Abstract
- Issue: An array of care gaps and structural barriers inhibits the U.S. primary health care system from fully meeting the needs of women across the life course. Recently, new models of technology-enabled primary health care have emerged, some of which seek to address these gaps and barriers. While these innovations have promise, many of them operate outside the traditional health care system and are only accessible, in their current form, to a narrow segment of consumers.
- Goals: To identify innovative care models, business models, and technologies for improving primary health care for women across ages, races/ethnicities, and socioeconomic backgrounds, and to recommend ways that policymakers, payers, entrepreneurs, clinical leaders, and investors can accelerate reform.
- Methods: Literature review, interviews with experts, and an all-day expert convening with innovators, primary care providers, advocates, policymakers, and payers.
- Findings and Conclusions: Policymakers, payers, entrepreneurs, clinical leaders, and investors each have a role to play in bringing about the changes necessary to achieve a more responsive primary health care system for women across the life course within the next 10 years.
Introduction
In the first report of this two-part series, we catalogued the major care gaps and structural barriers that inhibit the primary health care system from meeting the needs of women of all ages, races/ethnicities, and socioeconomic backgrounds. The fragility of the primary health care system has become markedly apparent in the wake of the COVID-19 pandemic, which placed a significant strain on the health care system (see the first report). To address these gaps and barriers, we proposed a framework for enhancing primary health care for all women through the stages of life (Exhibit 1).
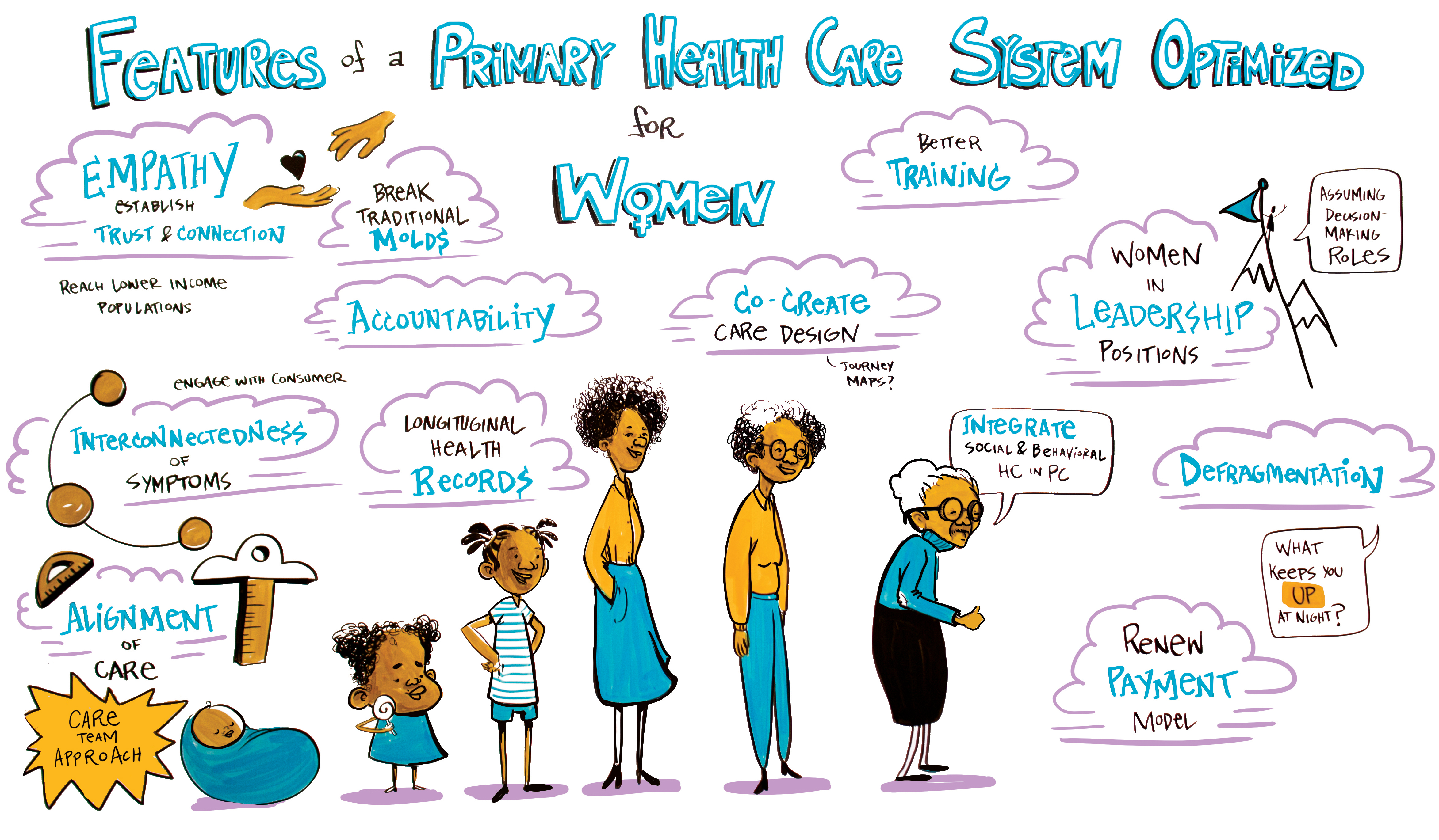
Recently, new models of technology-enabled primary health care have emerged, some of which seek to address these gaps and barriers. While these innovations have promise, many of them operate outside the traditional health care system and are only accessible, in their current form, to a narrow segment of consumers.
