Abstract
By expanding access to affordable insurance coverage for millions of Americans, the Affordable Care Act will likely increase demand for the services provided by federally qualified health centers (FQHCs), which provide an important source of care in low-income communities. A pair of Commonwealth Fund surveys asked health center leaders about their ability to function as medical homes. Survey findings show that between 2009 and 2013, the percentage of centers exhibiting medium or high levels of medical home capability almost doubled, from 32 percent to 62 percent. The greatest improvement was reported in patient tracking and care management. Despite this increased capability, health centers reported diminished ability to coordinate care with providers outside of the practice, particularly specialists. Ongoing federal funding and technical support for medical home transformation will be needed to ensure that FQHCs can fulfill their mission of providing high-quality, comprehensive care to low-income and minority populations.

OVERVIEW
Federally qualified health centers (FQHCs), also known as community health centers, provide comprehensive primary care, behavioral health services, and dental care to all patients regardless of their ability to pay or health insurance status. Located primarily in medically underserved areas, these centers are a core component of the health care delivery system for low-income and minority populations. In 2012, 21 million patients, the majority of whom were either uninsured (36%) or publicly insured (49%), made 85.6 million visits to the nation’s nearly 1,200 FQHCs operating in 8,500 sites.1 In addition to health services, FQHC staff provide patients with insurance eligibility and enrollment assistance, case management, language interpretation, and transportation services. It is clear that these safety-net providers are a critical source of care for low-income and minority populations.2
After Massachusetts implemented its health reform program in 2006, there was an increased demand for services at community health centers among newly insured low- and middle-income residents.3 The Affordable Care Act (ACA) has the potential to do the same at FQHCs nationwide, raising questions about the ability of these centers to continue providing high-quality, cost-effective care.
Since 2009, the federal government has provided FQHCs with unprecedented funding for health information technology (HIT) infrastructure to help them deliver more coordinated and efficient care to an ever-growing patient population.4,5 Health centers have also turned to the patient-centered medical home (PCMH) model, which uses HIT, including chronic disease registries and patient portals, along with quality improvement, care management, and enhanced access to meet the needs of their patient populations.
This issue brief presents findings from the 2009 and 2013 Commonwealth Fund Surveys of Federally Qualified Health Centers, which measure the extent to which FQHCs have adopted the medical home model and assess other characteristics that may make FQHCs better able to meet increasing demand. We identified 12 core functions indicative of medical home capability across six domains: patient access and communication, patient tracking and registries, care management, test and referral tracking, quality improvement, and coordination with external providers. A health center is considered to have high medical home capability if it can perform at least nine of the 12 core functions, medium capability if it performs six to eight functions, and low capability if it performs fewer than six functions (Table 1). (To learn how this study was conducted, see page 7.)
FINDINGS
Federally Qualified Health Centers Increased Their Ability to Function as Medical Homes from 2009 to 2013
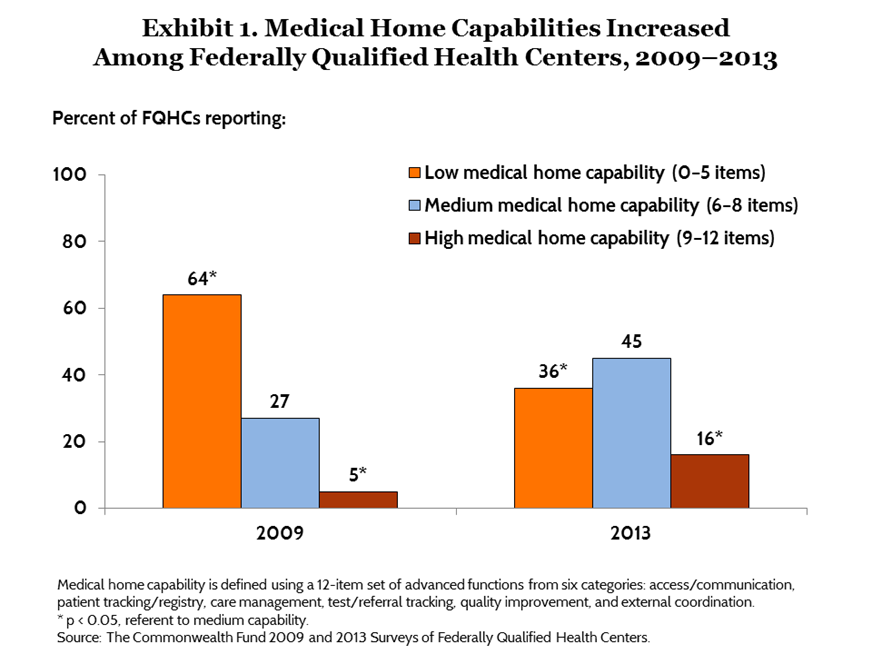
Between 2009 and 2013, the percentage of centers exhibiting high medical home capability more than tripled (Exhibit 1). In 2013, most centers (62%) reported a medium or high level of medical home capability. This is a marked improvement from 2009, when only 32 percent reported a medium or high level, and the majority (64%) exhibited low medical home capability. The largest gains were made in the domains of patient tracking and registry functions and care management capability. However, during this same time period, health centers’ performance decreased in the area of coordinating with external providers.
