In the Literature
Many experts say cross-cultural care can help meet the unique challenges that minority patients face in communicating with their health care providers and obtaining the best possible care. But while most doctors believe that cultural issues are important, many receive little or no training in this area, according to a survey of medical residents supported by The Commonwealth Fund and The California Endowment.
The survey, the results of which are reported in Resident Physicians' Preparedness to Provide Cross-Cultural Care (Journal of the American Medical Association, Sept. 7, 2005), asked resident physicians in their final year of training about attitudes toward cross-cultural care, preparedness to deliver such care, and the general educational climate surrounding cross-cultural training. Their answers, say the authors, suggest there is substantial room for improvement in graduate medical education—particularly in preparing physicians to deal with specific situations, like treating patients who distrust the U.S. health care system or have health practices at odds with Western medicine.
Agreement That Cultural Issues Matter
According to the study, which was limited to seven specialties in which physicians have direct contact with patients (emergency medicine, family practice, internal medicine, obstetrics/gynecology, pediatrics, psychiatry, and general surgery), nearly all residents (96%) believe it is moderately or very important to consider the patient's culture when providing care, although emergency medicine and surgery residents were significantly less likely to respond "very important" (43% and 47%, respectively) than other residents (67% to 94%). Many residents agreed that cross-cultural issues often resulted in negative consequences, including longer office visits (43%), patient nonadherence (21%), and delays in obtaining consent (19%).
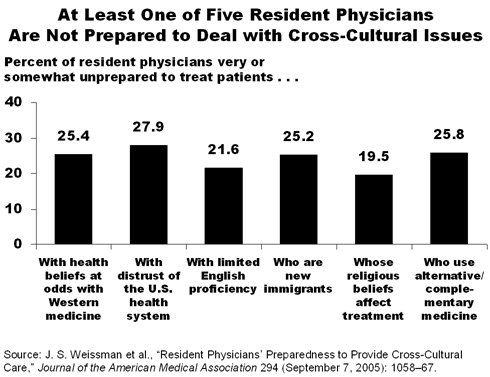
Lack of Preparedness and Training
Few residents said they were very or somewhat unprepared to treat patients from diverse cultures (8%) or racial and ethnic minorities (5%). When queried about specific circumstances, however, residents expressed less confidence. More than one of five residents reported a lack of preparedness to treat patients who have religious beliefs that may affect treatment (20%), use complementary medicine (26%), or are new immigrants (25%).
In comparison, residents reported high levels of technical competence. When they were questioned about preparedness to deliver services or manage common clinical problems in their specialties, 2 percent or less said they were unprepared to treat depression, vaginitis, or heart disease. A higher proportion of respondents, however, felt unprepared to counsel patients on psychosocial issues, like substance abuse or domestic violence.
A general lack of training may account for the low levels of preparedness, the study's authors say. Approximately half of residents reported receiving little or no training in understanding how to address patients from different cultures (50%), or how to identify patient mistrust (56%), relevant religious beliefs (50%), and relevant cultural customs (48%). While residents from programs that offered opportunities to study cultural competency were significantly less likely to report a lack of training, the differences were not great.
More than one-half of respondents (58%) cited time as a moderate or major problems in providing cross-cultural care. Other barriers included lack of language-appropriate written materials (62%) and poor access to interpreters (53%). Only 18 percent mentioned dismissive attitudes of attending physicians, while a greater percentage (30%) cited the lack of good role models.
Discussion
"Our results," write the authors, "suggest that residents may be receiving mixed educational messages." Residents perceive cross-cultural care as important and recognize its implications for delivering high-quality care, but they do not have the time or the mentors to deliver effective cross-cultural care and are not evaluated on their ability to do so. This leads to a troubling disconnect between advocating the importance of cultural competence and nurturing the appropriate climate to achieve it, the authors say. Improving cross-cultural education by increasing opportunities for training, mentoring, and evaluation can ultimately help eliminate racial and ethnic disparities in health care.
Facts and Figures:
- General surgery and emergency medicine residents were significantly more likely to report a lack of cross-cultural training compared with other specialties.
- Most respondents (66%) said they received little or no evaluation on cross-cultural aspects of patient–physician communication.
- Between 2000 and 2003, residency programs offering opportunities to develop cultural competence increased from 36 percent to 51 percent.