The ability to design and scale proven innovations and models across different geographies and demographic groups will be a decades-long endeavor. In many cases, it will require significant changes to how primary health care is designed, delivered, and financed. At the same time, the absence of diverse women’s perspectives in leadership discussions hampers the development of care models and approaches that are responsive to women’s needs.1
Policymakers, payers, clinical leaders, entrepreneurs, and investors each have a role to play in closing these gaps and overcoming these barriers. Clinical leaders and entrepreneurs need to continue to focus on designing and implementing these new models, while policymakers, payers, and investors need to accelerate this evolution by aligning incentives and developing accountability metrics to ensure redesigned primary health care models meet women’s needs.
In this second report, we describe key enablers of an enhanced primary health care system that will respond to women’s needs as they age and transition through stages of life. We also offer recommendations that health system stakeholders can adopt to achieve that vision.
Achieving a Comprehensive Primary Health Care System
Policymakers, payers, entrepreneurs, clinical leaders, and investors can advance five key reforms to meaningfully improve the primary health care system for women:
- Prepare primary health care providers to deliver comprehensive care that directly addresses women’s unique needs.
- Build integrated primary health care teams equipped with the expertise to respond to women’s health needs.
- Embrace primary health care visits as opportunities to build trusted relationships between women and providers and to effectively facilitate linkages to specialty and social services.
- Adopt care models and digital health innovations to expand access to integrated care for women across race/ethnicity, age, and socioeconomic status.
- Prioritize racial/ethnic and gender diversity in leadership across the health care industry.
Training for Primary Health Care Providers to Meet the Unique Needs of Women
Primary health care training programs can be redesigned to ensure that providers are adequately prepared to:
- Comprehensively address women’s primary health care needs.
- Partner with specialists to deliver integrated care.
- Deliver care in a culturally competent and age-sensitive manner.
