Concerns over how private equity is affecting health care access, quality, and costs in the United States have exploded in the past few years, reflecting the growing activity of private investors in health care markets.
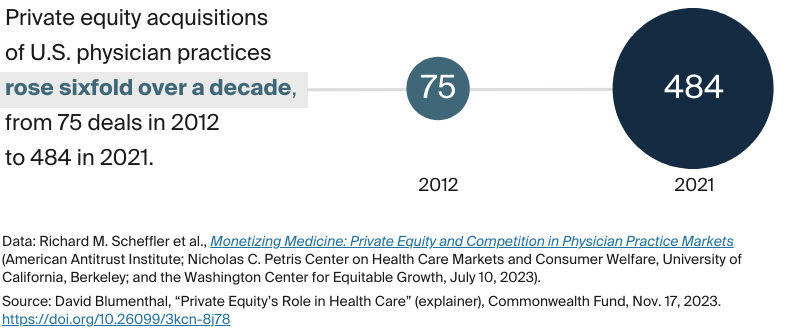
Private equity investors spent more than $200 billion on health care acquisitions in 2021 alone, and $1 trillion in the past decade. Private equity firms have long been active in hospital, nursing home, and home care settings. But recently, acquisitions of physician practices have skyrocketed, especially in high-margin specialties like dermatology, urology, gastroenterology, and cardiology. A recent study showed that in 13 percent of metropolitan areas, a single private equity firm owns more than half of the physician market for certain specialties.
Given their potential impact on the cost, quality, and access to health care in the U.S., these developments have generated considerable interest among federal and state policymakers.
What is private equity?
Strictly speaking, private equity in health care is a form of for-profit ownership reflecting investment in health care facilities by private parties. In general, for-profit health care organizations can take two forms: private or public.
- Public, investor-owned organizations sell shares to the public that trade on a stock exchange. UnitedHealth Group, which now owns thousands of physician practices, is one example. Another is Hospital Corporation of America. These organizations are regulated by multiple federal laws and agencies, including the U.S. Securities and Exchange Commission.
- Shares of private, investor-owned organizations — such as private equity–owned firms — are not traded on public markets. As such, they aren’t required to follow the same regulations as public companies.
As a form of ownership, private equity is not new to health care. A variety of private investors have invested in and owned health care facilities in the past. These have included individual physicians who invest in and own their for-profit private practices and pay taxes on their earnings. Physicians and other private investors have long owned health care facilities, such as specialty hospitals, dialysis units, ambulatory surgical centers, and imaging units.
What’s different now about private equity in health care?
There have been two key shifts in recent years. The first is in who’s doing the investing. Instead of physicians or small groups of investors using their own funds, investors now also include firms that manage funds for large groups of wealthy individuals or institutions. Fund managers and their investors may have little knowledge of health care, viewing it as just another market opportunity.
The second change relates to how they’re investing. Aggressively pursuing quick profits, some private equity firms are taking out loans, using their newly acquired health care facilities as collateral. The loans are used to pay back investors quickly and handsomely, while the health care organizations carry the debt. Another strategy is to sell the health care organization’s land, facilities, and other capital assets to other investors. The proceeds from the sales generate returns for fund managers and their investors. Health care organizations then rent those assets back from the new owners.
A third approach to getting a quick return is to flip the asset — selling the newly purchased health care organization to another buyer, such as a publicly traded company like CVS or Amazon, for a large multiple of the original price. To attract such a buyer, however, the private equity firm must boost the organization’s profits, which usually requires rapidly cutting costs, raising prices, or increasing the number of services provided.
All these strategies are legal, but until recently they hadn’t been deployed as widely or intensively in health care.
How does private equity impact health care costs, quality, and access?
More research is needed on how private equity ownership affects health care costs, quality, access, and equity. So far, the results on cost are clearest. Given its short-term financial focus, private equity tends to increase health care prices and utilization — and thus costs — to both patients and the larger society. Some new private owners of health care facilities may adopt reforms that make care more efficient and reduce costs, thus improving value. And there are examples of promising innovations, such as CareMore, a privately funded organization that reengineered care for high-risk elderly individuals. But in general, it’s much easier, and more common, for private owners to raise prices and volumes and to focus on high-margin services.
Regarding quality, there is no evidence that private equity ownership leads to systematic improvements in care. In fact, a widely cited study of nursing homes acquired by private equity owners showed a 10 percent increase in mortality among Medicare patients. However, there haven’t been additional studies demonstrating such dramatic, harmful effects.
In terms of access to care and equity, the financial pressures on acquired facilities to pay rent or repay loans are raising alarms about possible bankruptcies and closures of hospitals, nursing homes, and other health care facilities. This is especially concerning for those serving poor and rural communities, since these entities tend to be less lucrative financially.
Why are private equity firms investing in health care?
Several factors have driven private equity’s attraction to health care in recent years. One has been the low cost of capital resulting from low interest rates, which has spurred an influx of investors seeking to earn a piece of the $4 trillion health care economy.
A second factor has been the increasing commercialization of health care, which has made it more acceptable for private investors to treat health care — traditionally a nonprofit sector — like other markets. In fact, some nonprofit health care organizations have begun to look more and more like their for-profit brethren. Nonprofits have sought near-monopoly power in local markets through widespread mergers and acquisitions, which have enabled them to raise prices sharply. Compensation for nonprofit executives has also skyrocketed, as have their organizations’ capital reserves.
A third factor has been the ongoing failure of the U.S. health care system to deliver value and keep Americans healthy. With falling life expectancy, increasing maternal mortality, glaring inequities, soaring costs, and punishing medical debt, our health system is ripe for disruption. Private investors — with their energy, fresh perspective, and capital — offer hope for change.
What’s next for private equity in health care?
As interest rates rise and investors pick the low-hanging fruit in health care, it seems unlikely that private equity will maintain its current rate of expansion into the sector, at least for the short term. Public scrutiny of private investment in the health sector is also increasing, as concerns grow about the effects on costs, quality, equity, and access.
Policymakers’ first step in addressing these concerns will likely include new transparency rules to make it clear who owns private, for-profit health care organizations. Congress is considering such requirements, and the Security and Exchange Commission has issued a new rule requiring increased transparency about the identity of investors in private equity arrangements. It seems doubtful, however, that greater transparency rules alone could slow private equity’s penetration of health care markets.
Other potential changes include reforming antitrust laws to open the sale of local physician practices to scrutiny. The Federal Trade Commission recently sued a private equity firm that has been trying to dominate the anesthesia market in areas of Texas.
Some scholars believe that private equity serves as a divining rod for failures in our current health care market. Investors, they believe, are simply exploiting the system’s weaknesses for profit. In this sense, the growth of private equity is a symptom, not the cause, of our health system’s failure to meet the needs of Americans.
