Close to 4 million Americans would gain health insurance, and premium costs would drop an average of nearly 12 percent, if every state joined Massachusetts and New Jersey in enacting state-level individual mandates. These mandates would replace the Affordable Care Act’s (ACA) penalty for not having health insurance, a fee that Congress eliminated, effective 2019. That’s according to a new Commonwealth Fund/Urban Institute report by the Urban Institute’s Linda Blumberg, Matthew Buettgens, and John Holahan examining what would happen if all states adopted their own individual insurance mandates.
 The ACA requires most Americans to enroll in an insurance plan or pay a financial penalty — a move intended to stabilize insurance markets by encouraging healthy people to purchase and stay enrolled in a health plan. Now that the mandate penalty will be eliminated as of January 2019, the Congressional Budget Office predicts that premiums will increase and more people will lose their insurance coverage.
The ACA requires most Americans to enroll in an insurance plan or pay a financial penalty — a move intended to stabilize insurance markets by encouraging healthy people to purchase and stay enrolled in a health plan. Now that the mandate penalty will be eliminated as of January 2019, the Congressional Budget Office predicts that premiums will increase and more people will lose their insurance coverage.
Linda Blumberg, an author of the study and Institute Fellow in the Health Policy Center at the Urban Institute
“Although the repeal of the individual mandate penalty will have negative effects across our health care system, states can act to keep their health insurance markets stable and affordable by offsetting the expected coverage losses and premium increases beginning in 2019.”
David Blumenthal, M.D., Commonwealth Fund President
“Because of the ACA, more people have health insurance than ever before, and people with health problems can’t be denied coverage or charged more because of their condition. With the repeal of the individual mandate penalty, this report shows how states can exercise their own authorities to reduce the number of uninsured and make insurance more affordable for their residents.”
But if states acted on their own to replace the federal mandate, the new report finds that, compared with having no mandate:
- Millions more people would gain health insurance. Implementing state individual mandates across the country in 2019, when the federal penalties are lifted, would reduce the number of uninsured by 3.9 million — a decrease of 11.4 percent. In 2022, there would be 7.5 million fewer uninsured Americans.
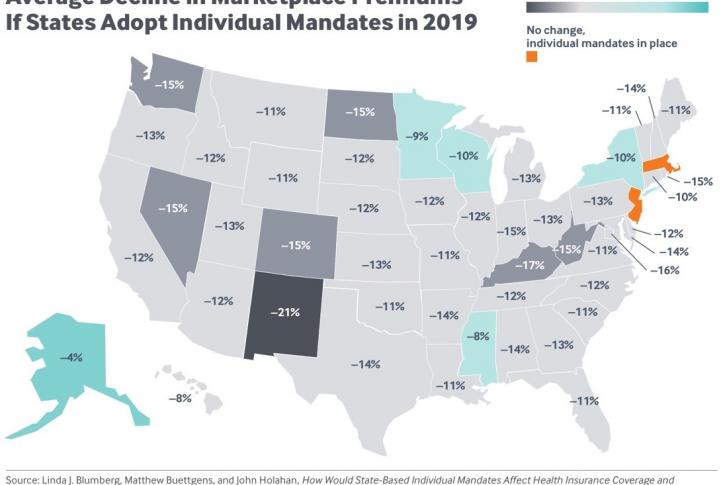
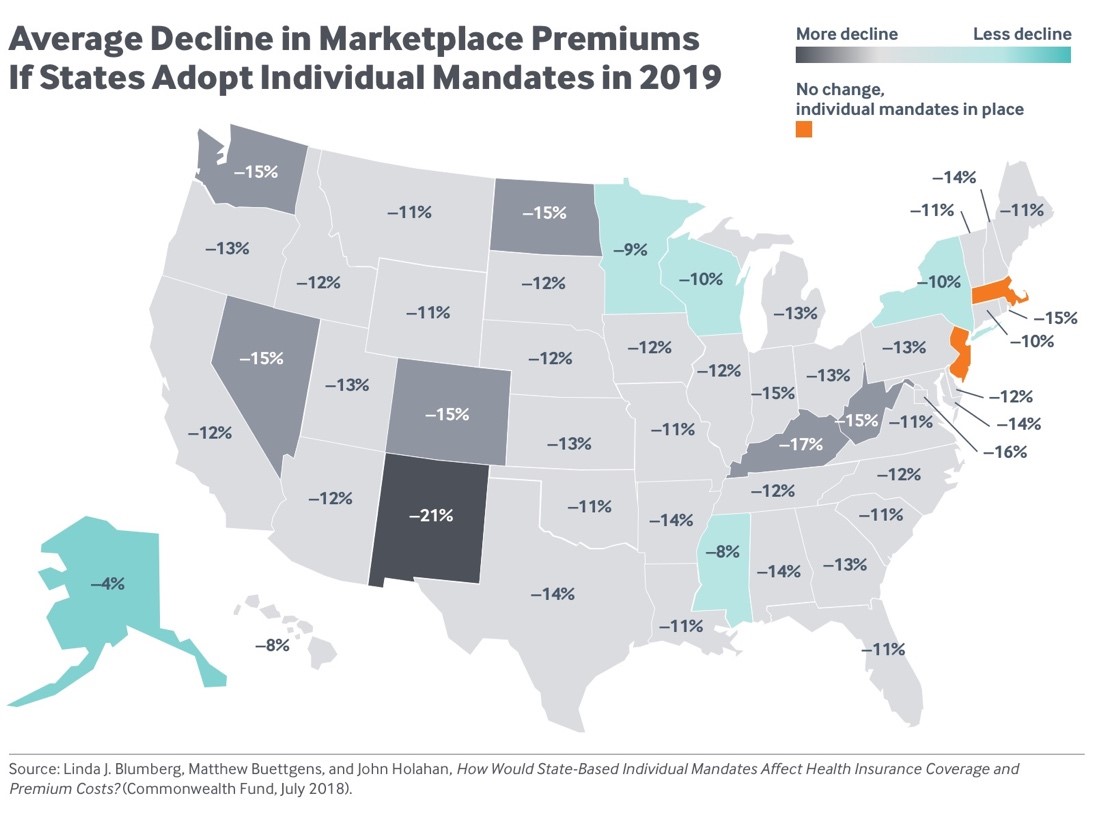
- Premiums would drop by an average of nearly 12 percent. If all states adopted an individual mandate, marketplace premiums would fall by an average of 11.8 percent. The impact would vary across states, depending on how many healthy people reenroll in the marketplaces. The larger the share of healthy enrollees in individually purchased plans today, the greater the impact on premium rates. In New Mexico, premiums would decrease by more than 20 percent, and they would drop by 15 percent or more in Colorado, the District of Columbia, Kentucky, Nevada, North Dakota, Washington, and West Virginia.