In a report on women’s health curricula, the U.S. Department of Health and Human Services emphasizes that medical training should take a life course approach to ensure that women’s evolving needs and changing professional and personal obligations are met throughout their lives. This approach compels practitioners to offer culturally competent care that accounts for the impact of gender, sexual orientation, income, and social factors on an individual’s lived experience and health.2

Medical curricula can highlight sex-specific differences in care by interweaving case studies and clinical simulations that focus on women; historically, these have disproportionately featured men.3 Medical training should emphasize empathy towards all patients and acknowledge systemic racism, the intersectionality between gender and race/ethnicity, and pervasive misconceptions in diagnosis and treatment (for instance, a mistaken belief in women’s high pain tolerance) to improve awareness of and responses to implicit and explicit bias. In recent years, medical schools have begun introducing modules and courses that aim to prepare future providers to address and openly confront systemic racism in medicine.4
Preparing Students and Clinicians to Provide Appropriate Care for Women
The Association of Professors of Gynecology and Obstetrics’ Women’s Healthcare Education Office developed a comprehensive set of medical training competencies to ensure that medical students of all specialties are prepared to provide appropriate care for women.5
In another example, the University of California, Los Angeles, approaches women’s health training through its Fellowship in Women’s Health. This fellowship opportunity, funded by the Department of Veterans Affairs (VA), accepts two primary health care physicians or ob/gyns each year and seeks to prepare providers to offer medical, surgical, and psychosocial care that is tailored to women’s needs.6 The VA has invested in a number of these fellowships across the national VA health system and sponsors mini-residencies for practitioners to increase their skills in caring for women in the context of primary health care. Through its efforts, the VA has trained several thousand Designated Women’s Health Providers who offer specialized care at every site where women veterans seek health services.7
Transforming Primary Health Care Practices for Women
While women often require care from cardiologists, neurologists, ob/gyns, and other specialists, these providers may not have the bandwidth or incentives to comprehensively address broad and intersecting health needs across the life course. Therefore, as women age and experience natural life transitions like menopause, they require the care and attention of a primary health care provider — possibly in consultation with other specialists — who can monitor their evolving needs and understand emerging patterns that may indicate future health risks.
Research has shown that integrated and team-based primary health care is associated with shorter hospital stays, better management of certain chronic conditions, higher quality care, and lower costs to the health system.8 For example, integrated primary health care teams are more effective than physicians alone in reducing emergency department visits and other higher-cost care among patients with more severe health needs.9 Creating primary health care teams that include multidisciplinary providers and providers with women’s health expertise can help to ensure that women’s needs are comprehensively and cost-effectively addressed in a timely fashion.
Primary health care teams should be multidisciplinary in nature and be able to integrate and coordinate specialty care, behavioral health, nutrition, and social supports. This may require multiple provider types, including nurses, physician assistants, and community health workers.
Retail Clinics: Disrupting Traditional Care Delivery
Retail health clinics are simplifying access to care and co-locating services in environments that intersect with common personal obligations. Retail clinics represent a convenient option for those who cannot obtain a timely appointment with their usual primary health care provider or for those seeking care outside of traditional primary health care practice operating hours. Ideally, retail clinic services should be memorialized in the individual’s primary health care record.
Ninety percent of providers in CVS Health MinuteClinic’s sexual and reproductive health offering are female clinicians. Over 1,100 MinuteClinics, which are located in CVS and Target stores in 33 states and Washington, D.C., offer a range of preventative and general wellness services provided by family nurse practitioners and physician assistants.11 Primary health care services include tuberculosis testing, sports physicals, diabetes treatment, hypertension treatment, and cholesterol screening. Women’s health services include birth control care, urinary tract infection management and, at select sites, pelvic exams.12 The clinics allow appointment-based or walk-in consultations after hours or on weekends, provide virtual access options, are co-located with pharmacies, and provide free parking. Most insurance plans, including Medicaid, are accepted, depending on the region.
Such efforts will require practice and culture change to designate roles and underscore the value of sharing responsibilities across provider types. Primary health care practices should also prioritize gender diversity in recruitment, as many women prefer to see female providers.10
To improve access to primary health care, practices must identify new entry points and co-locate services in more convenient locations such as work- and school-based clinics and retail settings. Providing services before and after business hours on weekdays and during the weekends is essential to improving service utilization.
Tailoring Integrated Care for Women
The Brigham and Women’s Hospital Gretchen S. and Edward A. Fish Center for Women’s Health offers integrated care for women with the goal of addressing women’s needs that are largely “under-diagnosed, under-treated, or underserved.”13 The Center has tailored the primary health care setting for women by adapting the physical space to promote safety and comfort. The primary health care practice invites rotations of specialty providers who offer sex-aware care in neurology, cardiology, dermatology, mental health, and other clinical disciplines. The Center looks to engage providers who recognize that a person-centered approach is essential to providing primary health care.
