The Affordable Care Act has survived another Supreme Court challenge. We can expect continued efforts to build and improve upon the law, including through a public option.
President Biden endorsed a federal public option during his campaign and has since called on Congress to act, although the White House has not released a detailed proposal. Several Democrats have introduced public option legislation; two congressional committees are currently seeking public input on a path forward.
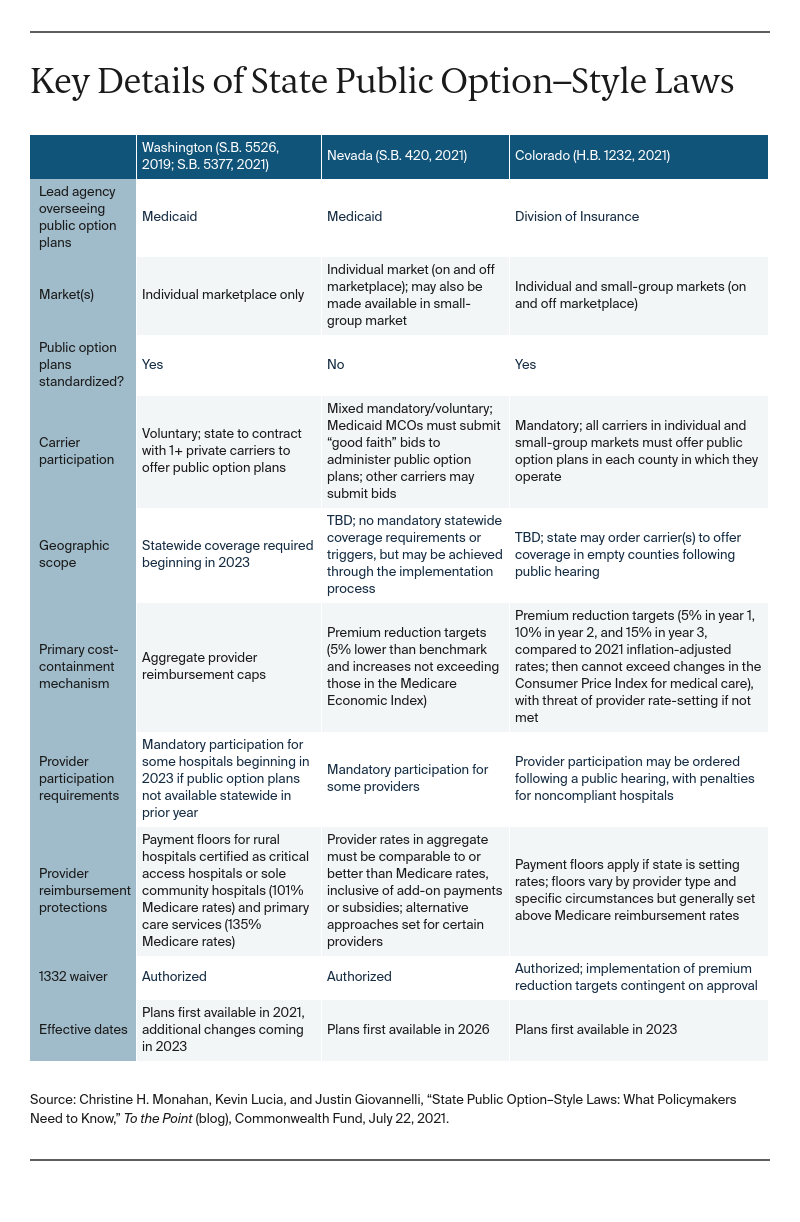
Meanwhile, Washington, Nevada, and Colorado recently enacted public option–style laws. These states’ experiences provide insight into what states can do and key issues for policymakers crafting new proposals.
What Is a Public Option?
Although definitions vary, the phrase “public option” broadly refers to a health plan created by the government to offer consumers a high-value, affordable alternative to fully private plans. Traditionally, “public option” has referred to publicly funded plans that may or may not rely on private entities to provide some administrative functions. More recently, however, the phrase has been applied to privately funded plans established pursuant to a state law and subject to certain heightened requirements meant to improve value and advance state goals, like cost containment. The Washington, Nevada, and Colorado laws generally fall into this latter category.