- Montana, West Virginia, North Dakota, and Kentucky would see the largest uptakes, percentage-wise, in coverage. Mandates in these states would reduce the number of uninsured residents by more than 20 percent, as more people enroll in individually purchased plans, Medicaid, or the Children’s Health Insurance Program. In California, 389,000 people would gain coverage under a state mandate.
- Uncompensated care costs would decline dramatically. When patients are uninsured and can't pay their medical bills, state and federal governments, as well as physicians, hospitals, and community health centers, absorb the costs of this uncompensated care. As more people gain coverage under state mandates, demand for uncompensated care would fall by $11.4 billion nationally, the new report finds. In Texas, uncompensated care costs would fall by $1.2 billion; in California, by $892 million; in Florida, by $747 million; and, in Georgia, by $548 million.
ADDITIONAL REPORT BACKGROUND
The report outlines the additional benefits of individual mandates for state economies. These include:
- Increased flow of federal dollars: With the passage of state-level mandates, the flow of federal dollars would increase to 27 states plus the District of Columbia, as more people enroll in Medicaid or take advantage of marketplace premium tax credits. In 21 states, federal spending would decline slightly under a mandate as a result of lower marketplace premiums and the consequent decrease in average premium subsidies.
- Increased state revenue: If every state implemented mandates effective in 2019, 8.8 million families would pay financial penalties to their state department of revenue for not complying with the law, amounting to $7.4 billion. Average penalties per family would range from a low of $630 in West Virginia to a high of $1,270 in Delaware.
IMPLICATIONS
By legislating comparable mandate penalties, states can mitigate the negative coverage and premium effects caused by eliminating the ACA’s individual mandate in 2019. Massachusetts, for example, legislated its own individual mandate in 2006 and New Jersey did so this year. Legislation has also been considered, but did not pass, in Maryland, Hawaii, and Connecticut. In the District of Columbia, an individual mandate passed as part of a larger budget bill and is expected to be signed by the mayor. However, there are riders to the D.C. budget in the U.S. House of Representatives intended to inhibit implementation, although it is not clear they would be successful.
The study’s authors note that state-level mandates face significant challenges. Some states, for example, do not have state income taxes, and new financial structures would have to be developed to collect individual mandate penalties. Other state political environments are not conducive to enacting individual mandate legislation, even in states where governors and state policymakers generally support the ACA.
ADDITIONAL PERTINENT RESEARCH
Dania Palanker, Rachel Schwab, and Justin Giovannelli, “State Efforts to Pass Individual Mandate Requirements Aim to Stabilize Markets and Protect Consumers,” To the Point (blog), Commonwealth Fund, June 14, 2018.