Executive Summary
Instability in coverage is a natural outgrowth of the patchwork health insurance system in the United States. People covered through employer-based insurance may lose coverage if they change jobs, their employer decides to stop offering insurance, or their share of the cost of the coverage becomes unaffordable. Coverage gaps also arise when people try to move from employer-based to public coverage, because the process is rarely facilitated and a large portion of those who lose job-based coverage are not eligible for public coverage. In addition, gaps occur within public coverage programs, triggered either by changes in family circumstances that make individuals ineligible for public insurance or by administrative complexity or other difficulties that result in failure to renew coverage. One study showed that over a four-year period, nearly four of 10 Americans under the age of 65 experienced one or more gaps in private or public health insurance coverage.
This report examines the extent, causes, and consequences of instability in public coverage programs for children and families. It focuses particularly on the phenomenon of "churning," which occurs when individuals lose and regain coverage in a short period of time, suggesting that the loss of coverage is not due to eligibility factors. It also looks at strategies that can make public program coverage more stable for children and families.
The findings are drawn from a variety of sources, including national and state studies, roundtable discussions and interviews with stakeholders and experts, and an in-depth examination of how state and local policies have affected instability and churning in four states: Louisiana, Rhode Island, Virginia, and Washington. The states were chosen based on their demonstrated interest in the issue of churning, the potential to find useful data, and a willingness on the part of state officials to participate. For a full discussion of the study states, see the Appendix.
Paying attention to the problem of coverage instability within public insurance programs, chiefly Medicaid and the State Children's Health Insurance Program (SCHIP), makes sense for several reasons.
- Coverage instability affects millions of children and families each year, taking a considerable toll on their ability to access needed health care in a timely manner and in an appropriate and cost-effective setting.
- Instability and churning result in a substantial amount of wasted time and spending. Medicaid and SCHIP officials, as well as health plans and providers that serve Medicaid and SCHIP enrollees, report significant costs related to churning.
- Solutions are at hand; coverage instability and churning on and off of public coverage are not intractable problems.
Churning Has Significant Consequences
Interventions to avert unnecessary instability and churning are important because the consequences in terms of health care delivery and costs are significant. While there is no single source of data on the extent of instability and churning in Medicaid and SCHIP, program administrators, health plan executives, and health providers agree that the problem is substantial. For example:
- Data from Louisiana show that over a two-year period, beginning in January 1999, 18 percent of children had a gap in Medicaid coverage. After significant changes in policy and practices, that proportion declined to 6 percent over a two-year period, beginning in January 2003.
- Data from Rhode Island's Medicaid agency show that one of four enrollees had a gap in Medicaid coverage over a 12-month period. Churning was common; about 60 percent returned to the program within the year.
- Virginia found that over an 18-month period, beginning in March 2004, about one-third of the children enrolled in Medicaid or SCHIP lost their coverage at some point.
- Washington's Medicaid agency found that in a three-month period in 2004, more than one-third (36%) of children whose coverage was terminated were reenrolled.
Table ES-1. Consequences of Insurance Instability and Churning | ||||
| Consequences | Groups Most Affected | |||
| States and Localities | Health Plans | Providers | Consumers | |
| Costs associated with enrolling, disenrolling, and reenrolling beneficiaries, including extra paperwork, system updates, extra mailings | x | x | x | |
| Costs associated with delivering "new member" services multiple times | x | x | ||
| Additional administrative costs associated with researching and reconciling billing problems | x | x | x | |
| Costs associated with verifying enrollment status, counseling consumers about coverage status, and assisting with enrollment | x | x | x | |
| Extra investments to attempt to help families retain coverage | x | x | x | |
| Extra staff time and costs to track and assist individuals participating in disease management programs who have lost coverage | x | x | ||
| Reduced effectiveness of disease management programs | x | x | x | x |
| Cost-shifting and depleted resources when Medicaid SCHIP payments are not available to reimburse safety-net providers | x | x | x | |
| Compromised continuity of care as returning enrollees are assigned to different plans or providers | x | x | x | |
| More difficulty measuring quality of care | x | x | x | x |
| Difficulty arranging care, particularly specialty care | x | x | ||
| Difficulty getting care, including preventive care | x | |||
| Unmet health care needs | x | |||
| Care provided in inappropriate settings | x | x | x | x |
| Higher costs for care when individuals reenroll | x | x | x | x |
| Source: Authors' analysis of data. |
Changes in Public Programs Can Substantially Reduce Churning
The causes of churning have been examined over the past several years and a range of practices that can contribute to coverage stability has been identified. However, a close examination of state experiences shows that these steps, taken in isolation, may have only limited value unless states commit to systemic changes.
Preventing loss of coverage at renewals. Churning is driven to a significant degree by low public coverage renewal rates. Many states have attempted to reduce renewal problems by developing simplified forms, streamlining verification requirements, and providing renewal assistance. These are important steps, but solutions that appear to have the greatest impact go to the heart of the problem: reducing the frequency of renewals and eliminating renewal requests when needed information is already on hand.
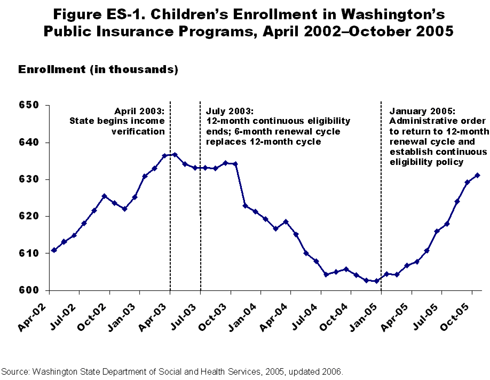
Washington's experience highlights the extent to which frequent renewals contribute to coverage gaps and instability. In 2003, as a result of budget pressures, Washington reversed some of the steps it had taken in earlier years. It eliminated "continuous" eligibility and required families to renew their eligibility every six months instead of annually. When the state reversed course yet again and returned to 12-month renewal periods, enrollment rebounded (Figure ES-1).
