Abstract
- Issue: Pharmacies are at center stage in the U.S. health care market given their role in dispensing medications and, during the COVID-19 pandemic, administering vaccines. Understanding the dynamics among pharmacy types and what lies ahead for this industry is critical for U.S. policymakers considering policies aimed at increasing the cost-effectiveness and affordability of prescription drugs.
- Goals: Identify and summarize industry trends in the pharmacy market and their implications for pharmaceutical prices and spending.
- Methods: Literature scan of articles in peer-reviewed journals, government reports, and newspapers and interviews with experts from academia, pharmacy benefit managers, and the pharmacy industry.
- Key Findings: The research uncovered four main aspects of the pharmacy industry that affect drug spending: 1) increased pharmacy consolidation and vertical integration, 2) rising challenges facing independent pharmacies, 3) growth of specialty pharmacies, and 4) the evolving role of mail-order pharmacies and e-commerce platforms.
Introduction
Pharmacies are where most patients receive prescription drugs and, increasingly, vaccines. Retail pharmacists advise patients on their medication regimens and help them avoid drug interactions and screen for possible side effects to medications. Interacting with both patients and physicians, the retail pharmacy sector plays a key role in the distribution and reimbursement of pharmaceuticals. Pharmacies affect drug spending by:
- marking up wholesale drug prices
- negotiating discounts and dispensing fees with pharmacy benefit managers
- substituting generics for more expensive brand-name products
- offering and accepting drug coupons and other non-insurance-based discounts.
Over the past two decades, the pharmacy market has changed significantly: there has been vertical and horizontal consolidation; new forms of pharmacies have emerged in addition to independent, chain retail, and mail-order pharmacies; services offered by retail pharmacies have increased; and new, potentially disruptive, entrants have emerged. There are conflicting theories on the impact of these market changes on competition, drug prices, access to pharmacy services, and the future of the industry. In this issue brief, we review these trends and identify how they may affect policy efforts to contain pharmaceutical prices and spending. A companion issue brief examines pharmacies’ role in making drug purchasing more efficient and in promoting access to preventive care.
Overview of Reimbursement to Pharmacies
Pharmacies buy drugs either directly from manufacturers or from wholesalers. They then contract with and are reimbursed by pharmacy benefit managers (PBMs), which act on behalf of health plans and employers, at negotiated rates plus dispensing fees. Patients also contribute to overall expenditures for prescription drugs through the copayments they provide to the pharmacy at the point of sale. Reimbursement rates between PBMs and pharmacies are based on different pricing benchmarks and vary depending on competitive dynamics and whether a drug is branded or generic (see Appendix).
Brand-name drugs account for approximately 10 percent of dispensed prescriptions,1 but about 75 percent of overall prescription drug spending because they are usually sold at high prices. During brand-name drugs’ market exclusivity periods, payers typically base reimbursement on the drug’s list price — the average wholesale price — minus a negotiated discount, plus a dispensing fee (on average, $2.05).
Generic drugs account for approximately 90 percent of prescription drugs dispensed in the U.S., with generics being dispensed 97 percent of the time they are available.2 Pharmacies traditionally derive a large share of their revenue from generic drugs. This reflects the large volume of generic drugs they dispense as well as the historically higher percentage markups on low-cost generic drugs compared to markups on brand-name drugs. In a recent study, gross generic margins3 for pharmacies averaged 42.7 percent compared to 3.5 percent for brand-name drugs.4
Reimbursement to pharmacies for generic drugs is based on maximum allowable cost (MAC) schedules. These schedules encompass a list of off-patent drugs that includes the maximum price the payer will pay for each drug. States establish their own MAC schedules for Medicaid generic drug reimbursement. PBMs also generate their own MAC schedules, but there is no industrywide standardization for how the benchmark is calculated or which drugs are included on the list.5
In addition to using a MAC schedule for generic drug reimbursement, PBM–pharmacy contracts increasingly include a total cap on generic drug spending called a generic effectiveness rate (GER). GERs stipulate that PBM reimbursement (net of patient copayments) for generics over the contract period does not exceed the average wholesale price, minus a specified percentage. (See Appendix for more on GERs.)
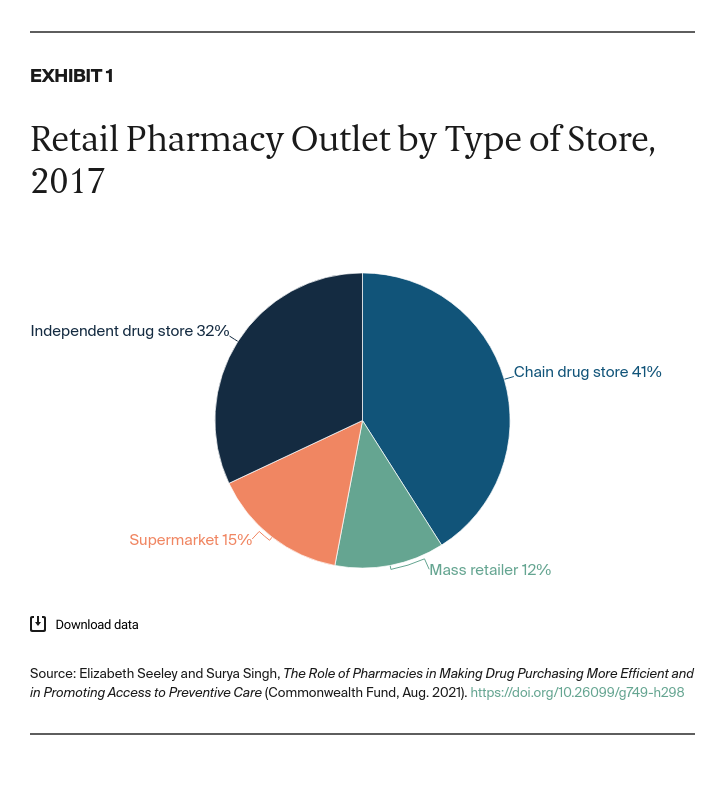
The pharmacy industry has undergone substantial changes over the past three decades. Vertical and horizontal mergers have resulted in a market dominated by large chain pharmacies, as well as supermarkets and mass retailers like Walmart.6 Of the roughly 60,000 retail pharmacies in the U.S., one-third are independent pharmacies and two-thirds are retail chains, supermarkets, or mass retailers,7 which generate 56 percent of retail prescription revenues. There is also a large mail-order industry that competes with brick-and-mortar pharmacies, accounting for 37 percent of retail pharmacy sales in 2017 (Exhibit 1).