This explainer was originally published on April 2, 2024, and updated on January 14, 2025.

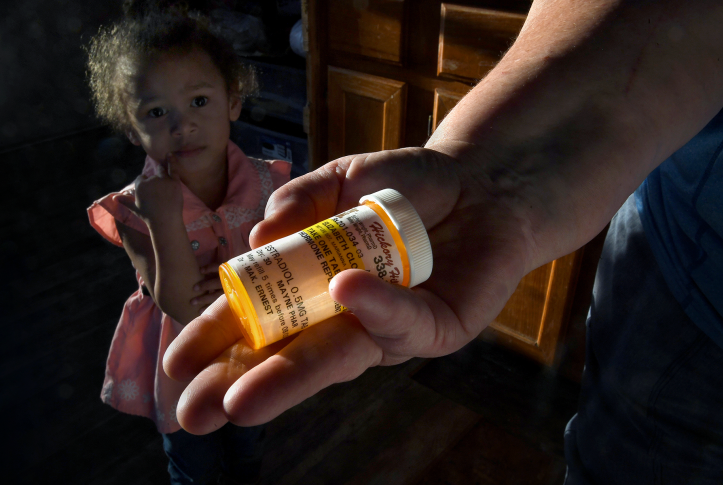
Elizabeth Cloinger holds an empty prescription bottle in front of her 3-year-old granddaughter, A’Riyiah Franklin, in Marianna, Ark. Because of a complicated verification process she did not understand, Cloinger was disenrolled from the Arkansas Works Medicaid program even though she is income-eligible — and she hasn’t filled that prescription in two years. Arkansas is one of only two states to implement Medicaid work requirements. Photo: Michael S. Williamson/Washington Post via Getty Images
Elizabeth Cloinger holds an empty prescription bottle in front of her 3-year-old granddaughter, A’Riyiah Franklin, in Marianna, Ark. Because of a complicated verification process she did not understand, Cloinger was disenrolled from the Arkansas Works Medicaid program even though she is income-eligible — and she hasn’t filled that prescription in two years. Arkansas is one of only two states to implement Medicaid work requirements. Photo: Michael S. Williamson/Washington Post via Getty Images
This explainer was originally published on April 2, 2024, and updated on January 14, 2025.
For most of its history, Medicaid, the joint state and federal health insurance program for people with low income, has not tied eligibility to employment. This changed during the first Trump administration, which encouraged state Medicaid agencies to test work requirements. The Centers for Medicare and Medicaid Services (CMS) approved 11 state proposals for implementing waiver-based demonstration programs between 2017 and 2021, although most of these proposals were never implemented, owing to legal challenges and economic disruption caused by the COVID-19 pandemic. The Biden administration then rescinded approval of all proposals in early 2021.
Under a new Trump administration, however, Medicaid work requirements may well have a second life. Here’s what the evidence shows about work requirements in Medicaid and other public programs and how they impact people trying to access services.
Federal and state policymakers have periodically proposed and established “community engagement” requirements — more commonly known as work requirements — for people enrolled in Medicaid. Whereas Medicaid eligibility is primarily based on income, work requirements add a new condition of eligibility for adults, making coverage contingent on working, volunteering, or engaging in educational activities for a minimum number of hours.
The 11 state work requirement proposals to date have varied in whom they apply to and how many hours of approved activities are required. Most of the proposals would require working-age Medicaid beneficiaries (ages 18 to 64) to prove they are working or engaging in other approved activities 80 hours a month, or 20 hours per week. Many, though not all, include exemptions from work requirements for people with disabilities, pregnant people, those deemed medically frail, and caregivers for young children or family members with a disability.
A large majority of adult Medicaid beneficiaries who can work already do. Before the COVID-19 pandemic, 62 percent of adult Medicaid beneficiaries who were not enrolled in Medicare and did not meet Social Security disability criteria were either working or in school. A 2023 analysis found that an even larger proportion of working-age adults on Medicaid, 71 percent, were either in school or working full or part time. An additional 12 percent were caregivers, and some part-time workers were also enrolled in school or work training programs.
Medicaid’s main objective is to provide health coverage to people with low income. Experts have raised concerns that adding work requirements to the program could cause many people to lose access to critical health services. Some believe the new policy cannot be tested safely or ethically in low-income communities because it risks participants losing coverage, which could negatively impact their health.
Because of the unique challenges they face in securing and maintaining employment, complying with work requirements can be especially difficult for Medicaid beneficiaries. Employed adults who rely on Medicaid frequently work in low-wage positions with variable hours, such as service or retail jobs, which often do not offer employer-sponsored insurance or affordable coverage. These jobs can prevent them from consistently meeting monthly requirements to work 80 hours. Low-income people are also likely to experience other barriers to employment, such as limited access to transportation, lack of internet access, caregiving responsibilities, and chronic health problems — any of which can make finding or keeping a job challenging.
