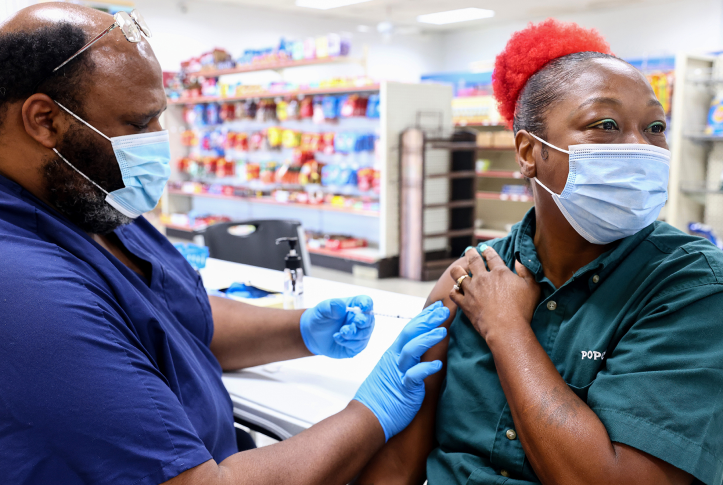
With ongoing COVID-19 surges, there is an urgent need to build vaccine confidence and increase vaccination among those yet unvaccinated. State-level data indicate that vaccination rates are significantly lower among people enrolled in Medicaid than the general population, contributing to disparities in COVID-19 outcomes.
The majority (61% in 2019) of Medicaid enrollees identify as Black, Hispanic, Asian American, or other nonwhite race or ethnicity. Disparities in COVID-19 vaccinations disproportionately impact these populations, which also have experienced elevated rates of infection, hospitalization, and death from COVID-19. It is crucial that we understand barriers to vaccination for all Medicaid beneficiaries.
As part of this effort, state Medicaid programs are developing innovative approaches to encourage vaccination among Medicaid enrollees. In partnership with the Commonwealth Fund, the National Academy for State Health Policy and the Duke–Margolis Center for Health Policy published a report that highlights successful strategies used by states and health plans. This report was informed by interviews with state officials, Medicaid managed care organization, and providers.
Promising practices from the report include:
- Using data to monitor progress, identify disparities, and target outreach. By improving data exchange among state immunization systems, health plans, and health system partners, states can improve their own data and identify disparities and target outreach. Several states have adopted formal agreements (known as data-use agreements) between their immunization programs and Medicaid programs that detail how data can be shared and used; some have shared immunization data with health plans, allowing the plans to directly target enrollees for vaccination education and incentives. However, gaps in available data on race, ethnicity, and other demographic characteristics make accurate tracking of the impact of outreach activities challenging.
- Supporting provider vaccination efforts. Reimbursing additional costs incurred by medical providers who administer vaccinations is critical. North Carolina’s Medicaid program began paying for counseling around vaccinations, even if an individual ultimately declined vaccination during the visit. In December 2021, the Biden administration announced that all Medicaid programs will be required to reimburse providers for counseling visits for eligible youth up to age 21. Understanding and reimbursing providers’ ongoing expenses as more vaccine choices become available, as booster doses are recommended, and as additional age groups are made eligible will be an ongoing challenge.
- Incentivizing Medicaid plans to reach vaccination targets. States have used a variety of strategies to encourage health plans to reach vaccination targets for the populations they serve, including creating performance measures that evaluate the degree to which evidence-based guidelines are followed, and incentive pools, which provide supplemental funding to encourage quality improvements in hospitals and among providers that serve a high volume of low-income patients. For example, Ohio’s Medicaid plans are working together to meet shared vaccination goals and can earn back funds held in reserve by the Medicaid program if all plans meet set benchmarks. These partnerships require flexibility and frequent reassessment to ensure goals are appropriate and attainable.
- Identifying opportunities to reduce barriers to vaccination. States have done significant work to ensure their Medicaid populations, including homebound people, are able to access COVID-19 vaccines. For example, Arizona, Connecticut, and Florida reimburse nonemergency medical transportation providers for driving eligible Medicaid members to and from their vaccination appointments.
- Providing technical assistance and communications resources. States have provided technical assistance and communications resources to providers who are working to vaccinate the Medicaid population. Oregon’s Medicaid officials established a learning collaborative to provide COVID-19 updates to their coordinated care organizations. Leadership discusses community vaccine uptake and strategies to increase rates, tailored by the local public health authorities. Considering the volume of misinformation spread online and through media outlets, it is crucial to support providers with tools to respond to false claims.
Building closer and more effective coordination among health providers, health plans, and community organizations that serve low-income populations can ensure that all stakeholders are part of the planning efforts, that those stakeholders are guided by a common mission, and that resources are aligned to achieve success. States and health plans play a critical role in addressing vaccination gaps for Medicaid populations, who often have lower vaccination rates than the general population. States can build on strategies outlined in the report to better support Medicaid beneficiaries and meet their needs during this continually changing and enduring public health crisis.