By Karen Davis and Kristof Stremikis
As U.S. federal policymakers embark on the much-needed expansion of our system of health insurance coverage, it is important to also examine how we organize and deliver health services. Looking closely at delivery will ensure both the best possible health outcomes for Americans and the most value for what we spend on health care.
Today, the U.S. health care delivery is disorganized and rife with examples of missed opportunities and waste. The high rate at which patients are readmitted to the hospital within 30 days of discharge is particularly alarming. Working within a payment system that doesn't encourage quality or efficiency, hospitals and post-acute providers often fail to properly coordinate services throughout the course of a patient's treatment and follow-up. This practice leads to hospital readmissions that are not only wasteful and costly but also potentially dangerous. To break this cycle, the U.S. needs to realign health care providers' financial incentives. Offering a "global fee" that covers a bundle of "best-practice" services for hospitalization and 30-day post-hospital care has great potential to improve care, reduce complications, and generate savings to finance health reform.
Evidence of Avoidable Complications and Costly Care
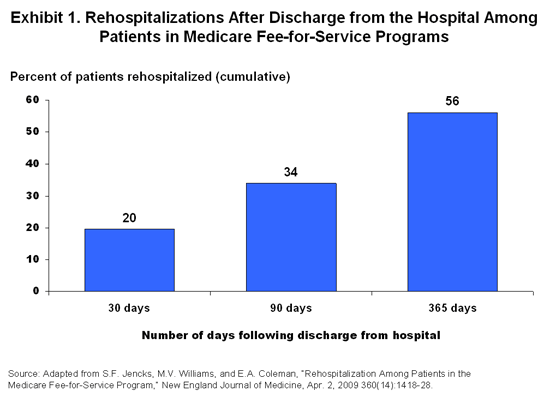
Hospital readmissions are a key indicator of overall health care quality. Commonwealth Fund-supported work has repeatedly demonstrated the troubling prevalence and costs of hospital readmissions in Medicare, as well as the wide variation in rates. A recent examination of fee-for-service claims data by Stephen Jencks, M.D., M.P.H., and colleagues found that one of five people with Medicare who was discharged from a hospital in 2003 and 2004 was readmitted within 30 days (Exhibit 1). While there is no doubt that some of these readmissions were unavoidable, it is likely that many could have been prevented with appropriate discharge planning, follow-up treatment, and post-acute care. In Dr. Jencks' study, half of the people who were hospitalized for reasons other than surgery were re-hospitalized without having seen an outpatient doctor for follow-up.
In its most recent national scorecard, the Commonwealth Fund Commission on a High Performance Health System found that the average 30-day hospital readmission rate for Medicare beneficiaries remained constant between 2003 and 2005, suggesting that we have not made needed improvements in post-acute care coordination and efficiency.
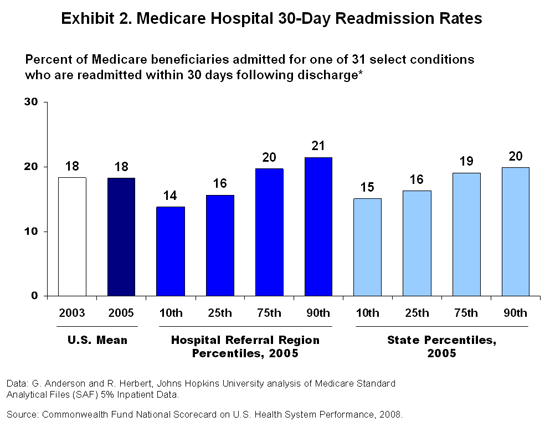
Fund studies have also uncovered wide variation across hospitals and geographic areas. The national scorecard revealed that the percentage of Medicare beneficiaries readmitted within 30 days (for 31 selected conditions) ranged from 14 percent for the 10 percent of hospital referral regions with the lowest readmission rates to 21 percent for the 10 percent of regions with the highest rates (Exhibit 2).
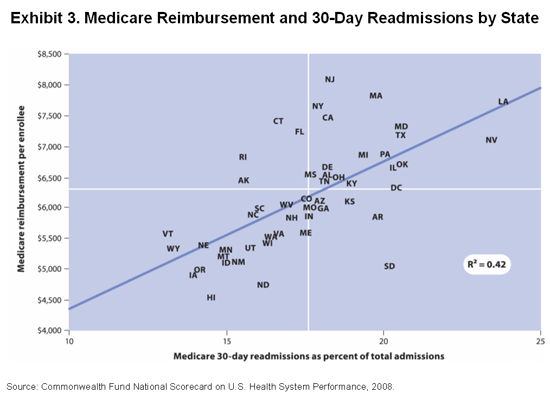
Finally, hospital readmissions are expensive and drive significant variation in Medicare spending, ultimately contributing to unsustainable growth in national health care expenditures. Dr. Jencks and colleagues estimated that the cost of unplanned hospital readmissions accounted for $17.4 billion of the $102.6 billion in total hospital payments made by Medicare in 2004. Analysis by Commonwealth Fund board member and Medicare Payment Advisory Commission (MedPAC) Chairman Glenn Hackbarth, J.D., has shown that a significant proportion of variation in Medicare spending can be traced to variability in readmissions and post-acute care. For example, spending on readmissions can vary from hospital to hospital by 54 percent and by as much as 71 percent for post-acute care for coronary-artery bypass grafting with cardiac catheterization, a common procedure. The Commonwealth Fund Commission documented the high correlation between hospital readmissions and total Medicare spending per beneficiary in its most recent state scorecard (Exhibit 3).
