Under the 2008 Maryland Kids First Act, Maryland is using state income tax forms to identify families with children who may be uninsured and eligible for Medicaid or CHIP and sending them information about how to enroll. Maryland's experience could provide important lessons for the many states that are considering and/or developing similar outreach strategies. The Act, signed in May 2008, requires the Medicaid and CHIP programs to coordinate with the state comptroller, who oversees state tax collection.
"Collaboration between the Medicaid and CHIP programs and the comptroller presented valuable new opportunities for outreach to potential enrollees, but also involved challenges that the agencies are continuing to address as the new approach evolves," said Charles Milligan, executive director of the Hilltop Institute at the University of Maryland, which is evaluating the Kids First Act under a SHARE (State Health Access Reform Evaluation) grant from the Robert Wood Johnson Foundation. The evaluation is focusing on how the Act was established and implemented, how well it is identifying and enrolling eligible children, and the advantages and disadvantages of using tax form information to reach potential Medicaid/CHIP enrollees.
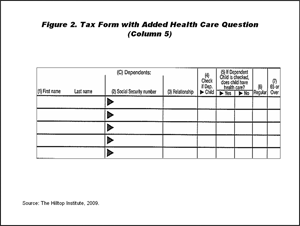
The comptroller was responsible for developing the language to include on the tax form, which for 2009 and 2010 tax returns asks individuals who report having dependent children the following: "Does child have health care?" (Figure 2). Due to space limitations, no detailed information about existing insurance coverage is collected on the tax form. There is no penalty for not answering the question about health care, and when parents leave it blank their children are counted as not having coverage. The approach is designed to be overly inclusive in order to maximize the number of potentially eligible children identified.
Figure 2. (Click to view)
After tax forms are submitted, the comptroller's office sends a mailing to taxpayers who reported having dependent children without health care and whose income falls within program eligibility (at or below 300 percent of the FPL). The mailing includes a cover letter developed by the Medicaid/CHIP program informing families that their children may be eligible for Medicaid or CHIP and asking for more detailed information about existing health insurance coverage. It also includes a Medicaid/CHIP application to be returned to that program.
Early results of the evaluation suggest that broad political commitment, as well as effective collaboration between Medicaid, the health department, and the comptroller's office, were important to the passage and implementation of the Kids First Act. Maryland's governor made the initiative a priority, and it also benefited from significant support in the state legislature and from the state comptroller.
Tax returns for 2008 identified 338,495 children who did not have health care, while 855,296 children did have health care, out of a census estimate of 1.5 million children in the state. It is still too early to estimate how many children have enrolled in public programs as a result of the tax form outreach strategy.
Challenges and Opportunities
The usefulness of income reported on tax returns for determining Medicaid/CHIP eligibility is a critical issue for the future of Maryland's—and other states'—outreach efforts. Major questions include whether annually reported income is too crude a measure for tracking children's eligibility, since income may change on a seasonal or monthly basis over the course of the year. Similarly, it is not clear whether reported income is an adequate proxy for eligibility, given that it may be subject to deductions and "disregard" rules.
The logistical and operational details of implementing the new system also made it more costly than anticipated, and presented practical challenges. The mailing costs associated with the outreach were much higher than they would have been for a more narrowly targeted effort. The new system required updates to the tax forms and to the comptroller's data systems to track responses to the new question as well as Medicaid eligibility thresholds. The wording of the question added to the tax form was vague (asking about "health care" rather than "health insurance") and did not ask for the age of the child or specify a time period, which could affect the accuracy of responses. The state is exploring how to modify the language on the tax form and other materials to elicit more accurate responses. Early evaluation has highlighted the importance of communication and problem-solving among stakeholders for addressing the operational challenges of implementing this kind of strategy.
Another critical issue involves the sharing or merging of tax and Medicaid/CHIP data systems. Data sharing between Medicaid and the comptroller could help target outreach by eliminating mailings to children that Medicaid data show are already enrolled. Data sharing would also enable the state to determine which enrollments result from this tax form–based outreach. However, current Maryland state tax laws strictly protect the privacy of taxpayers' financial information. And prior to the passage of the Children's Health Insurance Program Reauthorization Act of 2009 (CHIPRA), the Maryland Attorney General determined that state and federal confidentiality laws did not allow data sharing. CHIPRA encourages states to adopt Express Lane eligibility, which uses eligibility information for other state benefits—such as food stamps or Temporary Assistance for Needy Families—to satisfy some of the Medicaid or CHIP eligibility requirements. CHIPRA includes a provision that explicitly permits information-sharing across state agencies to enroll children in Medicaid or CHIP, "notwithstanding any other state or federal law." This suggests that Maryland could revisit its tax data-sharing laws, and potentially use parental consent on the tax form to make data-sharing possible. This approach could get more attention in states and nationally if it proves successful in Maryland.
Despite reductions in Maryland's Medicaid budget, this outreach strategy continues to move forward. The existence of legislation requiring and appropriating funds for the effort, and the strong support of the comptroller and governor, help ensure that it will continue.
|