In the Literature
In the first in-depth look at seniors' experiences with Medicare's prescription drug benefit, a new survey finds that the majority of seniors who lacked drug coverage in 2005—before the establishment of the benefit—obtained it in 2006. Even with Part D coverage, however, many seniors reported relatively high out-of-pocket spending in 2006. They were also more likely to skip prescribed medication than those who relied on other sources of drug coverage, such as employer-sponsored coverage or benefits from the Department of Veterans Affairs (VA).
The survey, which included self-reported responses from more than 16,000 noninstitutionalized seniors, was conducted in the fall of 2006 by Tufts-New England Medical Center with support from the Kaiser Family Foundation and The Commonwealth Fund. Findings were published in an Aug. 21 Health Affairs Web Exclusive article, "Medicare Prescription Drug Benefit Progress Report: Findings from a 2006 National Survey of Seniors."
More Seniors Report Drug Coverage
The Medicare drug benefit seems to have achieved a primary goal: increasing the number of seniors with drug coverage. "Fewer than 10 percent of seniors lacked prescription coverage in the fall of 2006, and half of all seniors were enrolled in a Part D plan," say the authors. One-third of seniors said they had no drug coverage in 2005, and among this group, 20 percent remained without any coverage in 2006. Seniors lacking drug coverage generally fell into two groups: 1) individuals who are hard to reach because of sociodemographic factors such as age, level of income and education, and geography (i.e., rural residents); and 2) those in relatively good health.
According to the survey, about 50 percent of all Medicare beneficiaries have drug coverage under Part D, another 31 percent under employer-sponsored plans, and 3 percent through the VA.
Part D Enrollees Report Higher Spending
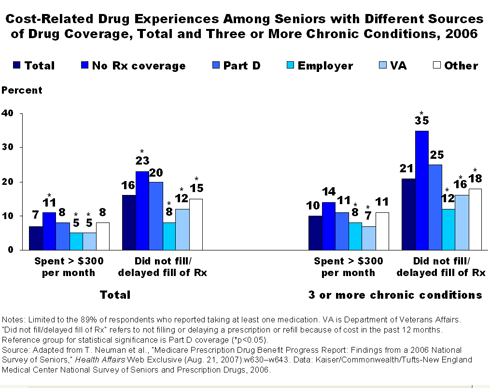
Not surprisingly, seniors without any coverage reported using significantly fewer medications but had higher rates of out-of-pocket spending and "cost-related nonadherence" (forgoing or delaying filling or refilling prescriptions) than seniors either in Part D plans or with other sources of coverage. Among seniors with coverage, those in Part D plans had higher rates of drug out-of-pocket spending in excess of $300 per month than those in employer plans or with other sources of coverage, despite taking a similar or smaller number of medications. Rates of cost-related nonadherence among Part D enrollees were about twice as high as they were for seniors with employer plans or VA benefits. The researchers discovered a similar pattern among seniors with three or more chronic conditions (see figure).
One of four Part D enrollees reported switching to a cheaper medication after enrolling in a Part D plan. This may be a result of beneficiaries moving into plans that use financial incentives, like tiered copayments, to steer enrollees toward lower-cost medications. More than one of seven Part D enrollees said they started ordering prescriptions by mail since signing up for the plan.
Low-Income Seniors Not Aware of Available Assistance
Low-income assistance under Part D is widely viewed as a great benefit to seniors with limited income and assets. Rates of out-of-pocket spending in excess of $100 and $300 per month were significantly lower for seniors receiving the low-income subsidy, including dual eligibles, than for other Part D enrollees. Still, other studies have found that an estimated 3.4 million to 4.7 million beneficiaries who are eligible for this assistance are not getting it. Among seniors with incomes at or below 150 percent of poverty who were not receiving the subsidy, only half said they were aware of the program, suggesting missed opportunities for education and outreach efforts.
Conclusions
Overall, the survey indicates that the drug benefit has reached the majority of seniors who lacked drug coverage in 2005. However, the findings also show that Part D plans provide less financial protection against high out-of-pocket drug spending and cost-related nonadherence than either employer plans or the VA. "More than a quarter of all seniors reported spending at least $100 per month on their medications, and 8 percent reported spending $300 or more each month," the authors write. Future research, they say, should focus on identifying the factors that contribute to high out-of-pocket spending among Part D enrollees including the coverage gap known as the "doughnut hole," formulary restrictions, and cost-sharing requirements. Additional research also is necessary to track the experiences of the most vulnerable beneficiaries to assess the long-term effects of the Medicare drug benefit on those with the greatest health needs.