Financial Incentives and Support for Quality Improvement Are Associated with Medical Home Capability
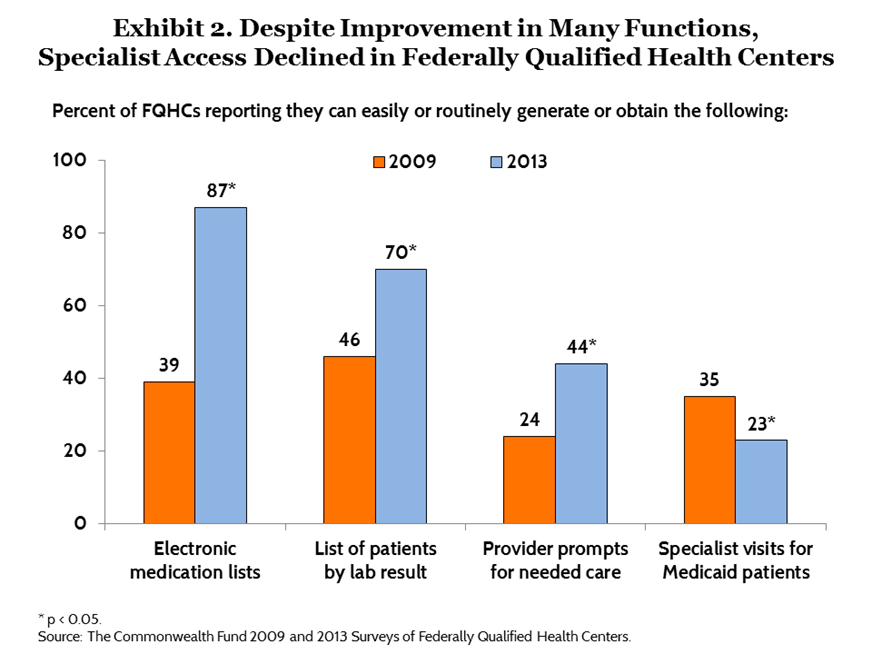
Survey results indicate that health centers that function as medical homes (whether recognized by an accreditation program or not) have greater support for quality improvement activities. Slightly more than one-third of centers overall report having enough dedicated staff (37%) and information systems (37%) to provide timely data and feedback on quality improvement activities. But among FQHCs with high medical home capability, those figures are higher: 56 percent have enough staff and 53 percent have the necessary information systems (Table 2). Overall, in 2013, a far greater percentage of centers (70% vs. 46% in 2009) said they could generate lists of patients according to lab results (Exhibit 2). The ability of centers to electronically generate lists of patients’ active medications more than doubled, from 39 percent in 2009 to 87 percent in 2013. The observed improvement in these patient tracking functions may be due in part to increased adoption of electronic medical record systems that automate these processes.6
Medical home capability is linked to financial incentives. The majority of health centers demonstrating high medical home capability reported receiving financial incentives for participating in quality improvement activities (60%), achieving certain clinical care targets (62%), and managing patients with chronic disease or complex needs (59%) (Table 2). Less than half of centers with low medical home capability reported receiving such support (31%, 43%, and 30%, respectively). Additionally, twice as many health centers with high medical home capability reported receiving incentives for high patient satisfaction ratings (34% compared to 17%). These findings support recent literature showing that adequate financial support can better facilitate medical home transformation.7,8
Health Centers with Higher Medical Home Capability Have Greater Workforce Stability
Transforming a practice to a medical home can be an arduous and painful process and the changes required may be disorienting to and demanding on staff.9 However, our results show that nearly half (47%) of health centers that met our definition of high medical home capability reported improved or much improved provider and staff satisfaction over the past two years, compared with only 39 percent of those with medium capability and 27 percent of those with low capability (Table 2). Those with high medical home scores also reported improved or much-improved ability to recruit and retain physicians, nurses, and support staff. These results indicate that while high staff turnover may be a barrier to effective transformation, it is not necessarily a symptom of the transformation process itself. (For further findings on health center workforce issues, see Ready or Not? How Community Health Centers View Their Preparedness to Care for Newly Insured Patients.)