Reimagining Annual Visits for Women as Opportunities to Deliver Integrated Primary Health Care
Primary health care providers must be equipped to offer women’s health services as part of a care team, ensuring each encounter is a positive, welcoming experience that engages the patient. This care team should include providers who are prepared to address reproductive health care, chronic conditions, behavioral health, and health-related social needs. For example, a primary health care provider may offer gynecologic services during an annual visit and an ob/gyn may provide wellness services as part of an integrated primary health care team.
Primary health care teams should tailor the focus of each visit based on the individual’s medical history and age as well as specific health experiences and risks that women tend to have at different life stages, such as fertility issues or neurological health. These stage-specific experiences are highlighted in the framework we developed for transforming primary health care for women (Exhibit 1). The visit should include timely conversations with women prior to the onset of key life transitions, such as menopause. In addition, primary health care visits should include routine screenings for nonclinical needs, such as food and housing insecurity, homelessness, interpersonal violence, and other social needs.
Providers can create a trusting environment for open dialogue and empower women to ask informed questions and make decisions about their care. For example, beginning each visit with the simple prompt, “What keeps you up at night?” can spark a holistic discussion about the patient’s physical and behavioral health and any social needs she might have.
In addition to an annual in-person visit, women should have regular opportunities to receive care throughout the year by leveraging various forms of virtual care, such as video visits, secure messaging, and remote monitoring, as needed and as clinically appropriate.
To enable primary health care teams to spend adequate time with women during visits, creative and broad adoption of delivery system and payment reforms are needed. These could include the full or partial capitation that is available to patient-centered medical homes,14 which reimburse providers for time invested in conducting comprehensive and empathetic consultations, developing relationships with patients, and screening for social needs.
“What Would You Like to Talk About Today?”
Tia Clinic is a stand-alone comprehensive women’s health clinic that offers gynecology, primary health care, and wellness services. Every patient visit starts with a common question: “What would you like to talk about today?”15 Other practices observe a similar approach by routinely asking women of reproductive age, “Would you like to become pregnant in the next year?”16 These questions can spark an open dialogue between providers and patients, help ensure that women’s concerns are addressed, and help build both trust and continued patient engagement.
Expanding the Use of Digital Innovations in Primary Health Care
Rapid and continuing advancements in digital technology are enabling a fundamental transformation in how primary health care is delivered. Developments in health information exchange, interoperability, mobile sensors and apps, and telemedicine, coupled with increasing adoption rates of smart phones and broadband internet access, are allowing for the design and implementation of digitally enabled primary health care models that are more accessible, convenient, and connected than ever before (Exhibit 2).
The perception towards and adoption of digital technology among primary health care providers has improved rapidly in recent years. A study found that nearly 90 percent of primary health care providers view adoption of digital health solutions as advantageous in enhancing their ability to care for patients. Adoption of digital tools that facilitate telehealth consultations, remote monitoring, and patient engagement is increasing year-over-year and is projected to continue expanding.17
As of May 7, 2020, all states plus Washington, D.C., have issued guidance to expand the use of telemedicine in their Medicaid programs during the COVID-19 pandemic.18 These types of digital tools can help primary health care providers deliver comprehensive care to women.
