North Dakota faces challenges common to other rural areas of the country that are relatively disadvantaged in attracting health care professionals and in deploying resources to serve small, geographically dispersed communities. Despite these challenges, the state's health care system appears to be performing better than many others in providing its citizens with accessible, relatively high-quality, and efficient health care services, as evidenced by the findings of two recent reports.
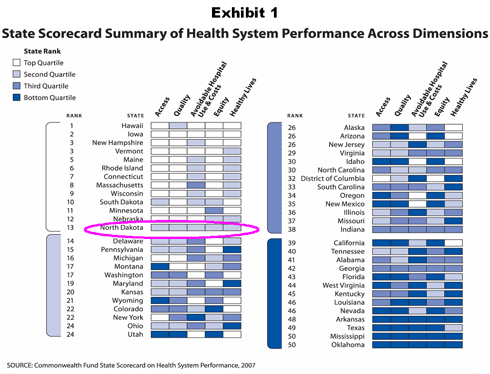
- North Dakota ranks in the top quartile of states on The Commonwealth Fund's State Scorecard on Health System Performance, which ranks states according to their performance across 32 key indicators of access, quality, utilization, equity, and health outcomes (Exhibit 1 and Appendix A).
- The latest Dartmouth Atlas of Health Care finds that North Dakota is one of the most efficient states in treating chronically ill Medicare patients in the last two years of life, with costs more than 25 percent below the national average.
The Commonwealth Fund's Commission on a High Performance Health System made a site visit to North Dakota in July 2007 to learn more about the state's achievements, focusing on three key areas: 1) supports for primary care and the concept of a medical home (discussed below), 2) organization of care through networks of coordination and cooperation; and 3) the innovative use of technology to meet patient needs and hold down costs. Commission members were impressed by the spirit of cooperation that was evident in the dynamics of health care provision in North Dakota. This cooperative ethos is driven by resource scarcity and fostered by a rural community culture that enhances a sense of mutual accountability among health professionals and their patients.
Health care providers, payers, and policymakers in rural North Dakota have learned that only through cooperative, interdependent relationships and a willingness to innovate in both the organization and regulation of services can they achieve the reach, care coordination, and economies of scale that are necessary for delivery of quality and efficient care in rural settings. These innovations provide insights and lessons that may be transferable to other rural areas of the country and to urban areas as well.