Realigning Incentives to Reward Efficiency and Increase Value
Recent proposals in President Obama's budget blueprint, the Commonwealth Fund Commission's "Path" report, and Senator Max Baucus' white paper on health reform would realign financial incentives to encourage greater coordination by bundling hospital payments for inpatient care, as well as post-acute health services for a predetermined number of days following hospitalization. Under the President's proposal, bundled payments are combined with reduced reimbursements for hospitals with high rates of 30-day readmission. The Administration expects this combination of incentives and penalties to save $8 billion through reduced readmissions and $18 billion through increased efficiency in post-acute care, totaling $26 billion in savings over the 10-year, 2010-2019 period.
The Commonwealth Fund Commission also recommends applying new payment methods to acute-care episodes to encourage hospitals and other providers to collaborate in developing the capacity to provide high-quality and efficient care for their patients. Offering a bundled acute-care payment (a global fee covering hospitalization and a specified set of services for 30 days following discharge) would give hospitals and other providers an opportunity to share the savings from their efforts to reduce complications of treatment and lower numbers of readmissions and would allow them more flexibility in allocating their resources. Over time, spending would slow as efficiency savings were shared between Medicare and providers. The Lewin Group estimated that within the context of comprehensive insurance expansion and other system-wide reforms, the bundled payment approach proposed by the Commission would reduce national health expenditures by $301 billion and save the federal government $211 billion over the 11-year, 2010-2020 period.
Senator Baucus' "Call to Action" on health reform includes a proposal for reducing hospital readmissions that utilizes global-care case rates and a phased strategy similar to the bundled payment approach outlined in the Medicare Payment Advisory Commission's June 2008 Report to Congress. Both the Senator and MedPAC call for initially disclosing readmission rates and resource use only to hospitals and physicians, allowing providers to understand spending levels and improve performance before releasing such data to the public. The Senator further recommends reducing reimbursement to hospitals with high rates of readmission for a small number of conditions before expanding the program to include a full range of services. Finally, the proposal includes support for additional testing and implementation of bundled payment policies among participants in the Centers for Medicare and Medicaid Services Acute Care Episode demonstration.
Promising Interventions Already Underway
Evidence suggests that health care providers can follow a number of proven strategies to reduce hospital readmissions and increase efficiency. With support from the Commonwealth Fund, the Institute for Healthcare Improvement (IHI) recently completed a survey of the published evidence on effective interventions to reduce rehospitalizations and a compendium of 15 promising initiatives already underway. In their review of the literature, IHI identifies four common themes among successful interventions: 1) enhanced care and support during transitions; 2) improved patient education and self-management support; 3) multidisciplinary team management; and 4) patient-centered care planning at the end of life.
The IHI compendium includes four interventions with very strong clinical trial or program evaluation evidence, seven with very good evidence, and four that have potential but require additional data. For the interventions bolstered by very strong evidence, patient education, post-discharge care planning, and provider coordination were among the factors that contributed to reduced rates of rehospitalization. Initiating reminder calls for preventive care, empowering nurse practitioners to work as care managers, and utilizing multidisciplinary clinical teams were all effective components of programs with very good evidence of reducing hospital readmissions.
Through its health plan, Geisinger Health System, on whose board of directors I serve, has pioneered testing payment of a global fee for a basket of best-practice services for various surgical procedures and obstetrical care. Beginning in 2006, Geisinger used American Heart Association and American College of Cardiology guidelines for coronary artery bypass graft surgery (CABG) to develop and implement 40 verifiable best-practice steps in performing this procedure. It increased the proportion of patients receiving all 40 best-practice steps from 59 percent to 86 percent within three months, and then reached and maintained 100 percent performance, with few exceptions. Its Geisinger Health Plan offered a global fee "with a warranty" covering pre-operative, operative, post-operative, and rehabilitative services for 90 days post-discharge. Complications declined by 21 percent, readmissions declined by 44 percent, and the average length of stay declined by half a day. In short, this change in delivery and payment was a win-win: it improved patient outcomes and reduced cost. Geisinger has subsequently extended this strategy to other areas, including hip replacement, cataract surgery, obesity surgery, and prenatal care and delivery of newborns.
A Win-Win
Offering a global fee for a package of best-practice services covering hospitalization and care for 30 days following discharge will reduce our overall hospital readmission rate, as well as the hospital and geographic variation in readmissions and post-acute-care spending. By realigning financial incentives to reward quality and efficiency, policymakers can eliminate the barriers to coordination among hospitals and post-acute providers built by the current fee-for-service payment system. Instead, providers will be encouraged to collaborate and rewarded for providing a continuum of care throughout the entire course of a patient's treatment and follow-up.
This is indeed a win-win strategy. The current health reform debate calls for bold hospital payment reform to enable hospitals, physicians, and post-acute care providers to achieve the best possible outcomes for patients, hold providers accountable for improving care and realizing the potential savings, and reward providers for doing so. Medicare should quickly replace its current hospital payment system with a global fee including post-discharge care.
New health insurance plans developed as part of health reform to cover the uninsured should similarly be encouraged to adopt innovative payment methods. Hospitals should be permitted to keep a share of the savings as a reward for better care, but the net savings to the federal government should be dedicated to covering the uninsured. Such savings could increase the $634 billion health reform reserve fund already proposed by the President over the 10-year period from 2010-2019 by more than $100 billion. These resources will help ensure that all Americans have affordable health insurance coverage. Lower premiums would also ease financial burdens on employers by $75 billion over 2010-2020. And premium savings for workers will provide financial relief in these difficult economic times. It is time to transform our current system of payment and delivery of health care into a system that not only provides better quality care but also bends the health-care cost curve.
We are interested in your feedback. Please take advantage of our commenting feature by clicking on the "Post a Comment" button.



