A new study released today by the Harvard University School of Public Health and The Commonwealth Fund documents that in five English-speaking nations—Australia, Canada, New Zealand, the United Kingdom, and the United States—the public is expressing concern about their health systems. The data reveal that the basis for dissatisfaction varies in response to how different health policy changes have affected everyday life.
Approximately 1,000 people in each of the five nations were interviewed by telephone by Louis Harris and Associates, Inc., from April to June 1998. The findings were released today at the 1998 International Symposium on Health Care Policy, organized by The Commonwealth Fund and Health Affairs, along with newly available data from the Organization for Economic Cooperation and Development (OECD) on the costs and performance of the different countries' health care systems. Families' experiences and views of their countries' health systems, in combination with data on system expenses and performance, tell a complex story of the high value placed on ready access to health care and on freedom from struggles to pay medical bills.
U.S. No Longer Unique in Broad Citizen Support for Major Health System Changes
The mood for change is clear across all five countries surveyed, with at most one in four respondents in any country saying their system "works pretty well, with only minor changes needed." Nearly one in three people in the United States (33%), New Zealand (32%), and Australia (30%) call for a "complete rebuilding" of their health systems, followed by nearly one-fourth (23%) of Canadians. In contrast, only 14 percent of the British want to rebuild their system.
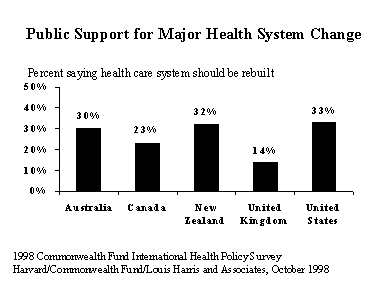 Confidence in health systems does not appear to coincide with levels of country spending on health care. Dissatisfaction is greatest in the United States, the country that spends the most, and lowest in Britain, the country that spends the least. "Americans are troubled about their health care system¾ especially the threat of financial burdens if a family member becomes ill," said Karen Davis, president of The Commonwealth Fund. "Within a changing marketplace, people are increasingly anxious about their ability to get specialized care."
In the past decade, efforts to control health care costs have become a priority in many industrialized countries. In the United States, major cost initiatives have involved private health insurance and managed care, while Australia, Canada, and New Zealand have led the way in governmental cost-cutting. In fact, according to Multinational Comparisons of Health Care: Expenditures, Coverage, and Outcomes, the new study using OECD data, health spending as a percentage of gross domestic product (GDP) declined in the 1990s in Canada. Public reaction, however, appears to reflect a loss of confidence and fear that quality of health care will be compromised.
Confidence in health systems does not appear to coincide with levels of country spending on health care. Dissatisfaction is greatest in the United States, the country that spends the most, and lowest in Britain, the country that spends the least. "Americans are troubled about their health care system¾ especially the threat of financial burdens if a family member becomes ill," said Karen Davis, president of The Commonwealth Fund. "Within a changing marketplace, people are increasingly anxious about their ability to get specialized care."
In the past decade, efforts to control health care costs have become a priority in many industrialized countries. In the United States, major cost initiatives have involved private health insurance and managed care, while Australia, Canada, and New Zealand have led the way in governmental cost-cutting. In fact, according to Multinational Comparisons of Health Care: Expenditures, Coverage, and Outcomes, the new study using OECD data, health spending as a percentage of gross domestic product (GDP) declined in the 1990s in Canada. Public reaction, however, appears to reflect a loss of confidence and fear that quality of health care will be compromised.
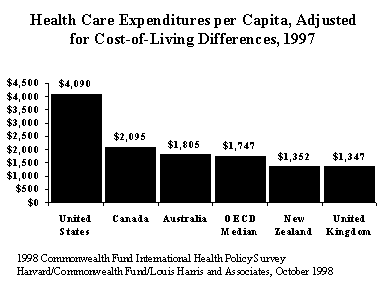 "In past international surveys, the United States often stood out in its view that the health system needed fundamental change or to be rebuilt completely," said Robert J. Blendon, professor of health policy and political analysis at the Harvard University School of Public Health and the John F. Kennedy School of Government. "Changing health care systems is very difficult politically. As a result, countries that used to give their systems high votes are approaching the level of concern the United States has had for years."
Perceived Problems Differ and Tend to Reflect Types of Access Difficulties
Perceptions of the major difficulties in each system differ. In the United States, the only nation surveyed that does not have a universal insurance system, affordability of care is the most frequently cited problem. In Canada, New Zealand, and the United Kingdom, people are most concerned with the level of governmental health care funding. Australians and New Zealanders also cite waiting times as a leading problem.