Medical Home Capability Is Linked to Greater Access to Specialty Care Overall, but Difficulties Remain for Medicaid Patients
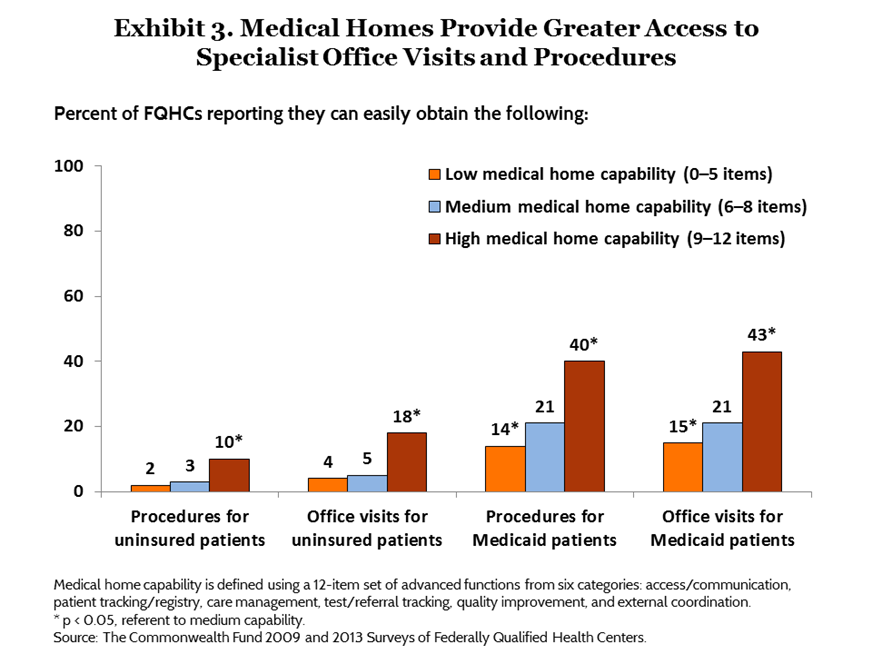
Though health centers have increased their patients’ access to primary care, they still struggle with obtaining specialty care for their patients, particularly for Medicaid and uninsured patients, who make up nearly three-quarters of the patient population served by FQHCs.10 From 2009 to 2013, the number of health centers reporting they can easily obtain specialist or subspecialist appointments for their Medicaid patients declined 34 percent (Table 1). Fewer than one-quarter of centers reported easily obtaining specialist or subspecialist appointments (22%) and procedures (22%) for their Medicaid patients. These figures drop to 7 percent and 4 percent, respectively, for uninsured patients (Table 3). Health centers with high medical home capability report they can easily obtain procedures or office visits with specialists for their Medicaid patients at double the rate of medium- and low-capability centers (Exhibit 3). Greater medical home capability is also correlated with the ability to track referrals. Nearly four of five (79%) high-capability health centers track specialist and subspecialist referrals until the consultation report returns to the referring provider; about half as many (42%) low-capability health centers are able to do this (Table 3).
