Introduction
In 2014, on the heels of a failed attempt to create a single-payer health care system in Vermont, policymakers turned their attention to how they might achieve their goal — lower health care spending and improved health outcomes — without disrupting the existing payment system. Their idea was to encourage the state’s largest payers — Medicare, Medicaid, and Blue Cross and Blue Shield of Vermont — to move more quickly from fee-for-service to risk-based contracting. In so doing, they would also encourage providers to pursue the state’s goals for improving residents’ health.
The concept appealed to OneCare Vermont, a large accountable care organization (ACO) that had engaged more than half the state’s physicians and nearly all its hospitals in its network but had struggled to earn savings in its previous contracts with insurers.
Under the “all-payer” ACO model, the three payers would steadily increase the number of patients cared for under risk-based contracts and provide additional financial support to OneCare to coordinate care for individuals considered to be high medical risks. In return, OneCare would take on downside financial risk for itself and participating hospitals, a move it hoped would spur the latter to collaborate with community partners in helping patients beyond their institutions’ walls.
OneCare’s vision is to unite the physical health, mental health, and social services sectors in serving patients with the most complex needs, much as the federal Accountable Health Communities initiative seeks to forge clinical and community partnerships to address factors such as unstable housing or social isolation that contribute to poor health.1 Rather than hiring its own staff to organize this effort, OneCare is relying on care coordinators already in the field as a result of Vermont’s Blueprint for Health. The Blueprint for Health, a statewide initiative, compels public and private payers to support nurses, social workers, community health workers, and others working to help patients manage their chronic conditions, find treatment for addiction and other behavioral health conditions, and connect with social supports.
OneCare offers these care coordinators additional funding as well as training and tools to collaborate. Its approach is purposefully nondirective: it assumes that given resources and opportunities to collaborate, communities will devise their own solutions. “We are not trying to come into a community and set up a different system of care,” says Sara Barry, OneCare’s director of clinical and quality improvement. “We’re trying to say, ‘How do we align with what you already have and bring those services more closely together?’”
This case study examines OneCare’s community-driven approach to care coordination, which it piloted in 2017 among a subset (around 29,000) of the state’s Medicaid beneficiaries. This year, the ACO is accountable for 42,000 Medicaid beneficiaries as well as 72,000 Medicare and Blue Cross and Blue Shield members.2 By 2022, Vermont aims to have nearly 70 percent of its 624,000 residents attributed to an ACO.3 Although the initiative is in its early stages, Vermont’s experiment in forging partnerships among health care payers and between clinical and community providers may offer lessons about the potential of care coordination to wring value out of a fragmented health care system.
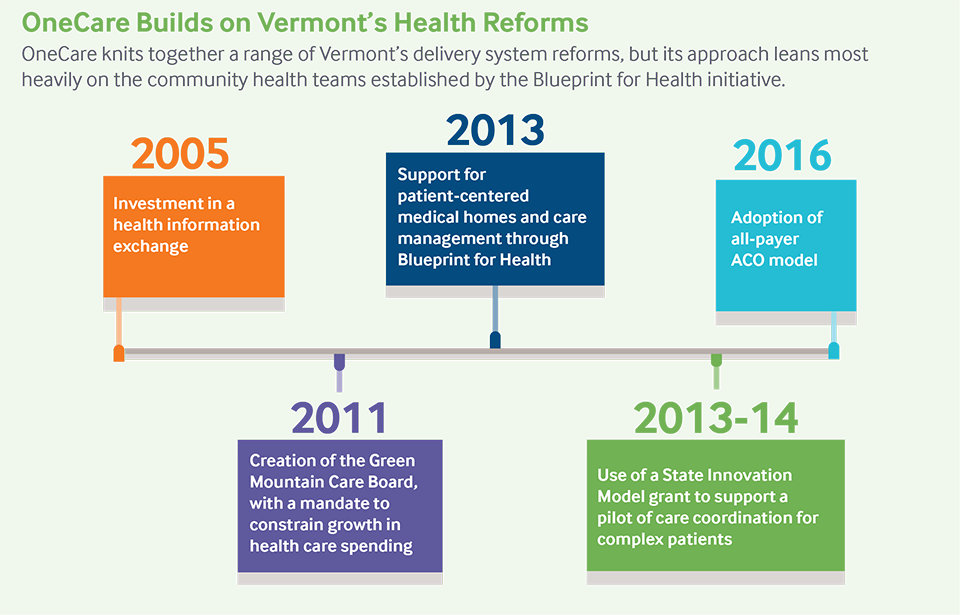
Note: Blueprint for Health legislation passed in 2006. A 2010 law expanded the pilot statewide and guaranteed by 2013 access to providers that wanted to participate. As of the first quarter of 2018, nearly all of Vermont’s primary care practices — 140 — had achieved patient-centered medical home recognition.
