicaid enrollees."
States seeking to reduce churning in Medicaid enrollment will face trade-offs between ensuring continuity of care and controlling health care expenditure growth resulting from improved access. Some of the expected spending increases may be offset by reductions in administrative costs related to churning—estimated at $400 to $600 per enrollee—and by reducing expenditures on hospital care that could be avoided with better ongoing care. How states view this cost trade-off may depend on their financial solvency, their willingness to extend eligibility to low-income residents, and the amount of churning they currently experience.
About the Study
The authors relied on data from the U.S. Census Bureau’s Survey of Income and Program Participation to predict how changes in monthly income would influence eligibility, assuming all states opted to expand Medicaid eligibility to those whose income was at or below 138 percent of the federal poverty level. The findings described here were based on the assumption that 85 percent of those eligible would opt into the program and that 15 percent would experience a disruption. The authors also simulated the effect of different opt-in and disruption rates.
The Bottom Line
Extending Medicaid coverage to the end of the calendar year would maximize the number of people covered by the program and produce the least disruption to beneficiaries.