Medical Home Capability Is Associated with Greater Provision of Behavioral Health, Dental, and Nonmedical Services
FQHCs are mandated to provide either directly or through established written arrangements and referrals all primary and preventive care their patients may need, as well as certain nonmedical services—such as benefit counseling, transportation, and language services—that enable patients to access care and improve their health.11 Despite these requirements, all health centers are not equally capable of providing such services consistently across all sites. More than half of health centers provide services such as dental care (53%) and mental or behavioral health care (53%), benefit counseling and insurance eligibility assistance (51%), and translation services of any kind (74%) (Table 3). Only 30 percent of health centers reported that patients can usually access transportation services when they need them. Across the board, a greater percentage of centers exhibiting high medical home capability are able to offer this array of services.
POLICY IMPLICATIONS
Federally qualified health centers form the foundation of the primary care safety net, serving as willing providers for Medicaid and uninsured patients and meeting the complex health and social needs of low-income and minority populations. By extending health care coverage to millions of Americans, the Affordable Care Act may increase patient demand for FQHC services. Our findings show that on the whole FQHCs have increased their ability to serve as medical homes, providing more comprehensive and coordinated care. As such, they are likely better prepared to meet any increased demands to meet patients’ complex needs under the ACA’s coverage expansions.
FQHCs’ progress in becoming medical homes may be attributable in part to concerted efforts by the Bureau of Primary Health Care to prioritize medical home transformation among the nation’s community health centers. FQHCs may receive federal technical assistance in the form of learning collaboratives, support for developing information centers, and cooperative agreements with state primary care associations and the National Association of Community Health Centers for on-the-ground support. FQHCs have also benefited from additional federal support for capacity expansion and practice transformation under the Affordable Care Act. The ACA authorized $11 billion in funding over five years to expand health center capacity. It also authorized programs that support the spread of the medical home model among health centers. For example, the FQHC Advanced Primary Care Practice Demonstration provided approximately 500 FQHCs with an additional per-member-per-month fee for Medicare beneficiaries, as well as support to achieve medical home recognition from the National Committee for Quality Assurance. In addition, the ACA’s Medicaid health home program aims to better coordinate care for Medicaid beneficiaries with multiple chronic conditions. Ongoing federal support for practice transformation in FQHCs will be critical in maintaining the capability of the primary care safety net to provide high-quality, comprehensive care for low-income and minority populations.
The Safety Net Medical Home Initiative12 (SNMHI), a five-year initiative that supported 65 community health centers in five states to transform into patient-centered medical homes, demonstrated the kind of support needed to assist community health centers in becoming medical homes. Technical assistance and peer-to-peer learning opportunities were highly instrumental in supporting community health centers in achieving medical home status.13 Even with a targeted, hands-on approach, however, many of the sites in the SNMHI did not achieve a high level of success until the third or fourth year. This extended pace of transformation is consistent with previous studies.14,15,16 Continued investment and assistance is necessary to maintain gains already achieved and to support forthcoming success.
FQHCs are making progress in increasing their medical home capability, but challenges remain. Obtaining access to specialty care for Medicaid and uninsured patients is challenging, and this is anticipated to intensify under the Affordable Care Act. FQHCs frequently rely upon inconsistent channels like informal relationships with subspecialists or contracts with community hospitals to obtain specialty care for their patients.17 Participating in integrated delivery systems, such as accountable care organizations, is one promising way to improve specialty care access, but centers will need additional support to overcome the financial and infrastructure challenges to participating in these models.18,19
FQHC patient populations are likely to have nonmedical needs, such as transportation problems, financial challenges, and inadequate access to food and housing, which can interfere with their ability to access care and to benefit from health care interventions. FQHCs tend to offer more nonmedical support services than do other practices, but they need sustainable means of financing these services to provide them consistently.20 Increasing medical home capability can help, as providers may be eligible to receive incentive payments for improving care coordination and linking patients to social services.21
Federally qualified health centers are a core component of the health care safety net and their significance will only increase as more low-income Americans gain health insurance and the remaining uninsured are left with few options to obtain affordable health care. Our surveys highlight areas where additional support is likely needed to enable these providers to continue fulfilling their important mission.