Telehealth solutions, including audio and video calls, texting, and app-based communications, can increase access to primary health care providers regardless of where the patient may be located. Telehealth can also enhance access to specialists, such as psychiatrists, cardiologists, neurologists, and others through virtual specialty consults. Remote monitoring tools can enable primary health care providers to deliver more continuous care to patients with chronic conditions, such as diabetes, heart failure, and chronic obstructive pulmonary disease. Digital tools like these can increase levels of patient engagement in care, which has been shown to lower costs and improve health outcomes.19
Technology Platforms for New Primary Health Care Business Models
Cityblock provides primary health care, women’s health, behavioral health care, and social services to vulnerable populations, leveraging a technology platform that provides a 360-degree view of individual health, including clinical and social needs. Cityblock engages community members in its technology and care model design processes to ensure that its approach responds appropriately to the unique needs of its clients.20
Iora Health, a technology-enabled primary health care company that offers team-based, person-centered care, developed its own technology platform and electronic health record (EHR) called Chirp. Chirp optimizes the system for clinical care (as opposed to billing) and enables Iora to constantly improve its technology.21
While digitally enabled primary health care models have tremendous potential, much work is needed to continuously evaluate and demonstrate their efficacy and impact. Moreover, most innovations are currently only available to a limited subset of the population that can pay out-of-pocket or is commercially insured. Moving forward, these ventures must seek to expand the reach of proven models to lower-income populations.
Opportunities for Policymakers, Payers, Entrepreneurs, Clinical Leaders, and Investors
As novel care models and technology-enabled solutions emerge, policymakers, payers, entrepreneurs, clinical leaders, and investors each have a unique role to play in accelerating the development and adoption of comprehensive primary health care approaches that meet the unique needs of women across the life course. Both a literature review and the roundtable discussion between national experts and industry leaders identified myriad opportunities to advance women’s primary health care. In this section, we discuss the most important and pressing of these opportunities.
Policymakers and Payers
Medicaid provides coverage for 25 million women ages 18 and older, and is the largest source of coverage for births in the United States.22 Of the population over age 65 that relies on Medicare coverage, 56 percent are women; among enrollees over age 85, two thirds are women.23 Federal and state programs, therefore, have a significant responsibility to ensure that women have access to age-sensitive care from appropriately-trained clinicians to address their needs comprehensively.
Policymakers and payers should:
- Expand Medicaid and create new, targeted coverage pathways or eligibility groups (for example, postpartum care, family planning services) that focus on improving coverage among women.
- Invest in Federally Qualified Health Centers to develop and deliver integrated women’s health and primary health care models.
- Augment and restructure primary health care reimbursement to pay providers for assessing and responding to social determinants of health.
- Require increased representation of women in clinical trials and increase federal grant funding for research on sex differences in disease progression and treatment.

Entrepreneurs and Clinical Leaders
Entrepreneurs and clinical leaders across the health care industry can enhance the primary health care system for women by designing and scaling solutions that respond to gaps and barriers in the system.
Entrepreneurs and clinical leaders should:
- Recruit teams that are diverse in gender and race/ethnicity and that reflect the communities they serve.
- Engage female patients across races/ethnicities in the co-creation and design of solutions for women.
- Leverage technology to enhance integration across physical health, behavioral health, and social support services.
- Broaden the number and types of entry points that individuals can use to seek primary health care, including through the use of virtual primary health care models.
- Measure primary health care access on the basis of race/ethnicity, income, and first language and tailor models to ensure inclusion.
- Commit to ensuring that innovations will reach women of all income levels, races/ethnicities, and socioeconomic backgrounds at each age and stage of life, including developing business roadmaps that identify pathways to reach women who are enrolled in Medicaid.
- Measure and demonstrate the return on investment of new care models and technologies in achieving positive health outcomes and disseminate lessons learned to encourage adoption of and continued investment in novel approaches across the industry.
Investors
Historically, investment in technologies and products designed to address women’s health needs has been low. Though women are the fastest-growing group of entrepreneurs in the United States, women receive less than 5 percent of small business lending. Some venture funds have recognized a particular disparity in the investments made in ventures directed by low- to moderate-income women and women of color.24 Beginning in 2015, venture capital investment in women’s health began to trend upward at a rapid pace, totaling $354 million in 2017.25 This shift in “femtech” investment may reflect a growing recognition of the value proposition and extraordinary market potential for these products.26 By 2025, the global market potential for femtech is projected to reach $50 billion.27

It will be essential for investors in health care venture funds to recognize that funding products and services for women is as important as funding female founders and female founders of color. To capitalize on the investment opportunity, funds must include women in investment decisions and remove the institutionalized bias against funding women-focused companies or companies focused on health needs of various racial and ethnic groups.
