Full text is available at:
http://content.healthaffairs.org/cgi/content/abstract
/27/5/1235?ijkey=xGyM8BnoFl/q2&keytype=ref&siteid=healthaff
In the Literature
Synopsis
Through innovations like patient-centered medical homes, chronic disease management, and bundled payment of acute-care episodes, Geisinger Health System in Pennsylvania is improving its quality of care and achieving better outcomes for patients, while at the same time lowering costs and increasing value.
Background
Serving central and northeastern Pennsylvania, Geisinger Health System comprises nearly 700 physicians across 55 clinical practice sites, three acute-care hospitals, a variety of specialty hospitals and ambulatory surgery campuses, a 215,000-member health plan, and other services and programs. Geisinger's 2.5 million patients are, on average, poorer, older, and sicker than patients nationally.
Innovative Practices
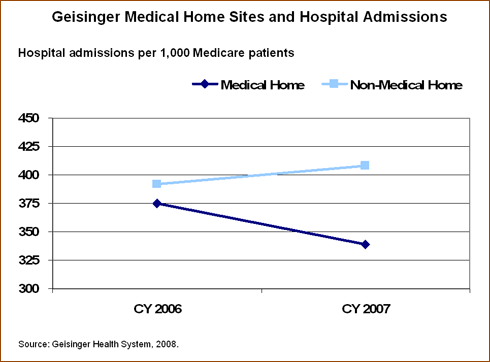
Medical homes. At Geisinger, the implementation of patient-centered medical homes has meant round-the-clock access to primary and specialty care services, which are enhanced through the use of nurse care coordinators, care management support, and home-based monitoring. Physicians and patients alike have access to electronic health records (EHRs); for patients, this means they can view lab results, schedule appointments, receive reminders, and e-mail their providers. To encourage physician participation in the medical home innovation, Geisinger provides practice-based monthly payments of $1,800 per physician, and stipends of $5,000 per 1,000 Medicare patients to help finance additional staff. Preliminary data show a 20 percent reduction in hospital admissions and 7 percent savings in total medical costs. Based on this success, Geisinger is expanding the initiative to additional practice sites.
Chronic disease care optimization. Geisinger provides coordinated, evidence-based care for patients with chronic diseases, including diabetes, congestive heart failure, and hypertension. Through its use of EHRs, Geisinger is able to standardize clinical practices, provide doctors with a "snapshot report" of patients' relevant clinical information, and generate automated reminders for patients as well as the clinical team. Patients can also self-schedule appointments and receive an after-visit summary to see how they are doing compared with their goal. In addition, practices receive performance reports that compare their results with historical trends and peer sites. Physicians may receive financial incentives linked to patient satisfaction, quality, and value goals. Initial results from more than 20,000 diabetic patients have shown statistically significant improvements in measures like glucose control, blood pressure, and vaccination rates.

Acute episode care. Although focusing on primary and chronic care is a priority for Geisinger, some patients will inevitably require acute intervention. To establish and implement best practices, develop a bundled package price for a single episode of care, and promote patient engagement, Geisinger created a new model for coronary artery bypass graft surgery. Teams translated guidelines into 40 discrete steps, which were then embedded into human and electronic workflows. If a step is not completed, providers are automatically alerted. To highlight the need for patient–provider partnership, a team revamped patient education materials and developed a "patient compact," which is signed by both the patient and Geisinger. The single-episode price includes preoperative evaluation and work-up, hospital and professional fees, routine discharge care, and management of related complications occurring up to 90 days post-surgery. Four months after the model was implemented, the proportion of patients receiving all 40 components increased from 59 percent to 100 percent. Geisinger has now expanded the program to include hip replacement and cataract surgery.
Addressing the Problem
Based on Geisinger's experience, the authors say that policymakers nationally should:
- recognize that EHRs are absolutely necessary but not sufficient for creating sustainable change in care delivery.
- align incentives so that providers are rewarded for enhancing value in health care.
- create policies that encourage greater organization of care delivery and payer-provider collaboration.
The Bottom Line
Geisinger has committed to implementing best practices and improving quality and outcomes. Its innovations show considerable promise for improving quality and enhancing value. For their best practices and care models to spread more broadly, health policies to align payment incentives, encourage greater organization of care delivery, and adoption of modern information technology are needed.
Editor's Note: Ronald A. Paulus, M.D., M.B.A., is Executive Vice President and Chief Technology and Innovation Officer; Karen Davis, Ph.D., is a board member; and Glenn D. Steele, M.D., Ph.D., is President and CEO of the Geisinger Health System.