ABOUT THIS STUDYData come from the 2009 and 2013 Commonwealth Fund Surveys of Federally Qualified Health Centers. Surveys were conducted among a nationally representative sample of executive directors or clinical directors at federally qualified health centers (FQHCs). The 2009 survey was completed by mail, online, or by phone by 795 FQHCs (response rate: 79%) between March and May 2009; the 2013 survey was completed by mail or online by 679 FQHCs (response rate: 60%) between June and October 2013. The survey sample was drawn from a list of all FQHCs that have at least one site that is a community-based primary care clinic. The list was provided by the federal Bureau of Primary Health Care. The survey consisted of a 12-page questionnaire that took approximately 20 to 25 minutes to complete. Medical home capability was measured using questions from the Short-Form Safety Net Medical Home Scale, developed by Robert Nocon and colleagues at the University of Chicago. This scale assesses six domains of the medical home: access and communication, patient tracking and registry, care management, test and referral tracking, quality improvement, and external coordination. It asks health centers to rate how well their clinic performs along 12 medical home functions, which represent an abbreviated version of a previously validated 52-item medical home scale. The short-form scale has been shown to correlate well with the full medical home scale. These functions are listed in Table 1 and include: before-hours, after-hours, and weekend visits for well care; same- or next-day appointments; clinical telephone advice on weekends or after-hours; electronic patient medication lists; lists of patients by lab result; patient reminder notices for preventive or follow-up care; provider prompts for appropriate services needed by patients (such as immunizations or screenings); tracking lab tests; collecting and reporting clinical outcome data; collecting and reporting patient experience data; obtaining timely specialist appointments for Medicaid patients; and receiving hospital discharge reports. In this study, a health center is considered to have high medical home capability if it can perform at least nine of the 12 core functions; medium capability is defined as meeting six to eight functions, and low capability is defined as meeting fewer than six functions. Data were weighted by number of patients, number of sites, geographic region, and urban/rural location to reflect the universe of primary care community centers as accurately as possible. |
Notes
1. U.S. Department of Health and Human Services, Bureau of Primary Health Care, 2012 Health Center Data (Washington, D.C.: DHHS, 2012).
2. V. A. Lewis, C. H. Colla, K. E. Schoenherr et al., “Innovation in the Safety Net: Integrating Community Health Centers through Accountable Care,” Journal of General Internal Medicine, July 2014 29(11):1484–90.
3. L. Ku, E. Jones, P. Shin et al.,“Safety-Net Providers After Health Care Reform: Lessons from Massachusetts,” Archives of Internal Medicine, Aug. 8, 2011 171(15):1379–84.
4. Patient Protection and Affordable Care Act of 2010 (P.L. 111-148, March 23, 2010).
5. American Recovery and Reinvestment Act of 2009 (P.L. 111-5, Feb. 17, 2009).
6. To learn more about HIT adoption and challenges at FQHCs, see J. Ryan, M. M. Doty, M. K. Abrams, and P. Riley, The Adoption and Use of Health Information Technology by Community Health Centers, 2009–2013 (New York: The Commonwealth Fund, May 2014).
7. M. B . Rosenthal, M. W. Friedberg, S. J. Singer et al., “Effect of a Multipayer Patient-Centered Medical Home on Health Care Utilization and Quality: The Rhode Island Chronic Care Sustainability Initiative Pilot Program,” JAMA Internal Medicine, Nov. 11, 2013 173(20):1907–13.
8. S. Alidina, E. C. Schneider, S. J. Singer et al., “Structural Capabilities in Small and Medium-Sized Patient-Centered Medical Homes,” American Journal of Managed Care, July 1, 2014 20(7):e265–e277.
9. E. H. Wagner, R. Gupta, and K. Coleman, “Practice Transformation in the Safety Net Medical Home Initiative: A Qualitative Look,” Medical Care, Nov. 2014 52(11 Suppl. 4):S18–S22.
10. DHHS, Bureau of Primary Health Care, 2012 Health Center Data, 2012.
11. Public Health Service Act, U.S. Code 42 (1944), § 254b.
12. This initiative was supported by The Commonwealth Fund, Qualis Health, and the MacColl Center for Health Care Innovation at the Group Health Research Institute.
13. K. Coleman, K. E. Phillips, N. van Borkulo et al., “Unlocking the Black Box: Supporting Practices to Become Patient-Centered Medical Homes,” Medical Care, Nov. 2014 52(11 Suppl. 4):S11–S17.