U.S. families are the most likely to report access, to-care difficulties in the five, country survey. The United States has the highest proportion reporting a time when they did not get needed care, and more than one in four families (28%) say getting needed care is difficult. Nearly one in three families report they have no regular doctor, indicating a lack of basic primary care as well as problems with continuity of care.
"In past international surveys, the United States often stood out in its view that the health system needed fundamental change or to be rebuilt completely," said Robert J. Blendon, professor of health policy and political analysis at the Harvard University School of Public Health and the John F. Kennedy School of Government. "Changing health care systems is very difficult politically. As a result, countries that used to give their systems high votes are approaching the level of concern the United States has had for years."
Perceived Problems Differ and Tend to Reflect Types of Access Difficulties
Perceptions of the major difficulties in each system differ. In the United States, the only nation surveyed that does not have a universal insurance system, affordability of care is the most frequently cited problem. In Canada, New Zealand, and the United Kingdom, people are most concerned with the level of governmental health care funding. Australians and New Zealanders also cite waiting times as a leading problem.
U.S. families are the most likely to report access, to-care difficulties in the five, country survey. The United States has the highest proportion reporting a time when they did not get needed care, and more than one in four families (28%) say getting needed care is difficult. Nearly one in three families report they have no regular doctor, indicating a lack of basic primary care as well as problems with continuity of care.
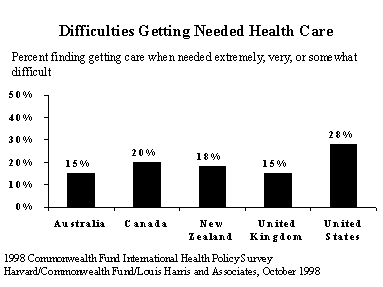 Access is also a concern in the other four countries. Indeed, Canadian and New Zealander responses are often similar to those in the United States in regard to getting needed care and difficulties seeing specialists or medical consultants. Canadians appear particularly concerned about access to specialists, with nearly half saying getting to see a specialist can be difficult.
Reasons for access difficulties, however, differ significantly across countries. U.S. families say their access problems are largely financial, with more than half citing lack of money or insurance as the main reason they did not get needed care. In the other nations, waiting times for care predominate as the major obstacle.
Reports on experiences waiting for nonemergency care underscore differences in access experiences. Waiting times for nonemergency care are longest by far in the United Kingdom and shortest in the United States. U.K. residents, however, are the least likely to report access difficulties among the five countries surveyed. In part, this may reflect apparently ready access to primary care physicians, including nights and weekends. A striking 44 percent of U.K. families say their physicians come to their homes when needed on nights or weekends—a rare experience in the United States or other countries.
U.S. Families Face Heavy Financial Burdens
Reflecting their access concerns, relatively high proportions of U.S. families report that medical bills have resulted in financial stress (18%) and that they have not filled prescriptions for medications because of costs (17%). The United States stands out in the extent to which families are paying for medical costs directly: nearly 19 percent say they paid more than $1,000 in the past year for medical bills that were not covered by insurance. Paying for prescription medications also appears problematic in Australia and New Zealand. U.K. residents are particularly well-protected: 44 percent indicate they did not pay any out-of-pocket costs for medical care in the last year, and less than 1 percent reported costs of more than $1,000.
Access is also a concern in the other four countries. Indeed, Canadian and New Zealander responses are often similar to those in the United States in regard to getting needed care and difficulties seeing specialists or medical consultants. Canadians appear particularly concerned about access to specialists, with nearly half saying getting to see a specialist can be difficult.
Reasons for access difficulties, however, differ significantly across countries. U.S. families say their access problems are largely financial, with more than half citing lack of money or insurance as the main reason they did not get needed care. In the other nations, waiting times for care predominate as the major obstacle.
Reports on experiences waiting for nonemergency care underscore differences in access experiences. Waiting times for nonemergency care are longest by far in the United Kingdom and shortest in the United States. U.K. residents, however, are the least likely to report access difficulties among the five countries surveyed. In part, this may reflect apparently ready access to primary care physicians, including nights and weekends. A striking 44 percent of U.K. families say their physicians come to their homes when needed on nights or weekends—a rare experience in the United States or other countries.