Building on Vermont’s History of Reform
OneCare Vermont was created in 2012 by two academic medical centers serving the state — the University of Vermont Medical Center and the Dartmouth-Hitchcock health system — and now includes 10 of the state’s 14 hospitals, a majority of its primary care and specialty care practices, and 21 of its 40 nursing homes.4 As noted above, what makes it different from many other ACOs is its engagement of partners other than hospitals and physicians: Area Agencies on Aging, mental health agencies, home health providers, and other community groups that are part of the ACO but unlike participating hospitals not at financial risk for its results. Its ability to do so is a function of the state’s past reforms to the health care delivery system, most notably the Blueprint for Health, which provides financial support for creation of patient-centered medical homes and “community health teams” made up of nurses, social workers, dietitians, asthma educators, community health workers, and others in each of the state’s 14 health service areas (HSAs).5
What Is the All-Payer ACO?
Vermont is partnering with the federal government in an ambitious effort to shift nearly all payment for medical services from a fee-for-service model to a value-based one that rewards providers for achieving the state’s cost-containment and quality-improvement goals. Under the all-payer model, Medicaid, Medicare, and Blue Cross and Blue Shield of Vermont (which has a nearly 90 percent share of the commercial market) have agreed to enter into contracts that require providers to assume the risk for meeting financial targets and performance benchmarks.
Over the course of five years, participants are expected to incrementally increase enrollment such that by 2022, 90 percent of all Medicare beneficiaries and 70 percent of commercially insured residents are covered by risk-based contracts (the state has not set specific targets for the Medicaid population). The approach has some similarities to that of Maryland, which seeks to contain health care spending by setting the rates by which all third parties — Medicare, Medicaid, and commercial insurers — pay for hospital care.6
Medicaid Next-Generation Pilot
In 2017, OneCare assumed financial risk for some 29,000 Medicaid beneficiaries (about 20 percent of the state’s total) in four regions: Berlin, Burlington, Middlebury, and St. Albans.7 It took responsibility for providing most medical and behavioral health services for these beneficiaries, from a budget of $90 million.8 Like Medicare’s Next Generation ACO Model, which was also launched in 2017, the Medicaid program offered the ACO the option to receive capitated payments.9 If actual expenditures in 2017 fell below the budgeted amount, OneCare would keep the first 3 percent of savings; if expenditures exceeded it, OneCare would make up the first 3 percent.
As part of the agreement, Vermont’s Medicaid agency ceded to OneCare some of its care management functions. The agency had been focusing its support on patients in the top 5 percent of health care spending. OneCare proposed to engage a broader population, including those with chronic diseases or behavioral health conditions who might be at rising risk. It also wanted to do away with eligibility criteria restricting which patients could be offered support, because the ACO’s leaders said these were administratively burdensome and left too many people out.
To identify Medicaid beneficiaries who may need support, OneCare analysts aggregate demographic information, data from the medical records of physicians and hospitals, and claims data supplied by Vermont’s Medicaid agency. They then analyze the data using a risk-prediction algorithm licensed through Johns Hopkins University that categorizes each Medicaid beneficiary — a mix of adults (45%); children (49%); and aged, blind, and disabled individuals (6%) — into one of four groups based on their predicted morbidity over the next year (Exhibit 1).10 Patients’ risk categorization is then provided to local care coordinators, who can then adjust it based on their knowledge of the patients and conversations with clinicians.
For example, based on claims data alone, an individual may not be identified as being at high or rising risk. But the care coordinator understands this person needs additional support because of a recent bout of homelessness or a death in the family.