14. R. J. Gilfillan, J. Tomcavage, M. B. Rosenthal et al., “Value and the Medical Home: Effects of Transformed Primary Care,” American Journal of Managed Care, Aug. 2010 16(8):607–14.
15. P. A. Nutting, W. L. Miller, B. F. Crabtree et al., “Initial Lessons from the First National Demonstration Project on Practice Transformation to a Patient-Centered Medical Home,” Annals of Family Medicine, May 2009 7(3):254–60.
16. P. A. Nutting, B. F. Crabtree, W. L. Miller et al., “Journey to the Patient Centered Medical Home: A Qualitative Analysis of the Experiences of Practices in the National Demonstration Project,” Annals of Family Medicine, May 2010 8(Suppl. 1):S45–S56.
17. K. Neuhausen, K. Grumbach, A. Bazemore et al., “Integrating Community Health Centers into Organized Delivery Systems Can Improve Access to Subspecialty Care,” Health Affairs, Aug. 2012 31(8):1708–16.
18. L. E. Felland, A. E. Lechner, and A. Sommers, Improving Access to Specialty Care for Medicaid Patients: Policy Issues and Options (New York: The Commonwealth Fund, June 2013).
19. S. Shortell, “Safety Net Challenges in Delivering Accountable Care,” Health Affairs Blog, Nov. 1, 2012.
20. R. Wells, R. S. Punekar, and J. Vasey, “Why Do Some Health Centers Provide More Enabling Services Than Others?” Journal of Health Care for the Poor and Underserved, May 2009 20(2):507–23.
21. D. Bachrach, H. Pfister, K. Wallis et al., Addressing Patients’ Social Needs: An Emerging Business Case for Provider Investment (New York: The Commonwealth Fund, May 2014).
Table 1. Medical Home Capability
| Total 2009 | Total 2013 | Absolute change | Relative change | |
| Percent distribution | 100% | 100% | — | — |
| Unweighted n | 795 | 679 | — | — |
| Medical Home Capability | ||||
| 0-5 of the below items | 64 | 36 | -28 | -44% |
| 6-8 of the below items | 27 | 45 | 18 | 67% |
| 9-12 of the below items | 5 | 16 | 11 | 220% |
| Access/Communication | ||||
| Before, after, AND weekend hour visits for well care | 18 | 26 | 8 | 44% |
| Patients are usually able to receive a same- or next-day appointment when they request one | 42 | 51 | 9 | 21% |
| Patients can usually get telephone advice on clinical issues on weekends or after regular office hours | 48 | 62 | 14 | 29% |
| Patient Tracking/Registry | ||||
| Routinely electronically use lists of all medications taken by a patient (including those prescribed by other doctors) |
39 | 87 | 48 | 123% |
| Can easily generate list of patients by lab result | 46 | 70 | 24 | 52% |
| Care Management | ||||
| Patients are usually sent reminder notices when it is time for regular preventive or follow-up care | 19 | 22 | 3 | 16% |
| Provider usually receives an alert/prompt at point of care for appropriate care services needed by patients (e.g., Pap smear or immunizations due) | 24 | 44 | 20 | 83% |
| Test/Referral Tracking | ||||
|
Lab tests ordered are usually tracked until results reach clinicians
|
56 | 66 | 10 | 18% |
| Quality Improvement | ||||
| Data on clinical outcomes are collected and reported at the provider level | 62 | 80 | 18 | 29% |
| Performance data from surveys of patient satisfaction and experiences with care are collected and reported at the provider level | 44 | 65 | 21 | 48% |
| External Coordination | ||||
| Providers can easily obtain timely appointments for office visits with specialists or subspecialists for Medicaid patients | 35 | 23 | -12 | -34% |
| Center usually receives a discharge summary or report from hospital | 36 | 32 | -4 | -11% |
Note: Data in bold: p ≤ 0.05.
Source: The Commonwealth Fund 2009 and 2013 Surveys of Federally Qualified Health Centers.
