This post had been updated since original publication in December 2019.
Yesterday, the Supreme Court denied a request by 21 Democratic state attorneys general and the U.S. House of Representatives for an expedited review of an appeals court decision that struck down the Affordable Care Act’s individual mandate. In December, the Fifth Circuit Court of Appeals agreed with a lower court decision issued in Texas v. U.S. that the individual mandate is unconstitutional. Unlike the lower court, the Fifth Circuit did not decide that the rest of the ACA is also unconstitutional. Instead, the judges remanded the decision — that is, they sent it back to the same lower court judge to consider. The Democratic attorneys general and the House of Representatives, who are defending the law, had hoped that an expedited review would settle the uncertainty about the law before the 2020 presidential election and the 2021 ACA open-enrollment period. More than a dozen patient advocacy groups had filed briefs in support of this position, along with insurer and provider organizations. The Trump administration, which has sided with the plaintiffs, asked the Court to deny the request.
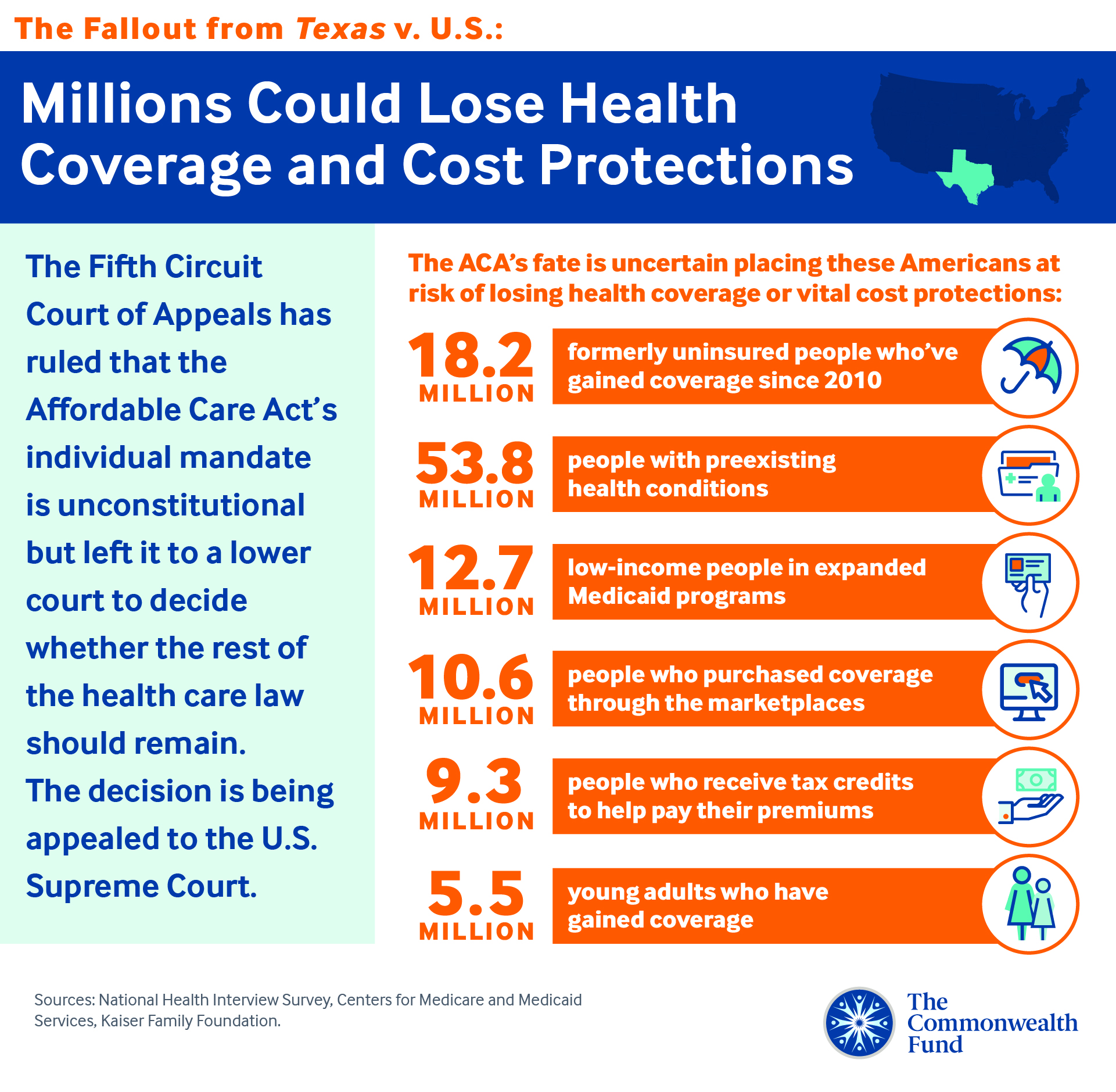
Whether the lower court decides that the rest of the law should be upheld or struck down with the mandate, the case is likely to be decided by the Supreme Court in 2021. No one knows how the Supreme Court will ultimately rule. But we do know that if the Court decides to strike down the ACA, the human toll will be immense and tragic. The law has granted unprecedented health security to millions:
- 18.2 million formerly uninsured people have gained coverage since 2010
- 53.8 million Americans with preexisting health conditions are now protected
- 12.7 million low-income people are insured through expanded Medicaid
- 10.6 million people have coverage through the ACA marketplaces, 9.3 million of whom receive tax credits to help them pay their premiums
- 5.5 million young adults have gained coverage, many by staying on their parents’ plans
- 45 million Medicare beneficiaries have much better drug coverage.
Such a decision will also trigger massive disruption throughout the U.S. health system. The health care industry represents nearly 20 percent of the nation’s economy; the ACA has touched every corner of it. The law restructured the individual and small-group health insurance markets, expanded and streamlined the Medicaid program, improved Medicare benefits, and reformed the way Medicare pays doctors, hospitals, and other providers. It was a catalyst for the movement toward value-based care and established a regulatory pathway for biosimilars — less expensive versions of biologic drugs. States have rewritten laws to incorporate the ACA’s provisions. Insurers, hospitals, physicians, and state and local governments have invested billions of dollars in adjusting to these changes.
The law’s popular preexisting health condition protections have made it possible for people with minor-to-serious health problems to apply for coverage in the same way healthier people have always done. These protections have given the estimated 53.8 million Americans with preexisting health conditions the peace of mind that they will never be denied health insurance because of their health.
More than 150 million people who get coverage through their employers now are eligible for free preventive care, and their children can stay on their policies to age 26.
The wide racial and income inequities in health insurance coverage that have been partly remedied by the ACA would return. Hospitals and providers, especially safety-net institutions, would struggle with mounting uncompensated care burdens and sicker and more costly patients who are not receiving the preventive care they need.
The ACA tore down financial barriers to health care for millions, many of whom were uninsured for most of their lives. It has demonstrably helped people get the health care they need in states across the country. Research indicates that Medicaid expansion has led to improved health status and lower mortality risk.
To date, neither the Trump administration nor Republicans in Congress have offered a replacement plan in the event the ACA is struck down. The historic progress made by Americans, particularly people of color and those with middle and lower incomes, could unravel. Further, the Supreme Court’s rejection of an expedited review coupled with uncertainty about the outcome may inflict near-term damage. Insurers may be less willing to sell plans in the ACA marketplaces next year; insurers who remain may raise premiums. Voters are already telling policymakers they are worried about their ability to afford health care. The Court’s decision to leave the future of the ACA in limbo until after the presidential election is certain to escalate those worries.
The author thanks Timothy Jost for helpful comments and Gabriella Aboulafia for research assistance.