Work requirements also place significant reporting burdens on Medicaid enrollees. Even those who work more than 20 hours a week risk losing their coverage if they are unable to consistently document and submit proof of the number of hours they’ve worked. Reporting work hours can be especially difficult for people with multiple jobs, people without internet or computer access, and people with limited English proficiency.
Only two states have implemented Medicaid work requirements. Arkansas, the first, launched its program in June 2018 and ended it in March 2019 because of a court order. While the policy was in effect, the state required Medicaid beneficiaries ages 19 to 49 to report 80 hours of approved work or community engagement activities each month through an online portal. Failure to report hours for any three months without an exemption resulted in a loss of coverage for the remaining calendar year.
In July 2023, Georgia implemented its Pathways to Coverage program, which incrementally expands the population that’s eligible for Medicaid, provided enrollees fulfill a work reporting requirement. It’s open to parents and childless adults under age 65 with annual income up to 100 percent of the federal poverty level ($25,820 for a family of three in 2024). Because Georgia has not expanded Medicaid to adults with incomes up to 138 percent of poverty, as allowed under the Affordable Care Act, parents in Georgia prior to the Pathways program were eligible for Medicaid only if their income fell below 31 percent of the federal poverty level ($7,700 for a family of three in 2023).
Georgia’s work requirement policy is considered particularly restrictive because, unlike other state proposals to date, it does not systematically exempt populations that tend to struggle with employment, like adults with disabilities or those caring for a young child. Since its rollout, Pathways to Coverage has cost over $26 million, with more than 90 percent of spending on program administration, not medical services.
In Arkansas, more than 18,000 Medicaid enrollees lost coverage in the nine-month period in which the work requirement was in effect. The reporting process was a major driver of coverage losses: many Medicaid enrollees who were subject to the work requirements found the reporting process confusing or inaccessible, and nearly a third of the target population was unaware of the policy altogether. People who lost coverage reported delaying care and skipping medications because of costs, as well as incurring serious medical debt. And, critically, there was no increase in employment in the target population.
In Georgia, where the work requirement applies only to people newly eligible for Medicaid, coverage gains have fallen far short of what policymakers anticipated. In the first year of Pathways to Coverage, 4,231 people had enrolled in Medicaid through the program, well below the state’s first-year enrollment projection of 100,000. Georgia’s stringent requirements for documenting and reporting work hours have contributed to low enrollment numbers.
Other safety-net programs have had work requirements in place for more than 20 years, with only brief suspensions during economic declines and the pandemic. This includes the Temporary Assistance for Needy Families (TANF) program, which provides time-limited cash assistance to low-income families with children through federal block grants to states, and the Supplemental Nutrition Assistance Program (SNAP), a federally funded, state-administered program to subsidize food costs for people with low income. TANF and SNAP have work requirements with varying exclusions, and both are allocated federal funding for employment training and work supports, such as childcare subsidies, though evidence suggests this funding is insufficient to meet the need. CMS, on the other hand, does not allow Medicaid funding to be used for work supports.
The Congressional Budget Office has found that work requirements in TANF and SNAP have had mixed results. While work requirements in both programs have led to slight gains in employment, they have not increased average income in the target populations. That’s largely because income gains from people working more have been offset by income losses from people removed from the programs for not complying with the requirements. Many people who lose SNAP or TANF benefits because of work requirements remain in poverty, as they have few, if any, alternative sources of income.
Medicaid work requirements have been legally contentious. To implement them, states must submit a proposal to CMS, whose approval depends on the administration’s stance on the policy. While the Biden administration had made it clear it would not approve states’ work requirement proposals, that is likely to change under the new Trump administration. Governors and legislators in several states, including Arkansas, have signaled their intention to continue submitting proposals.
But even if CMS approves a work requirement proposal, it can be delayed or overturned by litigation. Federal courts ruled against the previous Trump administration’s approvals in Arkansas, Kentucky, and New Hampshire, halting implementation in Arkansas and preventing it in the other two states. The Supreme Court took up appeals from Arkansas and New Hampshire but ultimately sent the cases back to lower courts while vacating earlier decisions against work requirements in both states. As a result, there is no binding precedent, and the cases could be relitigated.
Georgia’s earlier approval under Trump was rescinded by Biden before the policy took effect, leading the state to sue the federal government. A federal court ruled in Georgia’s favor because the proposal expands coverage to a group of people not previously covered, and the state has since implemented a work requirement.
Publication Details
Date
Contact
Akeiisa Coleman, Senior Program Officer, Medicaid, Expanding Coverage and Access, The Commonwealth Fund
[email protected]