Table 2. Benefits of Medical Homes
| Medical Home Capability* | ||||
| Total 2013 | Low | Medium | High | |
| Percent distribution | 100% | 36% | 45% | 16% |
| Unweighted n | 679 | 247 | 308 | 112 |
| Quality Improvement | ||||
| Center has enough support for the following quality improvement activities: | ||||
| Dedicated staff to lead QI activities | 37 | 26 | 38 | 56 |
| Information systems to provide timely data and feedback to staff on QI activities | 37 | 24 | 41 | 53 |
| Financial support for QI activities | 25 | 16 | 29 | 37 |
| Opportunities for staff training in QI | 22 | 13 | 24 | 37 |
| Opportunities for staff recognition for QI activities | 19 | 13 | 20 | 29 |
| Participation in learning communities and/or collaboratives | 32 | 26 | 33 | 41 |
| Access to practice facilitators or QI coaches for QI activities | 22 | 11 | 23 | 38 |
| Financial Incentives | ||||
| Center can receive financial incentives at provider and/or center level for the following: | ||||
| High patient satisfaction ratings | 23 | 17 | 23 | 34 |
| Achieving certain clinical care targets | 51 | 43 | 54 | 62 |
| Center participation in quality improvement activities | 42 | 31 | 45 | 60 |
| Managing patients with chronic disease or complex needs | 42 | 30 | 46 | 59 |
| Staff Turnover | ||||
| Over the past two years, the center's ability to recruit and retain the following staff has improved: | ||||
| Nurses | 26 | 20 | 27 | 37 |
| Physicians | 23 | 19 | 25 | 31 |
| Other staff (e.g., community health workers, case managers, benefit counselors) | 25 | 23 | 24 | 36 |
| Over the past two years, provider and staff satisfaction has improved | 35 | 27 | 39 | 47 |
Notes: Data in bold: p ≤ 0.05. Unweighted totals do not sum to 679 because of limited nonresponse.
Source: The Commonwealth Fund 2013 Surveys of Federally Qualified Health Centers.
Table 3. Access to Specialty and Nonmedical Services
| Medical Home Capability* | ||||
| Total 2013 | Low | Medium | High | |
| Percent distribution | 100% | 36% | 45% | 16% |
| Unweighted n | 679 | 247 | 308 | 112 |
| Nonmedical Services | ||||
| Patients can usually access the following services when they need them: | ||||
| Benefit counseling or insurance eligibility assistance | 51 | 43 | 55 | 60 |
| Transportation services | 30 | 23 | 36 | 34 |
| Dental care | 53 | 45 | 57 | 62 |
| Mental or behavioral health care | 53 | 42 | 57 | 66 |
| Non-English speakers can usually access the following services: | ||||
| Translation services | 74 | 67 | 78 | 80 |
| Bilingual clinical staff who provide translation | 53 | 49 | 56 | 58 |
| Bilingual nonclinical staff (e.g. front-desk staff) who translate for patients | 55 | 56 | 55 | 58 |
| Trained interpreters onsite within the center | 29 | 31 | 29 | 30 |
| Telephone lines to access off-site interpreters | 63 | 57 | 68 | 63 |
| Specialty Care Coordination | ||||
| Centers can easily obtain specialist/subspecialist office visits for: | ||||
| Uninsured patients | 7 | 4 | 5 | 18 |
| Medicare patients | 44 | 34 | 45 | 65 |
| Medicaid patients | 22 | 15 | 21 | 43 |
| Centers can easily obtain specialist/subspecialist procedures for: | ||||
| Uninsured patients | 4 | 2 | 3 | 10 |
| Medicare patients | 44 | 33 | 44 | 67 |
| Medicaid patients | 22 | 14 | 21 | 40 |
| Center's physicians have admitting privileges at affiliated local hospital | 65 | 61 | 67 | 70 |
| Patients can be referred for specialist/subspecialist care to affiliated local hospital | 80 | 77 | 81 | 86 |
| Referring provider usually receives a report back from the specialist/subspecialist about care given to the patient |
43 | 36 | 46 | 54 |
| Center usually tracks specialist/subspecialist referrals until the consultation report returns to the referring provider | 59 | 42 | 66 | 79 |
| Report from the specialist/subspecialist is usually received by the center within 30 days | 31 | 27 | 33 | 39 |
Notes: Data in bold: p ≤ 0.05. Unweighted totals do not sum to 679 because of limited nonresponse.
Source: The Commonwealth Fund 2013 Surveys of Federally Qualified Health Centers.