Louisiana has eliminated traditional renewals when it already has the information needed to evaluate children's ongoing eligibility through other program records and state databases. Instead of automatically sending renewal forms to families, the state conducts an internal eligibility review—or "ex parte" review—by examining Food Stamp Program records and other information available to the Medicaid agency. Families can be contacted by telephone if additional information is needed to complete the review. With these procedures in place, the more formal and complicated renewal process proves unnecessary for two of three children, thus dramatically reducing the number of children who lose coverage at renewal. At the same time, administrative costs associated with the renewal process and churning have decreased.
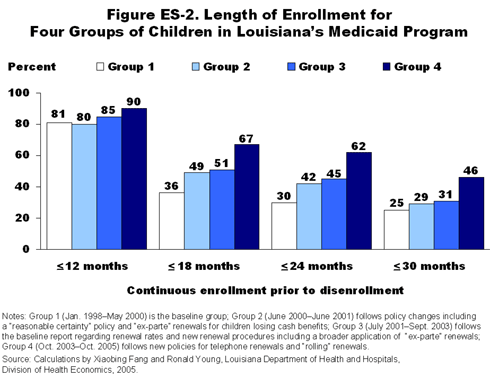
In Louisiana, comprehensive changes in the renewal process were accompanied by an explicit philosophical decision to make retention among eligible children a priority. As a result, Louisiana significantly improved the continuity of coverage for children (Figure ES-2).
Preventing transitions across public programs from disrupting coverage. Even though eligibility for Medicaid is no longer linked in any way to eligibility for or receipt of food stamps or Temporary Assistance for Needy Families (TANF) benefits, system failures, administrative burdens, and the lack of clear information for families can result in the loss of Medicaid coverage when welfare or food stamp benefits stop. In states that cover children through two different child health coverage programs, shifts in eligibility between SCHIP and Medicaid also can result in coverage gaps.
Washington has taken a number of steps to correct problems that had led to the loss of health coverage. Twelve-month continuous eligibility and computer system changes ensure that when cash benefits for a child end, the child's eligibility status is changed in the database and medical benefits continue. The system also facilitates simple and relatively seamless transfers among the three public coverage programs for children.
Mitigating the impact of premiums on churning. Premiums in SCHIP and Medicaid may contribute to coverage instability and churning, under certain circumstances, and recent federal law changes might prompt more states to consider imposing premiums. States have authority to impose premiums in SCHIP, subject to certain limitations, and now the Deficit Reduction Act of 2005 allows states to charge premiums in Medicaid for children whose family income is above 150 percent of the federal poverty line. The extent of coverage loss and churning that might result from premiums will depend on several factors, including the amount of the premiums, income levels of the families required to pay the charges, number of family members covered by the premiums, and procedures in place to facilitate premium collections. Two of the study states—Rhode Island and Virginia—have had some experience with premiums and each has closely watched the impact that premium payments may be having on enrollment and disenrollment. Although a premium was charged initially for SCHIP coverage in Virginia, the premiums were discontinued in 2002 when data showed that large numbers of children would have lost coverage if sanctions for nonpayment were imposed as originally planned. Rhode Island is implementing new policies related to methods for paying premiums to lessen the coverage losses that have occurred among the relatively small portion of enrollees who are charged premiums in its Medicaid program.
Other Factors Help to Reduce Churning
Beyond a state's particular policies and procedures, two additional factors appear to reduce instability and churning: measuring enrollment dynamics and having strong leadership focused on securing coverage for eligible children and families.
Importance of routine, standardized measurement. Consistent, routine measurement can demonstrate what does and does not work and pinpoint any needed adjustments. It also can help to establish accountability among public program staff.
While all states collect enrollment data, not all collect the data needed to provide a clear picture of enrollment dynamics. At a minimum, it is important to know how many people are entering and exiting the program each month. Measuring renewal rates and understanding the reasons for loss of coverage at renewal will clarify how much churning is occurring before and after interventions. In addition, longitudinal analyses that show enrollment patterns over time are essential to fully understand churning.
Many program and health plan administrators expressed a need for guidance about methods to measure insurance instability and churning. States vary considerably in terms of their capacity to report on renewal outcomes. Among states that track renewal outcomes or report on reasons for case closures, data elements and definitions differ considerably and coding regarding the reasons for loss of coverage is not precise. State-specific data on churning rates are limited and are not comparable across states because the analyses define and measure churning differently. Analysts noted that they would prefer not to "reinvent the wheel" and would welcome recommendations based on experience in other states. To set goals, administrators said that it would be helpful to know how to define and calculate a reasonable level of churning.
Leadership is key. The states' experiences underscore the importance of providing strong leadership at the top and letting people on the ground improvise and adapt. States operating under gubernatorial directives to increase enrollment and stability of coverage are better positioned to conduct comprehensive reviews of program renewal procedures, make changes, and revisit policies when changes do not produce desired results. Each of the four states studied has shown considerable leadership and commitment to solving instability and churning problems.
Conclusion
Publicly funded coverage is the only source of coverage available to millions of low-income children, families, and working parents who have no access to affordable job-based insurance. Its potential effectiveness is compromised when coverage is unstable. Moreover, coverage instability and churning result in significant and unnecessary costs for states, health plans, providers, and families. The experiences of these four states demonstrate that coverage instability within public programs is not inevitable. It can be averted to a significant degree by adopting key policies and procedures. An ongoing commitment to ensuring coverage stability can produce measurable, sometimes strikingly positive results for children and families and the health care system more broadly.