Coordinating the Care Coordinators
As noted, OneCare does not hire staff care coordinators. Instead, it offers employees at partner organizations the funds and resources required to help patients manage their medical conditions and address their social, financial, and psychological challenges. These professionals include:
- case managers, often nurses or social workers, who work as part of community health teams or are hired directly by primary care practices
- social workers and nurses employed by Area Agencies on Aging
- social workers, counselors, and other staff members working for the state’s hub-and-spoke system, which provides medication-assisted treatment for opioid use disorder
- social workers employed through the Support and Services at Home (SASH) program, which primarily helps older adults.11
Care coordinators offer support to patients who have been identified as being at high or rising risk. In 2017, 16 percent of patients — about 4,780 — were identified as such; thus far, about a third have a care team identified, and a quarter have a lead care coordinator who is responsible for coordinating with an individual’s care team. During initial encounters, the coordinators ask patients to tell them about their lives, their challenges, and the kinds of support they might need to achieve their goals.12 They typically use diagrams known as ecomaps to help patients and families visualize the social, financial, and medical support systems people already have in place and where they may need additional support. They may then show patients domain cards — each with a word and/or picture illustrating factors that can affect health, such as finances, housing, medication, and transportation — and ask them to select those that represent their immediate and longer-term priorities, whether that is finding reliable transportation or a better-paying job.13

** The Support and Services at Home (SASH) program is funded through Vermont’s Blueprint for Health.
To complement these qualitative approaches, care coordinators may use screening tools. One is the Vermont Self-Sufficiency Outcomes Matrix, which assesses patients’ functional health and the adequacy of their income, housing, health care coverage, and other social supports.
A frequent next step is for the care coordinator to convene a conference, inviting the patient and members of the support team identified on their ecomap. During the conferences, participants delineate each person’s role in supporting the patient, highlight any gaps in services or duplicative activity, and choose a lead care coordinator (if indicated), who then works with the patient to create a shared care plan. Some patients with complex needs may benefit from frequent conferences, while others may be seen by the full care team quarterly or yearly or when circumstances change.
When Blueprint for Health started, it was like, OK, here’s 14 communities; go ahead and do it 14 different ways. And now the conversation has become, how do we create some consistency statewide?
Each care plan outlines two goals identified by patients and two steps that might help them achieve these goals, such as signing up for Meals on Wheels in order to eat two regular meals daily. Care coordinators encourage small, practical steps, often translating clinicians’ advice into a course of action. “Someone might say, ‘My doctor just told me I’m prediabetic and need to eat better and exercise. What does that mean? I’ve been eating the same way for this long. I can’t run,’” says Stefani Hartsfield, former assistant director for Vermont’s SASH program. “So there is someone there to help figure it out.”
By focusing on patients’ goals — rather than physicians’ or care coordinators’ — care coordinators can help identify the underlying reasons why people may not make their health a priority. In one case, a woman with unmanaged diabetes and other chronic conditions said her primary goal was to figure out what had happened to a son she had given up for adoption decades earlier. A SASH care coordinator worked with the woman to locate her son, who was doing fine. Now reassured about his well-being, she chose to make managing her health conditions her next goal.
On a given day, care coordinators might offer a counseling session to a patient with depression or anxiety, help another find housing or job training, and provide education to help someone else manage a chronic disease like diabetes. They also might accompany patients with behavioral health problems to their primary care visits. Some coordinators are embedded in primary care offices or emergency departments to identify patients in need of support and connect them with multidisciplinary care teams.
Care Navigator
OneCare’s leaders worked with creators of the software platform Care Navigator to configure it to meet the needs of care coordinators who wanted a better way to communicate than phones or fax machines. As a supplement to patients’ electronic medical records, the software makes clear which health and social service staff are working with which patients and creates a system of notifications and prompts about hospital admissions, discharges, and other events. Using new tools and automated workflows, care coordinators can create task lists and track activities, while lead care coordinators use the software to facilitate collaboration. The software includes a library of educational resources for patients. It also enables them to upload photos and other information about themselves and to securely send notifications and messages to members of their care team.
Care Navigator also provides a platform for OneCare to document the services care coordinators provide, monitor their impact, and identify patterns — for example, the common unmet needs of dementia patients. Part of the additional funding OneCare provides to care coordinators covers the cost of conducting more systematic needs assessments, documenting them in Care Navigator, and using the technology to communicate and coordinate with one another. In 2017, 480 care coordinators were trained to use the system, and more than half had begun actively using it.
The software platform is used in other states by another ACO, a federally qualified health center, and behavioral health and long-term services and support organization consortiums to improve communication and coordination.
Goals and Shared Care Plan
Teams enter patients’ goals, then associate them with a particular domain of health or social determinant to enable analysis across communities.