Investors should:
- Aggressively hire diverse investment professionals to achieve gender parity across venture capital leadership.28
- Train investors to be more aware of gender-specific differences in health outcomes and experiences.
- Require diverse leadership and management teams at the health care companies they invest in.
Defining Success
Policymakers, payers, entrepreneurs, clinical leaders, and investors are challenged to use the framework proposed in these reports to define success measures and evaluate progress made towards achieving a primary health care system that optimally meets women’s needs in the next 10 years. Measures should include the following targets:
- Achieving equity in primary health care visit attendance and routine screenings across women of all racial/ethnic and socioeconomic backgrounds.
- Minimizing the number of women who do not have a primary health care provider.
- Adopting telehealth solutions across all primary health care practices.
- Augmenting medical school and residency curricula to include women’s health topics.
- Achieving parity in venture capital investments in women’s and men’s health solutions.
- Evolving health care leadership teams so that diverse women represent at least half of the decision makers.
Conclusion
Today’s primary health care system is not designed or operated in a manner that fully meets the physical health, behavioral health, or social needs of women, particularly as those needs evolve as women transition through various ages and stages of life. Policymakers, payers, entrepreneurs, clinical leaders, and investors all have roles to play in bringing about much needed reforms and in achieving a primary health care system that optimally serves women in the next 10 years.
How We Conducted This Study
To inform this effort, Manatt Health first reviewed current academic literature on primary health care and conducted interviews with 15 multidisciplinary industry leaders and subject matter experts representing innovators, payers, health systems, and academia. Learnings from this preliminary investigation informed a robust, all-day meeting that The Commonwealth Fund convened between 17 innovators and national experts in December 2019 on opportunities to transform primary health care for women. The convening participants were selected for their deep expertise, the breadth of organizations they represent across the health care industry, and their professional and personal perspectives on primary health care for women. A complete list of individuals who contributed to this work appears in the Acknowledgments section.
Acknowledgments
The Commonwealth Fund
- Yaphet Getachew, Program Associate
- Corinne Lewis, Senior Research Associate
- Eric Schneider, Senior Vice President for Policy and Research
Convening Participants
- Adimika Arthur, HealthTech for Medicaid
- Sydney Etheredge, Planned Parenthood Federation of America
- Seth Feuerstein, Yale School of Medicine
- Ann Garnier, Lisa Health
- Margaret Laws, HopeLab
- Debra Ness, National Partnership for Women and Families
- Neil Patel, Iora Health
- Ileana L. Piña, Wayne State University/American Heart Association
- Christine Ritchie, Massachusetts General Hospital
- Evan Schnur, Walmart
- Lisa Simpson, AcademyHealth
- Leah Sparks, Wildflower Health
- Emily Stewart, Community Catalyst
- Deneen Vojta, UnitedHealth Group
- Jane Weldon, CommonSpirit Health
Stakeholder Interview Participants
- Molly Coye, Executive in Residence, AVIA
- Joia Crear Perry, National Birth Equity Collaborative
- Susan Edgman-Levitan, Executive Director, John D. Stoeckle Center for Primary Care Innovation, Massachusetts General Hospital
- Mary Langowski, Founder and CEO, Rising Tide
- Emily Maxson, Chief Medical Officer, Aledade, Inc.
- Sharon Vitti, Senior Vice President and Executive Director, CVS Health/MinuteClinic
- Jeanette Waxmonsky, Vice President Integrated Care, Product Development at New Directions Behavioral Health
- Elizabeth Yano, Director, VA Center for the Study of Healthcare Innovation, Implementation & Policy
Manatt Health Subject Matter Experts
- Jocelyn Guyer, Managing Director, Manatt Health
- Brenda Pawlak, Managing Director, Manatt Health
- Carol Raphael, Senior Advisor, Manatt Health
- Edith Coakley Stowe, Director, Manatt Health
- Sharon Woda, Managing Director, Manatt Health
Graphic Recording
- Sasha Brito, ImageThink