In March, Congress temporarily raised the share of Medicaid costs that the federal government will pay, in response to COVID-19. This short-term step granted states welcome fiscal relief, but as the depth of the economic crisis becomes clearer, so does the need for additional and more-targeted support.
Medicaid: A Countercyclical Safety Net
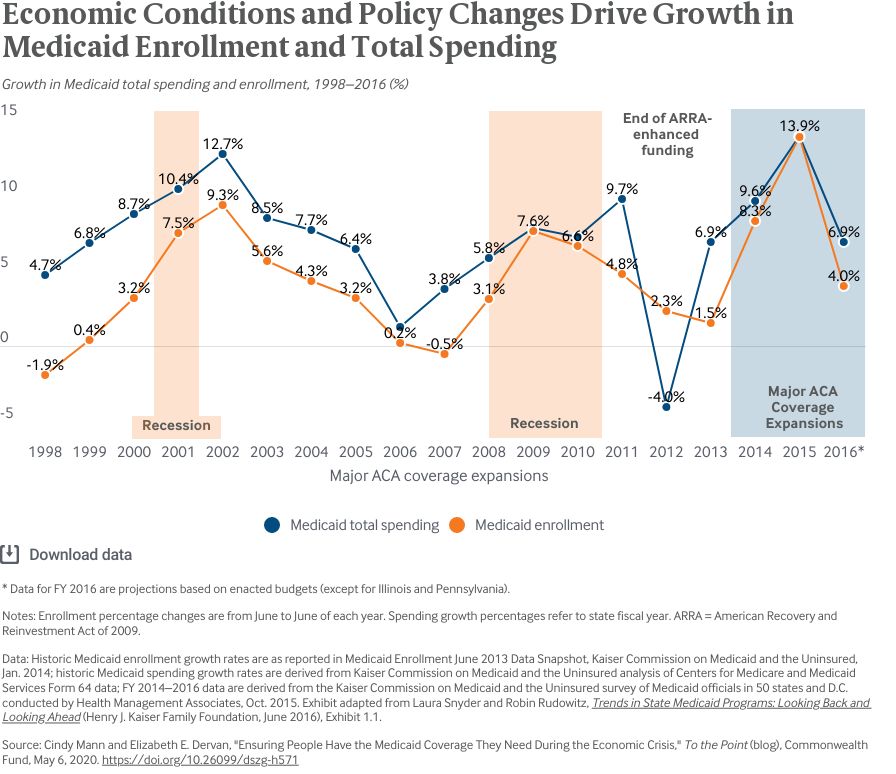
Medicaid plays a unique, countercyclical role during economic downturns. Recessions, like the one we are now in, drive up Medicaid enrollment as people become newly eligible because of job losses and reduced earnings. However, because Medicaid costs are borne by states and the federal government, recession-related enrollment drives up states’ Medicaid spending at the same time revenues are plummeting. This puts pressure on states to raise taxes or make program cuts to balance their budgets. States are not likely to raise taxes during a recession and so, absent federal relief, they will be compelled to make deep cuts to Medicaid given the size of the program relative to state budgets.
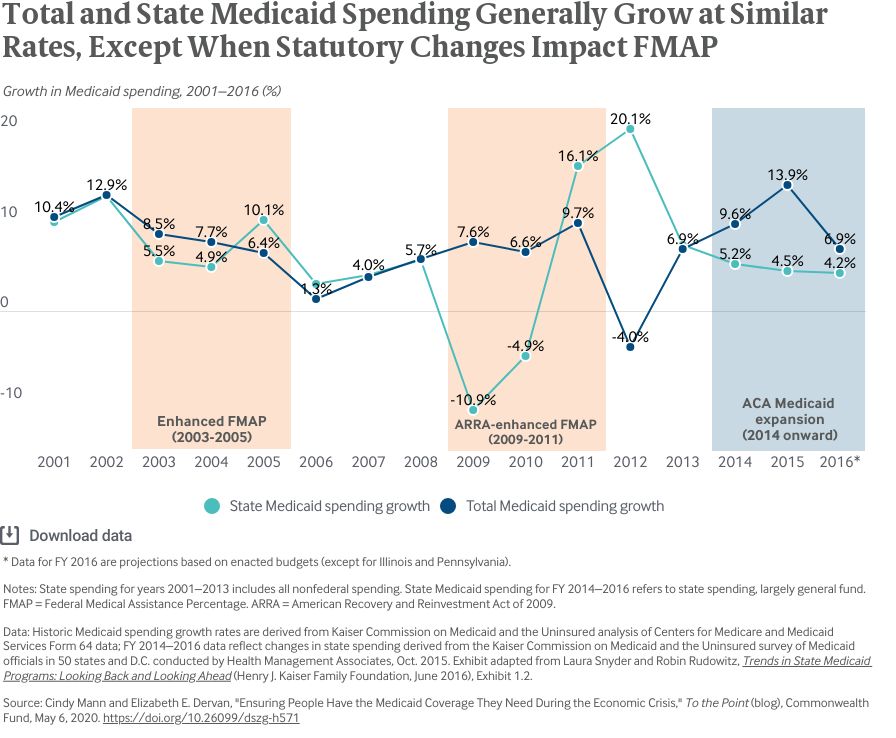
In past recessions, Congress has supported states and protected coverage by temporarily increasing the federal share of Medicaid costs. That share is set according to a state-specific rate called the Federal Medical Assistance Percentage (FMAP), which ranges from 50 percent to nearly 78 percent in normal times. Some services and populations, such as the Affordable Care Act’s expansion group, qualify for a higher federal match. Congress temporarily boosted states’ FMAP during the 2001 recession and the Great Recession of 2007 to 2009, each time conditioning the higher FMAP on states not cutting Medicaid eligibility. States that accept the FMAP increase must keep their Medicaid eligibility standards intact.