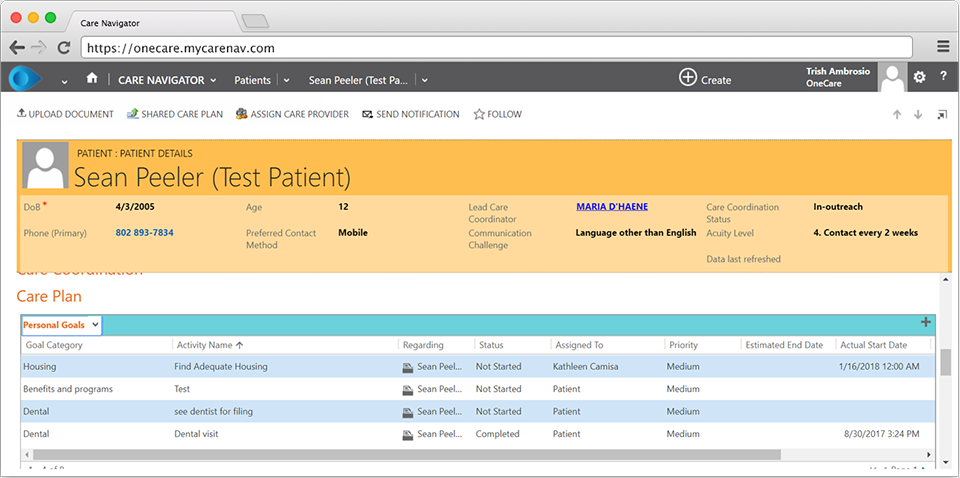
Patient Resources
About Me section contains information about what’s important to patients, the results of patient assessments, and access to a library of educational resources.
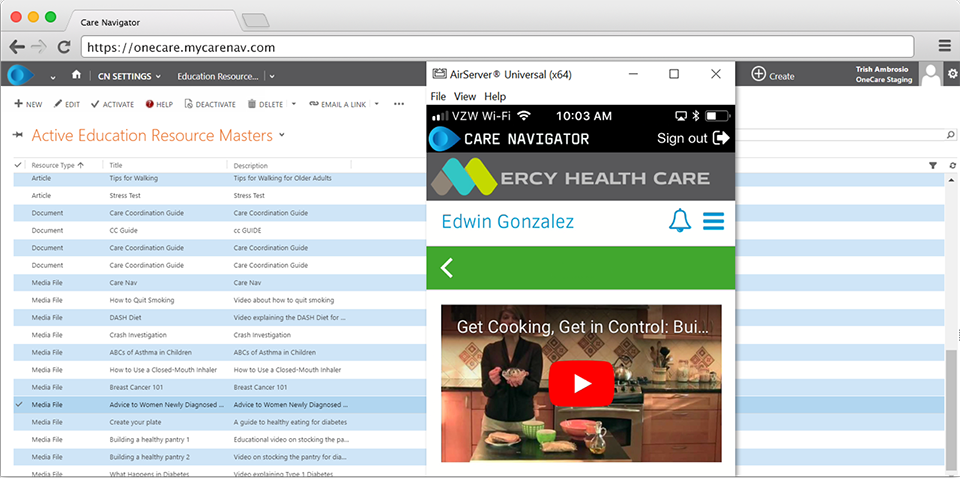
Documentation
The system logs the activities care coordinators perform day to day, triggering payment from OneCare for completing designated tasks.
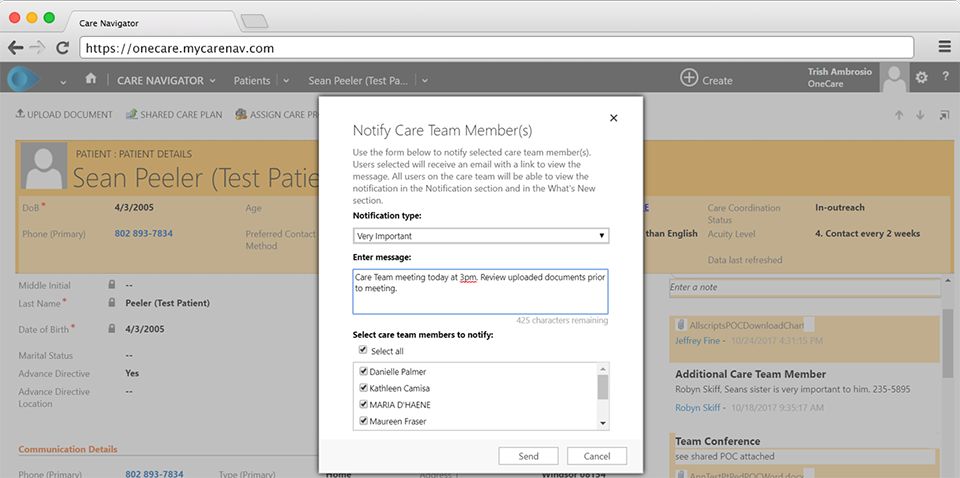
Screenshot images above © Copyright 2018 Intraprise Health. All rights reserved.