States Taking the Lead: Working with Private Carriers to Expand and Improve Coverage
All three states have already leveraged the Affordable Care Act: they operate their own marketplaces, took actions to promote access to adequate insurance, and expanded Medicaid. Nonetheless, access and affordability remain challenging, especially for rural residents, undocumented immigrants barred from accessing marketplace coverage, and people caught in the family glitch who are ineligible for premium tax credits. To address these challenges, the three states took broadly similar approaches in their public option laws:
- Public–private partnerships. Political and financial hurdles blocked the creation of a state-funded health plan in Washington and Colorado. Instead, both states tasked private carriers with offering new plans that meet heightened requirements — for cost containment, network adequacy, and care quality — relative to other plans on the market. Nevada’s law authorized a similar approach but allowed for a more ambitious state-funded plan administered by private carriers.
- Working within existing markets. The new plans will be offered on Affordable Care Act state-based marketplaces and meet the requirements to qualify for federal subsidies. In Nevada and Colorado, plans will be made available to individuals outside the marketplace as well. Small employers will have access to public option plans in Colorado and potentially in Nevada. Accordingly, in all three states, the public option plans should expand coverage options for consumers in the marketplace and could potentially drive down premiums of marketplace plans. In Nevada and Colorado, the plans also are intended to provide new, more affordable options for residents who cannot access the marketplaces.
- Striving for affordability. The states are seeking to provide more affordable coverage and contain costs but had to make concessions to bring providers to the table, both politically (for providers to support — or at least not actively oppose — the changes) and practically, in terms of participating in public plan networks that may pay lower rates.
- Driving broader system improvements. The states aim to leverage the new plans to advance broader delivery system reforms and reduce disparities and inequities in health and health care. For example, public option plans in Washington must implement value-based purchasing recommendations from the Bree Collaborative, while Colorado is leveraging network adequacy requirements to increase the diversity and cultural responsiveness of provider networks.
- Leveraging 1332 waivers. State officials are authorized to seek Section 1332 waivers, which allow states to reap the benefit of federal cost-savings generated by new state programs. Public option programs that lower marketplace premiums — and, thus, federal spending on premium tax credits — may entitle states to federal dollars (called “pass-through funds”) that may be used to further boost affordability (e.g., by supplementing new state subsidy programs in Washington and Colorado) or to advance equity.
Ensuring Access and Affordability
During implementation of its public option–style law, Washington faced the challenge of persuading carriers and providers to participate while trying to constrain premiums. All three states have learned from Washington’s early experience and adopted different incentives and requirements to reconcile these competing interests.
To promote cost containment, Washington capped plans’ statewide aggregate provider reimbursement rate at 160 percent of Medicare. Several carriers opted to participate, but many hospitals refused to join a public option network. Because carriers were unable to form adequate networks without these hospitals, about half of the state’s counties did not have a public option plan in 2021. In response, Washington passed legislation that would ensure statewide availability of public option plans, including requiring certain hospitals to contract with a public option plan in 2023 if a public option plan is not available in each county in 2022.
Nevada and Colorado instead sought to contain costs by setting premium-reduction targets for their public option plans and are providing carriers with flexibility on how to achieve savings. Recognizing carriers may not welcome this responsibility, Nevada will require all Medicaid managed care organizations to submit “good faith” bids to administer the public option plan, while Colorado will require all carriers to offer the public option plan in each county where they operate.
To bring in providers, Nevada will require any provider participating in its Medicaid program or other state plans to enroll in at least one public option plan network. Colorado will require providers to participate only if a public hearing shows that carriers cannot meet premium reduction or network adequacy requirements. If this happens, the state can set reimbursement rates on providers and fine or suspend hospitals that refuse to accept the set rates.
All three states also included reimbursement floors tied to Medicare rates for some or all providers to mitigate hospital and physician stakeholders’ concerns.
Looking Ahead
Even the most ambitious states can face barriers when adopting reforms such as public options. These barriers — which may be financial, political, or logistical — suggest that federal action may be necessary for more aggressive cost containment and coverage gains.