U.S. Families Face Heavy Financial Burdens
Reflecting their access concerns, relatively high proportions of U.S. families report that medical bills have resulted in financial stress (18%) and that they have not filled prescriptions for medications because of costs (17%). The United States stands out in the extent to which families are paying for medical costs directly: nearly 19 percent say they paid more than $1,000 in the past year for medical bills that were not covered by insurance. Paying for prescription medications also appears problematic in Australia and New Zealand. U.K. residents are particularly well-protected: 44 percent indicate they did not pay any out-of-pocket costs for medical care in the last year, and less than 1 percent reported costs of more than $1,000.
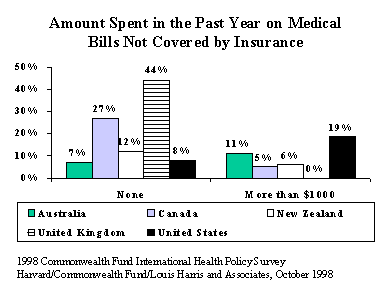 "In all countries, increased exposure to medical costs leads to increased problems getting access to needed medical care as well as to increased public discontent," said Karen Donelan, managing director of the Harvard Opinion Research Program. "While many experts agree that cost-sharing makes sense, for some people it clearly results in increased worry and diminished access."
Concerns About Quality of Health Care and Access
Currently, similar proportions of the public in all five countries rate the quality of overall medical care, doctor care, and hospital care as "excellent," with Canada highest in all categories. Yet, in no country do more than 37 percent of the population rate care as excellent.
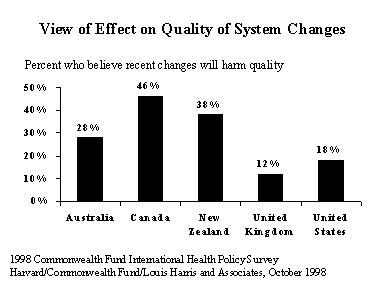
Those surveyed differed in their views about the likely impact of recent policy changes on quality of care in the future. Canada and New Zealand voice the most concern: 46 percent of Canadians and 38 percent of New Zealanders say they expect that recent changes could harm the quality of care available to them. In contrast, half of U.K. and U.S. residents (47%) expect no change in quality, and less than one in five anticipate harmful effects.
"In all countries, increased exposure to medical costs leads to increased problems getting access to needed medical care as well as to increased public discontent," said Karen Donelan, managing director of the Harvard Opinion Research Program. "While many experts agree that cost-sharing makes sense, for some people it clearly results in increased worry and diminished access."
Concerns About Quality of Health Care and Access
Currently, similar proportions of the public in all five countries rate the quality of overall medical care, doctor care, and hospital care as "excellent," with Canada highest in all categories. Yet, in no country do more than 37 percent of the population rate care as excellent.
Those surveyed differed in their views about the likely impact of recent policy changes on quality of care in the future. Canada and New Zealand voice the most concern: 46 percent of Canadians and 38 percent of New Zealanders say they expect that recent changes could harm the quality of care available to them. In contrast, half of U.K. and U.S. residents (47%) expect no change in quality, and less than one in five anticipate harmful effects.
 The survey finds considerable public fear for future access to care as well as quality. In Australia, Canada, New Zealand, and the United States, one in five people or more say they are "very worried" that they will not be able to get advanced care or treatment if seriously ill or will not be able to afford medical care. New Zealanders express the greatest degree of concern: well over a third worry about access and paying for care, though these concerns do not seem to stem directly from personal experiences with these problems. In all five countries, concerns about the affordability of long-term care services exceed concerns about general medical care or waits for care. People in the United Kingdom express the least fear for their health care future.
New OECD data indicate that the United States lags in some quality indicators, as measured by selected health care outcomes. New international comparisons reveal that the United States has the highest rate of premature deaths (preventable if appropriate medical knowledge had been applied or public health principles had been in force) and continues to rank low among industrialized nations in terms of life expectancy and infant mortality. "International comparisons of outcomes measures indicate that greater attention should be given in the United States to factors that could improve health outcomes," said Gerard Anderson, director of the Johns Hopkins University Center for Hospital Finance and Management.
U.S. Uninsured: A Different Experience
With the exception of the United States, all countries surveyed have universal insurance coverage. The survey finds that being without health insurance puts families at high risk. The uninsured are three times as likely to have difficulties getting care (65% vs. 20%), to have gone without needed care (37% vs. 10%), and to have gone without recommended care because of costs (42% vs. 13%). "Despite living in a country rich in medical care resources, the uninsured in United States stand out in the severity of access problems," said Cathy Schoen, vice president for research and evaluation at The Commonwealth Fund. "Although our national health care expenditures lead the world, we lag in health care access and financial security."