Nancy Reynolds, a SASH coordinator in St. Albans, leads exercise and wellness classes at senior housing centers. She also makes regular home visits to check on isolated seniors, including a woman in her late 80s who runs a farm and, like a number of rural Vermonters, speaks only French.
All this work is organized through Care Navigator, a proprietary software platform that OneCare licensed to give care coordinators a way to collaborate. Once patients’ shared care plans are created, different team members can use the platform to document the steps they’re taking to help patients meet their goals. Records are accessible to all members of the team (with plans to expand to patients and their caregivers later this year), and members can communicate with one another as needs change. Reynolds sees this technology as game-changing. “I will know I’m not working in a vacuum,” she says.
Sharing Best Practices and Promoting Standardization
With the variation in patients’ needs and provider networks, OneCare has given each region involved in the Medicaid pilot — Berlin, Burlington, Middlebury, and St. Albans — some flexibility in developing priorities and care coordination approaches.14 At the same time, the ACO has sought to assess what’s working and to promote standardization, in part by convening monthly meetings of administrative and frontline staff from participating health and social service organizations.
At these in-person and virtual “Core Team” meetings, participants describe the various care coordination activities under way in their regions and explore ways to leverage resources most effectively, building on work already begun through the Blueprint for Health. The Core Team meetings also offer opportunities for care coordinators and their supervisors to brainstorm potential solutions to shared challenges.
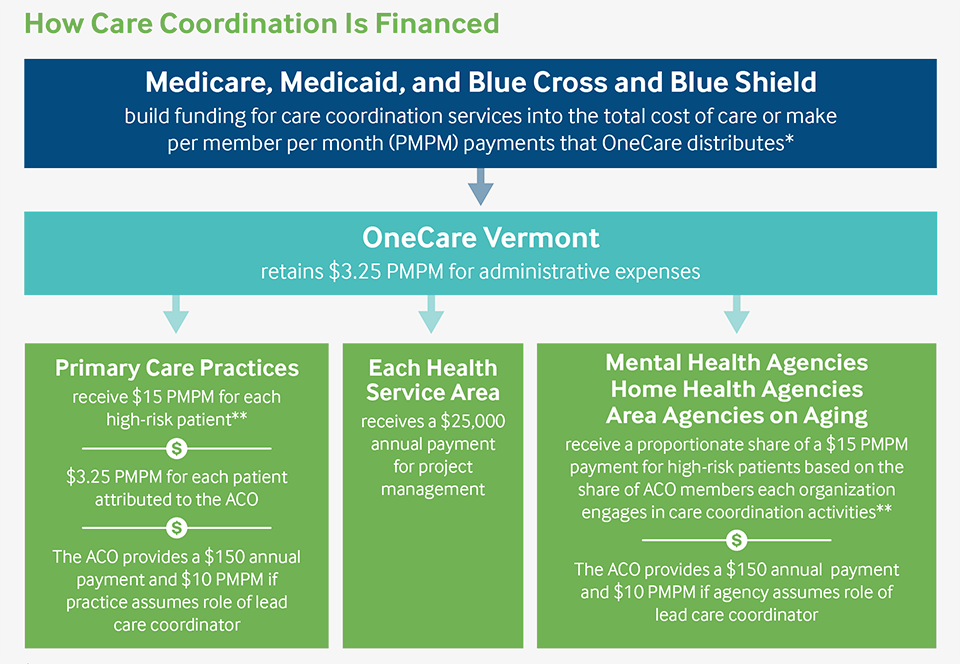
** The population defined as “high risk” varies by payer. For example, in the Medicaid contract, 16 percent of beneficiaries are deemed high risk; for the Blue Cross and Blue Shield contract, only 3 percent are.
