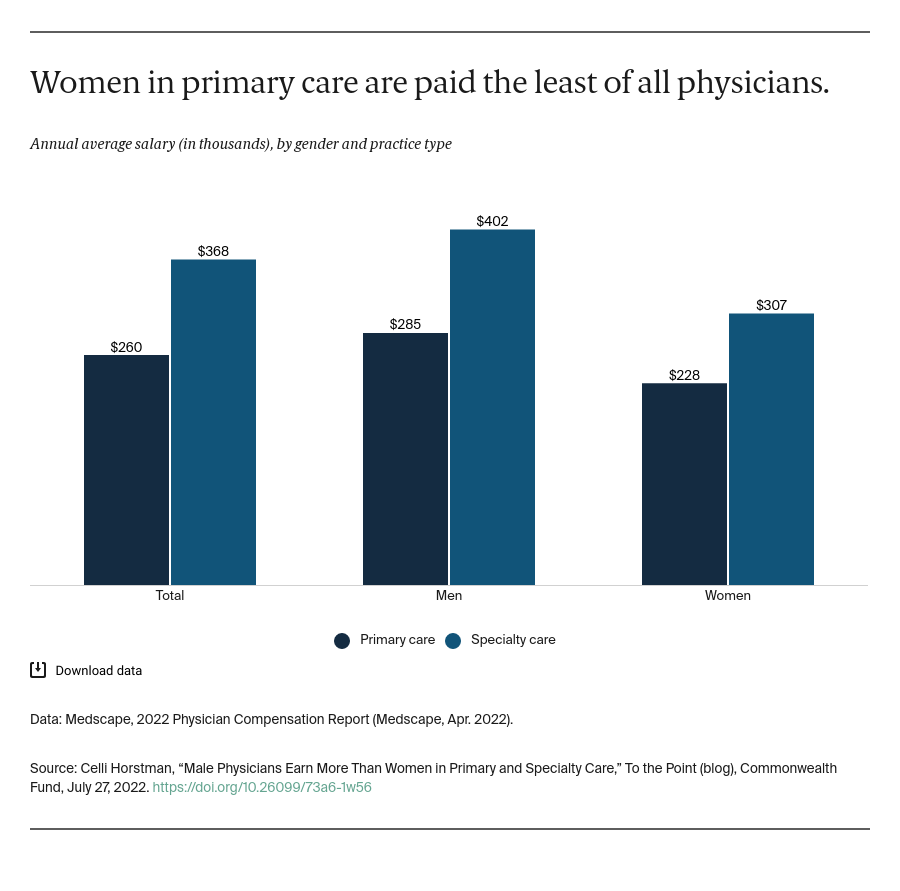
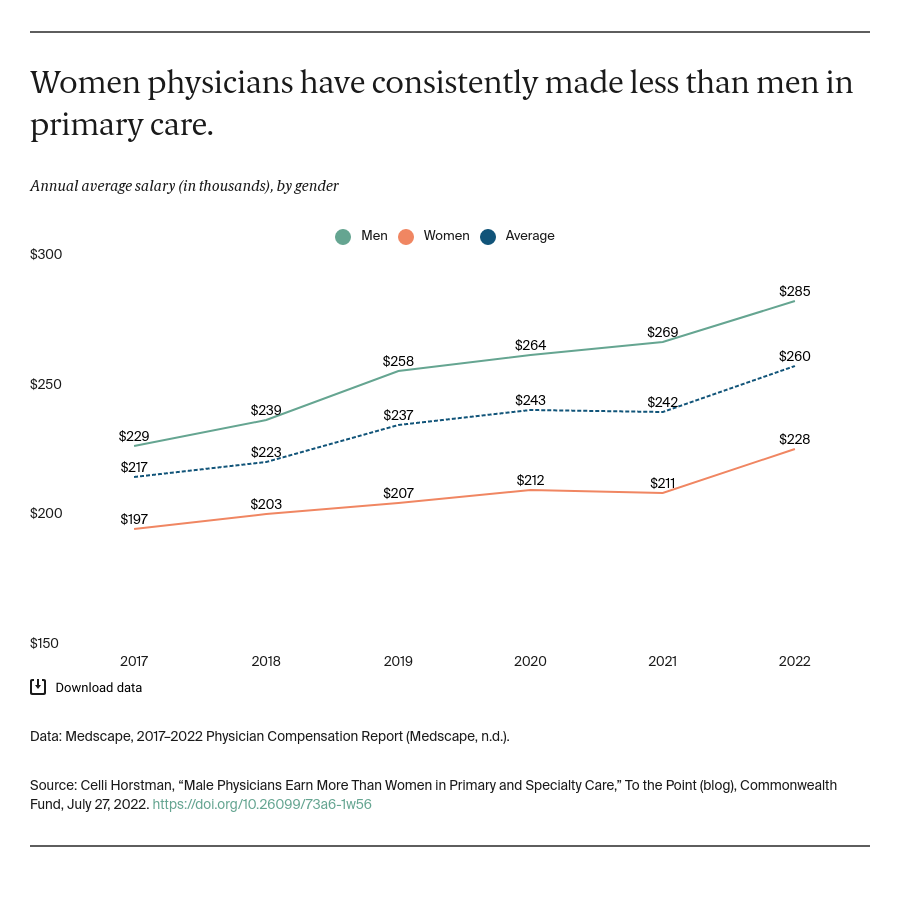
The earnings gap between men and women in primary care has substantially increased over the past five years, from a difference of $32,000 in annual salaries in 2017 to $57,000 in 2022. In fact, women physicians in primary care today can expect to earn salaries similar to those men earned in 2017.
Some studies have found that when accounting for specialty type, up to 55 percent of the gender compensation gap is accounted for, because primary care physicians are consistently paid less than specialists. This is partly because our health system pays more for services and procedures provided by specialists, like surgeries, than those provided by primary care, like care coordination and preventive services that promote whole-person care. Coinciding with differences in pay across specialties, more women are in primary care, pediatrics, and obstetrics/gynecology compared to other specialties. In these specialties, annual salaries, regardless of gender, are lower. There is a compounding effect — women are overrepresented in the lowest-paid specialties and are also paid less than men within these specialties.
How we pay for health care is also a contributing factor. In our fee-for-service approach, the number of patients and the volume and type of services rendered play a large role in revenues and compensation. Previous research has found that women physicians tend to see fewer patients, spend more time with their patients, and provide more services with lower reimbursement rates, like counseling. This all leads to lower revenue. Some research has found that patients treated by women physicians had lower readmission rates than those treated by men, which can lower costs for health systems. These practice approaches are important aspects of patient-centered care. In a system that pays for the quantity of services provided, rather than the quality of care, women — or any physicians who provide patient-centered care — may be at a disadvantage.
Some experts have suggested that value-based payment (VBP) approaches have the potential to mitigate the impact of payment on the compensation gap. Under VBP models, payments are made up front and meant to cover all services provided; they are designed to promote cost savings and high-quality care. Shifting the focus from the volume of services provided to the overall care experience may be beneficial for women physicians.
A key component of VBP is the potential for savings when providers and health systems perform efficiently and improve quality. Health systems could translate savings into bonuses for physicians, which would present another way to increase female physicians’ salaries. But, with women’s base salaries already lower than men’s, health systems would need to actively leverage VBP model design to close the physician gender compensation gap.
Research suggests that in addition to the gender gap in physician compensation, there are further disparities based on race and ethnicity. More research is needed, as most compensation studies have not accounted for race and gender, and few explore race and ethnicity alone. Unless we fully understand the scale, scope, and underlying structural factors of the compensation gap, health care cannot move toward equity in the workforce.