Cross-National Learning
All nations surveyed are learning hard lessons about containing health care costs in a time of increasing consumer demand for improved quality. Today, the vast majority of people in each country surveyed indicate that they think their health system needs more than minor changes.
The preoccupation with containing health costs has apparently led to growing public fears that access to health care and quality of care are being compromised. In Australia, Canada, and New Zealand, recent changes have brought major concerns about waiting times for care and access to specialists. Change has come hard in these countries, and the public appears to be unsettled by the shape it has taken.
In the United Kingdom, the National Health Service is turning 50 and appears to remain popular. U.K. families are the least concerned for their personal health care future and relatively low proportions voice support for major rebuilding. Families are well-protected financially. Although waiting times are often long, people in the United Kingdom appear more accepting of longer waiting times for nonemergency services than respondents in other countries. There is strong support for increased funding of the public health system.
In the United States, support for complete system rebuilding is at about the same level as it was a decade ago. The failure of legislation to enact universal coverage means that many people continue to lack insurance or face gaps in coverage. U.S. residents continue to confront barriers to access and face large out-of-pocket financial burdens.
The survey indicates how important health care experiences and major policy changes are to individual and family health and security. Exposure to high out-of-pocket costs, difficulties getting access to care, and fears that quality of care is declining prompt widespread public dissatisfaction across international borders. As countries grapple with how to improve the health and quality of life of citizens with efficient use of resources, popular perceptions of the impact of change are likely to be of increasing importance.
The survey finds considerable public fear for future access to care as well as quality. In Australia, Canada, New Zealand, and the United States, one in five people or more say they are "very worried" that they will not be able to get advanced care or treatment if seriously ill or will not be able to afford medical care. New Zealanders express the greatest degree of concern: well over a third worry about access and paying for care, though these concerns do not seem to stem directly from personal experiences with these problems. In all five countries, concerns about the affordability of long-term care services exceed concerns about general medical care or waits for care. People in the United Kingdom express the least fear for their health care future.
New OECD data indicate that the United States lags in some quality indicators, as measured by selected health care outcomes. New international comparisons reveal that the United States has the highest rate of premature deaths (preventable if appropriate medical knowledge had been applied or public health principles had been in force) and continues to rank low among industrialized nations in terms of life expectancy and infant mortality. "International comparisons of outcomes measures indicate that greater attention should be given in the United States to factors that could improve health outcomes," said Gerard Anderson, director of the Johns Hopkins University Center for Hospital Finance and Management.
U.S. Uninsured: A Different Experience
With the exception of the United States, all countries surveyed have universal insurance coverage. The survey finds that being without health insurance puts families at high risk. The uninsured are three times as likely to have difficulties getting care (65% vs. 20%), to have gone without needed care (37% vs. 10%), and to have gone without recommended care because of costs (42% vs. 13%). "Despite living in a country rich in medical care resources, the uninsured in United States stand out in the severity of access problems," said Cathy Schoen, vice president for research and evaluation at The Commonwealth Fund. "Although our national health care expenditures lead the world, we lag in health care access and financial security."
Cross-National Learning
All nations surveyed are learning hard lessons about containing health care costs in a time of increasing consumer demand for improved quality. Today, the vast majority of people in each country surveyed indicate that they think their health system needs more than minor changes.
The preoccupation with containing health costs has apparently led to growing public fears that access to health care and quality of care are being compromised. In Australia, Canada, and New Zealand, recent changes have brought major concerns about waiting times for care and access to specialists. Change has come hard in these countries, and the public appears to be unsettled by the shape it has taken.
In the United Kingdom, the National Health Service is turning 50 and appears to remain popular. U.K. families are the least concerned for their personal health care future and relatively low proportions voice support for major rebuilding. Families are well-protected financially. Although waiting times are often long, people in the United Kingdom appear more accepting of longer waiting times for nonemergency services than respondents in other countries. There is strong support for increased funding of the public health system.
In the United States, support for complete system rebuilding is at about the same level as it was a decade ago. The failure of legislation to enact universal coverage means that many people continue to lack insurance or face gaps in coverage. U.S. residents continue to confront barriers to access and face large out-of-pocket financial burdens.
The survey indicates how important health care experiences and major policy changes are to individual and family health and security. Exposure to high out-of-pocket costs, difficulties getting access to care, and fears that quality of care is declining prompt widespread public dissatisfaction across international borders. As countries grapple with how to improve the health and quality of life of citizens with efficient use of resources, popular perceptions of the impact of change are likely to be of increasing importance.