In the summer of 2017, Jane Suder, R.N., who oversees care management at Northwestern Medical Center, presented the story of a local woman with chronic obstructive pulmonary disease, diabetes, anxiety, and apparent cognitive impairments. The woman had lost her housing, leading her repeatedly to the emergency department, sometimes because of a medical complication and sometimes because she didn’t know where else to go. “It’s trying to help figure out how to assist people with similar needs who really need a village around them,” Suder said. The group discussed ways to secure short-term motel stays for the woman until longer-term housing could be arranged, as well as how to meet her medical needs and expedite her enrollment in Medicaid and other benefit programs. They also discussed using the Care Navigator software to create a central repository of available resources and best practices for helping patients with such complex needs.
To support the work of the Core Team and the rollout of the Care Navigator software, OneCare has launched a training series for care coordinators, supervisors, and other leaders and is developing standard job descriptions and promoting professional competencies such as using ecomaps and domain cards or creating shared care plans.
Provider Payment and Allocation of Financial Risk
OneCare receives additional funding from payers to support care coordination activities and distributes it to ACO participants in a way designed to promote shared responsibility (Exhibit 2). It provides $25,000 annually to support project management in each of the pilot’s four regions, while per member per month payments are distributed to primary care practices as well as to Area Agencies on Aging, home health agencies, and mental health agencies. These participants are not at financial risk under the ACO contract, and the additional payments are a substantial increase over Blueprint for Health’s funding for community health initiatives, which has remained level for several years. For instance, smaller primary care practices (such as those with two staff physicians and 600 attributed patients) may earn as much as $38,000 in additional revenue during a year. “In some cases, practices have been able to use these additional funds, combined with their Blueprint funding, to hire another care coordinator,” says Sarah Jemley, OneCare’s care coordination program administrator.
We have so many different community agencies that are in many ways driven by altruism and have budgets that are short already. We are trying to redistribute dollars from high-cost events to upstream community support services.
Participating hospitals receive fixed payments, thus taking downside financial risk, which is “key to unlocking profound change in how hospitals interact with the community,” says Norm Ward, M.D., OneCare’s chief medical officer.
Although leaders at some of the state’s small hospitals were initially reluctant to take on financial risk, given thin operating margins, nearly all eventually joined. They understood that current payment models were unsustainable and “want to be on the ground floor of creating a new approach,” says Stephen Leffler, M.D., the University of Vermont’s chief population health officer.
Hospitals were also drawn by the prospect of having access to OneCare’s analytic tools, which enable panel management, performance tracking, and care coordination. “In the past it’s been us saying to hospitals, ‘Here are five things you can focus on to improve care and capture savings,’” says Todd Moore, OneCare’s CEO. “Now the hospitals are calling to say, ‘Run me a query on everyone who has tested positive for prediabetes.’ They are clamoring for more and more specific data on where they think there are opportunities to improve care and achieve savings.”
OneCare hopes that this blend of financial carrots and sticks will be sufficient to encourage hospitals, ambulatory care providers, and social service providers to work together to improve population health and contain health care spending — an approach that in 2018 it extended to patients covered by Medicare and Blue Cross and Blue Shield’s commercial insurance. Under the all-payer ACO, these insurers have committed to supporting coordination of community-based care, aligning performance measures, and shifting to greater use of risk-based contracting. Pat Jones, the health care project director for Vermont’s regulatory body, the Green Mountain Care Board — one of the signatories to the all-payer ACO contract — says this should encourage “all boats to row in the same direction” and reduce the “noise” created from working under contracts with varying benchmarks and expectations.15
Harmonizing performance measurement among Vermont’s three largest payers also helps focus attention on the state’s priorities: expanding access to primary care, reducing the prevalence and morbidity of chronic disease, and reducing the number of deaths from suicide and drug overdose. In coordination with the Green Mountain Care Board, OneCare and its payers are working to align quality performance targets around these population health goals. It hopes to eventually reduce the total number of quality metrics across payer contracts to 17 from 44.
Early Results
While medical claims are still trickling in for 2017, preliminary data suggest that OneCare is making progress in achieving the state’s population health goals. They show that Medicaid beneficiaries attributed to the ACO are making greater use of primary care and behavioral health services, as well as pharmacy benefits, compared with other beneficiaries. Over the first nine months of the contract, for example, the percentage of beneficiaries with early to late-stage disease who lacked a primary care visit fell to 2 percent from 4 percent. Those who were deemed to be at high or rising risk (levels 3 and 4) also had substantially fewer emergency department visits during the first nine months of 2017 compared with similar periods in the prior two years, and fewer hospitalizations compared with the prior year (Exhibits 3 and 4). “These changes in utilization were what we had hoped and expected to see,” OneCare’s Sara Barry says. “Nothing about this model is about rationing care.”
OneCare has found Medicaid beneficiaries deemed to be at highest risk are a relatively stable group, with little movement from one risk category to the next over time. This information lends credence to the ACO’s approach of targeting services to the subset of patients who might benefit the most.
Despite these improvements, the ACO is not likely to achieve savings in the first year of the Medicaid contract. The total cost of care for 2017 was forecasted to be 1.5 percent above budget, meaning the ACO would owe money back to the state.16 Moore, the CEO, says preliminary data show that the four hospitals that received prospective payments reduced hospitalizations and other institutional care sufficiently to achieve savings. However, these savings were offset because some Medicaid beneficiaries attributed to the ACO sought care outside those hospitals, including at out-of-state hospitals, leading to fee-for-service charges that tipped the balance in the first year. (In 2018, 10 of the ACO’s hospitals will have assumed downside risk, lessening the chances that a patient will receive care from an institution that is paid on a fee-for-service basis.)
To call attention to opportunities for cost savings and performance gaps, OneCare is tracking cost, utilization, and performance on quality measures at the hospital and regional levels through a software platform that allows users to drill down to the facility, provider, or patient level.
Ultimately, the definition of success for the ACO may vary by payer. The state wants to constrain growth in health care spending to 3.5 percent annually and has prioritized three population health goals, on which OneCare appears to be making headway. But leaders at Blue Cross and Blue Shield want to see savings for their customers and evidence that the community health teams are reaching its members, particularly those with complex needs whom the health plan’s care managers have had difficulty engaging. “If they can figure out a way to do that, that’s very exciting and would have value,” says Josh Plavin, M.D., M.P.H., Blue Cross and Blue Shield’s chief medical officer.
Looking Forward
OneCare’s bold experiment has been enabled by Vermont’s small size, which engenders trust and familiarity among health system leaders and policymakers, and by the lack of competition among private insurers, including Medicare Advantage plans. OneCare has also built on the state’s long-term commitment to health reform, including the creation of the Green Mountain Care Board to constrain spending and the pursuit of a federal State Innovation Model grant, which supported the development and testing of an integrated approach to complex care management. Vermont’s aging and declining population has also created pressure for reform.
Even with these tailwinds, OneCare faces significant hurdles. Much of its early focus has been on community-led care coordination — supporting the customization of a technology platform to facilitate communication, providing training in best practices for engaging high-risk patients, and developing analytic tools to identify risk and evaluate impact. More extensive institutional reforms may be harder to accomplish, yet it may be that changes in provider behavior will lead to the greatest cost savings. “In the short term, I firmly believe that we can save money around transitions of care and by delivering much-needed mental health and substance abuse treatment,” Stephen Leffler, of the University of Vermont, says. “But driving costs out of the hospital, direct costs or fixed costs, and redistributing those out into the community in a meaningful way is going to be difficult.”
With a rapid timeframe for implementation, the all-payer model also requires the ACO to keep its eye on three distinct populations at once and meet the competing demands of its payers. Studying the impact of myriad approaches will be critical to winning support for the care-coordination approach. Without evidence of impact, employers may be reluctant to sign on to the all-payer model.
“These are businesspeople who need to have some compelling evidence to suggest that there’s a reason to get involved, that there’s a reason to put dollars at risk potentially, or just to fund additional administrative costs to support the operation of an ACO,” says Andrew Garland, vice president of client relations and external affairs at Blue Cross and Blue Shield.
Through its data analytics infrastructure, OneCare is attempting to add rigor and measurement to the work of care coordinators. Assessing comparative performance, however, may not be easy, given the variation both in the population of HSAs and in their problem-solving techniques. Many rely on different staffing configurations — for example, some depend on credentialed care coordinators, while others use lay workers.
But if OneCare is successful at identifying and spreading innovative approaches, it could accelerate investments like these not just in Vermont, but in other parts of the nation where leaders are seeking more evidence on effective ways to address the social determinants of poor health.
